Comedian Hong Yun-hwa recently revealed a 40kg weight loss journey, citing severe respiratory distress as her primary motivation. This case highlights the critical link between obesity and obstructive sleep apnea, emphasizing how significant weight reduction can reverse life-threatening pulmonary complications and drastically improve systemic metabolic health.
While celebrity weight loss is often framed through the lens of aesthetics, Hong’s admission that she found it “hard to breathe” points to a clinical reality: the physiological burden of Class II or III obesity. When excess adipose tissue (fat) accumulates around the neck and thoracic cavity, it creates mechanical restriction of the airways and reduces lung compliance, leading to chronic hypoxia—a state where the body is deprived of adequate oxygen.
In Plain English: The Clinical Takeaway
- Breathing and Weight: Excess weight can physically compress the lungs and block airways, making simple breathing a struggle.
- Metabolic Reset: Losing significant weight doesn’t just change looks; it lowers blood pressure and reduces the risk of Type 2 Diabetes.
- Medical Supervision: Rapid loss of 40kg requires clinical monitoring to prevent gallbladder issues and muscle wasting.
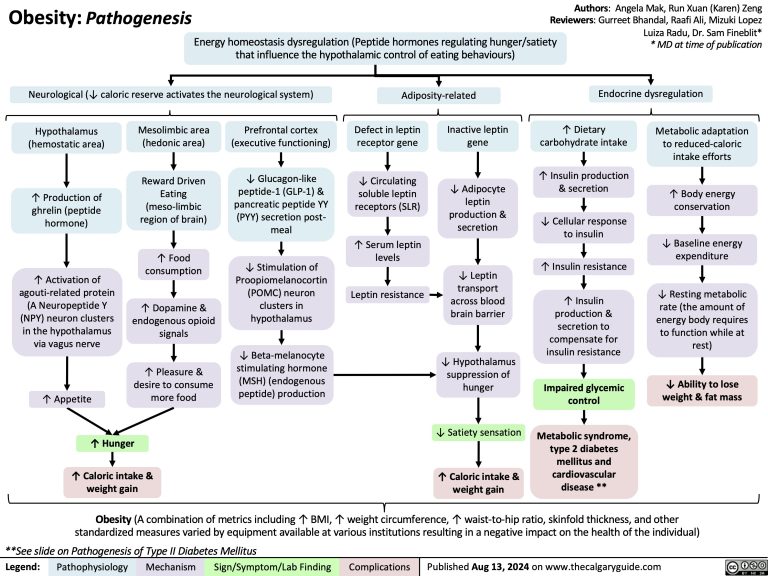
The Pathophysiology of Obesity-Induced Respiratory Distress
The “difficulty breathing” described by Hong is likely a manifestation of Obstructive Sleep Apnea (OSA) or Obesity Hypoventilation Syndrome (OHS). In these conditions, the mechanism of action involves the collapse of the upper airway during sleep or the inability of the diaphragm to fully expand the lungs due to abdominal pressure.
Clinically, this leads to intermittent hypoxia, which triggers a cascade of systemic inflammation. Over time, this increases the workload on the right ventricle of the heart, potentially leading to pulmonary hypertension. By shedding 40kg, a patient significantly reduces the “extrapulmonary load,” allowing for improved gas exchange and a reduction in the sympathetic nervous system’s “fight or flight” response triggered by oxygen deprivation.
“Obesity is not a failure of will, but a complex chronic disease. The intersection of adipose tissue accumulation and respiratory failure represents a critical tipping point where medical intervention becomes a necessity for survival, not just a lifestyle choice.” — Dr. Tedros Adhanom Ghebreyesus, Director-General of the World Health Organization (WHO).
Comparing Modern Weight Loss Interventions
In the current clinical landscape of 2026, the approach to losing 40kg has evolved beyond simple caloric restriction. We now see a tiered integration of pharmacological agents and surgical options, depending on the patient’s Body Mass Index (BMI) and comorbidities.
