Florida is currently experiencing a measles outbreak, with 143 cases reported statewide as of March 21, 2026. Collier County remains the epicenter, accounting for 73% of these cases, largely stemming from an outbreak at Ave Maria University. While cases continue to rise, the rate of increase has slowed compared to previous weeks, and Florida now ranks fourth nationally for measles incidence.
This resurgence of measles, a highly contagious viral illness, underscores the critical importance of vaccination. Measles isn’t simply a childhood rash; it’s a systemic infection that can lead to severe complications, particularly in vulnerable populations. The current outbreak highlights a concerning trend of declining vaccination rates and the potential consequences for public health. The virus, belonging to the paramyxovirus family, spreads through respiratory droplets produced by coughing or sneezing. Its high transmissibility – an R0 value between 12 and 18 – means that one infected person can spread the disease to a large number of unvaccinated individuals.
In Plain English: The Clinical Takeaway
- Measles is back: Cases are increasing, especially in Southwest Florida, but the spread is slowing.
- Vaccination is key: The MMR (Measles, Mumps, Rubella) vaccine is highly effective at preventing measles and its complications.
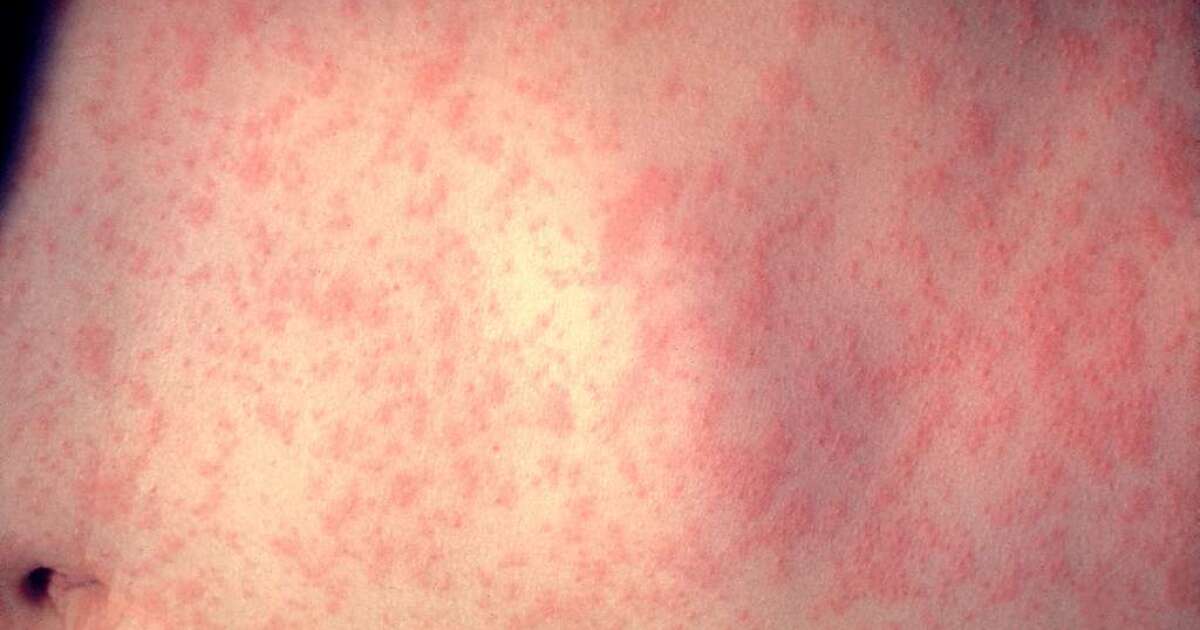
- Understand the symptoms: Fever, cough, runny nose, and a characteristic rash are signs of measles. Seek medical attention immediately if you suspect infection.
The Epidemiology of the 2026 Outbreak: A National Perspective
As of March 20, 2026, the U.S. Centers for Disease Control and Prevention (CDC) has recorded 1,487 measles cases nationwide. While Florida’s case count is significant, We see surpassed by South Carolina (698 cases), Texas, and Utah. This geographic distribution isn’t random. Areas with lower vaccination coverage are predictably experiencing higher incidence rates. The current outbreak is largely driven by imported cases from international travel, particularly from regions experiencing ongoing measles epidemics. Approximately 72% of Florida’s cases were acquired within the state, indicating sustained community transmission. This suggests that even limited pockets of unvaccinated individuals can fuel outbreaks.
