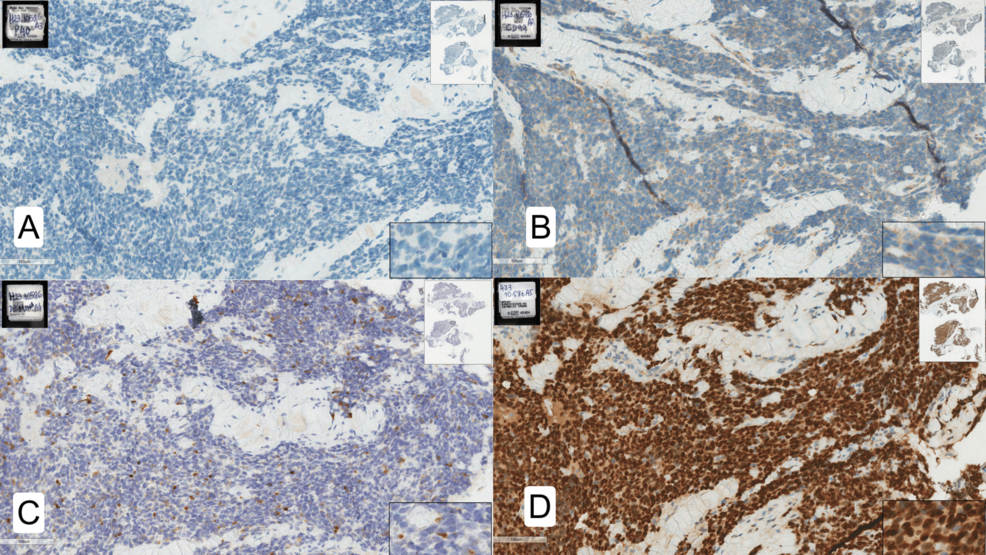
A multidisciplinary medical team successfully managed a child with severe Autism Spectrum Disorder (ASD) through 30 radiotherapy sessions using a tailored anesthetic strategy. This approach mitigated severe behavioral dysregulation and ensured precise radiation delivery, providing a clinical blueprint for treating neurodivergent pediatric oncology patients who cannot tolerate standard immobilization.
The intersection of pediatric oncology and neurodivergence presents one of the most grueling challenges in modern clinical practice. For a child with ASD, the sensory environment of a radiotherapy suite—characterized by the humming of a linear accelerator (LINAC), the restrictive nature of thermoplastic immobilization masks, and the clinical sterility of the room—can trigger profound behavioral crises. In such cases, the risk is not merely psychological distress, but clinical failure; any movement during radiation can result in “geographic miss,” where the beam strikes healthy tissue instead of the tumor, potentially compromising the curative intent of the treatment.
In Plain English: The Clinical Takeaway
- Precision through Stillness: Children with ASD may find radiation equipment terrifying; specialized anesthesia ensures they remain perfectly still so the radiation hits only the cancer.
- Customized Sedation: Not all “sleep medicine” is the same. Doctors use specific drugs that keep the child calm without suppressing their breathing too heavily.
- Team-Based Care: Success requires a “multidisciplinary” approach, meaning surgeons, anesthesiologists, and behavioral therapists work as one unit.
The Neuro-Pharmacological Balance: Managing Sedation in ASD
The primary clinical hurdle in this case was the requirement for 30 consecutive sessions of absolute immobility. Standard general anesthesia (GA) carries cumulative risks when administered repeatedly over several weeks. The medical team had to balance the “mechanism of action”—the specific way a drug affects the body—of various sedatives to avoid both under-sedation (leading to movement) and over-sedation (leading to respiratory failure).
A critical component of such strategies often involves Dexmedetomidine, a selective alpha-2 adrenergic agonist. Unlike traditional hypnotics, Dexmedetomidine provides “cooperative sedation,” meaning the patient remains calm and easily arousable but lacks the anxiety and agitation typically associated with the radiotherapy environment. This represents particularly vital for ASD patients who may experience “emergence delirium”—a state of extreme confusion and agitation upon waking from anesthesia—which is statistically more prevalent in neurodivergent populations.
