Recent medical alerts highlight the risks of Bisphenol A (BPA) and sodium nitrite—common additives in processed foods favored by children—which act as endocrine disruptors and potential carcinogens. These substances interfere with hormonal signaling and promote cellular mutations, necessitating a shift toward additive-free diets to protect pediatric long-term health.
As a physician, I find the intersection of pediatric nutrition and chemical toxicology particularly concerning. The source material identifies a critical vulnerability: children are not merely “small adults.” Their metabolic pathways are still developing, making them significantly more susceptible to the cumulative effects of BPA and synthetic preservatives. When we discuss “carcinogenic foods,” we are not talking about an immediate diagnosis of cancer, but rather the incremental increase of statistical risk over decades of exposure.
In Plain English: The Clinical Takeaway
- BPA is a “hormone mimic”: It tricks your body into thinking it’s a natural hormone, which can disrupt growth and development in children.
- Processed meats are the primary culprits: Sodium nitrite, used to keep meats pink and “fresh,” can convert into nitrosamines, which are linked to colorectal cancers.
- Prevention is additive-free: Reducing reliance on canned goods and cured meats significantly lowers the chemical load on a child’s developing liver and kidneys.
The Molecular Mechanism: How BPA and Nitrites Trigger Cellular Dysfunction
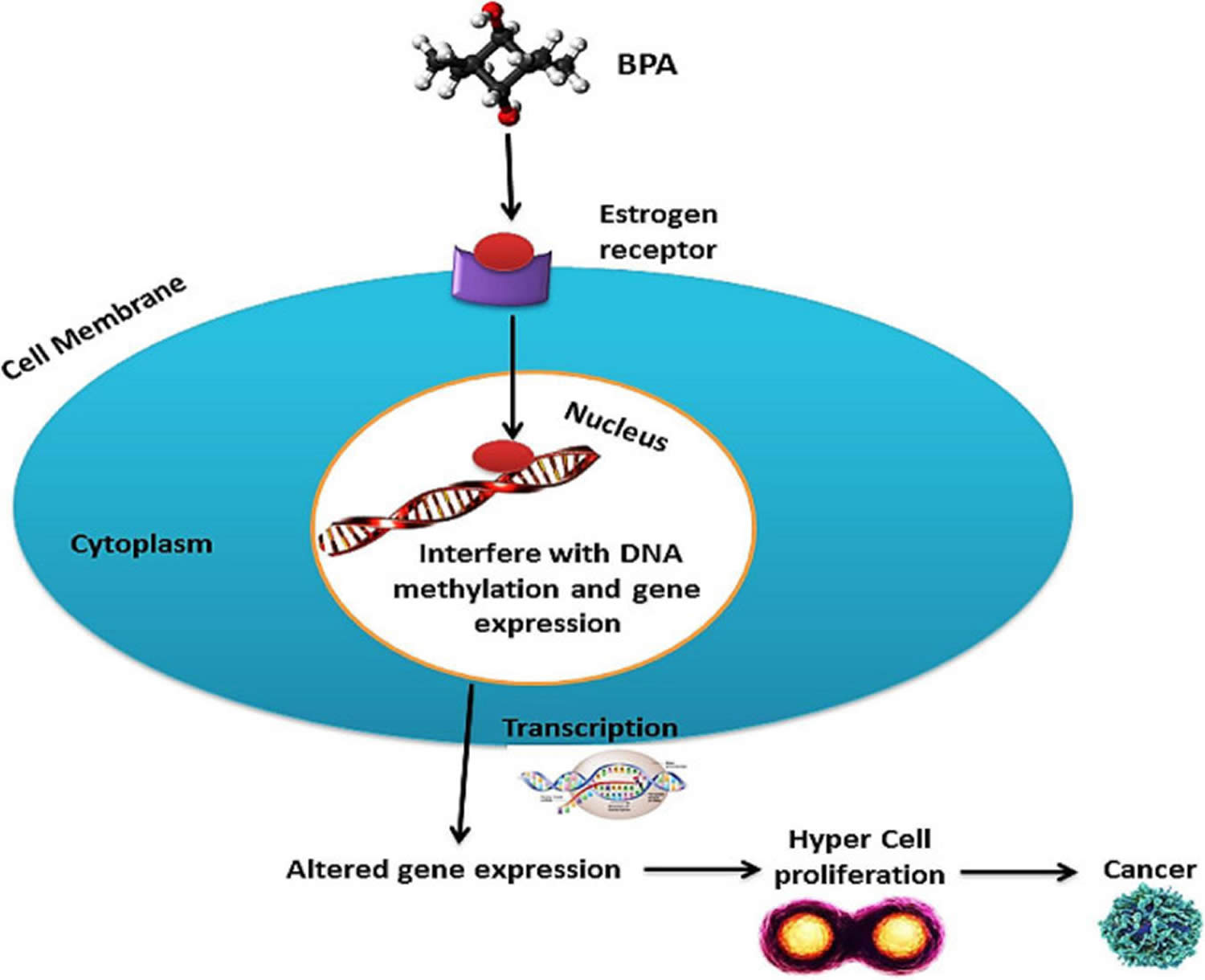
To understand why these substances are dangerous, we must examine their mechanism of action—the specific biochemical process through which a substance produces its effect. Bisphenol A (BPA) is a known xenoestrogen. So it mimics estrogen by binding to estrogen receptors (ERs) in the body, effectively “jamming” the lock and sending incorrect signals to cells.
