The Centers for Disease Control and Prevention (CDC) has released a “Novel Vital Signs” report detailing the escalating prevalence of arthritis in the United States. The data reveals that over 50 million adults suffer from arthritis, highlighting a critical need for improved public health interventions and systemic musculoskeletal care.
This report is not merely a statistical update. it is a clinical alarm. Arthritis is not a singular condition but a broad category of over 100 diseases affecting the joints, ranging from the degenerative wear of osteoarthritis to the autoimmune assault of rheumatoid arthritis. When millions of citizens face chronic joint inflammation, the ripple effect extends beyond physical pain to profound economic instability and a decline in global workforce productivity.
In Plain English: The Clinical Takeaway
- It is an epidemic of mobility: More than 1 in 4 U.S. Adults now live with arthritis, significantly impacting their ability to work and perform daily tasks.
- Early detection is key: Identifying joint inflammation early can prevent permanent joint destruction and long-term disability.
- Management is holistic: Treatment requires a combination of medication, physical activity, and weight management to reduce the load on joints.
The Pathophysiology of Joint Degeneration and Systemic Inflammation
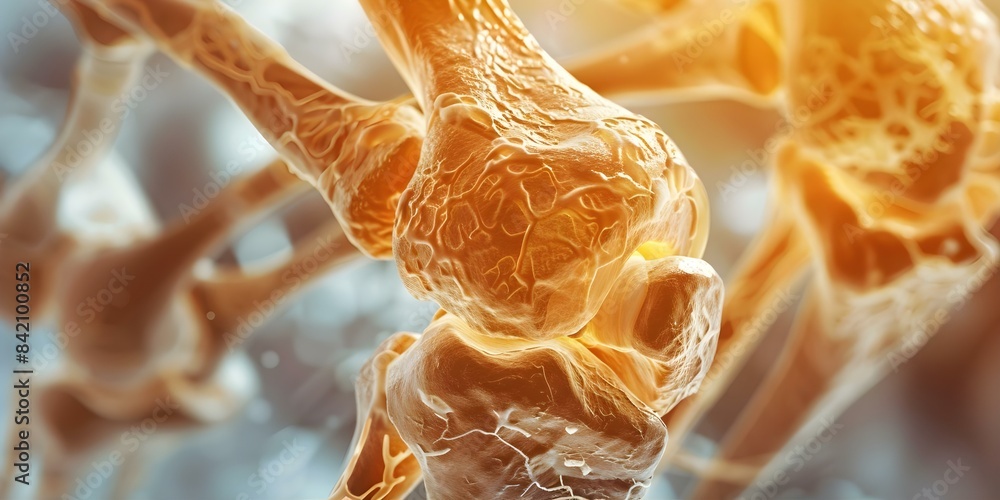
To understand the CDC’s findings, we must examine the mechanism of action—the specific biological process—of joint degradation. In osteoarthritis, the primary driver is the breakdown of articular cartilage, the smooth tissue that cushions the ends of bones. This is often a result of mechanical stress or “wear and tear.”

Conversely, autoimmune arthritis, such as rheumatoid arthritis (RA), involves a systemic immune response where the body attacks the synovium (the lining of the joint capsule). This leads to chronic inflammation, or synovitis, which can eventually erode the bone itself. The relationship between these two is critical: although one is localized and mechanical, the other is systemic and immunological.
The burden is further complicated by comorbidities. Obesity acts as a catalyst, increasing the mechanical load on weight-bearing joints and triggering the release of pro-inflammatory cytokines—signaling proteins that promote inflammation—from adipose (fat) tissue. This creates a vicious cycle where inflammation leads to inactivity, and inactivity leads to further weight gain and joint decay.
Global Healthcare Integration and the Access Gap
While the CDC focuses on the American landscape, the epidemiological trends mirror those seen globally. In the United Kingdom, the NHS faces similar pressures, where the aging population is driving a surge in demand for joint replacement surgeries. In Europe, the European Medicines Agency (EMA) continues to evaluate biologic DMARDs (Disease-Modifying Antirheumatic Drugs), which target specific parts of the immune system to stop joint destruction.
