
Commandment Secures Dominant 6 ¾ Length Victory
Commandment has emerged as the definitive favorite for the 2026 Kentucky Derby following a dominant 6 ¾ length victory in his final prep. By splitting the field on the final ... Read More
Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

Commandment has emerged as the definitive favorite for the 2026 Kentucky Derby following a dominant 6 ¾ length victory in his final prep. By splitting the field on the final ... Read More
Continuous Coverage

Kyotographie is an annual international photography festival in Kyoto, Japan, transforming historic sites into immersive galleries. The 2026…

Quebec grocery retailers are implementing aggressive price cuts on proteins and dairy as of late April 2026. This…
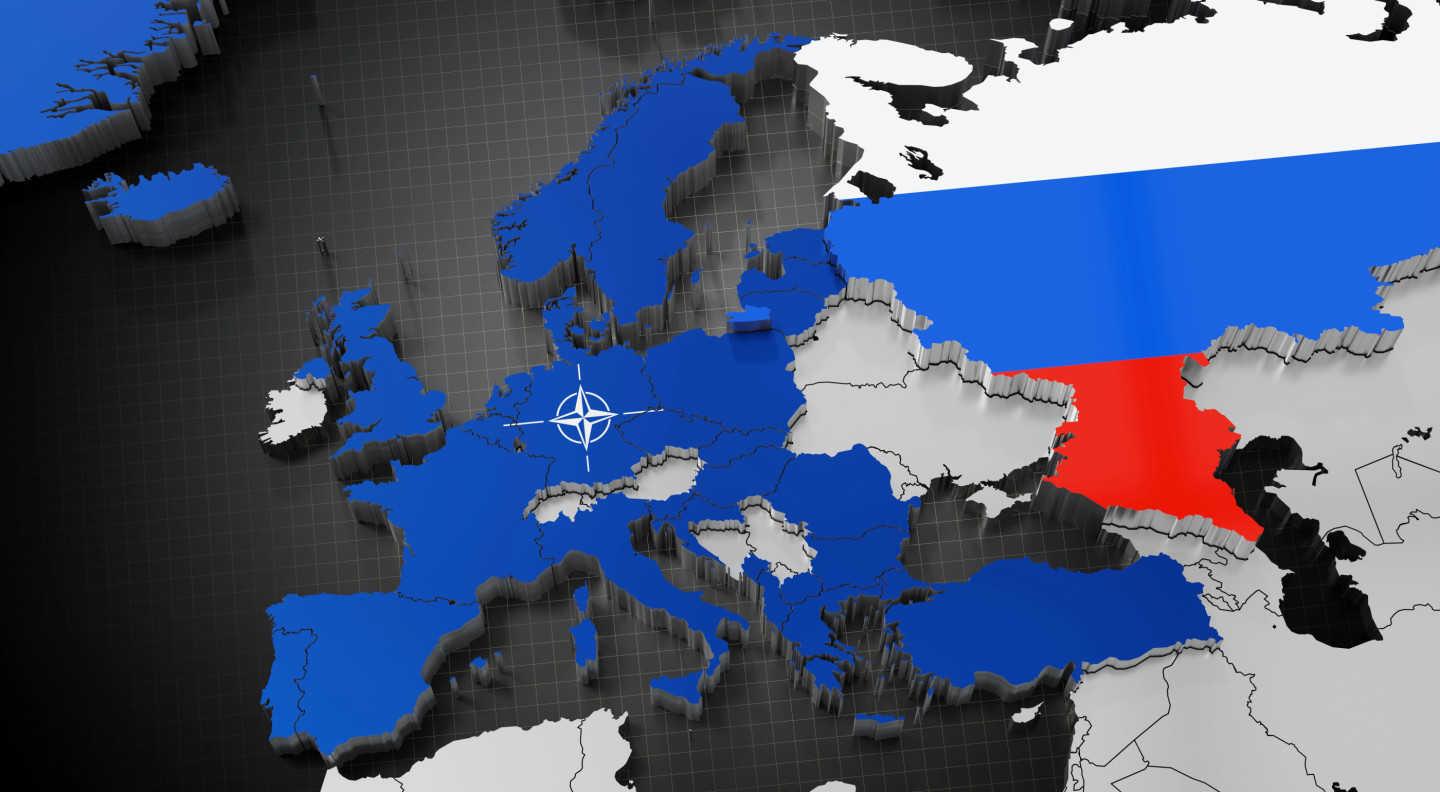
NATO is intensifying defensive postures across the Baltic states as intelligence suggests Russia could attempt an offensive move…
There is a specific, rhythmic soundtrack to urban life in Taiwan—the unmistakable, tinny melody of Beethoven’s “Für Elise”…

Former actor Chen Zhenhua is recovering from Stage 4 Nasopharyngeal Carcinoma (NPC) after 18 months of intensive treatment.…
/data/photo/2025/11/09/690fb7a2a4367.jpg)
AC Milan will face Chelsea at the Gelora Bung Karno Stadium in Jakarta on August 8, 2026. This…
Global Affairs

Concarneau faces Paris 13 Atletico this Thursday, April 30, 2026, at the Stadio Guy-Piriou in the Championnat National.…
Markets And Money

Shares of **Volkswagen (VWAGY)** are facing pressure Monday following the release of Q1 2026 earnings, revealing a 28%…
Digital Culture
Huawei is deploying the Watch Fit 5 and Watch 5 series this week, debuting at a global launch…
Science And Wellbeing

Uranium Mining Expansion in the U.S. Raises Groundwater Contamination Concerns Expanding uranium mining operations in the United States…
Screen And Sound
A leading restaurant chain is moving into Oslo’s artistic Grünerløkka district, marking a pivotal shift in the neighborhood’s…
Fixtures And Form

North Queensland Cowboys head coach Todd Payten is currently the sole NRL coach without a contract beyond the…