“`html
Medicare Spending on Diabetes Drugs Soars, Rebates Mask True Costs
Table of Contents
- 1. Medicare Spending on Diabetes Drugs Soars, Rebates Mask True Costs
- 2. Dramatic Increase in GLP-1 Utilization
- 3. Shifting Market Share Among GLP-1 Medications
- 4. Claims Data Reveals Rapid Growth
- 5. What are the potential impacts of the GLP‑1 surge on Medicare Part D beneficiaries?
- 6. Medicare Part D’s GLP‑1 Surge: Two Million Enrollees and $27 B Gross Spending – What Comes Next
- 7. The GLP-1 phenomenon: Beyond Diabetes
- 8. The Financial Strain on medicare Part D
- 9. Impact on Beneficiaries: Access and Affordability
- 10. What’s Next? Potential Policy Changes & Future Outlook
- 11. Real-World Example: The Rise of Speciality Tier Costs
- 12. France Travail Data Breach: A Reminder of Data Security Concerns
Washington – Medicare part D spending on Glucagon-Like Peptide-1 (GLP-1) medications – a class of drugs initially designed to treat Type 2 diabetes and now gaining popularity for weight loss – has skyrocketed in recent years, but the actual cost to the program is significantly lower then reported due to ample rebates from manufacturers. The use of newer, more expensive GLP-1s, such as Ozempic and Mounjaro, is driving this trend, while prescriptions for older drugs in the same category are declining.
Dramatic Increase in GLP-1 Utilization
Gross spending on these medications reached $27.5 billion in 2024, a fivefold increase from 2019. This surge reflects greater access to and demand for the latest GLP-1 therapies. However, manufacturers provide significant rebates, estimated at around 50%, effectively reducing the net cost to Medicare. With a 50% rebate factored in, net spending on GLP-1s in 2024 is estimated at approximately $14 billion.
The landscape of GLP-1 prescriptions is evolving. Newer drugs like Ozempic and Mounjaro now dominate the market, eclipsing older options such as Byetta, Victoza, and Trulicity. The potential introduction of oral formulations of these drugs could further alter prescribing patterns, offering patients a more convenient administration method. This shift towards newer drugs has also coincided with recent FDA approvals expanding the use of these medications to treat conditions beyond diabetes, like cardiovascular disease and sleep apnea, though these uses aren’t yet fully reflected in Part D data.
Claims Data Reveals Rapid Growth
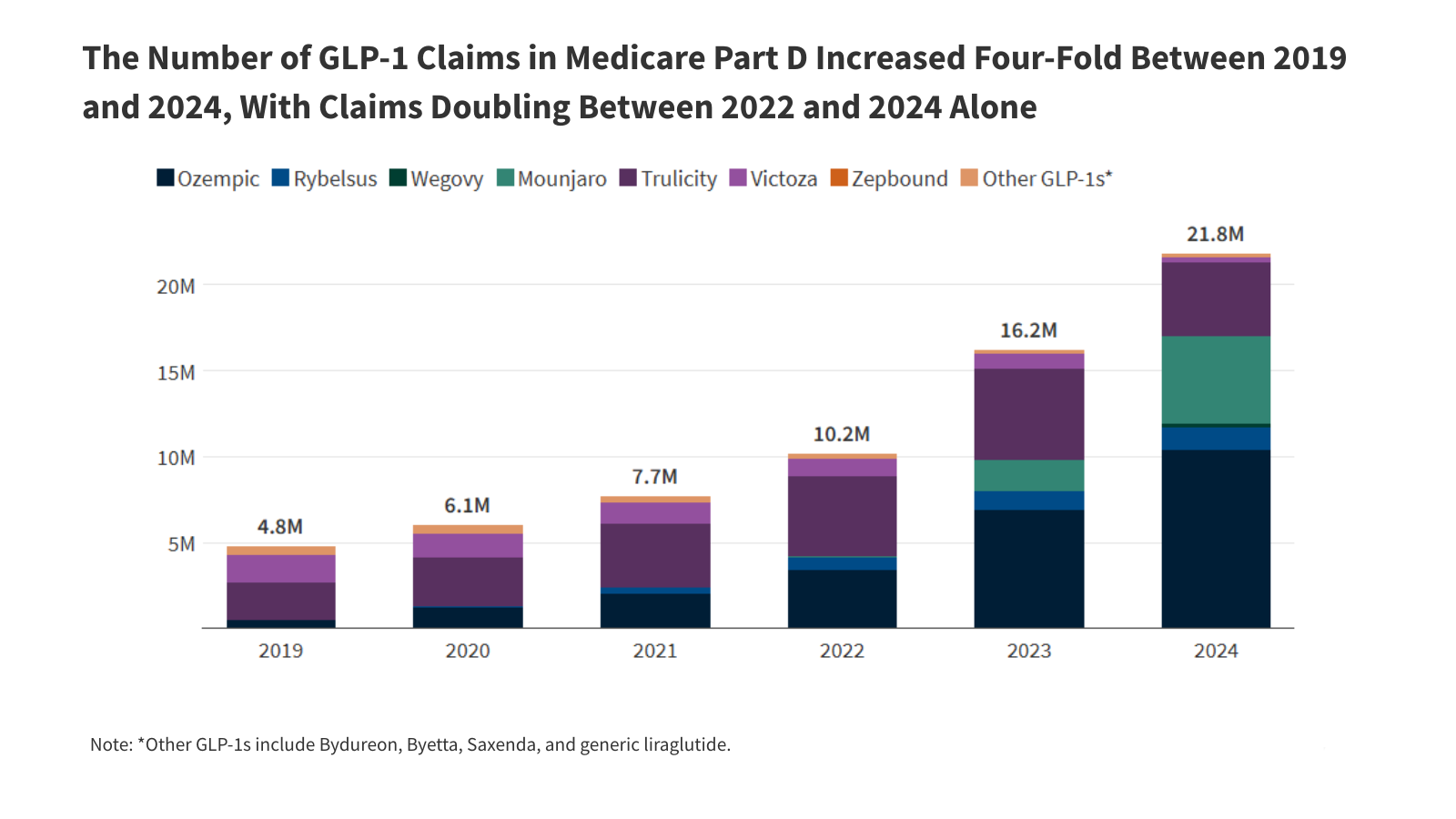
The number of Medicare Part D claims for GLP-1s has quadrupled between 2019 and 2024, jumping from 4.8 million to 21.8 million. This growth has accelerated recently, with claims doubling between 2022 and 2024 alone. Ozempic prescriptions have seen a remarkable 82% average annual growth since 2019,reaching over 10 million claims in 2024,up from just 524,000 in 2019. Mounjaro, a newer entrant, has experienced even faster growth – a staggering 549% annual increase – with 5.1 million claims filed in 2024 compared to 122,000 in 2022.
