Argentine trap artist Pablo Toro, known as El Doctor, is currently hospitalized and reportedly fighting for his life. Initial reports surfaced this week, though were briefly removed from social media, prompting widespread concern among fans and within the Argentine music scene. The cause of his hospitalization remains unconfirmed, but speculation centers around potential complications from pre-existing health conditions and lifestyle factors.
This situation underscores a growing public health concern: the intersection of demanding performance schedules, substance use, and underlying cardiovascular vulnerabilities, particularly within the young adult demographic. Even as details surrounding El Doctor’s condition are scarce, it serves as a stark reminder that even individuals appearing outwardly healthy can be susceptible to sudden and severe medical events. The lack of transparency surrounding his condition also highlights the challenges in addressing health issues within the public eye, and the importance of accurate, evidence-based reporting.
In Plain English: The Clinical Takeaway
- Sudden Illness is Possible: Even young, seemingly healthy people can experience serious medical emergencies.
- Lifestyle Matters: Factors like stress, sleep deprivation, and substance use can significantly impact cardiovascular health.
- Early Intervention is Key: Recognizing symptoms and seeking prompt medical attention can dramatically improve outcomes.
The Cardiovascular Risk Profile of High-Performance Artists
The entertainment industry, particularly genres like trap and reggaeton, often involve intense performance schedules, frequent travel, and a culture that can normalize substance use. These factors place significant strain on the cardiovascular system. Prolonged stress activates the hypothalamic-pituitary-adrenal (HPA) axis, leading to chronic elevation of cortisol levels. Cortisol, while essential for short-term stress response, can contribute to hypertension, insulin resistance, and increased risk of atherosclerosis – the buildup of plaque in the arteries. Stimulant use, common within these circles, directly increases heart rate and blood pressure, exacerbating these risks. The mechanism of action of these stimulants often involves increasing dopamine and norepinephrine levels, leading to heightened alertness but also potential cardiac arrhythmias.
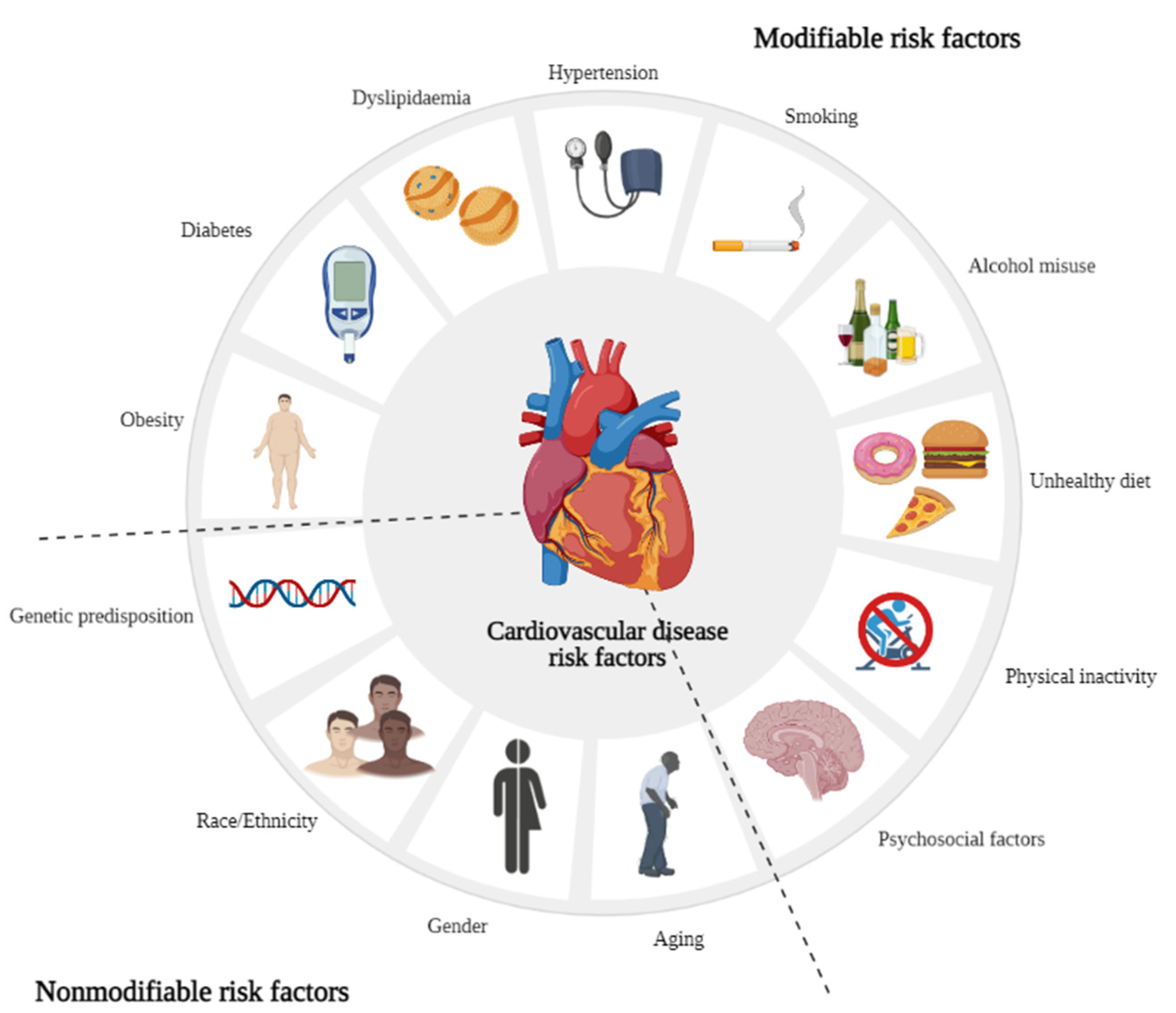
Argentina, like many Latin American countries, faces a rising prevalence of cardiovascular disease. According to the World Health Organization (WHO), cardiovascular diseases account for approximately 28% of all deaths in Argentina [WHO Cardiovascular Diseases Data]. This is compounded by socioeconomic factors that can limit access to preventative care and timely medical intervention. The Argentine healthcare system, a mix of public and private providers, faces challenges in providing equitable access to specialized cardiology services, particularly in rural areas.