The decline in vaccination rates is a complex issue, influenced by factors such as vaccine hesitancy, misinformation, and access barriers. The misconception that measles is a mild illness persists, despite the potential for serious complications like pneumonia, encephalitis (brain swelling), and even death. The mechanism of action of the MMR vaccine involves introducing a weakened (attenuated) form of the measles virus to stimulate the body’s immune system. This triggers the production of antibodies, providing long-lasting immunity. The vaccine undergoes rigorous testing in three phases: Phase I assesses safety, Phase II evaluates immunogenicity (antibody production), and Phase III confirms efficacy in large-scale, double-blind placebo-controlled trials.
Geo-Epidemiological Bridging: Impact on Florida Healthcare Systems
The outbreak is placing a strain on healthcare resources in affected counties, particularly Collier County. Emergency departments are seeing an increase in patients presenting with measles-like symptoms, requiring isolation protocols and specialized care. The Florida Department of Health (DOH) is working to contain the outbreak through contact tracing, vaccination campaigns, and public health education. Still, the lack of readily available vaccination status data for reported cases, as noted in the DOH’s reportable disease tracker, hinders effective outbreak response. This data gap limits the ability to quickly identify and target unvaccinated individuals for vaccination.
The situation also highlights the importance of collaboration between state and federal health agencies. The CDC provides technical assistance and resources to support state and local health departments in outbreak investigations and control efforts. The outbreak underscores the need for improved surveillance systems to detect and respond to emerging infectious disease threats. The National Center for Immunization and Respiratory Diseases (NCIRD) at the CDC is actively monitoring the outbreak and providing updated guidance to healthcare providers and the public.
| State | Reported Measles Cases (as of March 20, 2026) |
|---|---|
| South Carolina | 698 |
| Texas | (Data not publicly available, but exceeding Florida) |
| Utah | (Data not publicly available, but exceeding Florida) |
| Florida | 143 |
| Collier County (FL) | 104 |
Funding & Bias Transparency
The data utilized by the U.S. Measles Tracker and the CDC are primarily funded through federal appropriations allocated to public health surveillance and disease control programs. The development and ongoing evaluation of the MMR vaccine have been supported by pharmaceutical companies, including Merck & Co. While these companies contribute to research and development, it’s crucial to acknowledge potential biases. Independent research and rigorous regulatory oversight by agencies like the Food and Drug Administration (FDA) are essential to ensure the safety and efficacy of vaccines. The FDA’s Biologics Price Assessment and Research (BPAR) division plays a critical role in evaluating vaccine quality and safety.

“The current measles outbreak is a stark reminder of the importance of maintaining high vaccination coverage rates. Even small declines in vaccination can lead to a resurgence of this preventable disease.” – Dr. Nancy Messonnier, Director of the National Center for Immunization and Respiratory Diseases (NCIRD) at the CDC, speaking in a recent press briefing.
Contraindications & When to Consult a Doctor
The MMR vaccine is generally safe and well-tolerated. However, certain individuals should avoid receiving the vaccine. These include pregnant women, individuals with a history of severe allergic reaction to any component of the vaccine, and individuals with weakened immune systems due to conditions like leukemia or HIV/AIDS. Consult a doctor immediately if you experience any of the following symptoms: high fever (over 103°F), difficulty breathing, seizures, or severe rash after vaccination. If you suspect you or a family member has been exposed to measles, contact your healthcare provider immediately. Early diagnosis and supportive care can help prevent complications.
The long-term consequences of measles infection can be significant, even in individuals who recover. Research suggests a potential link between measles infection and an increased risk of subacute sclerosing panencephalitis (SSPE), a rare but fatal neurological disorder that can develop years after the initial infection. Longitudinal studies are ongoing to further investigate these potential long-term effects.
Looking ahead, sustained efforts to improve vaccination rates, address vaccine hesitancy, and strengthen public health infrastructure are crucial to prevent future measles outbreaks. Continued surveillance, rapid response to suspected cases, and effective communication with the public are essential components of a comprehensive measles control strategy.
References
- Centers for Disease Control and Prevention. (2026). Measles. https://www.cdc.gov/measles/index.html
- World Health Organization. (2024). Measles. https://www.who.int/news-room/fact-sheets/detail/measles
- Plotkin, S. A., Orenstein, W. A., & Offit, P. A. (2018). Plotkin’s Vaccines (6th ed.). Elsevier.
- American Academy of Pediatrics. (2023). Red Book: 2023 Report of the Committee on Infectious Diseases. American Academy of Pediatrics.
- Johns Hopkins Bloomberg School of Public Health. (2026). U.S. Measles Tracker. https://usmeasles.org/