Chicago Cubs pitcher Cade Horton will undergo season-ending elbow surgery following a ligament injury. The procedure, likely a Ulnar Collateral Ligament (UCL) reconstruction, aims to restore stability to the medial elbow, a critical requirement for the high-velocity torque generated during professional pitching maneuvers.
While this news focuses on a professional athlete, the clinical implications reach far beyond the diamond. The “Tommy John” phenomenon—the surgical repair of the UCL—has become a cornerstone of sports medicine, reflecting a broader trend in orthopedic interventions for repetitive strain and ligamentous failure. For the general public, this highlights the vulnerability of connective tissues under extreme mechanical load and the evolution of graft-based regenerative medicine.
In Plain English: The Clinical Takeaway
- What happened: A critical ligament in the elbow snapped or tore, making it impossible to throw a ball with power or stability.
- The fix: Surgeons replace the damaged ligament with a healthy tendon from elsewhere in the body or a donor.
- The road back: Recovery is long (often 12-18 months) because ligaments heal much slower than muscles.
The Biomechanics of UCL Failure and the Mechanism of Action
The Ulnar Collateral Ligament (UCL) is the primary stabilizer against valgus stress—the force that pushes the forearm outward during the late cocking and early acceleration phases of a pitch. When the torque exceeds the tensile strength of the collagen fibers, a partial or complete rupture occurs.
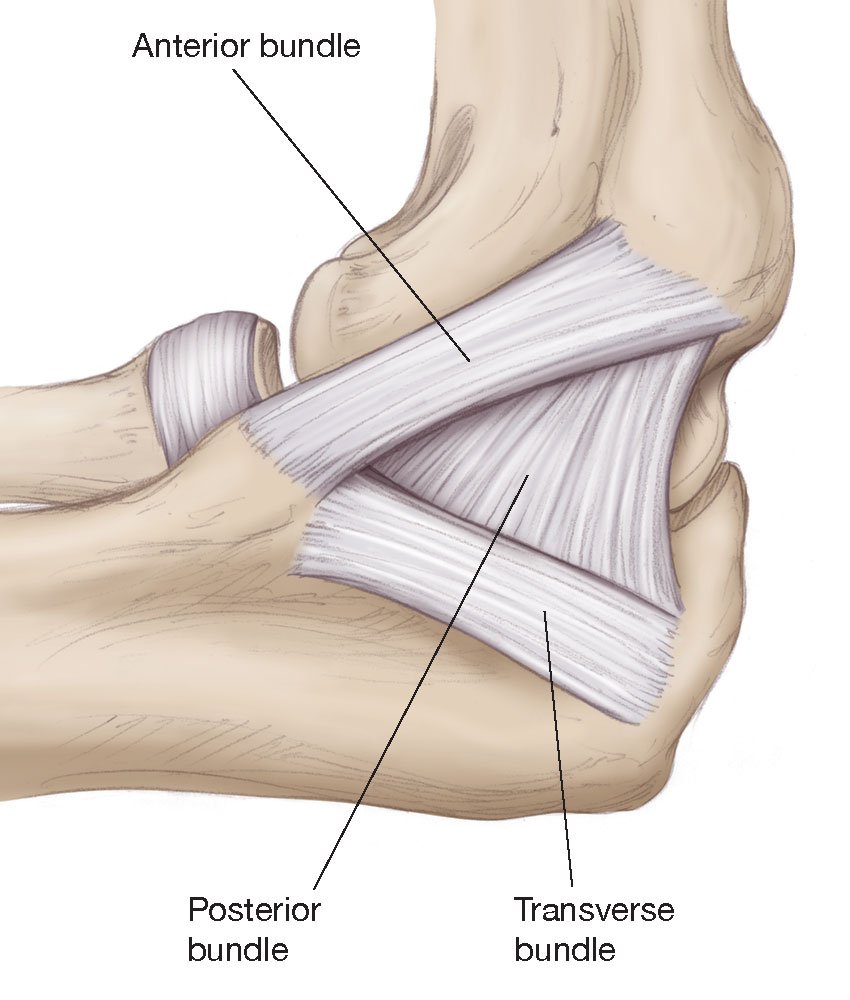
The surgical mechanism of action involves a process called “ligament reconstruction.” Unlike a simple repair, where the torn ends are sewn back together, reconstruction involves drilling tunnels into the humerus, and ulna. A graft—either an autograft (from the patient’s own palmaris longus tendon) or an allograft (from a donor)—is threaded through these tunnels to create a new, functional ligament.
