Meningococcal disease, a serious bacterial infection causing inflammation of the membranes surrounding the brain and spinal cord, has seen a concerning rise in incidence since 2021. The Centers for Disease Control and Prevention (CDC) recently updated its vaccine recommendations, prompting similar adjustments from the American Academy of Pediatrics and the American Academy of Family Physicians, to address this growing public health threat. This increase impacts all age groups, but particularly adolescents and young adults.
The resurgence of meningococcal disease underscores the critical importance of vaccination and heightened awareness of its symptoms. Although historically controlled through widespread immunization programs, recent data reveals a shift in circulating strains and a potential decline in immunity, necessitating a reevaluation of preventative strategies. This isn’t simply a US phenomenon; similar trends are being observed globally, demanding a coordinated international response.
In Plain English: The Clinical Takeaway
- What’s happening: Meningococcal disease, a dangerous infection, is becoming more common, especially in teens and young adults.
- Why it matters: This infection can cause serious illness, including brain damage and even death, but it’s preventable with vaccines.
- What to do: Talk to your doctor about getting vaccinated or ensuring your vaccinations are up-to-date, especially before travel or attending large gatherings.
Understanding the Meningococcal Threat: Serogroups and Pathogenesis
Meningococcal disease is caused by the bacterium Neisseria meningitidis, which exists in several serogroups, the most common being A, B, C, W, and Y. The disease manifests as meningitis (inflammation of the membranes surrounding the brain and spinal cord) or septicemia (bloodstream infection). The mechanism of action involves bacterial adhesion to the nasopharyngeal epithelium, followed by invasion of the bloodstream and subsequent crossing of the blood-brain barrier. This leads to inflammation, cerebral edema, and potentially life-threatening complications like hearing loss, neurological damage, and amputation. The inflammatory cascade is driven by the release of lipopolysaccharide (LPS) from the bacterial cell wall, triggering a cytokine storm.

The Shifting Landscape: Epidemiology and Vaccine Updates
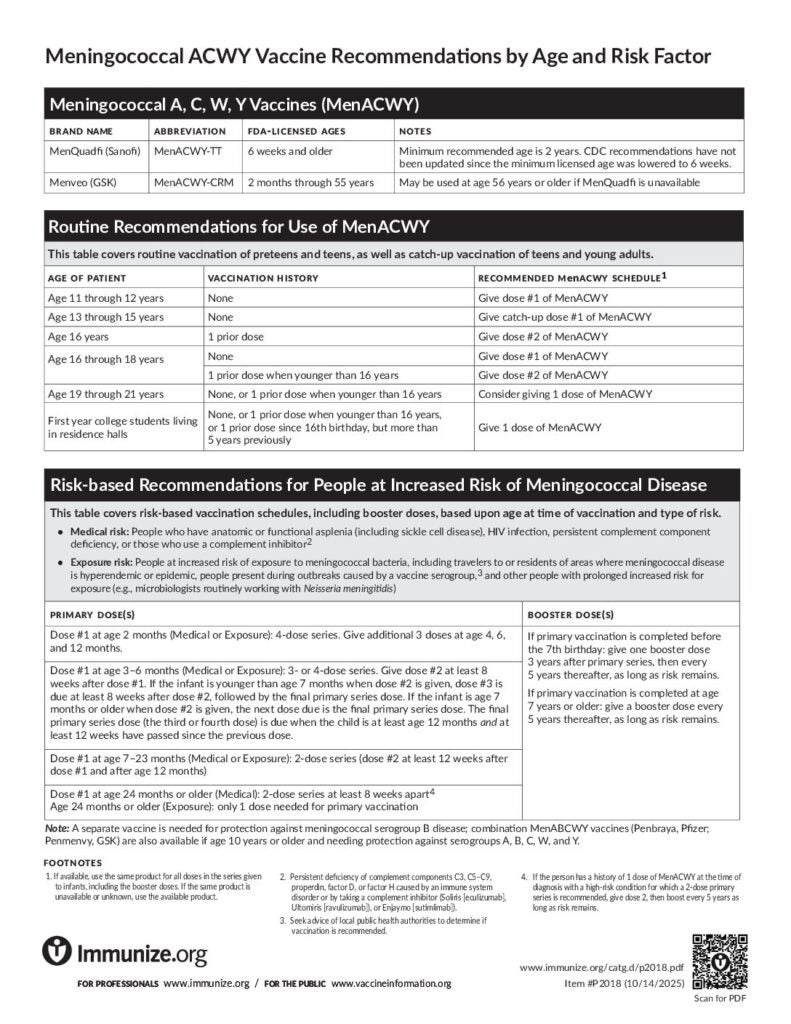
Data from the CDC indicates a significant increase in cases caused by serogroup Y, particularly in the Southeastern United States. Between 2021 and 2023, cases of serogroup Y meningococcal disease increased by 148% compared to the previous three-year period. CDC Meningitis Website This surge prompted the CDC to revise its recommendations in February of this year, now advocating for a meningococcal B vaccine (MenB) for all adolescents aged 16-18 years, and a booster dose of a serogroup A, C, W, and Y vaccine (MenACWY) at age 16. Previously, the MenACWY booster was recommended at age 11-12. The American Academy of Pediatrics swiftly followed suit with similar guidance.