| GLP-1 Medication | 2019 Claims (Millions) | 2024 Claims (Millions) | % Change |
|---|---|---|---|
| Ozempic | 0.524 | 10.0 | +1812% |
| Mounjaro | 0.122 | 5.1 | +4082% |
Total GLP-
What are the potential impacts of the GLP‑1 surge on Medicare Part D beneficiaries?
Medicare Part D’s GLP‑1 Surge: Two Million Enrollees and $27 B Gross Spending – What Comes Nextthe dramatic rise in prescriptions for glucagon-like peptide-1 (GLP-1) receptor agonists – initially hailed for diabetes management, and now widely used for weight loss – is significantly impacting Medicare Part D. Recent data reveals that approximately two million beneficiaries are now enrolled in Part D plans covering these medications,resulting in a staggering $27 billion in gross spending for 2025. This surge presents both opportunities and challenges for the program, beneficiaries, and the healthcare landscape.Understanding the implications and potential future changes is crucial for navigating this evolving situation. The GLP-1 phenomenon: Beyond DiabetesGLP-1s,including drugs like semaglutide (Ozempic,Wegovy) and tirzepatide (Mounjaro,Zepbound),have revolutionized the treatment of type 2 diabetes.Their ability to improve blood sugar control, promote weight loss, and offer potential cardiovascular benefits has driven unprecedented demand. However, off-label prescriptions for weight loss – even in individuals without diabetes – have fueled the exponential growth in utilization and, consequently, costs within Medicare Part D. This trend isn’t limited to Medicare. The broader demand has led to supply chain issues and, at times, shortages, impacting access for those who genuinely need these medications for diabetes management. The Financial Strain on medicare Part DThe $27 billion figure represents a substantial increase in Part D spending. This increase is impacting premiums, cost-sharing requirements, and the overall financial stability of the program. Several factors contribute to the high cost: * High drug Prices: GLP-1s are among the most expensive drugs covered by Part D. * Increased Utilization: The sheer number of prescriptions filled has skyrocketed. * Off-Label Use: Prescribing for weight loss, without a diabetes diagnosis, adds to the financial burden. * Rebate System Complexity: The current rebate system, where manufacturers negotiate discounts with Part D plans, isn’t fully clear and doesn’t necessarily translate into lower costs for beneficiaries. Impact on Beneficiaries: Access and AffordabilityWhile GLP-1s offer significant health benefits, access and affordability remain major concerns for Medicare beneficiaries. * High Cost-Sharing: Even with insurance coverage, co-pays and deductibles can be substantial, making these medications inaccessible for some. * Prior Authorization & Step Therapy: Many Part D plans are implementing stricter utilization management techniques, such as prior authorization (requiring pre-approval from the insurer) and step therapy (requiring patients to try less expensive medications first). * Coverage Gaps: Some plans may not cover all GLP-1s, or may have limitations on the quantity or duration of coverage. * The inflation Reduction Act’s Impact: The inflation Reduction Act (IRA) is beginning to impact drug prices, with negotiations for some medications under Medicare Part D.However, the full effect of the IRA on GLP-1 costs is still unfolding. What’s Next? Potential Policy Changes & Future OutlookSeveral potential changes are being considered to address the challenges posed by the GLP-1 surge:
Real-World Example: The Rise of Speciality Tier CostsMany Part D plans have moved GLP-1 medications to the specialty tier, resulting in significantly higher co-pays. For example, a beneficiary might pay a co-pay of $50 for a preferred brand-name drug, but $200 or more for a GLP-1 on the specialty tier. This cost difference can be prohibitive for individuals on fixed incomes. France Travail Data Breach: A Reminder of Data Security ConcernsWhile seemingly unrelated, the recent data breach at France Travail, resulting in a €5 million fine (as reported on January 29, 2026, by Le Monde), underscores the importance of data security within healthcare systems. As more health data is digitized and shared, protecting patient privacy and data integrity becomes paramount. This is particularly relevant as Part D plans increasingly rely on electronic prescribing and data analytics to manage utilization and costs.Robust cybersecurity measures are essential to safeguard beneficiary information. Dr. Priya Deshmukh - Senior Editor, Health History at Stake: Djokovic vs. Alcaraz in the Australian Open FinalNikki Bella returns to WWE, eyes Royal Rumble after taking a break |