The Silent Threat: Recognizing and Addressing Bowel Cancer Symptoms
Bowel cancer, also known as colorectal cancer, is a malignancy arising from the colon or rectum. Recent reports, including personal accounts published in The Irish Times and MSN, highlight the critical importance of prompt medical evaluation for persistent gastrointestinal symptoms. Early detection, through screening programs like BowelScreen in Ireland, significantly improves treatment outcomes and survival rates. This article will delve into the clinical aspects of bowel cancer, its global impact, and the latest advancements in diagnosis and treatment.
In Plain English: The Clinical Takeaway
- Don’t Ignore Changes: Persistent changes in bowel habits, blood in your stool, or unexplained abdominal pain are *not* normal and require a doctor’s visit.
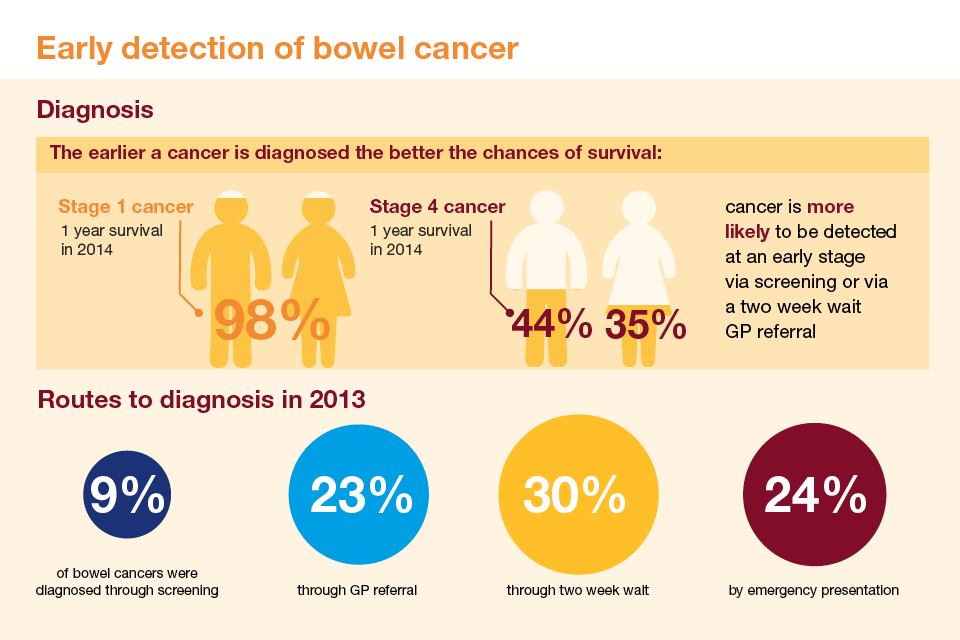
- Screening Saves Lives: Regular screening, especially for those over 50 or with a family history, can detect cancer early when it’s most treatable.
- It’s Treatable: Bowel cancer is highly treatable, particularly when caught early. Don’t let fear delay seeking medical attention.
Understanding the Pathophysiology of Colorectal Cancer
Colorectal cancer typically develops over several years. It often begins as a polyp – an abnormal growth in the colon or rectum. While not all polyps become cancerous, certain types, particularly adenomatous polyps, have a high malignant potential. The process, known as the adenoma-carcinoma sequence, involves genetic mutations that lead to uncontrolled cell growth and proliferation. The primary mechanism of action driving this progression is the accumulation of mutations in genes like APC, KRAS, and TP53, disrupting cellular signaling pathways and leading to genomic instability. These mutations can be inherited (contributing to familial cancer syndromes like Lynch syndrome and familial adenomatous polyposis) or acquired through environmental factors and lifestyle choices.

Global Epidemiology and Regional Healthcare Access
According to the World Health Organization (WHO), colorectal cancer is the third most common cancer globally, accounting for approximately 10% of all cancer cases. In 2020, there were over 1.9 million new cases and nearly 940,000 deaths worldwide. Incidence rates vary significantly by geographic region, with higher rates observed in developed countries like Australia, New Zealand, and Western Europe. This disparity is often linked to dietary factors, lifestyle habits, and access to screening programs.
