Influenza vaccination campaigns are underway globally, with Curitiba, Brazil, initiating a targeted “Day D” program this past Saturday to immunize children, the elderly, and pregnant women against circulating influenza strains. This proactive public health measure aims to reduce severe illness and hospitalization rates during the peak flu season, mirroring similar initiatives across South America and prompting heightened surveillance by international health organizations.
The urgency stems from a complex interplay of factors, including antigenic drift – the constant evolution of influenza viruses – and the potential for co-circulation with other respiratory pathogens like RSV and SARS-CoV-2. Although the Brazilian initiative focuses on vulnerable populations, understanding the broader immunological landscape and vaccine efficacy is crucial for optimizing global influenza control strategies.
In Plain English: The Clinical Takeaway
- Flu Shots Save Lives: Getting vaccinated significantly lowers your risk of getting sick with the flu, especially if you’re young, old, or pregnant.
- Flu Viruses Change: The flu vaccine is updated every year because the virus constantly mutates. This ensures the vaccine matches the strains currently circulating.
- Beyond the Shot: Good hygiene – washing your hands, covering your cough – is still important, even after vaccination, to prevent spreading the virus.
The Evolving Landscape of Influenza Vaccine Development
Current influenza vaccines are primarily based on inactivated or live-attenuated influenza viruses (LAIV), or recombinant hemagglutinin (HA) proteins. These vaccines stimulate an immune response, primarily through the production of neutralizing antibodies that target the HA protein, a key component of the virus responsible for entry into host cells. However, the effectiveness of these vaccines varies significantly, typically ranging from 40% to 60%, due to the aforementioned antigenic drift. The mechanism of action relies on presenting viral antigens to the adaptive immune system, triggering both humoral (antibody-mediated) and cellular immunity.
Recent research, largely funded by the National Institutes of Health (NIH) and the Biomedical Advanced Research and Development Authority (BARDA) in the US, is focusing on the development of a “universal” influenza vaccine. These vaccines aim to elicit a broader immune response targeting more conserved viral proteins, such as the matrix protein 2 ectodomain (M2e) or the neuraminidase (NA) stalk, offering protection against a wider range of influenza strains. Phase I and II clinical trials for several universal vaccine candidates are currently underway, showing promising results in terms of safety and immunogenicity.
Global Surveillance and Regional Impact
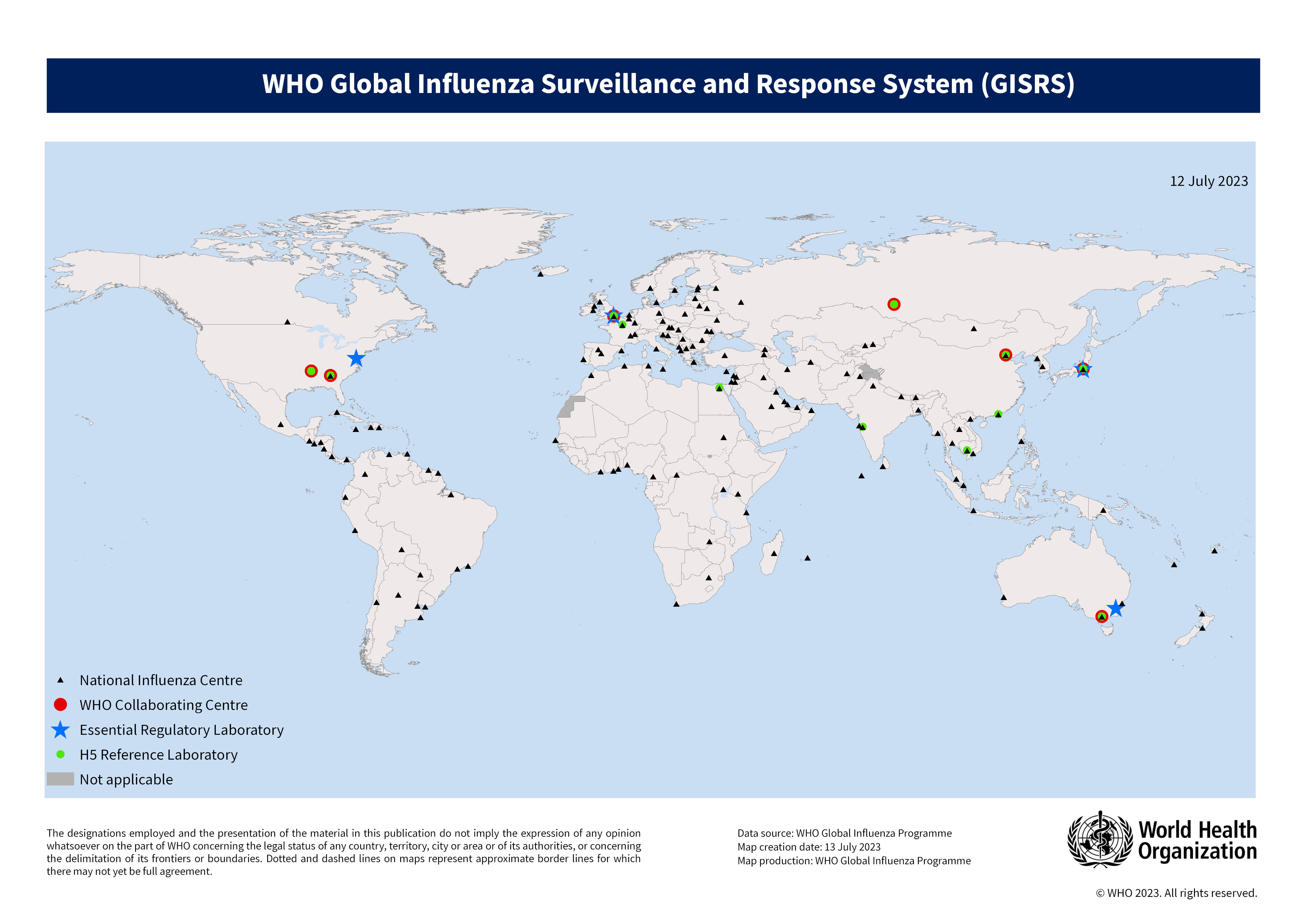
The World Health Organization (WHO) plays a critical role in global influenza surveillance, coordinating a network of national influenza centers that monitor circulating strains and recommend vaccine compositions twice a year. This surveillance data informs vaccine manufacturers and public health authorities, enabling them to tailor vaccination strategies to the specific strains prevalent in different regions.
