Older adults often face sexual dysfunction due to musculoskeletal stiffness and genitourinary syndrome of menopause (GSM). Addressing these challenges requires a multidisciplinary approach involving physical therapy, pelvic floor rehabilitation, and hormonal or non-hormonal therapies to restore flexibility and comfort, improving quality of life for aging couples globally.
The conversation surrounding sexual health in the seventh decade of life is frequently sidelined by clinical paternalism. When a partner expresses that they are “not flexible enough” for intimacy, This proves rarely a simple matter of agility. Instead, it is often a complex intersection of sarcopenia (age-related muscle loss), joint degeneration, and systemic endocrine shifts that affect tissue elasticity.
For patients in the UK, US, and Europe, this represents a significant gap in geriatric primary care. While the NHS and CDC provide guidelines on chronic disease management, “sexual wellness” is seldom integrated into the standard care plan for those over 70, leading many to suffer in silence or believe their condition is an inevitable part of aging.
In Plain English: The Clinical Takeaway
- Stiffness is Treatable: Physical limitations in older age are often reversible through targeted stretching and pelvic floor therapy.
- Hormones Matter: Lack of flexibility is often compounded by vaginal atrophy, which makes intimacy painful; What we have is treatable with localized estrogen.
- Communication is Clinical: Sexual dysfunction is a medical symptom, not a personal failure, and should be discussed with a healthcare provider.
The Pathophysiology of Age-Related Rigidity and Dyspareunia
The sensation of “not being flexible enough” often stems from a combination of osteoarthritis and a decrease in collagen synthesis. As we age, the synovial fluid in joints diminishes, and connective tissues lose their elasticity. When this is paired with dyspareunia—the medical term for painful sexual intercourse—the psychological response is often to avoid intimacy entirely to prevent physical distress.
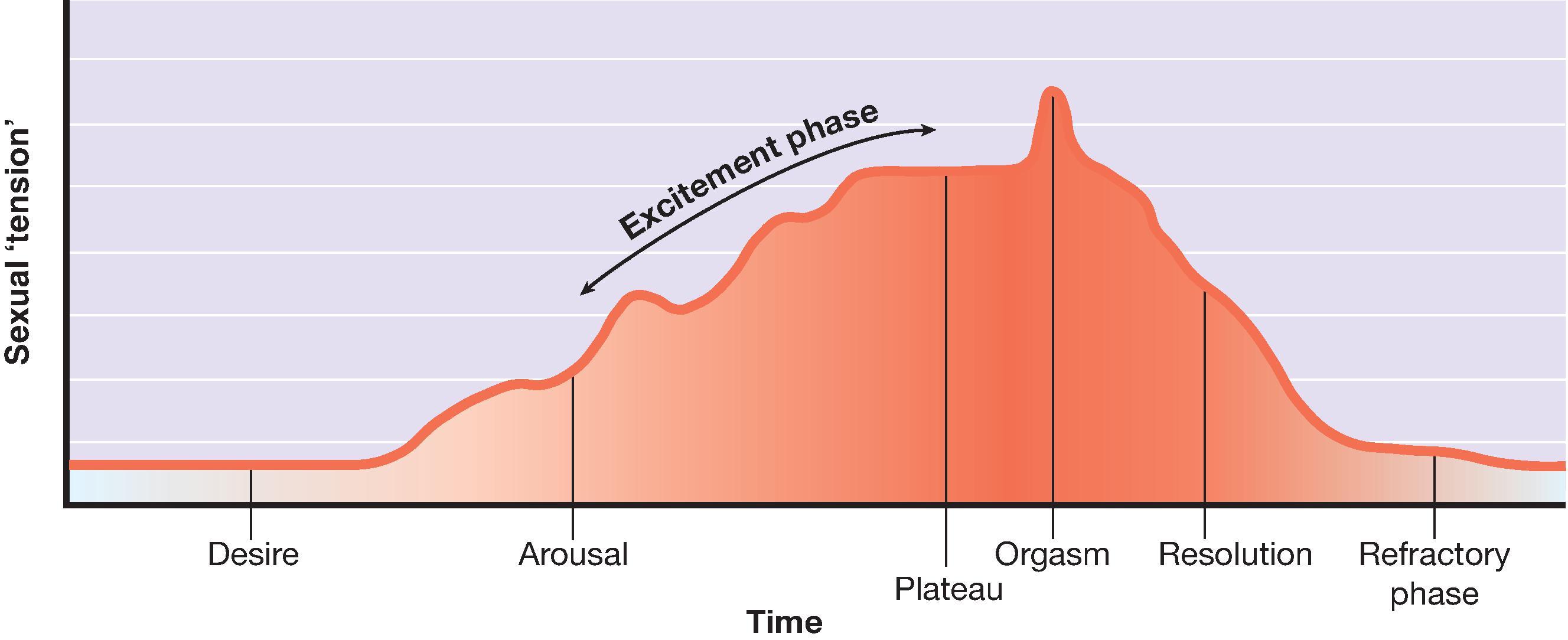
In postmenopausal women, the mechanism of action for this discomfort is primarily the decline of estrogen. This leads to the thinning of the vaginal epithelium (the lining) and a decrease in lubrication. This condition, known as Genitourinary Syndrome of Menopause (GSM), creates a cycle where the lack of lubrication increases friction, which in turn makes the patient feel “stiff” or “unflexible” due to the pain associated with movement.