The “Information Gap” in the CDC report lies in the disparity of access. In the US, the fragmented nature of healthcare means that patients in rural areas often lack access to rheumatologists—specialists in joint diseases. This leads to a reliance on primary care providers who may not be equipped to manage complex autoimmune flare-ups, often resulting in delayed diagnoses and irreversible joint damage.
“The challenge we face is not just the prevalence of arthritis, but the gap between the onset of symptoms and the initiation of evidence-based treatment. Every month of untreated inflammation in rheumatoid arthritis increases the risk of permanent disability.”
This insight, echoed by leading epidemiologists, underscores the need for a shift from reactive treatment to proactive screening. The funding for these reports typically comes from federal appropriations via the Department of Health and Human Services (HHS), ensuring that the data remains independent of pharmaceutical influence, though the treatments themselves are developed by private industry.
Comparing the Primary Drivers of Joint Disability
To better understand the scale of the crisis, the following table summarizes the key differences between the most prevalent forms of arthritis discussed in the clinical literature.
| Feature | Osteoarthritis (OA) | Rheumatoid Arthritis (RA) | Gout (Crystalline) |
|---|---|---|---|
| Primary Cause | Cartilage wear/Mechanical stress | Autoimmune attack on synovium | Uric acid crystal deposition |
| Key Symptom | Stiffness, localized pain | Symmetrical joint swelling, fatigue | Acute, intense pain (often toe) |
| Systemic Effect | Low (Localized to joint) | High (Affects organs/blood) | Moderate (Can affect kidneys) |
| Primary Goal | Pain management & Mobility | Remission & Preventing Erosion | Lowering Serum Urate levels |
The Economic and Psychological Toll of Chronic Inflammation
The CDC’s report highlights a staggering intersection between health and economics. Arthritis is a leading cause of work disability. When we analyze this through a public health lens, we witness that the loss of productivity is not just a corporate issue but a societal one. Chronic pain often leads to clinical depression, which in turn reduces a patient’s adherence to physical therapy, creating a downward spiral of health decline.
From a clinical perspective, the use of double-blind placebo-controlled trials (the gold standard of research where neither the patient nor the doctor knows who receives the treatment) has shown that early intervention with biologics can significantly alter the trajectory of the disease. However, the cost of these “biologics” remains a barrier to entry for many, necessitating a policy shift toward more affordable specialty pharmacy access.
Contraindications & When to Consult a Doctor
While lifestyle modifications like low-impact exercise are generally recommended, certain interventions have strict contraindications (reasons why a specific treatment should not be used). For instance, patients with severe cardiovascular disease or active infections should exercise extreme caution with corticosteroids, as these can suppress the immune system or elevate blood pressure.
Make sure to seek immediate medical consultation if you experience:
- Sudden, severe swelling in a single joint accompanied by a fever (which may indicate septic arthritis, a medical emergency).
- Morning stiffness that lasts longer than 60 minutes, a hallmark sign of inflammatory arthritis.
- Unexplained weight loss or extreme fatigue coinciding with joint pain.
- Joint redness and warmth that does not subside with rest.
The Future of Musculoskeletal Health
The trajectory of arthritis management is moving toward “Precision Medicine.” Instead of a one-size-fits-all approach, clinicians are beginning to use biomarkers to predict which patients will respond to specific medications. The goal is to move from managing symptoms to achieving clinical remission.
As we move forward, the integration of digital health monitoring and a renewed focus on metabolic health—specifically the reduction of systemic inflammation through diet and exercise—will be the primary defense against the rising tide of joint disability. The CDC report serves as a necessary catalyst for this systemic change.
References
- Centers for Disease Control and Prevention (CDC) – Arthritis Data and Statistics
- PubMed – National Library of Medicine: Rheumatology and Joint Disease Pathophysiology
- The Lancet – Global Burden of Musculoskeletal Diseases
- JAMA – Clinical Guidelines for Osteoarthritis Management
- World Health Organization (WHO) – Noncommunicable Diseases and Disability

