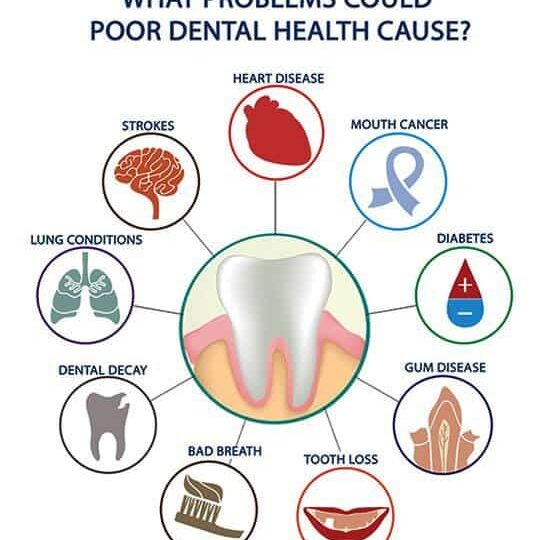
Neglected oral hygiene allows pathogenic bacteria to enter the bloodstream, triggering systemic inflammation linked to cardiovascular disease. Regular dental care mitigates this risk by preventing periodontal infection. Patients must understand the mouth-body connection to protect long-term heart health.
Recent warnings from medical authorities in Southeast Asia highlight a critical public health issue that resonates globally: the direct correlation between dental neglect and life-threatening systemic conditions. As a physician, I see patients often compartmentalize oral health from general wellness. This is a dangerous misconception. The oral cavity is not an isolated ecosystem; it is a gateway. When dental caries or periodontal disease travel untreated, the integrity of the gum tissue compromises, allowing bacteria to translocate into the circulatory system. This process, known as bacteremia, can seed distant organs, particularly the heart valves and arterial walls, exacerbating conditions like endocarditis and atherosclerosis.
The Mechanism of Oral-Systemic Translocation
To understand the risk, we must examine the mechanism of action. The primary culprit is often chronic periodontitis, a severe gum infection that damages the soft tissue and destroys the bone that supports your teeth. In this inflammatory state, the sulcular epithelium—the barrier between the gum and the tooth—becomes ulcerated. This creates an open wound roughly the size of a palm in severe cases, providing a direct entry point for oral pathogens like Porphyromonas gingivalis and Streptococcus mutans.
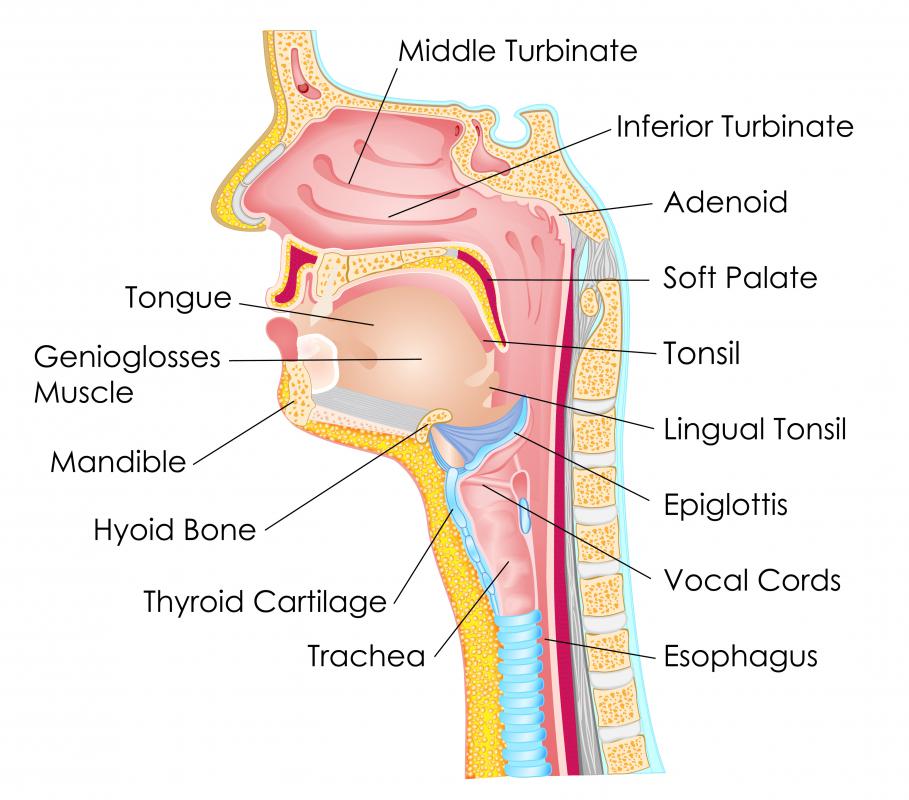
Once these bacteria enter the bloodstream, they do not merely pass through. They can adhere to damaged endothelial lining in the arteries, contributing to plaque formation. The body’s immune response to this chronic oral infection releases pro-inflammatory cytokines, such as C-reactive protein (CRP), into the systemic circulation. Elevated CRP is a well-established marker for increased cardiovascular risk. The inflammation originating in the mouth amplifies the inflammatory burden on the heart.
