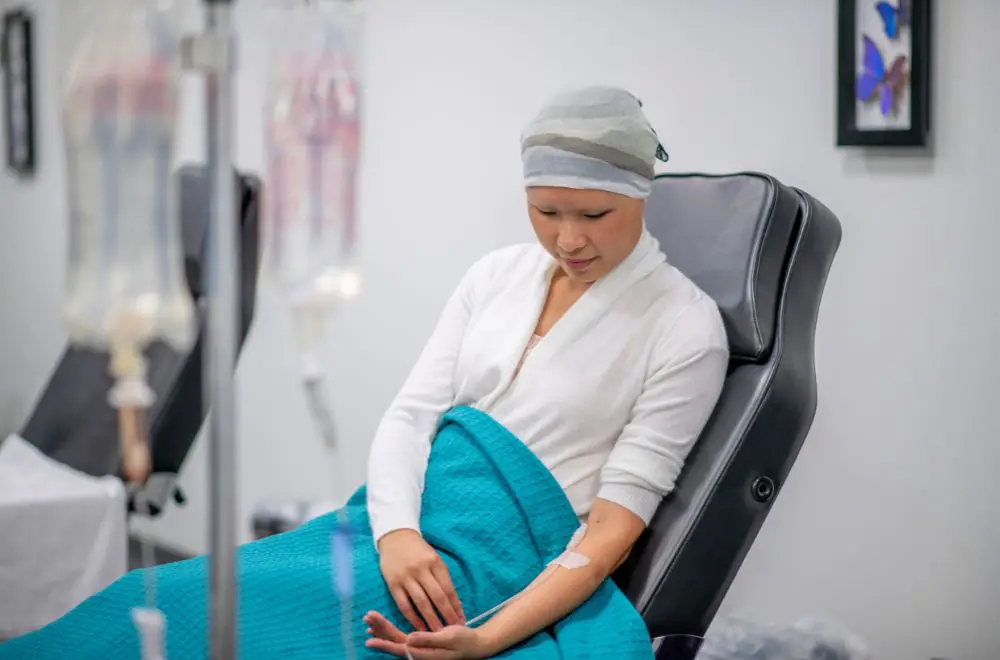
Fresh regulatory changes in Belgium are restricting transport reimbursements for cancer patients, creating systemic financial barriers to essential care. This shift increases “financial toxicity,” potentially leading to missed chemotherapy or radiotherapy sessions, which directly compromises clinical outcomes for vulnerable oncology populations across the region.
The intersection of administrative policy and clinical efficacy is where patient safety is often most vulnerable. When a healthcare system implements restrictive reimbursement rules, it does not merely change a ledger; it alters the biological trajectory of the disease. For a patient undergoing a rigorous oncology protocol, the ability to physically reach the clinic is as critical as the drug itself. The current crisis in Belgium highlights a dangerous disconnect between bureaucratic cost-saving measures and the physiological requirements of cancer treatment.
In Plain English: The Clinical Takeaway
- Financial Toxicity is Real: The stress of paying for transport is not just a money issue; it is a medical issue that can worsen a patient’s physical and mental health.
- Consistency is Key: Missing even one scheduled treatment session (non-adherence) can allow cancer cells to develop resistance to medication, making the treatment less effective.
- Advocate Early: Patients struggling with transport costs should immediately contact their hospital’s social work department to find alternative funding or emergency grants.
The Biological Cost of Treatment Non-Adherence
In oncology, the “mechanism of action”—the specific biochemical interaction through طريق which a drug produces its effect—relies heavily on precise timing. Most chemotherapy regimens are designed in cycles to maximize the killing of rapidly dividing cells while allowing healthy tissues to recover. When a patient misses an appointment due to transport costs, they experience “treatment non-adherence” (the failure to follow a prescribed medical plan).

Interrupting a chemotherapy cycle can lead to a phenomenon known as “tumor regrowth” or the selection of resistant clones. If the concentration of the drug in the bloodstream drops below the therapeutic threshold for too long, the remaining cancer cells may mutate, rendering the subsequent doses less effective. This represents particularly dangerous in aggressive malignancies where the window for curative intervention is narrow.