In the Americas, the Pan American Health Organization (PAHO) works closely with national health ministries to strengthen influenza surveillance and vaccination programs. The “Day D” campaign in Curitiba is part of a broader effort to increase influenza vaccination coverage across Brazil, which has historically faced challenges in achieving high vaccination rates, particularly among vulnerable populations. The EMA (European Medicines Agency) and the FDA (Food and Drug Administration) in the US maintain rigorous standards for influenza vaccine safety and efficacy, requiring extensive clinical trials and post-market surveillance.
“The development of a truly universal influenza vaccine remains a significant challenge, but the progress we’ve made in recent years is encouraging. Targeting conserved viral proteins offers the potential to overcome the limitations of current vaccines and provide long-lasting protection against a wider range of influenza strains,”
Dr. Anthony Fauci, former Director of the National Institute of Allergy and Infectious Diseases (NIAID)
Data on Vaccine Efficacy and Strain Matching
| Influenza Season | Vaccine Effectiveness (VE) – Overall | VE – H1N1 Strain | VE – H3N2 Strain | Strain Match (WHO Recommendation) |
|---|---|---|---|---|
| 2022-2023 | 52% | 68% | 36% | Good |
| 2021-2022 | 38% | 45% | 30% | Moderate |
| 2020-2021 | 49% | 56% | 42% | Good |
Source: CDC Influenza Vaccine Effectiveness Report, 2023
Funding and Potential Biases
It’s crucial to acknowledge the funding sources behind influenza research and vaccine development. Pharmaceutical companies like Sanofi, GSK, and Seqirus are major players in the influenza vaccine market and invest heavily in research and development. While this investment is essential for innovation, it also raises potential concerns about bias in research findings. Independent research funded by government agencies like the NIH and philanthropic organizations is vital for ensuring objectivity and transparency. The WHO’s vaccine recommendations are based on scientific evidence and are subject to rigorous review by independent experts.
Contraindications & When to Consult a Doctor
Influenza vaccination is generally safe for most individuals. However, certain contraindications exist. Individuals with a severe allergic reaction to eggs (a common component of some vaccines) or any vaccine component should avoid vaccination. Guillain-Barré Syndrome (GBS), a rare neurological disorder, has been exceptionally rarely associated with influenza vaccination; individuals with a history of GBS should discuss the risks and benefits with their doctor.
Consult a doctor immediately if you experience any of the following symptoms after vaccination: difficulty breathing, hives, swelling of the face or throat, or a high fever accompanied by severe headache or stiff neck. These symptoms could indicate a severe allergic reaction or another serious medical condition.
Looking ahead, the continued development of universal influenza vaccines, coupled with enhanced global surveillance and vaccination efforts, holds the key to mitigating the impact of this persistent public health threat. The ongoing research into mRNA vaccine technology, successfully deployed during the COVID-19 pandemic, also offers promising avenues for developing more effective and rapidly adaptable influenza vaccines. The challenge lies in translating these scientific advancements into equitable access to vaccines for all populations, ensuring that the benefits of influenza prevention reach those who need them most.

