Discover the latest in health: evidence‑based wellness tips, medical breakthroughs, nutrition guidance, fitness insights, and expert advice for a healthier, happier life.
Arteriovenous malformations (AVMs) are abnormal connections between arteries and veins, and while relatively common in other areas of the body, they are exceedingly rare in the pancreas. A recent case report details the successful surgical management of a pancreatic head AVM, offering valuable insights into the diagnosis and treatment of this unusual condition. The case, highlighting the complexities of such presentations, underscores the importance of a multidisciplinary approach for optimal patient outcomes.
Pancreatic AVMs pose a diagnostic challenge due to their rarity and often nonspecific symptoms. These can include abdominal pain, gastrointestinal bleeding, and, in some cases, pancreatitis. Accurate diagnosis typically requires advanced imaging techniques, such as computed tomography (CT) angiography or magnetic resonance angiography (MRA). The increasing availability and sophistication of these imaging modalities are leading to more frequent detection of these lesions, even those that may be asymptomatic.
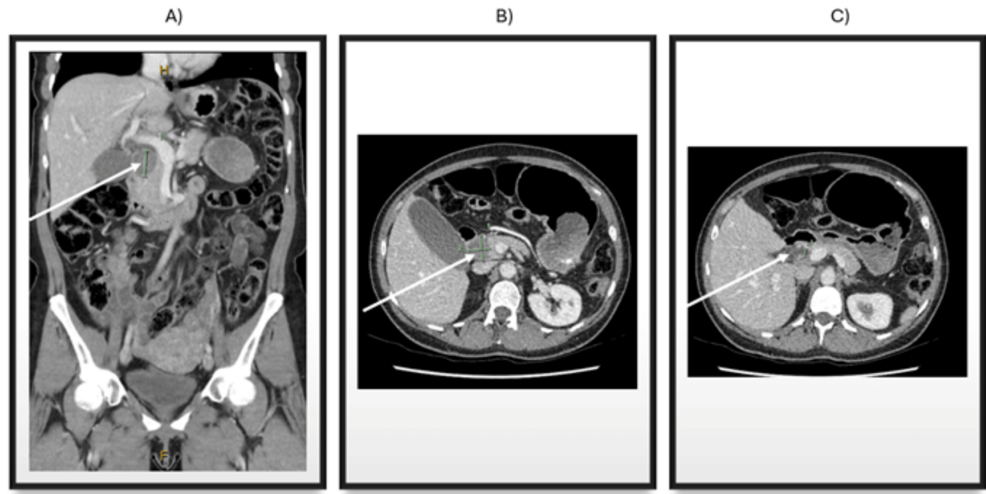
The case report, which doesn’t specify patient demographics, details a patient presenting with abdominal pain who was found to have an AVM in the head of the pancreas. Initial imaging revealed a complex network of abnormal blood vessels. Given the potential for complications like hemorrhage or thrombosis, surgical intervention was deemed necessary. The surgical team, utilizing a meticulous approach, successfully resected the AVM while preserving the surrounding pancreatic tissue and vital structures.
Understanding Pancreatic Arteriovenous Malformations
AVMs occur when there is an abnormal connection between arteries and veins, bypassing the normal capillary network. In the pancreas, these malformations are thought to be congenital, meaning they are present at birth, even though they may not become clinically apparent until later in life. The exact cause of these malformations remains unclear, but some theories suggest they may result from developmental errors during vascular formation. According to research published in PubMed, cardiac abnormalities were identified early in the epidemic of AIDS, predating the isolation of HIV, and the causation and pathogenesis of cardiovascular disease linked to HIV infection continue to be a focus of intense speculation. [1]
The clinical presentation of pancreatic AVMs can vary widely. Some patients may be asymptomatic, with the AVM discovered incidentally during imaging performed for other reasons. Others may experience more significant symptoms, such as abdominal pain, nausea, vomiting, or gastrointestinal bleeding. In rare cases, AVMs can lead to pancreatitis or even life-threatening hemorrhage. The diagnostic process often involves ruling out other potential causes of abdominal pain, such as pancreatitis, cholecystitis, or peptic ulcer disease.
Surgical Approach and Considerations
Surgical resection remains the primary treatment option for symptomatic pancreatic AVMs. The goal of surgery is to remove the AVM while preserving as much normal pancreatic tissue as possible. This can be a challenging undertaking, as the AVMs are often located in close proximity to vital structures, such as the bile duct and major blood vessels.
The surgical approach typically involves a careful dissection of the AVM from the surrounding tissues. The surgeon must meticulously control bleeding throughout the procedure, as AVMs are prone to hemorrhage. In some cases, embolization – a procedure to block the abnormal blood vessels – may be performed prior to surgery to reduce the risk of bleeding. Advances in cardiac imaging modalities and immunology have deepened our understanding of the pathogenesis of HIV-associated cardiovascular disease. [2]
Future Directions and Research
As pancreatic AVMs are rare, there is a limited amount of data available to guide treatment decisions. Further research is needed to better understand the natural history of these lesions and to identify the optimal surgical techniques. The development of less invasive treatment options, such as endovascular techniques, is also an area of ongoing investigation. The review highlights key evidence gaps in the field and suggests future directions for research to better understand the complex HIV-CVD interactions. [3]
The successful management of this case underscores the importance of a collaborative approach involving experienced surgeons, radiologists, and other specialists. Continued vigilance and a high index of suspicion are crucial for the timely diagnosis and treatment of these rare but potentially serious lesions. The increasing survival rates in HIV patients, due to advances in treatment, have led to a greater understanding of the long-term cardiac manifestations of the disease. [4]
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Have you or someone you know been affected by a rare vascular malformation? Share your experiences and thoughts in the comments below.