Childhood cancer survival is a global equity crisis. Whereas high-income nations achieve survival rates exceeding 80%, children in low- and middle-income countries (LMICs) often face rates below 20%. This disparity is driven by inadequate diagnostic registries, a lack of pathological review, and systemic barriers to standardized care.
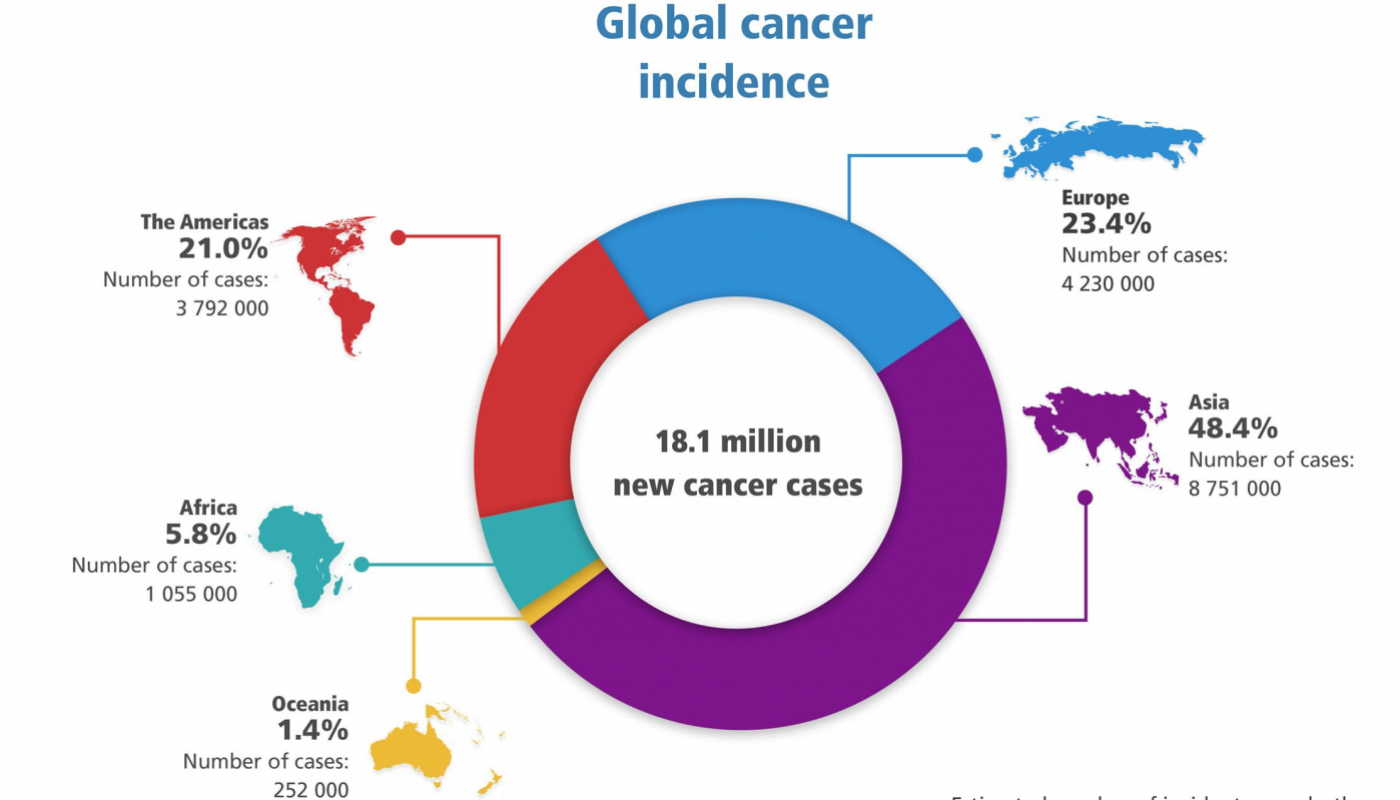
The tragedy of pediatric oncology is not merely a lack of medicine, but a lack of visibility. In this week’s analysis of global health metrics, we confront a staggering reality: only 21% of the global population lives in regions with population-based cancer registries. These registries are the foundational infrastructure required to track incidence, identify clusters, and measure the efficacy of treatments. Without them, we are fighting a ghost—treating patients without knowing the true scale of the epidemic or why certain populations are failing to respond to standard protocols.
In Plain English: The Clinical Takeaway
- Diagnosis is more than location: Knowing a tumor is in the abdomen isn’t enough; doctors must use morphology (examining the actual shape and structure of cells) to know exactly what the cancer is.
- The “Data Gap” kills: In many parts of the world, cancer is only recorded when a child dies, meaning we miss the chance to intervene early.
- Geography is destiny: A child’s chance of survival currently depends more on their country’s healthcare infrastructure than on the biological aggressiveness of their tumor.
