The Rise of Predictive Embryo Selection: Ethical and Clinical Considerations
Recent advancements in polygenic risk scoring (PRS) are enabling prospective parents to select embryos based on predicted genetic predispositions to certain traits and diseases. This practice, gaining traction in fertility clinics across Asia and increasingly discussed globally, raises complex ethical and legal questions surrounding genetic determinism, reproductive autonomy, and potential societal impacts. The technology, while promising, demands careful scrutiny and robust regulatory frameworks.
The core of this emerging field lies in preimplantation genetic testing for polygenic traits (PGT-P). Unlike traditional PGT, which screens for single-gene disorders like cystic fibrosis, PGT-P assesses an embryo’s risk for conditions influenced by multiple genes – such as heart disease, type 2 diabetes, and certain cancers – using PRS. These scores are derived from genome-wide association studies (GWAS) that identify genetic variants associated with specific traits. However, it’s crucial to understand that PRS provides a *probability*, not a certainty, of developing a condition.
In Plain English: The Clinical Takeaway
- It’s not a guarantee: Genetic scores predict risk, they don’t definitively say if a child *will* develop a disease. Many factors, including lifestyle and environment, play a role.
- Limited scope: Currently, PRS is most accurate for common, complex diseases with strong genetic components. It’s less reliable for rarer conditions or traits influenced by many genes.
- Ethical debate: Choosing embryos based on predicted traits raises questions about what constitutes a “desirable” trait and the potential for exacerbating social inequalities.
Understanding Polygenic Risk Scores and Their Limitations
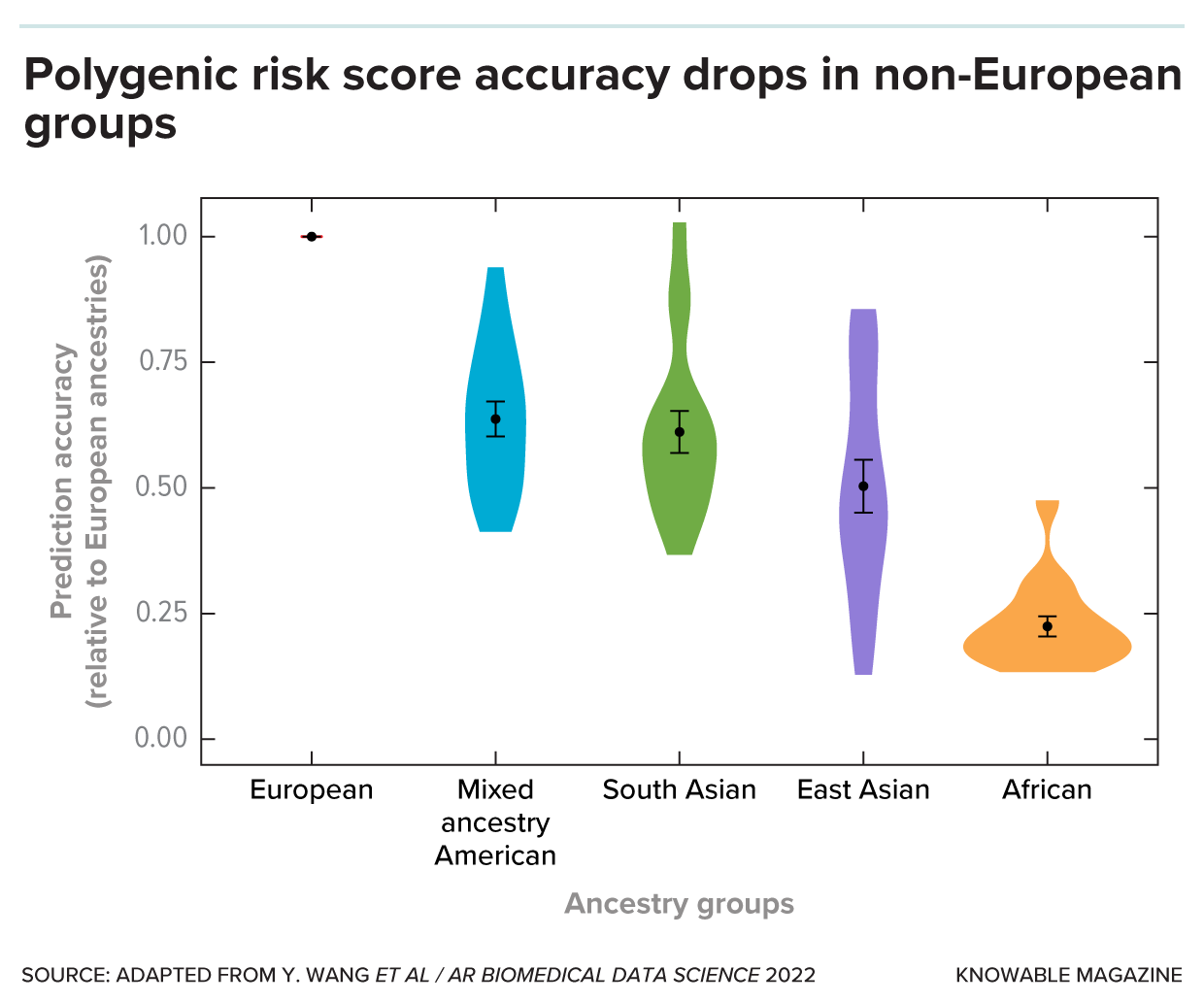
PRS are calculated by summing the effects of numerous genetic variants, each contributing a small amount to the overall risk. The accuracy of these scores depends heavily on the size and diversity of the GWAS used to generate them. Most current PRS are based on studies conducted on individuals of European ancestry, leading to concerns about their applicability to other populations. A study published in Nature Genetics in 2023 highlighted significant disparities in PRS accuracy across different ethnic groups, emphasizing the necessitate for more diverse genomic datasets. https://www.nature.com/articles/s41588-023-01108-7
The mechanism of action involves whole genome sequencing (WGS) of embryos created through in vitro fertilization (IVF). Following WGS, the embryo’s genome is compared to reference populations to generate a PRS for a range of traits. Clinicians then present prospective parents with information about the predicted genetic risk for each embryo, allowing them to craft a selection. This process differs significantly from preimplantation genetic diagnosis (PGD), which identifies embryos carrying specific, known disease-causing mutations. PGD is a diagnostic test. PGT-P is a predictive assessment.
