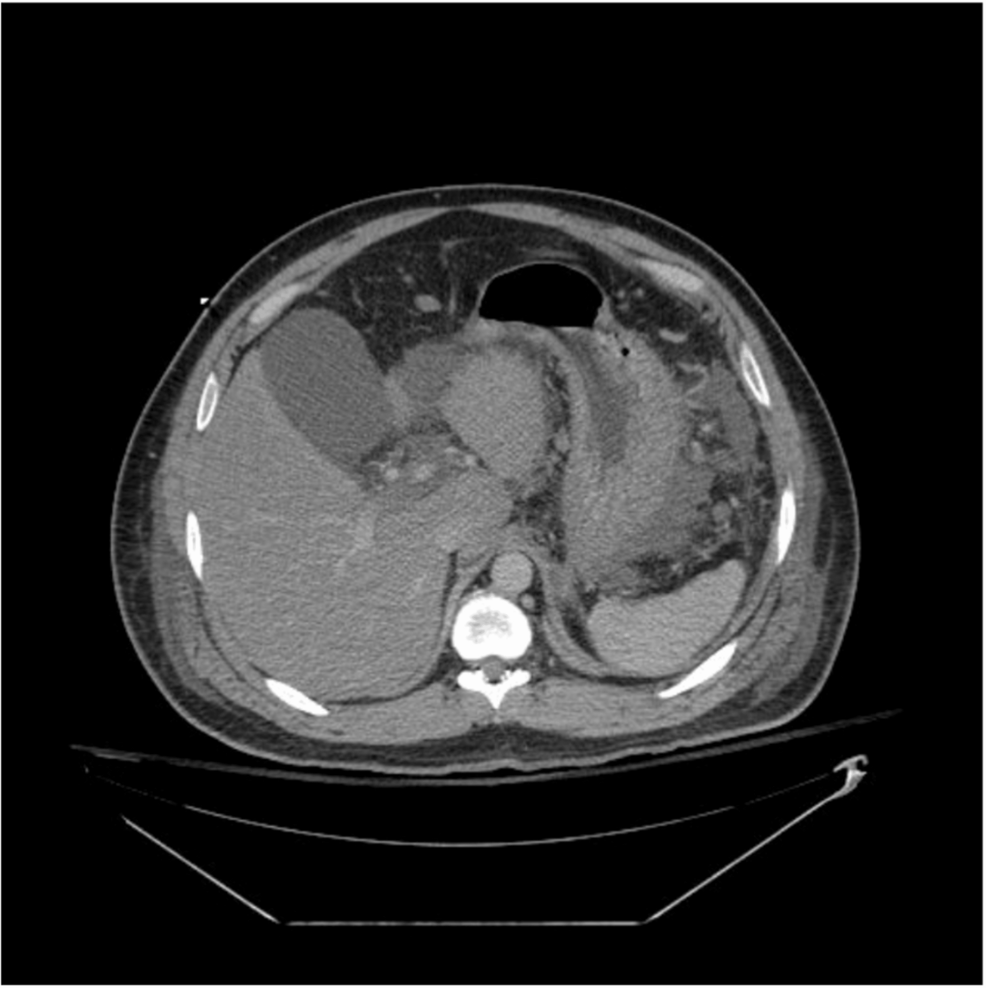
Hypertriglyceridemia-induced acute pancreatitis (HTG-AP) represents a critical metabolic emergency where excessive blood fats trigger severe pancreatic inflammation. Recent clinical case reports underscore the necessity of rapid lipid-lowering interventions to prevent tissue necrosis. Immediate medical management focuses on reducing triglyceride levels below 1000 mg/dL to halt systemic organ failure and improve survival rates.
As we navigate the health landscape of 2026, the correlation between metabolic syndrome and severe pancreatic events remains a pressing public health concern. This week’s discussion around acute necrotizing pancreatitis due to hypertriglyceridemia is not merely about a single case report. it is a sentinel warning about the rising tide of lipid disorders globally. When triglyceride levels surge, typically exceeding 1000 milligrams per deciliter, the blood becomes lipemic, creating a toxic environment for the pancreas. This condition is increasingly prevalent alongside rising rates of obesity and type 2 diabetes, demanding heightened vigilance from both clinicians and patients.