“Financial toxicity is not merely a socioeconomic burden; it is a clinical complication. When patients are forced to choose between transportation and basic needs, we see a measurable decline in survival rates and a sharp increase in emergency room admissions for preventable complications.” — Dr. Sarah Jenkins, Lead Epidemiologist in Health Equity.
Financial Toxicity and the Psychoneuroimmunology of Stress
The term “financial toxicity” refers to the detrimental impact that the cost of cancer care has on a patient’s quality of life and clinical outcomes. This is not just a psychological burden; it has a physiological manifestation. Chronic stress triggered by financial instability activates the Hypothalamic-Pituitary-Adrenal (HPA) axis, leading to a sustained release of cortisol.
Elevated cortisol levels are known to suppress the immune system, specifically inhibiting the activity of T-cells and Natural Killer (NK) cells. In a patient already immunocompromised by chemotherapy, this additional immunosuppression increases the risk of opportunistic infections and can hinder the body’s innate ability to fight the tumor. The “sick system” described by patients is, contributing to a biological environment that favors disease progression over recovery.
| Cost Category | Clinical Impact of Lack of Funding | Patient Outcome Risk |
|---|---|---|
| Direct Transport | Missed radiotherapy/chemotherapy sessions | Increased risk of recurrence/metastasis |
| Indirect Logistics | Delayed diagnostic imaging (CT/MRI) | Late-stage detection of complications |
| Ancillary Costs | Poor nutrition due to diverted funds | Cachexia (muscle wasting) and frailty |
Geo-Epidemiological Bridging: A Global Perspective
The Belgian crisis is a cautionary tale that echoes challenges seen in other healthcare models. In the United Kingdom, the National Health Service (NHS) provides some transport assistance, but “postcode lotteries” often dictate the level of support, leading to regional disparities in cancer survival rates. In the United States, while Medicare and Medicaid offer some non-emergency medical transportation (NEMT), the fragmented nature of private insurance often leaves “under-insured” patients in a similar predicament to those in Belgium.
The European Medicines Agency (EMA) ensures that life-saving drugs are approved and available, but the “last mile” of delivery—getting the patient to the drug—remains a national regulatory failure. Without standardized “Patient Access Protocols” that include logistics, the high-cost innovations in immunotherapy and targeted biologics are rendered useless for those who cannot afford the commute.
Research into these barriers is frequently funded by national health ministries or non-profit patient advocacy groups. However, the lack of integrated funding for “social determinants of health” (the non-medical factors that influence health outcomes) remains a systemic blind spot in Western medicine.
Contraindications & When to Consult a Doctor
While transport issues are administrative, the resulting health changes are clinical. Patients and caregivers should seek immediate medical intervention if any of the following occur due to missed appointments:
- Unexpected Weight Loss: A sudden drop in weight may indicate that the cancer is progressing due to interrupted treatment.
- New or Worsening Pain: Increased pain at the tumor site or new bone pain may suggest metastasis.
- Severe Fatigue: While common in cancer, a sudden “crash” in energy may indicate anemia or infection resulting from a gap in supportive care.
- Psychological Crisis: Severe anxiety or depression stemming from financial stress can lead to clinical depression, which requires pharmacological or therapeutic intervention.
The Path Toward Systemic Recovery
Solving the crisis of transport reimbursement requires moving beyond a “cost-per-trip” mindset to a “value-based care” model. The cost of providing a taxi or a reimbursement check is negligible compared to the cost of a patient returning to the hospital with advanced-stage complications since they missed three cycles of chemotherapy.
To prevent further clinical decline, healthcare systems must integrate social workers directly into the oncology multidisciplinary team (MDT). By identifying financial fragility at the point of diagnosis, clinicians can implement “preventative logistics,” ensuring that the biological potential of the treatment is not throttled by the poverty of the patient.