A recent nationwide study in South Korea reveals that approximately one in three (31.7%) antibiotic prescriptions for children and adolescents are inappropriate, raising concerns about escalating antibiotic resistance and potential harm to this vulnerable population. The study, commissioned by the Korea Disease Control and Prevention Agency (KDCA), highlights particularly high rates of misuse in prophylactic antibiotic administration before surgery.
The implications of this finding extend far beyond South Korea, mirroring a global struggle against antibiotic overuse. The developing immune systems and gut microbiomes of children are particularly susceptible to the disruptive effects of unnecessary antibiotic exposure, potentially leading to long-term health consequences. This report underscores the urgent need for standardized guidelines, increased specialist access, and robust antibiotic stewardship programs tailored to pediatric care.
In Plain English: The Clinical Takeaway
- Antibiotics aren’t always the answer: Many illnesses in children, like common colds and viral infections, don’t respond to antibiotics and shouldn’t be treated with them.
- Overuse creates “superbugs”: When antibiotics are used too often, bacteria can evolve and become resistant, making infections harder to treat.
- Talk to your doctor: If your child needs antibiotics, craft sure you understand why, how long to take them, and potential side effects.
The Growing Threat of Pediatric Antibiotic Resistance
Antibiotic resistance occurs when bacteria change over time and no longer respond to drugs designed to kill them. This phenomenon, accelerated by inappropriate antibiotic utilize, poses a significant threat to global public health. Children are especially vulnerable because their immune systems are still developing, and they are more likely to experience frequent infections. The mechanism of action behind antibiotic resistance is complex, involving genetic mutations that allow bacteria to evade the drug’s effects or actively pump it out of the cell. Research published in Nature Microbiology details the various mechanisms of resistance, including enzymatic degradation of the antibiotic and alterations in the bacterial target site.
South Korea’s Findings and the Role of Prophylactic Antibiotics
The KDCA study, conducted across 20 medical institutions, revealed a particularly alarming trend in the use of prophylactic antibiotics – those administered before surgery to prevent infection. A staggering 75.1% of these prescriptions were deemed inappropriate. This often involved prescribing antibiotics for procedures where the risk of infection was low or selecting antibiotics with unnecessarily broad spectra of activity. Broad-spectrum antibiotics kill a wide range of bacteria, including beneficial ones, further disrupting the gut microbiome and increasing the risk of resistance. The study also noted a lack of dedicated pediatric infectious disease specialists and pharmacists in many hospitals, with 65.9% of surveyed institutions having only one or zero pediatric infectious disease physicians.
Global Context and Regulatory Responses
The situation in South Korea is not unique. The World Health Organization (WHO) has identified antibiotic resistance as one of the top 10 global public health threats facing humanity. The WHO estimates that antimicrobial resistance could cause 10 million annual deaths by 2050 if no action is taken. In the United States, the Centers for Disease Control and Prevention (CDC) actively promotes antibiotic stewardship programs in healthcare settings. The Food and Drug Administration (FDA) regulates antibiotic approvals and monitors resistance patterns. Similarly, the European Medicines Agency (EMA) coordinates efforts to combat antibiotic resistance across Europe. These agencies emphasize the importance of using antibiotics only when necessary, selecting the right antibiotic for the specific infection, and completing the full course of treatment as prescribed.
“The inappropriate use of antibiotics in children is a critical issue that demands immediate attention. We need to invest in training healthcare professionals, developing standardized guidelines, and educating the public about the responsible use of these life-saving drugs.” – Dr. Helen Chu, Professor of Epidemiology, University of Washington.
Funding and Potential Bias
The KDCA-commissioned study was funded by the South Korean government, specifically through the Ministry of Health and Welfare. While government funding ensures a degree of public accountability, it’s important to acknowledge that research priorities can be influenced by policy objectives. The research team at Bundang Seoul University Hospital has a strong track record in infectious disease research and is considered a reputable institution. Still, transparency regarding potential conflicts of interest is crucial in all scientific endeavors.
Data on Antibiotic Use in Pediatric Populations
| Region | Antibiotic Prescription Rate (per 1000 population) – Children (0-14 years) | Most Commonly Prescribed Antibiotic Class |
|---|---|---|
| United States | 800-1000 | Amoxicillin |
| United Kingdom | 500-700 | Penicillins |
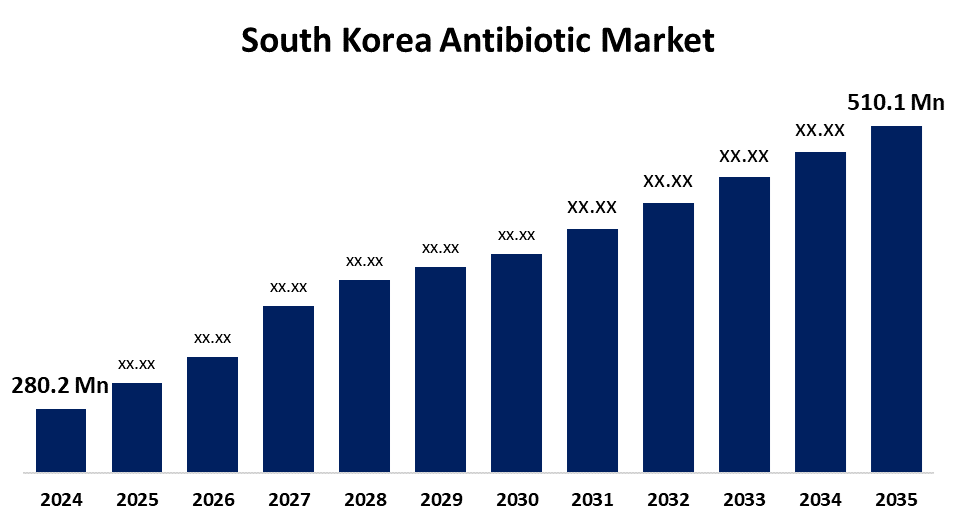
| South Korea (2026) | 650 (estimated based on KDCA report) | Cephalosporins |
| Germany | 400-500 | Penicillins |
Contraindications & When to Consult a Doctor
While antibiotics are essential for treating bacterial infections, they are not without risks. Individuals with a known allergy to penicillin or other beta-lactam antibiotics should avoid these medications. Patients with certain medical conditions, such as inflammatory bowel disease, may be more susceptible to antibiotic-associated diarrhea. It’s crucial to consult a doctor if your child experiences any of the following symptoms while taking antibiotics: severe diarrhea, vomiting, rash, difficulty breathing, or signs of an allergic reaction. Do not pressure your doctor to prescribe antibiotics for viral infections like the common cold or flu, as they are ineffective and contribute to antibiotic resistance.
The KDCA plans to address these issues by developing standardized guidelines for antibiotic use in children and adolescents, expanding the scope of surgical prophylactic antibiotic management to include pediatric patients, and strengthening antibiotic surveillance systems. These measures represent a crucial step towards safeguarding the health of future generations and preserving the effectiveness of these vital medications. The long-term success of these initiatives will depend on sustained investment, ongoing monitoring, and a collaborative effort involving healthcare professionals, policymakers, and the public.
References
- Lantibiotics and the Rise of Antibiotic Resistance – Nature Microbiology
- Antimicrobial Resistance – World Health Organization
- Antibiotic Resistance – Centers for Disease Control and Prevention
- Antibiotic Resistance – European Medicines Agency
- Antibiotic stewardship programs in pediatric hospitals: a systematic review. – Pediatric Infectious Disease Journal