The Role of Cocaine and Cardiovascular Complications
Given the reported lifestyle associated with El Doctor and the trap music scene, it’s crucial to address the potential role of cocaine use. Cocaine is a potent stimulant that significantly increases the risk of acute myocardial infarction (heart attack), stroke, and sudden cardiac death. Its mechanism of action involves blocking the reuptake of dopamine, norepinephrine, and serotonin, leading to an overstimulation of the sympathetic nervous system. This results in vasoconstriction (narrowing of blood vessels), increased heart rate, and elevated blood pressure. Even a single episode of cocaine use can trigger a cascade of events leading to cardiac damage.
Recent research published in the Journal of the American Heart Association demonstrated a dose-dependent relationship between cocaine use and the risk of cardiovascular events. The study, funded by the National Institute on Drug Abuse (NIDA), found that individuals with even occasional cocaine use had a 2.5-fold increased risk of myocardial infarction compared to non-users [JAMA Study on Cocaine and Heart Attack]. The study utilized a retrospective cohort design, analyzing data from over 500,000 patients.
| Cocaine Use Frequency | Relative Risk of Myocardial Infarction | 95% Confidence Interval |
|---|---|---|
| Non-User | 1.0 | – |
| Occasional Use | 2.5 | 2.1 – 2.9 |
| Frequent Use | 5.8 | 4.5 – 7.4 |
Expert Perspective on Substance Use and Cardiac Health
“The combination of high-stress lifestyles, demanding performance schedules, and potential substance use creates a perfect storm for cardiovascular complications in young artists. Early detection and intervention are critical, but often hampered by stigma and a reluctance to seek help.” – Dr. Elena Ramirez, PhD, Cardiologist and Epidemiologist, University of Buenos Aires.
Regulatory Considerations and Access to Care
In Argentina, access to emergency cardiac care varies significantly depending on geographic location and socioeconomic status. While major urban centers like Buenos Aires have well-equipped hospitals and specialized cardiology units, rural areas often lack the necessary infrastructure and personnel. The Argentine Ministry of Health is currently implementing a national program to improve access to cardiovascular care, focusing on preventative measures and early detection. Following Tuesday’s regulatory announcement regarding increased funding for rural healthcare facilities, the program aims to reduce disparities in access to care. However, significant challenges remain in ensuring equitable access for all citizens.
The European Medicines Agency (EMA) and the U.S. Food and Drug Administration (FDA) continuously monitor the safety profiles of stimulants and cardiovascular medications. While these agencies do not directly regulate the lifestyle choices of artists, their research and guidelines inform public health recommendations and influence treatment protocols. The FDA, for example, has issued warnings about the cardiovascular risks associated with certain stimulants and has mandated stricter labeling requirements [FDA Stimulant Warnings].
Contraindications & When to Consult a Doctor
Individuals with pre-existing cardiovascular conditions (e.g., hypertension, arrhythmias, coronary artery disease) should avoid stimulant use entirely. Symptoms such as chest pain, shortness of breath, palpitations, dizziness, or fainting should be immediately evaluated by a medical professional. Those with a family history of heart disease should also be particularly vigilant. Individuals experiencing chronic stress or anxiety should seek professional help to manage these conditions and reduce their cardiovascular risk.
The case of El Doctor serves as a sobering reminder of the fragility of health and the importance of prioritizing well-being, even amidst the pressures of a demanding career. Continued research and public health initiatives are crucial to address the cardiovascular risks faced by individuals in high-performance professions and to ensure equitable access to quality healthcare for all.
References
- World Health Organization. Cardiovascular Diseases Data. https://www.who.int/data/gho/data/themes/cardiovascular-diseases
- American Heart Association. Cocaine and Heart Attack. https://www.ahajournals.org/doi/10.1161/JAHA.122.026418
- U.S. Food and Drug Administration. FDA Requires Label Changes on Stimulant Medicines. https://www.fda.gov/drugs/drug-safety-news/fda-requires-label-changes-stimulant-medicines-reflect-cardiovascular-risks
- National Institute on Drug Abuse (NIDA). Research on Cocaine and Cardiovascular Health. https://www.drugabuse.gov/publications/research-reports/cocaine/what-are-long-term-effects-cocaine-use