In Plain English: The Clinical Takeaway
- Open Wounds in the Mouth: Severe gum disease creates tiny open sores that let bacteria enter your blood during chewing or brushing.
- Heart Inflammation: These bacteria and the body’s fight against them cause swelling in blood vessels, increasing the risk of heart attacks.
- Prevention is Treatment: Regular brushing, flossing and dental checkups are not just for teeth; they are cardiovascular prevention tools.
Global Guidelines and Regulatory Perspectives
From a regulatory standpoint, the connection between oral health and systemic disease is increasingly recognized by major health bodies. In the United States, the Centers for Disease Control and Prevention (CDC) notes that nearly half of adults aged 30 or older have some form of periodontal disease. While the FDA does not regulate toothbrushes as medical devices for heart disease prevention, the American Heart Association (AHA) acknowledges the association in their scientific statements.
In Europe, the European Society of Cardiology integrates oral health assessments into broader cardiovascular risk management protocols. The NHS in the United Kingdom similarly emphasizes that poor oral health can complicate the management of diabetes and heart conditions. For patients, this means that access to dental care is not merely a cosmetic concern but a component of primary care. However, disparities in insurance coverage often limit this access, creating a geo-epidemiological gap where lower-income populations face higher risks of both dental decay and subsequent cardiac events.
Research into this field is often funded by a combination of National Institutes of Health (NIH) grants and private dental associations. It is crucial for patients to recognize that while toothpaste manufacturers may fund specific studies on plaque reduction, the broader epidemiological links are established through independent, peer-reviewed longitudinal studies. Transparency in funding ensures that recommendations are based on public health data rather than commercial product efficacy.
Regarding the scientific consensus, Dr. Thomas Van Dyke, Vice President of Applied Clinical Research at the Forsyth Institute, has previously noted the significance of this link.
“The evidence suggests that periodontal disease may be a risk factor for heart disease. We know that inflammation is a common denominator in both conditions,”
stated Dr. Van Dyke in published interviews regarding the AHA’s position. This underscores that while brushing alone may not cure heart disease, managing oral inflammation is a critical variable in the overall risk equation.
| Risk Factor | Oral Health Impact | Systemic Consequence | Prevalence Estimate |
|---|---|---|---|
| Chronic Periodontitis | Gum recession, bone loss | Elevated C-Reactive Protein | ~42% of adults >30 yrs |
| Dental Caries | Tooth decay, pulp infection | Risk of Bacteremia | ~26% of adults 20-64 yrs |
| Poor Hygiene | Plaque accumulation | Endothelial Dysfunction | Variable by region |
Contraindications & When to Consult a Doctor
While maintaining oral hygiene is universally beneficial, specific populations require heightened vigilance. Patients with prosthetic heart valves, a history of infective endocarditis, or certain congenital heart defects are at higher risk for adverse events following dental procedures that manipulate gum tissue. In these cases, antibiotic prophylaxis (preventative antibiotics) may be prescribed before dental operate to prevent bacteria from seeding the heart valves. This is a specific contraindication for standard dental cleaning without medical clearance.
Patients should consult a physician immediately if they experience persistent gum bleeding accompanied by unexplained fever, fatigue, or heart palpitations. These could be signs that an oral infection has become systemic. Individuals managing diabetes must recognize that periodontal disease can make blood sugar control more difficult, creating a bidirectional risk loop. If you notice loose teeth, persistent bad breath, or gums that pull away from teeth, seek professional dental intervention promptly.
Looking toward the future trajectory of public health, we anticipate tighter integration between medical and dental records. As value-based care models evolve, treating periodontal disease may become a metric for managing cardiovascular risk scores. Until then, the most effective tool remains mechanical plaque removal through brushing and flossing, supported by regular professional assessment.
References
- Centers for Disease Control and Prevention. Oral Health Surveillance Report.
- American Heart Association. Periodontal Disease and Atherosclerotic Vascular Disease.
- National Library of Medicine. PubMed Central: Oral-Systemic Health Links.
- National Health Service. Gum Disease Overview and Complications.
- The Forsyth Institute. Research on Oral-Systemic Connections.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment.