
Taiwan Military Procurement Budget Clash: HIMARS Payments at Risk
The clock is ticking in Taipei, and the sound is deafening. It is the rhythmic, stressful countdown of a payment deadline for some of the most lethal hardware the United ... Read More
Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

The clock is ticking in Taipei, and the sound is deafening. It is the rhythmic, stressful countdown of a payment deadline for some of the most lethal hardware the United ... Read More
Continuous Coverage

On May 8, 2026, MFE-MediaForEurope (EUR: MFE) secured prime-time dominance as Grande Fratello Vip outperformed Rai1’s programming. This…

Péter Magyar has been sworn in as Hungary’s Prime Minister, ending Viktor Orbán’s 16-year tenure. This historic transition…

Georgia’s Prosecutor General’s Office has arrested five current and former law enforcement officers charged with violent attacks against…
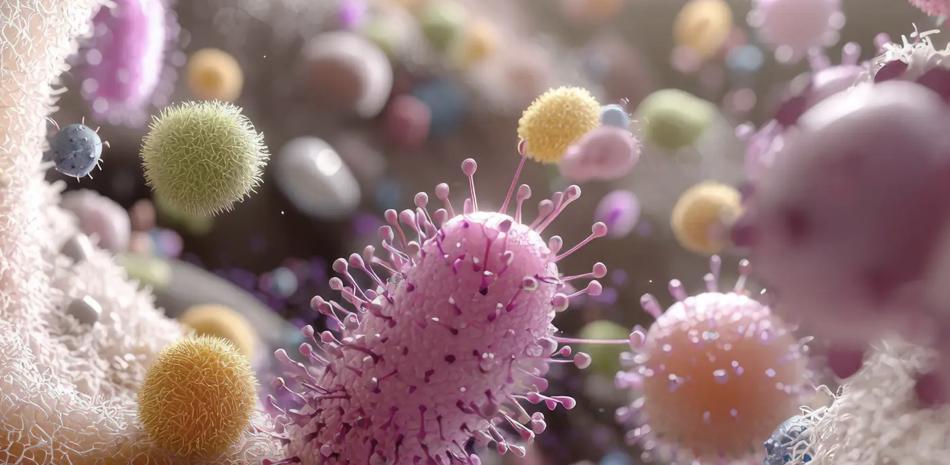
AI-driven biosecurity risks now pose a systemic threat to global markets. By lowering the barrier to synthesize novel…
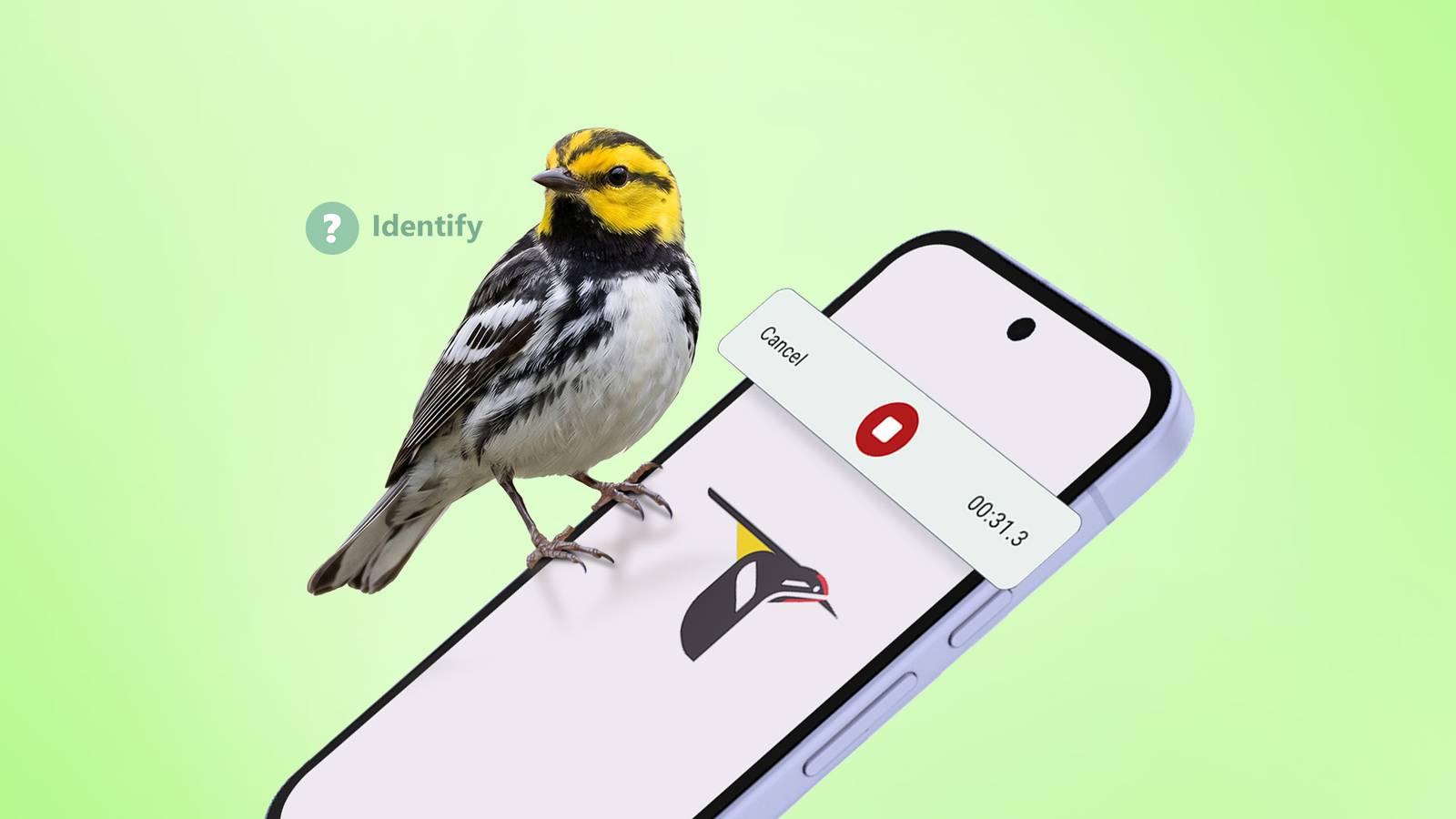
Merlin Bird ID, developed by the Cornell Lab of Ornithology, is a bio-acoustic AI tool that leverages real-time…
US President Donald Trump and Chinese President Xi Jinping are negotiating a “grand bargain” to resolve systemic trade…
Global Affairs

Billionaire Ken Griffin is clashing with New York City’s leadership over proposed luxury taxes targeting the ultra-wealthy. Despite…
Markets And Money

Trump Media &. Technology Group (NASDAQ: DJT) has reported operational losses exceeding $400 million, driven by high infrastructure…
Digital Culture

Meta is integrating premium customization and utility features into WhatsApp for iOS, expanding “WhatsApp Plus” capabilities to Apple…
Science And Wellbeing

Veterinarians recommend life-stage-specific dry dog foods to ensure precise nutrient ratios tailored to a dog’s metabolic needs. By…
Screen And Sound
ESPN is pivoting its “Watch” ecosystem into a full-scale direct-to-consumer (DTC) powerhouse by May 2026, decoupling premium sports…
Fixtures And Form

Boxing dynasties are redefining the sport’s commercial and tactical landscape in 2026. By combining familial instincts with high-performance…