Within Europe, access to colorectal cancer screening varies considerably. Countries like Germany and the Netherlands have well-established national screening programs offering fecal occult blood tests (FOBT) or colonoscopies to individuals aged 50 and over. Ireland’s BowelScreen program, highlighted in recent news, provides a similar service, but participation rates remain a concern. The European Commission is actively working to harmonize screening guidelines and improve access across member states. In the United States, the Centers for Disease Control and Prevention (CDC) recommends regular screening starting at age 45, utilizing options like colonoscopy, sigmoidoscopy, stool DNA tests (like Cologuard), and FOBT.
Funding and Bias Transparency
Much of the research into colorectal cancer diagnostics and treatment is funded by a combination of public grants (e.g., from the National Institutes of Health in the US and the Medical Research Council in the UK) and pharmaceutical companies. For example, the development of novel targeted therapies and immunotherapies has been heavily reliant on funding from companies like Bristol Myers Squibb and Merck. It is crucial to acknowledge potential biases inherent in industry-sponsored research and to critically evaluate study methodologies and results. Independent, publicly funded research remains essential for ensuring objectivity and advancing scientific understanding.
“Early detection is paramount in improving outcomes for colorectal cancer patients. We need to continue to emphasize the importance of screening and address barriers to access, particularly in underserved populations.” – Dr. Carol Burt, Epidemiologist, CDC (as stated in a 2024 CDC press briefing).
Current Treatment Modalities and Clinical Trial Data
Treatment for colorectal cancer depends on the stage of the disease, the patient’s overall health, and other factors. Common treatment modalities include surgery (resection of the tumor), chemotherapy, radiation therapy, targeted therapy, and immunotherapy.
Recent advancements in targeted therapy have shown promising results. For example, drugs targeting the KRAS G12C mutation, such as sotorasib, have demonstrated efficacy in patients with advanced colorectal cancer harboring this specific mutation. However, these therapies are often associated with side effects, and not all patients are eligible. Immunotherapy, particularly checkpoint inhibitors like pembrolizumab, has shown benefit in a subset of patients with microsatellite instability-high (MSI-H) tumors. MSI-H status indicates a deficiency in DNA mismatch repair, making cancer cells more susceptible to immune attack.
| Treatment Modality | Typical Side Effects | Estimated Efficacy (Stage III Colon Cancer) |
|---|---|---|
| Surgery | Pain, infection, bowel obstruction | 70-80% 5-year survival |
| Chemotherapy (FOLFOX) | Nausea, vomiting, fatigue, neuropathy | 60-70% 5-year survival (adjuvant) |
| Radiation Therapy | Skin irritation, fatigue, diarrhea | Variable, often used in conjunction with chemotherapy |
| Targeted Therapy (Cetuximab) | Skin rash, diarrhea, infusion reactions | Increases progression-free survival in specific cases |
Contraindications & When to Consult a Doctor
While colorectal cancer screening is generally safe, certain individuals may have contraindications. These include those with severe underlying medical conditions that increase the risk of complications from colonoscopy (e.g., severe heart disease or bleeding disorders). Individuals with a known allergy to the sedative medications used during colonoscopy should also discuss alternative screening options with their doctor.
Consult a doctor immediately if you experience any of the following symptoms:
- Persistent change in bowel habits (diarrhea, constipation, or narrowing of the stool) lasting longer than two weeks.
- Rectal bleeding or blood in your stool.
- Unexplained abdominal pain, cramping, or bloating.
- Unintentional weight loss.
- Fatigue and weakness.
The Future of Colorectal Cancer Prevention and Treatment
The future of colorectal cancer management lies in personalized medicine, utilizing genomic profiling to tailor treatment strategies to individual patients. Liquid biopsies, which analyze circulating tumor DNA in the blood, are emerging as a promising tool for early detection, monitoring treatment response, and identifying emerging resistance mechanisms. Research into the gut microbiome and its role in colorectal cancer development is gaining momentum, potentially leading to novel preventative strategies based on dietary interventions and microbiome modulation. Continued investment in research and public health initiatives is crucial for reducing the burden of this preventable and treatable disease.
References
- American Cancer Society. (2024). Colorectal Cancer. https://www.cancer.org/cancer/colon-rectal-cancer.html
- National Cancer Institute. (2023). Colorectal Cancer Treatment (PDQ®)–Health Professional Version. https://www.cancer.gov/types/colorectal/hp
- World Health Organization. (2021). Colorectal cancer. https://www.who.int/news-room/fact-sheets/detail/colorectal-cancer
- Siegel, R. L., Miller, K. D., Fuchs, H. E., & Jemal, A. (2022). Cancer statistics 2022. CA: a cancer journal for clinicians, 72(1), 7–33. https://doi.org/10.1002/caac.21708