To quantify the impact of these changes, consider the following clinical breakdown of common geriatric barriers to intimacy:
| Condition | Primary Physiological Cause | Clinical Impact on Intimacy | Primary Intervention |
|---|---|---|---|
| Sarcopenia | Loss of skeletal muscle mass | Reduced stability and range of motion | Resistance training / Protein intake |
| GSM | Estrogen deficiency | Vaginal dryness and tissue atrophy | Local estrogen/Non-hormonal lubricants |
| Osteoarthritis | Cartilage degradation | Joint pain during specific positions | Physical therapy / Adaptive positioning |
Bridging the Gap: From Clinical Theory to Patient Access
The approach to treating these issues varies significantly by region. In the United Kingdom, patients accessing the NHS may find that pelvic health physiotherapy is available but often has long waiting lists. In the United States, access is more immediate through private insurance, but the cost of long-term physical therapy can be a barrier for those on fixed Medicare incomes.

the European Medicines Agency (EMA) and the FDA have differing perspectives on the long-term use of vaginal estrogen. While generally considered safe for local use, there is ongoing debate regarding the risk-benefit ratio for women with a history of estrogen-dependent tumors. This necessitates a personalized “precision medicine” approach rather than a one-size-fits-all prescription.
“Sexual health is an integral part of overall health and well-being throughout the life course. The misconception that sexual desire or capability disappears with age is a barrier to providing essential care for the elderly.” — World Health Organization (WHO) Guidelines on Sexual Health.
Funding for research into geriatric sexual health has historically been lower than that for reproductive health in younger populations. Much of the current data is funded by academic institutions and non-profit health organizations, though pharmaceutical interests in “age-tech” and hormonal creams are beginning to drive more clinical trials in this demographic.
The Role of Adaptive Intimacy and Physical Rehabilitation
Addressing “flexibility” requires more than just stretching; it requires a shift in the conceptualization of sex. From a clinical perspective, the goal is to maintain the “mechanism of action” of intimacy while minimizing joint stress. This involves the use of assistive devices, such as wedges or pillows, to reduce the angle of hip flexion, thereby decreasing the load on the lumbar spine and hip joints.
Integrating a regimen of gentle yoga or Tai Chi has been shown in longitudinal studies to improve proprioception—the body’s ability to sense its position in space—which reduces the fear of injury during intimacy. When patients combine physical movement with the treatment of GSM, the perceived “stiffness” often vanishes, as the fear of pain is removed.
Contraindications & When to Consult a Doctor
While lifestyle adjustments and lubricants are generally safe, certain interventions require strict medical oversight. Patients should consult a physician immediately if they experience:
- Unexplained Vaginal Bleeding: Any post-menopausal bleeding is a red flag and requires an immediate biopsy to rule out endometrial hyperplasia or malignancy.
- Severe Joint Inflammation: If “stiffness” is accompanied by redness, warmth, or fever, it may indicate inflammatory arthritis or an infection rather than simple age-related rigidity.
- Cardiovascular Limitations: Patients with severe heart failure or unstable angina should consult a cardiologist before engaging in vigorous physical activity or starting certain hormonal therapies.
- History of Breast Cancer: Those with hormone-sensitive cancers must avoid estrogen-based therapies unless specifically cleared by an oncologist.
The trajectory for aging populations is moving toward a “whole-person” model of care. By treating sexual dysfunction not as a social awkwardness but as a clinical symptom of musculoskeletal and endocrine change, we can restore dignity and intimacy to the elderly. The key lies in the transition from passive aging to active rehabilitation.
References
- PubMed – National Library of Medicine (Research on Genitourinary Syndrome of Menopause)
- World Health Organization (WHO) – Sexual Health and Aging Frameworks
- The Lancet – Longitudinal Studies on Geriatric Musculoskeletal Health
- Journal of the American Medical Association (JAMA) – Clinical Guidelines for Postmenopausal Care