Global Regulatory Landscape and Regional Impacts
The regulatory landscape surrounding PGT-P is fragmented. Currently, the practice is largely unregulated in many countries, including much of Asia. In the United States, the Food and Drug Administration (FDA) has not yet established specific guidelines for PGT-P, even though it is monitoring the field closely. The European Society of Human Reproduction and Embryology (ESHRE) has issued non-binding recommendations, urging caution and emphasizing the need for robust ethical oversight. https://www.eshre.eu/Guidelines-and-Recommendations/PGT-guidelines The United Kingdom’s Human Fertilisation and Embryology Authority (HFEA) is currently reviewing the ethical and legal implications of PGT-P, with a public consultation planned for late 2026.
This lack of harmonization creates challenges for international reproductive tourism. Prospective parents may travel to countries with more permissive regulations to access PGT-P, raising concerns about equitable access and the potential for exploitation. The cost of PGT-P – typically several thousand dollars per IVF cycle – limits access to affluent individuals, potentially exacerbating existing health disparities.
Funding & Bias Transparency
Much of the foundational research in polygenic risk scoring has been funded by the National Institutes of Health (NIH) in the United States and the Medical Research Council (MRC) in the United Kingdom. However, several companies offering PGT-P services have received venture capital funding, creating a potential conflict of interest. Transparency regarding funding sources and potential biases is crucial for maintaining public trust.
“The biggest challenge isn’t the technology itself, but the interpretation and communication of risk. We need to ensure that prospective parents understand the limitations of PRS and are not misled into believing they can ‘design’ a perfect baby.” – Dr. Emily Carter, Professor of Bioethics, University of Oxford.
Data Summary: Accuracy of Polygenic Risk Scores
| Trait | Population | PRS Accuracy (R2) | Source |
|---|---|---|---|
| Coronary Artery Disease | European Ancestry | 0.10-0.15 | PLoS Genetics (2018) |
| Type 2 Diabetes | European Ancestry | 0.15-0.20 | The Lancet (2019) |
| Schizophrenia | European Ancestry | 0.20-0.25 | Nature Neuroscience (2022) |
| Height | European Ancestry | 0.25-0.35 | Genome Biology (2020) |
Contraindications & When to Consult a Doctor
PGT-P is not appropriate for individuals with a family history of severe, single-gene disorders that can be detected through traditional PGD. It is too not recommended for individuals who have unrealistic expectations about the ability of PRS to predict future health outcomes. Prospective parents experiencing anxiety or distress related to genetic risk assessment should consult with a genetic counselor or mental health professional. Symptoms of undue stress, obsessive thinking about genetic risks, or feelings of guilt or shame warrant immediate professional intervention. Individuals with pre-existing mental health conditions should proceed with extreme caution and under the guidance of a qualified healthcare team.
The Future of Predictive Embryo Selection
The field of PGT-P is rapidly evolving. Ongoing research is focused on improving the accuracy of PRS, expanding their applicability to diverse populations, and developing more sophisticated algorithms that can predict a wider range of traits. However, the ethical and legal challenges remain significant. A thoughtful and inclusive public dialogue is essential to ensure that this powerful technology is used responsibly and equitably. The long-term societal consequences of widespread embryo selection based on genetic predictions are still unknown, and careful monitoring will be crucial in the years to come. The World Health Organization (WHO) is expected to release a formal position statement on PGT-P in early 2027, providing further guidance to member states. https://www.who.int/news-room/research-and-development
References
- Choi, S. W., et al. “Genome-wide association studies of complex traits in diverse populations.” Nature Genetics 55.1 (2023): 108-118.
- Visscher, P. M. “Polygenic scores for common diseases.” The Lancet 394.10211 (2019): 1863-1875.
- Plomin, R., et al. “Predicting polygenic risk scores from genome-wide association studies.” Genome Biology 21.1 (2020): 269.
- O’Reilly, P. F., et al. “Multiple independent variants influence height in humans.” PLoS Genetics 14.8 (2018): e1002786.
- Schizophrenia Working Group of the Psychiatric Genomics Consortium. “Biological insights from genome-wide association studies of schizophrenia.” Nature Neuroscience 25.10 (2022): 1448-1459.