In Plain English: The Clinical Takeaway
- Threshold Alert: Triglyceride levels above 1000 mg/dL significantly increase the risk of sudden pancreatic inflammation.
- Immediate Action: Treatment often requires hospitalization to rapidly lower fat levels using insulin or plasma filtration.
- Prevention: Long-term management relies on fibrates, omega-3 fatty acids, and strict dietary carbohydrate restriction.
The Lipotoxic Cascade: Mechanism of Action
To understand the severity of this condition, one must examine the cellular mechanism known as lipotoxicity. In patients with severe hypertriglyceridemia, the capillary beds within the pancreas become overloaded with chylomicrons, which are large lipoprotein particles that transport dietary lipids. When these particles accumulate, pancreatic lipase—an enzyme meant for digestion—hydrolyzes the triglycerides into free fatty acids.
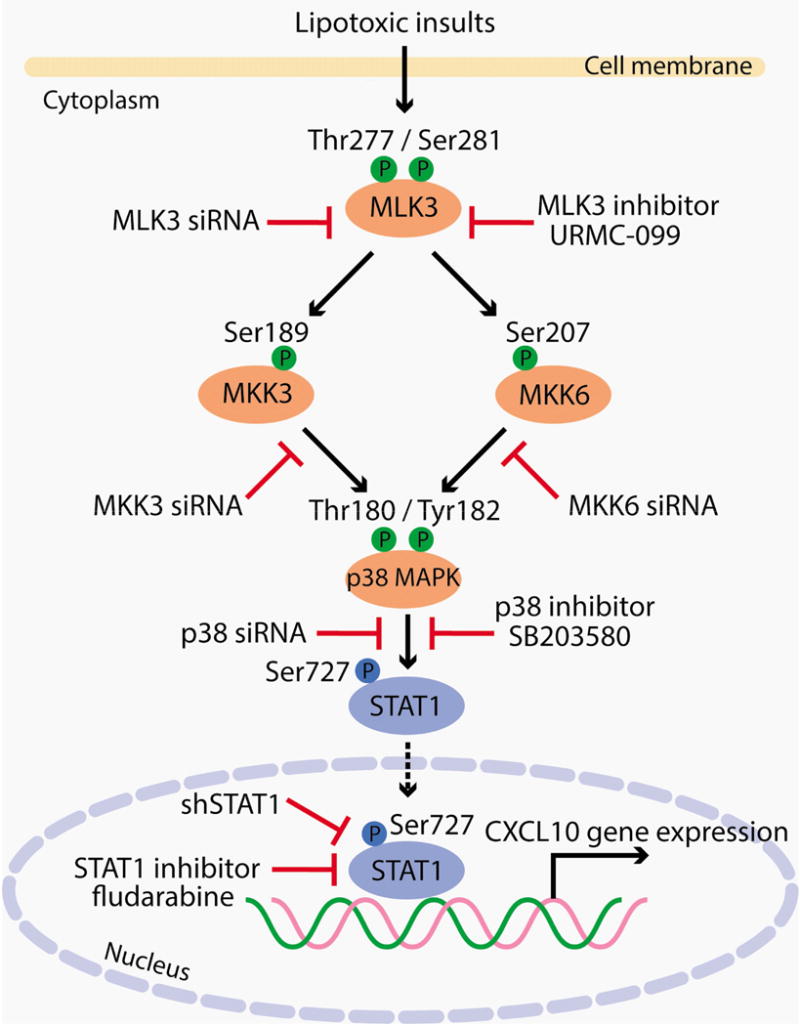
These free fatty acids are directly toxic to the acinar cells of the pancreas. This process triggers an inflammatory cascade, leading to edema, hemorrhage, and potentially necrosis, where pancreatic tissue dies. This represents distinct from gallstone pancreatitis, as the root cause is metabolic rather than mechanical obstruction. The systemic release of inflammatory cytokines can lead to multi-organ failure, affecting the lungs and kidneys. Understanding this pathway is crucial for developing targeted therapies that interrupt lipolysis before irreversible damage occurs.
