
2026 French Open: BWF World Tour Super 750 Paris
The 2026 HSBC BWF World Tour Super 750 Yonex French Open arrives in Paris from October 20–25, 2026, at the Arena Grand Paris in Tremblay-en-France, marking a bold shift from ... Read More

Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

The 2026 HSBC BWF World Tour Super 750 Yonex French Open arrives in Paris from October 20–25, 2026, at the Arena Grand Paris in Tremblay-en-France, marking a bold shift from ... Read More
Continuous Coverage

The U.S. and Iran have reached a proposed agreement to ease tensions in the Strait of Hormuz, with…

Here is the verified, fact-checked article for **archyde.com**: In a trend that has reshaped Indian politics, the line…

For many, Mother’s Day is a celebration of gratitude and family bonds. Though, for those navigating the void…

Walk through any affluent neighborhood in Tokyo or Osaka during the winter months, and you will see them:…

A Ukrainian soldier survived two weeks embedded within a Russian dugout by masquerading as an enemy combatant, exposing…

Nearly 2,000 British holidaymakers have joined a coordinated legal action against TUI, Europe’s largest tour operator, after falling…
Global Affairs

European content creators are increasingly migrating to Las Vegas to leverage the city’s evolution into a global “attention…
Markets And Money

President Donald Trump has announced that the United States will move to free shipping vessels in the Strait…
Digital Culture

Elon Musk testified this week in an Oakland federal court, alleging that OpenAI CEO Sam Altman and president…
Science And Wellbeing
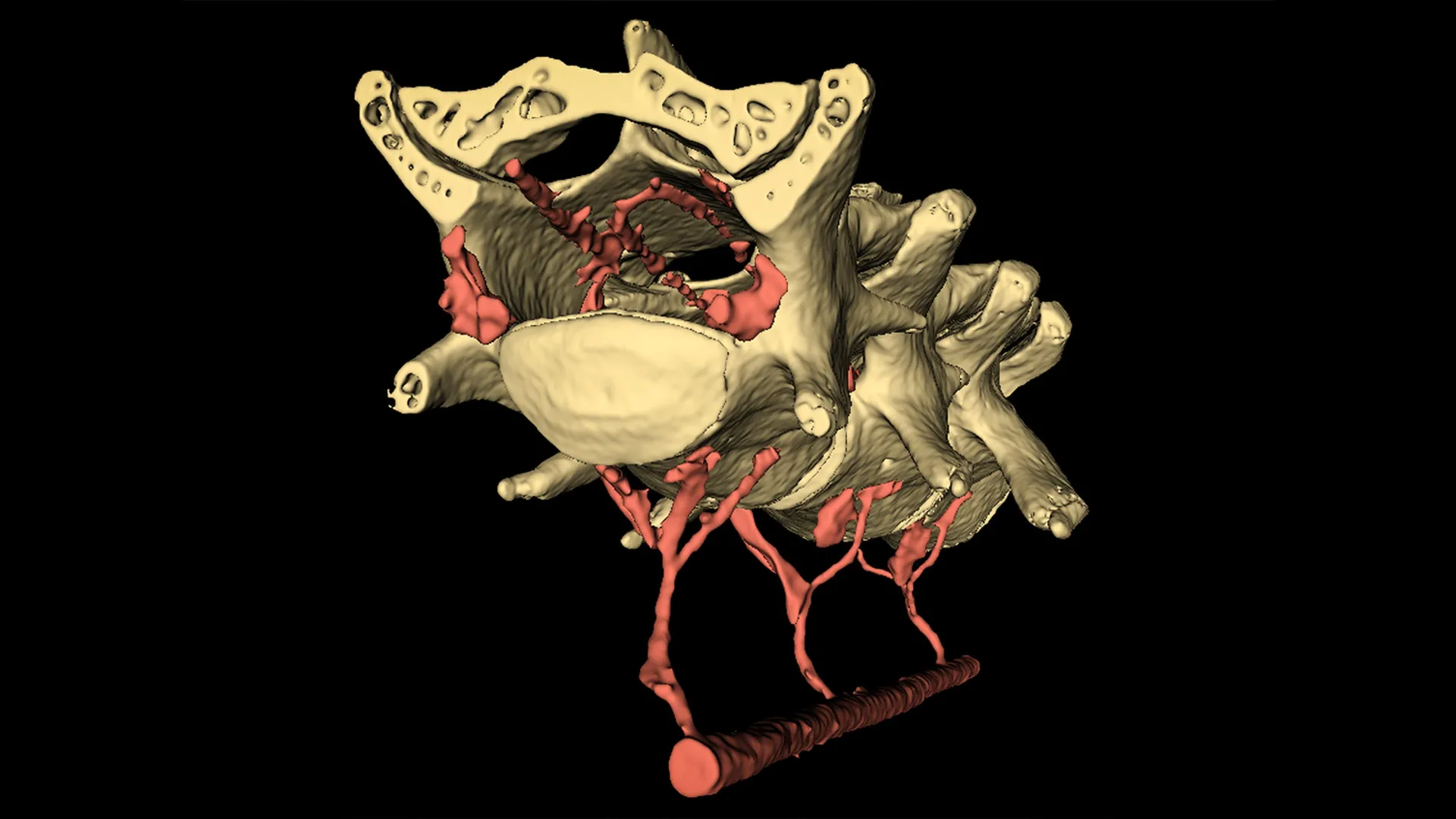
Here is your verified, clinically rigorous and public-health-focused article: Scientists have discovered that subtle movements—like tightening abdominal muscles—trigger…
Screen And Sound

The Blue Devils men’s track and field team dominated Sunday’s competition, securing five event wins and scoring 172…
Fixtures And Form

Here’s the verified, data-driven deep dive into Cameron Young’s 2026 season—why he’s not just a “chill” golfer, but…