The Diagnostic Blind Spot: Why Morphology Trumps Location
In adult oncology, the site of the tumor (e.g., lung or colon) often provides a strong clue to the cancer’s identity. In pediatric oncology, Here’s a dangerous assumption. Pediatric cancers are characterized by their morphology—the specific biological architecture of the cells—rather than their anatomical site. For instance, a mass in the abdomen of a toddler could be a Wilms tumor (originating in the kidney) or a neuroblastoma (originating in the adrenal glands). These two diseases require entirely different chemotherapy regimens and surgical approaches.
To differentiate these, clinicians rely on histopathology, the microscopic examination of tissue samples. Still, in many LMICs, the “pathology bottleneck” is severe. A lack of trained pathologists and specialized staining equipment means many children are treated based on the location of the mass rather than the cellular identity. This leads to suboptimal treatment and increased toxicity without clinical benefit.
The mechanism of action for most pediatric chemotherapy involves targeting rapidly dividing cells. When the wrong drug is administered given that of a morphological misdiagnosis, the child is exposed to severe contraindications—conditions or factors that serve as a reason to withhold a certain medical treatment due to the harm that it would cause the patient—without any hope of tumor regression.
The Geography of Survival: Mapping the 80/20 Divide
The disparity in outcomes is not a result of biological differences between children, but a failure of health systems. In the United States, the FDA and National Cancer Institute (NCI) ensure that clinical trials are integrated into standard care. In Europe, the EMA coordinates similar rigorous standards. In contrast, much of the Global South relies on passive follow-up, a system where data is only collected through death certificates rather than active patient tracking.
This creates a lethal feedback loop: because deaths aren’t accurately recorded, the perceived burden of childhood cancer remains low, which in turn justifies low funding for oncology wards and pathology labs.
| Metric | High-Income Countries (HICs) | Low/Middle-Income Countries (LMICs) | Clinical Impact |
|---|---|---|---|
| Average Survival Rate | >80% | <20% – 60% | Extreme disparity in mortality |
| Registry Coverage | High (>90%) | Low (<20%) | Inability to track incidence |
| Diagnostic Tooling | Molecular Profiling | Basic Imaging/Clinical Exam | High rate of misdiagnosis |
| Treatment Access | Multimodal (Surgery/Chemo/Rad) | Primarily Basic Chemotherapy | Higher relapse rates |
Scaling the Infrastructure: From Passive Tracking to Active Intervention
Addressing this gap requires a shift from passive observation to active surveillance. The World Health Organization (WHO) has launched the Global Initiative for Childhood Cancer, aiming to raise survival rates to at least 60% in all countries. This requires the implementation of double-blind placebo-controlled trials tailored to LMIC populations to ensure that the drugs being exported are effective across different genetic backgrounds and nutritional statuses.
“The survival gap in pediatric cancer is a moral failure of global health. We have the cures; what we lack is the delivery system and the diagnostic precision to apply them where they are needed most.” — Dr. Rima Nashat, WHO Consultant on Childhood Cancer.
the integration of liquid biopsies—testing blood for circulating tumor DNA—could bypass the need for invasive surgical biopsies in regions where sterile operating theaters are scarce. This would allow for a more rapid, non-invasive assessment of morphology and treatment response.
Funding and Bias Transparency
Much of the current data on global pediatric cancer disparities is funded by the World Health Organization (WHO) and supported by grants from non-governmental organizations such as St. Jude Children’s Research Hospital. While these organizations are highly respected, funding is often earmarked for specific “high-visibility” cancers (like leukemia), potentially leaving rarer pediatric sarcomas under-researched in the Global South.
Contraindications & When to Consult a Doctor
While this article discusses global health policy, parents and caregivers should be vigilant about pediatric warning signs. Seek immediate professional medical intervention if a child exhibits:
- Unexplained lumps: Any firm, non-tender mass in the abdomen, neck, or groin.
- Persistent fever: A fever that does not respond to standard antipyretics and is accompanied by extreme fatigue.
- Unexplained bruising: Petechiae (slight red/purple spots) or bruising without a clear history of trauma, which may indicate bone marrow infiltration.
- Sudden vision changes: A white pupil (leukocoria) visible in photographs or a sudden onset of strabismus (crossed eyes).
Clinical Warning: In resource-limited settings, avoid “alternative” or “traditional” cures for suspected tumors. These often delay the window for curative chemotherapy, rendering the cancer incurable by the time a medical facility is reached.
The Path Forward: A Test of Global Equity
The fight against childhood cancer is the ultimate equity test for global health. We possess the clinical knowledge to cure the vast majority of these children; the barrier is no longer scientific, but logistical and political. By investing in population-based registries and pathology infrastructure, the global medical community can move from a state of reactive grief to proactive cure. The goal is a world where a child’s survival is determined by the science of their disease, not the coordinates of their birth.