Regulatory Landscape and Global Treatment Access
From a regulatory perspective, the management of HTG-AP varies by region, impacting patient access to life-saving therapies. In the United States, the Food and Drug Administration (FDA) approves fibrates and prescription omega-3 acid ethyl esters for severe hypertriglyceridemia. However, in acute settings, therapeutic plasma exchange (plasmapheresis) is often utilized off-label to mechanically remove lipids from the blood.
Conversely, the European Medicines Agency (EMA) maintains strict guidelines on lipid-lowering agents, emphasizing lifestyle modifications alongside pharmacotherapy. Disparities in access to plasmapheresis can affect outcomes in lower-resource settings where equipment availability is limited. This geo-epidemiological bridge highlights the require for standardized global protocols for HTG-AP management to ensure equitable care regardless of location.
“Early recognition of hypertriglyceridemia as the etiology of pancreatitis is vital. Delayed treatment increases the risk of local complications and systemic inflammatory response syndrome.” — American College of Gastroenterology Clinical Guidelines
Transparency regarding research funding is essential in maintaining trust. Much of the foundational data regarding HTG-AP management comes from publicly funded institutions and non-profit organizations like the National Pancreas Foundation. Unlike pharmaceutical-driven trials for chronic maintenance, acute management protocols are largely derived from observational cohorts and consensus guidelines, reducing the risk of commercial bias in emergency care recommendations.
| Intervention Strategy | Mechanism | Primary Indication | Common Side Effects |
|---|---|---|---|
| Insulin Infusion | Activates lipoprotein lipase to clear triglycerides | Acute severe hypertriglyceridemia | Hypoglycemia, hypokalemia |
| Therapeutic Plasma Exchange | Refractory cases with organ failure | Hypotension, citrate toxicity | |
| Fibrates (e.g., Fenofibrate) | Increases fatty acid oxidation | Long-term prevention | Myopathy, elevated liver enzymes |
Nutritional Integration and Myth Debunking
In the realm of wellness and nutrition, social media often propagates misinformation regarding “quick fixes” for high triglycerides. It is imperative to separate peer-reviewed fact from fiction. Although intermittent fasting shows promise in metabolic health, acute hypertriglyceridemia requires immediate medical intervention, not dietary experimentation. Long-term longitudinal studies indicate that sustained carbohydrate restriction is more effective than fat restriction alone for lowering triglyceride levels, as excess carbohydrates are converted to triglycerides in the liver via de novo lipogenesis.
Patients must avoid alcohol completely during recovery, as ethanol exacerbates lipid metabolism disorders. Over-the-counter supplements cannot replace prescription fibrates in high-risk patients. The integration of evidence-based lifestyle changes must occur under the supervision of a healthcare provider to monitor liver function and muscle health, ensuring that the cure does not become iatrogenic.
Contraindications & When to Consult a Doctor
Certain populations face higher risks and must exercise caution. Patients with a history of recurrent pancreatitis or uncontrolled diabetes should monitor lipid panels regularly. Contraindications for specific lipid-lowering therapies include severe renal impairment or active liver disease. If you experience severe epigastric pain radiating to the back, accompanied by nausea or vomiting, seek emergency care immediately. These symptoms warrant professional medical intervention to rule out necrotizing pancreatitis. Do not attempt to manage severe abdominal pain at home with over-the-counter analgesics.
The trajectory for HTG-AP management is moving towards personalized medicine, utilizing genetic profiling to identify patients prone to severe lipid metabolism errors. As we progress through 2026, the integration of rapid diagnostic tools will hopefully reduce the time from presentation to treatment. Until then, vigilance regarding metabolic health remains the best defense against this life-threatening condition.