The rise of GLP-1 (Glucagon-like peptide-1) receptor agonists has shifted the paradigm. These medications mimic hormones that target the area of the brain that regulates appetite and sluggish gastric emptying. However, the global disparity in access remains stark. While the FDA in the United States has expedited approvals for newer dual-agonists, the NHS in the UK and similar European systems under the EMA maintain stricter titration protocols to manage costs and long-term safety.
| Intervention | Primary Mechanism | Typical Efficacy (Weight Loss %) | Primary Clinical Risk |
|---|---|---|---|
| Lifestyle Modification | Caloric Deficit & Hypertrophy | 5% – 10% | Low adherence rates |
| GLP-1 Receptor Agonists | Appetite Suppression/Satiety | 15% – 22% | Gastrointestinal distress |
| Bariatric Surgery | Restrictive/Malabsorptive | 25% – 35% | Nutritional deficiencies |
Funding, Bias, and the Pharmaceutical Influence
It is imperative to disclose that much of the recent data driving the “weight loss revolution” is funded by pharmaceutical giants such as Novo Nordisk and Eli Lilly. While the clinical trials—typically double-blind placebo-controlled studies—show statistically significant results, the industry’s influence can sometimes overshadow the importance of lean muscle mass preservation.
Rapid weight loss, especially when achieved via pharmacological means, can lead to sarcopenia (the loss of skeletal muscle). Without a rigorous protein-intake protocol and resistance training, a significant portion of that 40kg loss may be muscle rather than fat, which can paradoxically lower the basal metabolic rate (BMR) and increase the likelihood of weight regain.
Geo-Epidemiological Impact and Patient Access
The global burden of obesity is rising, but the response is fragmented. In East Asia, where BMI thresholds for “obesity” are often lower than in Western nations due to different risk profiles for Type 2 Diabetes, there is an increasing demand for medicalized weight loss. However, the “medicalization” of weight loss risks ignoring the socio-economic drivers of obesity, such as food deserts and urban design.
Patients in the US often have faster access to the latest pharmacological breakthroughs but face higher out-of-pocket costs, whereas patients in the UK may face longer waiting lists for bariatric surgery despite the procedure being covered by the state. This creates a “health equity gap” where the ability to resolve respiratory distress depends heavily on geography and insurance status.
Contraindications & When to Consult a Doctor
Rapid weight loss is not universally safe. Certain individuals must exercise extreme caution or avoid aggressive weight-loss protocols entirely:
- Patients with a history of Pancreatitis: Some GLP-1 medications are contraindicated due to the risk of acute pancreatitis.
- Individuals with Gallbladder Disease: Rapid weight loss increases the risk of cholelithiasis (gallstones) due to changes in bile composition.
- Pregnant or Nursing Women: Most pharmacological weight-loss agents are strictly prohibited during these periods.
- Patients with Severe Renal Impairment: Changes in protein intake and fluid balance during rapid loss can strain kidney function.
Seek immediate medical attention if you experience: Severe abdominal pain, persistent vomiting, sudden shortness of breath (unrelated to exertion), or signs of extreme electrolyte imbalance, such as cardiac arrhythmias.
The Future of Metabolic Health
Hong Yun-hwa’s journey serves as a poignant reminder that weight loss is often a matter of respiratory and cardiovascular survival. As we move forward, the medical community must pivot from “weight loss” to “metabolic health.” So prioritizing the preservation of lean mass and the resolution of comorbidities like sleep apnea over the number on the scale.
The integration of personalized nutrition, guided by genomic testing and continuous glucose monitoring (CGM), will likely replace the “one size fits all” diet. The goal is no longer just to lose 40kg, but to ensure that the remaining body composition supports a long, healthy, and breathable life.
References
- PubMed: Clinical Trials on GLP-1 Receptor Agonists and Metabolic Syndrome
- World Health Organization (WHO): Global Report on Obesity and Noncommunicable Diseases
- The Lancet: Longitudinal Studies on Bariatric Surgery vs. Pharmacological Intervention
- Centers for Disease Control and Prevention (CDC): Adult Obesity Prevalence and Respiratory Impact
- JAMA: Guidelines for the Management of Obesity in Adults

