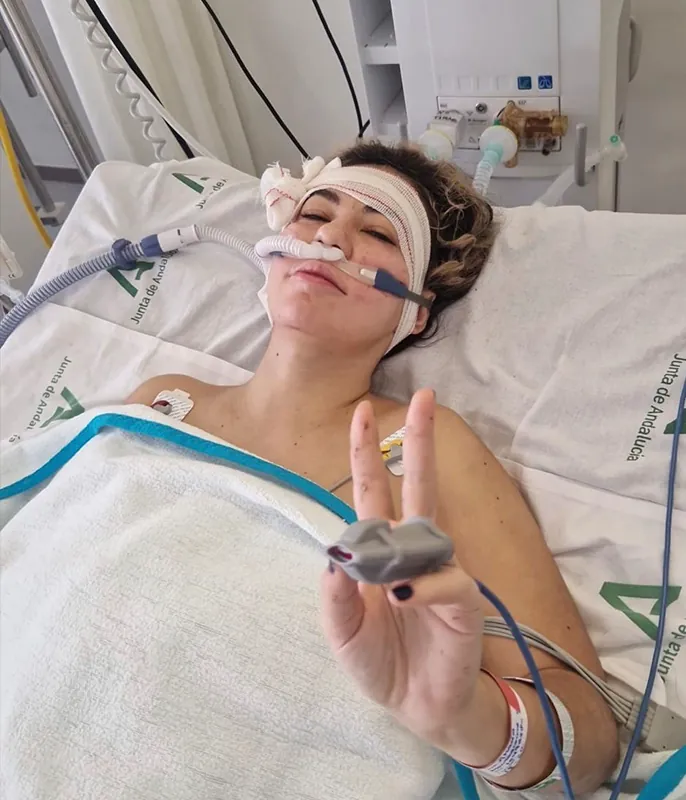
Dr. Amalia Montealegre, a 31-year-old physician, is currently recovering at home in Huelva after surviving the Alvia train crash in Adamuz. Her transition from acute hospital care to voluntary home recovery underscores the complex clinical management of polytrauma—multiple severe injuries—and the critical necessity of integrated psychological rehabilitation.
The case of Dr. Montealegre is more than a narrative of survival; It’s a clinical case study in the “survivor’s paradox.” For medical professionals, the transition from clinician to patient often introduces a unique psychological burden. When a physician possesses an intimate understanding of the pathology and potential complications of their own injuries, the recovery process can be fraught with heightened anxiety and a tendency toward self-diagnosis, which can complicate the therapeutic alliance between the patient and the treating team.
In Plain English: The Clinical Takeaway
- Polytrauma Recovery: Healing from a high-velocity accident requires a phased approach, moving from “damage control” (stopping bleeding and stabilizing organs) to long-term functional rehabilitation.
- The Mental-Physical Link: Physical wounds often heal faster than the neurological impact of trauma. Psychological support is not “optional” but a clinical requirement for full recovery.
- Voluntary Discharge: Requesting to move home (voluntary discharge) is possible only when the patient is hemodynamically stable and has a verified support system to manage medication and physical therapy.
The Pathophysiology of High-Velocity Deceleration Injuries
In accidents like the Alvia crash, the body undergoes rapid deceleration. This creates “shear forces” where internal organs continue moving forward while the skeletal frame stops abruptly. This mechanism of action—the way the injury is produced—often results in blunt force trauma to the thoracic and abdominal cavities.

Clinically, this often leads to the Coagulopathy of Trauma, a state where the blood’s ability to clot is severely impaired due to a combination of hemorrhage, acidosis, and hypothermia. To combat this, modern trauma centers utilize “Damage Control Surgery” (DCS). Instead of attempting a definitive, hours-long repair of all injuries, surgeons perform rapid, life-saving interventions to stop bleeding and contain contamination, leaving the final reconstruction for a later date when the patient’s physiology has stabilized.
For survivors like Dr. Montealegre, the subsequent phase involves managing the systemic inflammatory response syndrome (SIRS), where the body’s immune system overreacts to the widespread tissue damage. This requires a precise balance of corticosteroids and nutritional support to prevent multi-organ dysfunction syndrome (MODS).