The funding for the epidemiological studies informing these recommendations primarily comes from federal grants through the CDC and the National Institutes of Health (NIH). Independent research, such as that conducted by Dr. Anna Goodman at University College London, also contributes to our understanding of the disease.
“The rise in serogroup Y cases is particularly concerning because it suggests a potential waning of immunity from earlier vaccination efforts, or the emergence of new strains with altered antigenic properties,”
says Dr. Goodman. Dr. Anna Goodman Profile
Global Impact and Regional Healthcare System Responses
The increase in meningococcal disease isn’t limited to the United States. Europe, particularly the UK, has also experienced outbreaks, prompting the National Health Service (NHS) to implement enhanced surveillance and vaccination programs. UK Department of Health and Social Care The European Medicines Agency (EMA) continuously monitors vaccine safety and efficacy across the European Union. In regions with limited access to healthcare, such as sub-Saharan Africa, meningococcal disease remains a significant public health challenge, often occurring in epidemic waves. The World Health Organization (WHO) plays a crucial role in coordinating vaccination campaigns and providing technical assistance to affected countries.
| Vaccine Type | Serogroups Covered | Typical Schedule (US) | Efficacy (Phase III Trials) | Common Side Effects |
|---|---|---|---|---|
| MenACWY | A, C, W, Y | 11-12 years, Booster at 16 years | 85-95% | Pain/Redness at injection site, Mild fever |
| MenB | B | 16-18 years | 70-80% | Pain/Redness at injection site, Fatigue, Headache |
Clinical Trial Insights and Regulatory Pathways
The development of meningococcal vaccines has followed a rigorous clinical trial process. Phase I trials assess safety and immunogenicity in a small group of healthy volunteers. Phase II trials evaluate dosage and refine the vaccination schedule. Phase III trials, involving thousands of participants, demonstrate efficacy and monitor for rare adverse events. The MenACWY vaccines have been available for decades, with established safety profiles. The MenB vaccines, still, are relatively newer, and ongoing surveillance is crucial to monitor long-term efficacy and potential rare side effects. Regulatory approval in the US is granted by the Food and Drug Administration (FDA), while in Europe, it’s the EMA that oversees the process. The FDA’s Biologics Price Competition and Innovation Act (BPCIA) pathway influences the availability of biosimilar vaccines, potentially lowering costs and increasing access.
Contraindications & When to Consult a Doctor
Meningococcal vaccines are generally safe, but certain individuals should exercise caution. Those with a severe allergic reaction to a previous dose of the vaccine or to any vaccine component should not receive it. Individuals with a moderate or severe acute illness, with or without fever, should postpone vaccination until they recover. Infants younger than 9 months are at higher risk of adverse reactions. Consult a doctor immediately if you or your child develops symptoms of meningococcal disease, including high fever, severe headache, stiff neck, nausea, vomiting, sensitivity to light, and confusion.
Looking ahead, continued surveillance, research into new vaccine technologies (such as mRNA vaccines targeting multiple serogroups), and global collaboration are essential to combat the evolving threat of meningococcal disease. The recent increase in cases serves as a stark reminder that complacency can have serious consequences, and proactive public health measures are paramount to protecting vulnerable populations.