To understand the pharmacological trade-offs, the following table summarizes the agents typically considered for repeated pediatric sedation:
| Anesthetic Agent | Mechanism of Action | Primary Benefit for ASD | Key Clinical Risk |
|---|---|---|---|
| Dexmedetomidine | Alpha-2 Adrenergic Agonist | Low respiratory depression; reduced agitation | Bradycardia (slow heart rate) |
| Propofol | GABA-A Receptor Agonist | Rapid onset and quick recovery | Hypotension; respiratory apnea |
| Sevoflurane | Inhalational Anesthetic | Uncomplicated titration via mask | Higher incidence of emergence delirium |
Global Access and the Multidisciplinary Gap
While this case report demonstrates a successful outcome, it highlights a significant disparity in global healthcare infrastructure. The ability to provide daily, specialized anesthesia for a month requires a high-density concentration of pediatric anesthesiologists and radiation oncologists. In the United States, access to such “high-acuity” multidisciplinary care is often dictated by insurance networks and the proximity to academic medical centers. In the United Kingdom, the NHS provides a more centralized approach, but waiting lists for pediatric radiotherapy can create windows of disease progression that complicate the anesthetic window.
the regulatory landscape regarding the off-label use of certain sedatives in children varies. While the FDA in the US and the EMA in Europe have strict guidelines, the “clinical necessity” of treating a child with a malignancy often allows for these tailored protocols. Yet, the lack of standardized, peer-reviewed guidelines for ASD-specific radiotherapy anesthesia means that most treatments remain “case-by-case,” leaving many families in rural or underserved areas without access to these life-saving modifications.
“The challenge in pediatric neurodivergence is that the ‘standard of care’ is often built for the neurotypical brain. When we treat children with ASD, the anesthetic plan is as much a part of the cure as the radiation itself.” — Dr. Elizabeth Moore, Pediatric Anesthesiology Researcher.
Funding, Bias, and Clinical Integrity
Transparency in medical reporting is paramount to avoid “publication bias,” where only successful cases are shared. This case report, published in Cureus, is a descriptive study of a single patient. Case reports are the lowest tier of evidence in the hierarchy of clinical research; they identify possibilities but do not prove universal efficacy. The research was conducted as part of standard clinical care, meaning there was no external pharmaceutical funding to bias the choice of anesthetic agents. The primary motivation was patient survival and safety, not drug promotion.
For a broader perspective on pediatric sedation, the PubMed database and the Lancet provide longitudinal data on the safety of repeated anesthesia, suggesting that while risks exist, the morbidity of untreated pediatric cancer far outweighs the risks of controlled sedation.
Contraindications & When to Consult a Doctor
Tailored anesthetic strategies are not suitable for every patient. Certain “contraindications”—medical reasons why a treatment should not be used—must be screened for before initiating a 30-session protocol:
- Cardiovascular Instability: Patients with congenital heart defects may not tolerate the bradycardia associated with alpha-2 agonists.
- Severe Obstructive Sleep Apnea (OSA): Children with severe airway obstructions are at a higher risk for post-sedation respiratory failure.
- Hepatic or Renal Impairment: Since the liver and kidneys metabolize these drugs, impairment can lead to toxic accumulation and prolonged sedation.
Immediate medical intervention is required if a child exhibits:
- Cyanosis (bluish tint to lips or skin) during or after sedation.
- Uncontrollable emergence delirium that poses a risk of self-harm.
- A sudden drop in oxygen saturation (SpO2) below 92% during the procedure.
The Future of Neuro-Inclusive Oncology
The success of this strategy suggests a shift toward “neuro-inclusive” medicine. The integration of behavioral psychology into the surgical and oncological workflow is no longer an optional luxury but a clinical necessity. As we move toward 2027, the goal is to move beyond case reports and toward randomized controlled trials (RCTs) that can establish a gold-standard protocol for ASD patients. By refining the synergy between pharmacology and behavioral support, we can ensure that a diagnosis of autism is never a barrier to receiving life-saving cancer treatment.