Bridging the Gap: European Trauma Protocols vs. Global Standards
The management of Dr. Montealegre within the Spanish National Health System (SNS) reflects the European Medicines Agency (EMA) and European Society for Trauma and Emergency Surgery (ESTES) guidelines. Spain’s decentralized healthcare model allows for rapid stabilization in regional centers followed by transfer to specialized tertiary hospitals.
Compared to the American College of Surgeons’ (ACS) ATLS (Advanced Trauma Life Support) model used in the US, the European approach often emphasizes a more integrated, long-term social-medical recovery phase. This is evident in the ability of patients to transition to home-based recovery in provinces like Huelva, provided there is a coordinated “bridge” of care between the hospital and local primary care physicians.
“The success of polytrauma recovery is not measured by the survival of the initial impact, but by the patient’s return to a baseline of functional independence and psychological equilibrium,” states Dr. Marcus Thorne, a lead researcher in trauma epidemiology.
Funding for the protocols governing these recoveries is largely public, driven by government health budgets in the EU, which reduces the “financial toxicity” often seen in US trauma cases, where the cost of ICU stays can lead to secondary psychological stress for the survivor.
Clinical Progression: Acute Stabilization to Rehabilitation
The following table summarizes the clinical markers monitored during the transition from the ICU to home recovery for polytrauma survivors.
| Clinical Phase | Primary Physiological Goal | Key Biomarkers/Metrics | Primary Risk Factor |
|---|---|---|---|
| Acute (0-72 Hours) | Hemodynamic Stability | Lactate levels, MAP (Mean Arterial Pressure) | Hemorrhagic Shock |
| Intermediate (Days-Weeks) | Tissue Regeneration | CRP (C-Reactive Protein), WBC Count | Sepsis / Nosocomial Infection |
| Rehabilitative (Weeks-Months) | Functional Recovery | FIM (Functional Independence Measure) | PTSD / Muscle Atrophy |
The Neurobiology of Trauma and PTSD in Medical Professionals
Beyond the physical fractures, the Alvia crash triggers a cascade in the Hypothalamic-Pituitary-Adrenal (HPA) axis. This is the body’s central stress response system. In survivors, a hyper-active HPA axis can lead to Post-Traumatic Stress Disorder (PTSD), characterized by intrusive memories and hyper-vigilance.
For a physician, this is compounded by “clinical introspection.” They may subconsciously monitor their own symptoms for signs of pulmonary embolism—a common complication of long-term immobilization—which can lead to a state of chronic anxiety. Evidence-based treatment now favors Trauma-Focused Cognitive Behavioral Therapy (TF-CBT) and, in some cases, pharmacological intervention using SSRIs (Selective Serotonin Reuptake Inhibitors) to modulate serotonin levels in the synaptic cleft, reducing the intensity of the fear response.
Contraindications & When to Consult a Doctor
While home recovery is the goal, certain “red flags” indicate that a trauma survivor’s condition has deviated from the expected recovery trajectory. Immediate medical intervention is required if any of the following occur:
- Respiratory Distress: Sudden shortness of breath or chest pain, which may indicate a pulmonary embolism (a blood clot that has traveled to the lungs).
- Neurological Shifts: Sudden confusion, extreme lethargy, or a decrease in consciousness, suggesting potential delayed intracranial pressure or metabolic imbalance.
- Infection Signs: High fever (above 38.5°C) or purulent discharge from surgical sites, indicating a secondary bacterial infection.
- Acute Psychological Crisis: Severe insomnia, suicidal ideation, or complete social withdrawal, necessitating urgent psychiatric triage.
The recovery of Dr. Amalia Montealegre serves as a reminder that the “cure” for catastrophic injury is not found in the operating theater alone. It is a longitudinal process requiring the seamless integration of surgical precision, pharmacological stability, and psychological fortitude. As we move toward more personalized medicine, the focus will likely shift toward biomarkers that can predict which survivors are most at risk for long-term PTSD, allowing for preemptive intervention.
References
- PubMed: Clinical Management of Polytrauma and Damage Control Surgery
- The Lancet: Long-term Outcomes of High-Velocity Impact Survivors
- World Health Organization (WHO): Guidelines on Mental Health in the Aftermath of Disaster
- JAMA: The Impact of Professional Medical Knowledge on Patient Recovery Trajectories