This process relies on ligamentization, where the body slowly transforms the transplanted tendon into a ligament-like structure. This is a biological metamorphosis that requires strict adherence to rehabilitation protocols to avoid graft failure.
Epidemiological Trends in Ligamentous Injuries
The prevalence of UCL injuries is rising globally, not just in Major League Baseball (MLB), but among youth athletes. This shift is attributed to the “year-round” sports culture and the increased velocity of pitches at younger ages, which places immense stress on immature skeletal structures.
In the United States, the FDA has seen an increase in the approval of biological adjuncts to surgery, such as Platelet-Rich Plasma (PRP) injections, to accelerate healing. In Europe, the EMA (European Medicines Agency) maintains a cautious approach to some of these regenerative therapies, emphasizing the need for more robust, double-blind placebo-controlled trials to prove efficacy over standard physical therapy.
“The surge in UCL reconstructions among adolescent pitchers is a public health signal. We are seeing a mismatch between the mechanical demands of the modern game and the biological maturation of the adolescent elbow.” — Dr. James R. Anderson, Orthopedic Surgeon and Lead Researcher in Sports Medicine.
Research funded by the American Orthopaedic Society for Sports Medicine (AOSSM) suggests that the risk of a second UCL tear is significant, particularly if the initial biomechanical flaw—such as poor shoulder mobility or core instability—is not corrected during rehabilitation.
Comparative Recovery Outcomes: UCL Reconstruction vs. Internal Brace
Modern orthopedics is shifting toward “Internal Brace” augmentation, where a high-strength fiber tape is used to reinforce the native ligament. This differs from the traditional Tommy John surgery by preserving more of the patient’s original tissue.
| Feature | Traditional UCL Reconstruction | Internal Brace Augmentation |
|---|---|---|
| Procedure Type | Full Ligament Replacement | Ligament Reinforcement |
| Avg. Recovery Time | 12 – 18 Months | 6 – 9 Months |
| Primary Goal | Structural Replacement | Stability & Faster Return |
| Success Rate | High (80-90% return to play) | Emerging (Promising early data) |
The Global Impact on Patient Access and Healthcare Systems
The “professionalization” of this surgery has created a trickle-down effect. In the UK, the NHS typically reserves such intensive reconstructive surgeries for severe trauma or high-impact occupational needs, whereas in the US, a privatized healthcare model allows a wider range of “weekend warriors” to access these procedures via elective surgery.
This disparity creates a gap in epidemiological data. We are seeing an increase in “medical tourism” where patients travel to specialized clinics in the US to receive the latest biological grafts and PRP treatments that may not yet be standard of care in their home countries.
Contraindications & When to Consult a Doctor
UCL reconstruction is not suitable for everyone. It is contraindicated in patients with active systemic infections, severe uncontrolled diabetes (which impairs collagen synthesis), or those with advanced degenerative joint disease in the elbow.
Make sure to consult an orthopedic specialist if you experience:
- Medial Elbow Pain: Sharp pain on the inside of the elbow during gripping or throwing.
- Instability: A feeling that the elbow is “giving way” during physical activity.
- Neurological Symptoms: Numbness or tingling in the ring and pinky fingers, which may indicate ulnar nerve compression associated with ligament laxity.
The Future of Connective Tissue Regeneration
The trajectory of sports medicine is moving away from “replacement” and toward “regeneration.” Current research published in PubMed indicates that stem cell scaffolds may eventually eliminate the need for donor grafts entirely.
For athletes like Cade Horton, the focus will now shift from the operating table to the training room. The success of the surgery is only 50% of the equation; the remaining 50% is the meticulous, evidence-based restoration of the kinetic chain to ensure that the new ligament is not subjected to the same catastrophic forces that caused the initial failure.
References
- The Lancet – Orthopedic Surgery and Regenerative Medicine Trends.
- JAMA (Journal of the American Medical Association) – Longitudinal Studies on Sports-Related Ligament Injuries.
- Centers for Disease Control and Prevention (CDC) – Data on Youth Sports Injuries and Preventative Health.
- World Health Organization (WHO) – Global Standards for Surgical Safety and Rehabilitation.