In children, this endocrine disruption can lead to precocious puberty and metabolic dysfunction. Simultaneously, sodium nitrite, often added to processed meats to prevent botulism, undergoes a chemical reaction in the acidic environment of the stomach. This process creates nitrosamines, which are potent alkylating agents. These agents can damage DNA, leading to mutations that may eventually trigger oncogenesis, or the formation of tumors.
“The cumulative exposure to endocrine-disrupting chemicals during critical windows of development—such as infancy and childhood—can permanently reprogram metabolic and reproductive trajectories, increasing the lifelong risk of chronic disease.” — Dr. Shanna dopson, Environmental Health Specialist.
Global Regulatory Disparities: FDA vs. EFSA
The danger is compounded by a “regulatory gap” between global health authorities. While the U.S. Food and Drug Administration (FDA) maintains that current BPA levels in food are safe, the European Food Safety Authority (EFSA) has recently slashed the Tolerable Daily Intake (TDI) for BPA by several thousand times, citing new evidence of impacts on the immune system.
This means a snack deemed “safe” in the United States might be considered a public health risk in the European Union. For parents, this highlights the importance of looking beyond local regulatory labels and focusing on the ingredient list. The prevalence of these additives is often funded and pushed by the industrial food complex, where shelf-life stability is prioritized over long-term epidemiological outcomes.
| Additive | Primary Source | Biological Impact | Regulatory Status (EU/US) |
|---|---|---|---|
| BPA | Can linings, plastics | Endocrine disruption / Estrogen mimicry | Strictly limited in EU / Generally recognized as safe (GRAS) in US |
| Sodium Nitrite | Bacon, Ham, Sausages | Nitrosamine formation / DNA damage | Monitored/Limited / Widely permitted |
| Phthalates | Food packaging | Hormonal interference / Metabolic shift | Highly restricted in EU / Variable in US |
Epidemiological Trends and Funding Bias
Much of the early research defending these additives was funded by the chemical and food processing industries, creating a significant conflict of interest. Whereas, independent, peer-reviewed studies published in PubMed and The Lancet have consistently shown a correlation between high processed-meat consumption and an increased risk of colorectal cancer.

The World Health Organization (WHO)‘s International Agency for Research on Cancer (IARC) has classified processed meats as Group 1 carcinogens—the same category as tobacco. This classification is based on “sufficient evidence” that these foods cause cancer in humans. When we apply this to a child’s diet, we are essentially introducing a known carcinogen during their most vulnerable stage of growth.
Contraindications & When to Consult a Doctor
While the general population should reduce these additives, certain groups are at higher risk. Children with pre-existing endocrine disorders, such as congenital hypothyroidism or early-onset metabolic syndrome, should be strictly monitored. Individuals with a family history of colorectal cancer should exercise extreme caution with nitrite-cured meats.
Consult a pediatrician or a registered dietitian if your child exhibits signs of endocrine disruption, such as unusually early development of secondary sex characteristics or unexplained metabolic shifts. If a child has a known allergy to preservatives or exhibits severe gastrointestinal distress after consuming processed foods, a clinical dietary assessment is warranted.
The Path Toward Preventative Nutrition
The objective is not to incite panic, but to foster health literacy. The transition from processed “convenience” foods to whole, organic alternatives is the most effective clinical intervention we have for reducing chemical exposure. By opting for fresh proteins and glass-packaged goods, we bypass the primary vectors of BPA and nitrites.
As we move through 2026, the medical consensus is shifting toward a “precautionary principle.” We no longer wait for a 100% mortality rate to prove a substance is harmful. we act when the statistical probability of harm outweighs the convenience of the product. Protecting the next generation requires a commitment to evidence-based nutrition over industrial efficiency.
References
- World Health Organization (WHO) – Carcinogenicity of Processed Meats
- Centers for Disease Control and Prevention (CDC) – Environmental Health and Endocrine Disruptors
- PubMed – Longitudinal Studies on Bisphenol A and Pediatric Development
- European Food Safety Authority (EFSA) – Re-evaluation of BPA Tolerable Daily Intake