France is launching its first AI-augmented pilot hospital under the France 2030 initiative. This sovereign infrastructure project integrates artificial intelligence into clinical workflows to enhance diagnostic precision, optimize patient triage and secure health data, marking a strategic shift toward autonomous, high-tech public healthcare delivery across the European Union.
The transition from traditional digitized records to an “augmented” hospital represents a fundamental shift in the mechanism of action—the specific process by which a system produces an effect—of healthcare delivery. For decades, hospitals have stored data; they have rarely used that data in real-time to predict patient deterioration. By deploying a sovereign cloud—a data infrastructure owned and operated within national borders to ensure strict privacy and security—France is attempting to solve the tension between the hunger for “Big Data” in machine learning and the absolute necessity of patient confidentiality.
In Plain English: The Clinical Takeaway
- Faster Triage: AI helps doctors identify the sickest patients more quickly, reducing wait times in emergency departments.
- Precision Diagnosis: AI acts as a “second set of eyes” for radiologists and pathologists, catching tiny anomalies that humans might miss.
- Data Privacy: Because the system is “sovereign,” your medical data stays in France and is not shared with foreign tech giants.
The Architecture of Clinical Decision Support Systems
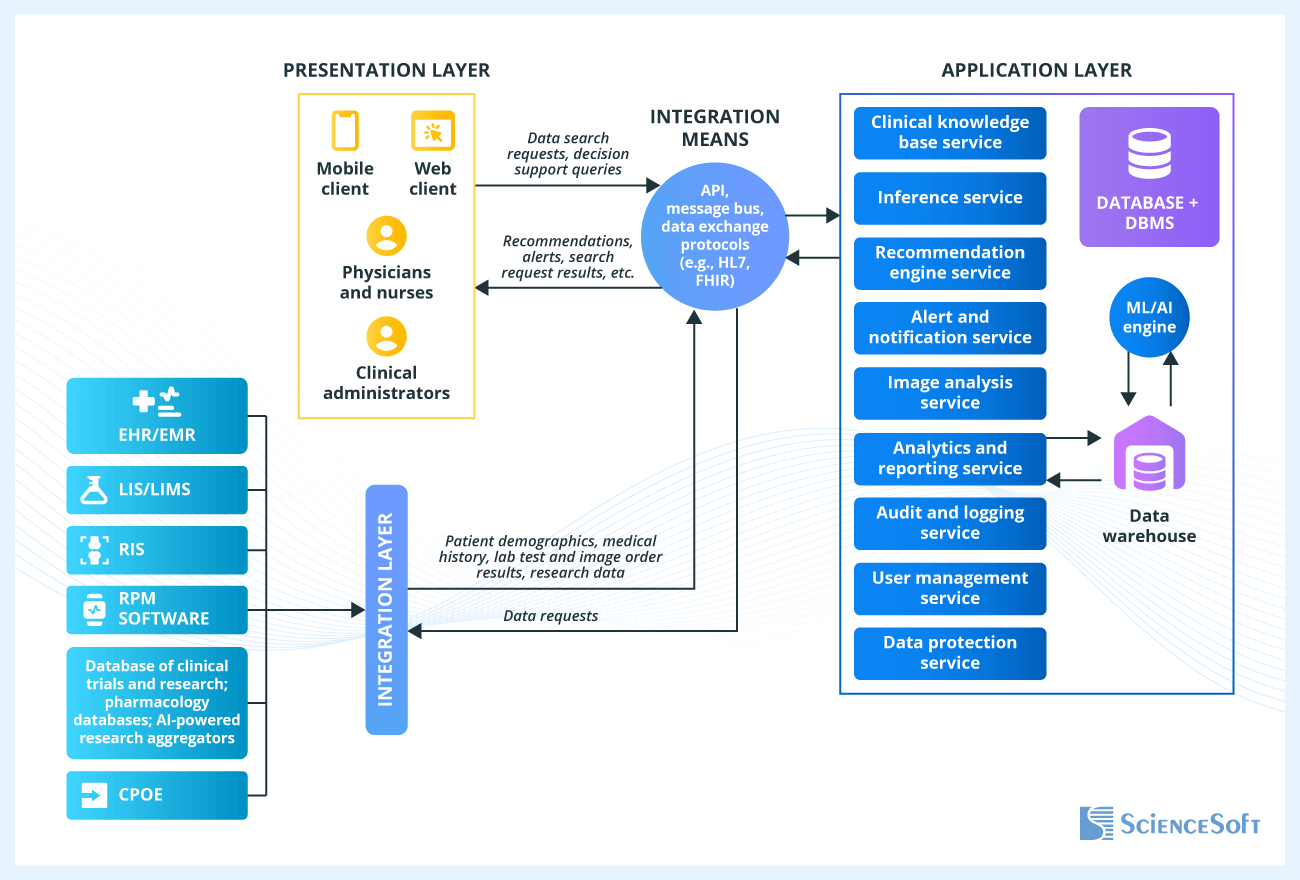
At the core of this initiative is the deployment of Clinical Decision Support Systems (CDSS). These are software tools designed to analyze patient data and provide clinicians with evidence-based suggestions for diagnosis or treatment. Unlike basic software, these systems utilize deep learning—a subset of AI that mimics the human brain’s neural networks—to recognize patterns in longitudinal data (data collected over a long period of time).
