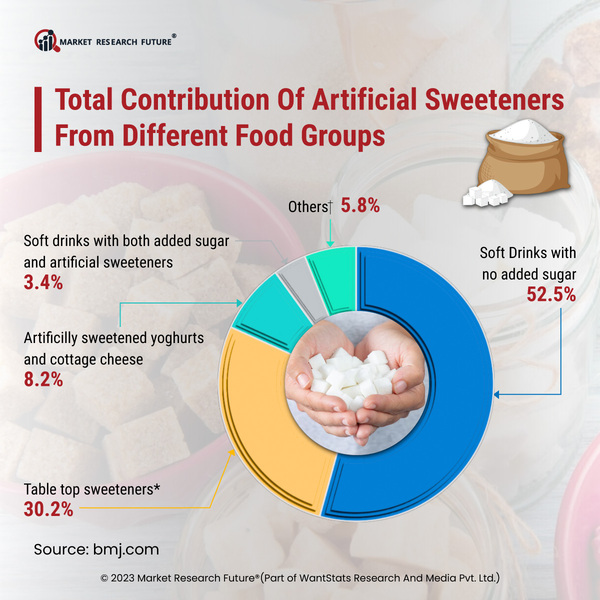
A recent study using murine models indicates that the non-nutritive sweeteners sucralose and stevia may alter gut microbiome composition and impair glucose oral tolerance, with metabolic effects potentially persisting across generations. While these findings suggest epigenetic risks, medical experts caution that rodent data cannot be directly extrapolated to human clinical outcomes.
For decades, the public health narrative has framed artificial sweeteners as a “safe harbor” for those managing obesity or Type 2 Diabetes. However, this research suggests that the interaction between synthetic sweeteners and our internal microbial ecosystem is far more complex than a simple caloric subtraction. If the consumption of these additives influences gene expression—not just in the individual, but in their offspring—we are facing a paradigm shift in how we evaluate food additives.
In Plain English: The Clinical Takeaway
- Mice, Not Men: The study found significant metabolic changes in mice; however, human biology is vastly different, and these results are not yet proven in people.
- Gut Health Matters: The sweeteners may cause “dysbiosis” (an imbalance of gut bacteria), which can change how the body processes sugar.
- Generational Caution: There is emerging evidence that metabolic “programming” could be passed to offspring, though more human longitudinal data is required.
The Microbiome-Metabolism Axis: How Sweeteners Rewrite Gut Chemistry
The core of this research centers on the gut microbiome—the trillion-strong community of bacteria residing in the intestines. The study observed that sucralose and stevia induced a state of dysbiosis, where the balance of beneficial and harmful bacteria is disrupted. This shift is critical because gut bacteria play a primary role in glucose oral tolerance (the body’s ability to clear sugar from the bloodstream after ingestion).

When the microbiome is altered, the mechanism of action involves the disruption of the intestinal barrier and the modulation of GLP-1 (glucagon-like peptide-1), a hormone essential for insulin secretion. In the study, mice consuming these sweeteners exhibited a diminished capacity to regulate blood glucose levels, mimicking early markers of insulin resistance. This suggests that while these sweeteners contain no calories, they may “trick” the metabolic system into a state of dysfunction.
From a clinical perspective, What we have is a warning about the “metabolic paradox.” By replacing sugar with sweeteners to avoid glucose spikes, users may inadvertently damage the highly biological machinery required to maintain glycemic control. This is particularly concerning for patients with pre-diabetes who rely on these substitutes to manage their HbA1c levels (a measure of average blood sugar over three months).
Epigenetic Programming: The Risk of Transgenerational Metabolic Drift
Perhaps the most provocative finding is the evidence of transgenerational inheritance. The researchers noted that the negative metabolic effects were not limited to the mice consuming the sweeteners but were as well present in their offspring. This occurs through epigenetics—the study of how environment and behavior can cause changes that affect the way your genes perform without changing the DNA sequence itself.
The study points toward changes in gene expression, specifically involving DNA methylation. This process acts like a “dimmer switch” for genes; in this case, the sweeteners may have “dimmed” the genes responsible for efficient glucose metabolism in the next generation. This suggests that our current dietary choices could potentially program the metabolic health of our children before they are even born.
“The observation that non-nutritive sweeteners can induce metabolic phenotypes in offspring is a sobering reminder that ‘zero calories’ does not mean ‘zero biological impact.’ We must move beyond the calorie-centric model of nutrition to an epigenetic one.”
This research was primarily funded by academic grants aimed at metabolic health, reducing the likelihood of industry bias often found in sweetener-funded trials. However, the transition from murine models to human application remains the primary hurdle for regulatory bodies.
Global Regulatory Divergence: FDA vs. EFSA
The implications of this study put pressure on global health authorities. In the United States, the FDA maintains the “Generally Recognized as Safe” (GRAS) status for sucralose and stevia. However, the European Food Safety Authority (EFSA) has historically been more stringent regarding the additive “Acceptable Daily Intake” (ADI).
If transgenerational risks are confirmed in humans, we may witness a shift in the UK’s NHS dietary guidelines, moving away from “sugar substitutes” and toward a holistic reduction of all sweet tastes to reset the palate and protect the microbiome.
| Marker | Control Group (Water) | Sucralose Group | Stevia Group |
|---|---|---|---|
| Gut Microbiome | Stable/Diverse | Significant Shift (Dysbiosis) | Moderate Shift |
| Glucose Tolerance | Normal | Impaired/Reduced | Slightly Impaired |
| Gene Expression | Baseline | Altered (Metabolic Genes) | Altered (Metabolic Genes) |
| Offspring Impact | None | Metabolic Dysfunction | Metabolic Dysfunction |
Contraindications & When to Consult a Doctor
While the general population does not demand to panic, certain groups should exercise heightened caution and consult a healthcare provider regarding their intake of non-nutritive sweeteners:
- Pregnant and Lactating Women: Given the transgenerational findings, those in the “first 1,000 days” of fetal and infant development should prioritize whole foods over synthetic sweeteners.
- Patients with IBD or Leaky Gut: Individuals with existing intestinal permeability may be more susceptible to the dysbiotic effects of sucralose.
- Type 2 Diabetics: If you notice that your blood glucose levels remain high despite using sweeteners, your microbiome may be impacting your insulin sensitivity.
If you experience chronic bloating, unexplained glucose fluctuations, or a sudden change in digestive regularity after switching to a high-sweetener diet, a consultation with a gastroenterologist or registered dietitian is warranted.
this study serves as a critical piece of a larger puzzle. It reminds us that the human body does not perceive “zero calories” as “nothing.” It perceives a chemical signal that triggers a biological response. Until long-term human trials can debunk or confirm these epigenetic risks, the most prudent medical advice remains a gradual reduction in the consumption of both refined sugars and their synthetic counterparts.
References
- World Health Organization (WHO) – Guidelines on Non-Sugar Sweeteners
- PubMed Central – Gut Microbiome and Metabolic Syndrome Research
- The Lancet – Longitudinal Studies on Artificial Sweeteners and Cardiometabolic Risk
- Centers for Disease Control and Prevention (CDC) – Diabetes and Metabolic Health Data