For example, in the context of sepsis—a life-threatening reaction to infection—the AI can monitor vitals like heart rate and lactate levels in real-time. By identifying a “sepsis signature” hours before clinical symptoms manifest, the system triggers an alert, allowing for the early administration of antibiotics. This shift from reactive to proactive medicine is critical, as every hour of delayed treatment in septic shock increases mortality risk significantly.
To ensure the integrity of these systems, the France 2030 program emphasizes the “Human-in-the-Loop” (HITL) model. This means the AI does not prescribe medication or perform surgery autonomously; it provides a probability-based recommendation that a licensed physician must verify and sign off on, maintaining the gold standard of medical accountability.
Geo-Epidemiological Bridging: France, the EMA, and the Global Stage
This pilot program does not exist in a vacuum. It is a direct response to the regulatory frameworks established by the European Medicines Agency (EMA) and the emerging EU AI Act. While the United States FDA has approved hundreds of AI-enabled medical devices through its “Software as a Medical Device” (SaMD) pathway, Europe is taking a more cautious, centralized approach to data sovereignty.
The French model creates a blueprint for other NHS-style single-payer systems in the UK, and beyond. By building a sovereign infrastructure, France avoids the “vendor lock-in” seen in some US hospitals that rely exclusively on proprietary algorithms from a single corporation. This ensures that the AI can be updated based on peer-reviewed clinical evidence rather than corporate profit motives.
“The deployment of AI in health must be governed by a commitment to transparency and equity. Without rigorous oversight, we risk automating existing biases in healthcare delivery, which could exacerbate disparities for marginalized populations.” — World Health Organization (WHO) Guidance on Ethics and Governance of AI for Health.
The following table summarizes the operational differences between a standard digital hospital and the AI-augmented model being pioneered in France:
| Clinical Function | Traditional Digital Hospital | AI-Augmented Hospital |
|---|---|---|
| Patient Triage | Manual assessment by nursing staff. | Predictive scoring based on real-time vitals. |
| Diagnostic Imaging | Radiologist review of static images. | AI-assisted anomaly detection (Computer Vision). |
| Data Sovereignty | Often hosted on global third-party clouds. | National sovereign cloud infrastructure. |
| Treatment Planning | Based on general clinical guidelines. | Precision medicine tailored to patient biomarkers. |
Funding, Bias, and the Quest for Algorithmic Neutrality
This project is funded by the France 2030 investment plan, a government-led initiative. Because the funding is public, the project is subject to higher transparency requirements than private ventures. But, a critical clinical concern remains: algorithmic bias. AI is only as decent as the data it is trained on. If the training sets lack diversity in ethnicity, age, or gender, the AI may produce inaccurate recommendations for certain patient populations.
To mitigate this, the program is integrating diverse datasets from across the French healthcare system, ensuring that the “training phase” of the AI includes a representative cross-section of the population. This is essential for maintaining the statistical significance of the AI’s outputs across different demographic strata.
the integration of these tools is being monitored through PubMed-indexed studies to ensure that the “augmented” workflow actually improves patient outcomes rather than simply increasing the volume of alerts—a phenomenon known as “alarm fatigue” which can lead to clinician burnout.
Contraindications & When to Consult a Doctor
While AI augmentation improves system efficiency, it is not a replacement for clinical judgment. Patients should be aware of the following:
- Automation Bias: There is a risk that clinicians may over-rely on AI suggestions. Always question your provider: “Is this recommendation based on the AI’s finding or your clinical assessment?”
- Data Anomalies: AI can occasionally produce “hallucinations” or false positives. If an AI-driven screening suggests a condition that contradicts your physical symptoms, insist on a secondary human review.
- When to Seek Immediate Care: AI tools are for optimization, not emergency diagnosis. If you experience acute chest pain, sudden neurological deficits (slurred speech, facial drooping), or severe respiratory distress, do not wait for a digital triage system—seek immediate emergency medical intervention.
The Future Trajectory of Augmented Medicine
The France 2030 pilot is a calculated gamble on the future of public health. By prioritizing sovereign infrastructure, France is positioning itself as a leader in “Ethical AI.” The success of this program will be measured not by the complexity of its code, but by the reduction in mortality rates and the increase in clinician wellbeing.
As we move toward a more integrated model of care, the goal is a symbiotic relationship: the AI handles the massive computational burden of data analysis, while the physician focuses on the empathetic, nuanced, and complex task of patient care. This is the essence of translational medicine—taking high-level scientific innovation and turning it into a tangible bedside benefit.
References
- World Health Organization (WHO) – Ethics and Governance of Artificial Intelligence for Health
- The Lancet Digital Health – Peer-reviewed studies on AI clinical integration
- European Medicines Agency (EMA) – Regulatory frameworks for digital health
- JAMA Network – Clinical trials on AI-assisted diagnostics

