Many people contract chickenpox during childhood, but having the illness doesn’t mean the virus disappears from the body. The varicella-zoster virus can remain dormant within the system for years, even decades, and reactivate, causing a different illness, according to a specialist from the National Autonomous University of Mexico (UNAM).
According to José Luis Alfredo Mora Guevara, academic secretary of the Faculty of Higher Studies Zaragoza (FES) UNAM, reactivation of the virus in someone who has had chickenpox leads to herpes zoster, a condition that typically presents in adulthood. Approximately 220,000 new cases of herpes zoster occur annually in Mexico, primarily among individuals over the age of 50.
Understanding the lifecycle of the varicella-zoster virus is crucial for preventative care. This virus, as explained by Cleveland Clinic, is responsible for causing chickenpox, herpes zoster, and other infections. It establishes itself within the nerve ganglia, structures composed of neurons responsible for transmitting sensory information throughout the body.
These ganglia, characterized by cells that are long-lasting and slow to renew, provide an ideal refuge for the virus. While the immune system can monitor and suppress viral activity for extended periods, its effectiveness relies on maintaining a strong and healthy immune response.
Historical observations, dating back over a century, revealed that herpes zoster lesions follow specific pathways on the skin, commonly affecting only one side of the body. These areas correspond to dermatomes, regions connected to specific sensory nerves. Subsequent studies confirmed the virus resides within the neurons of nerve ganglia and, upon reactivation when the body’s defenses are weakened, travels along a nerve, causing inflammation, nerve damage, and intense pain.
Mora Guevara emphasizes that herpes zoster can only develop in individuals who have previously had chickenpox, as it represents a reactivation of the same virus within the nervous system.
Recognizing the Symptoms of Herpes Zoster
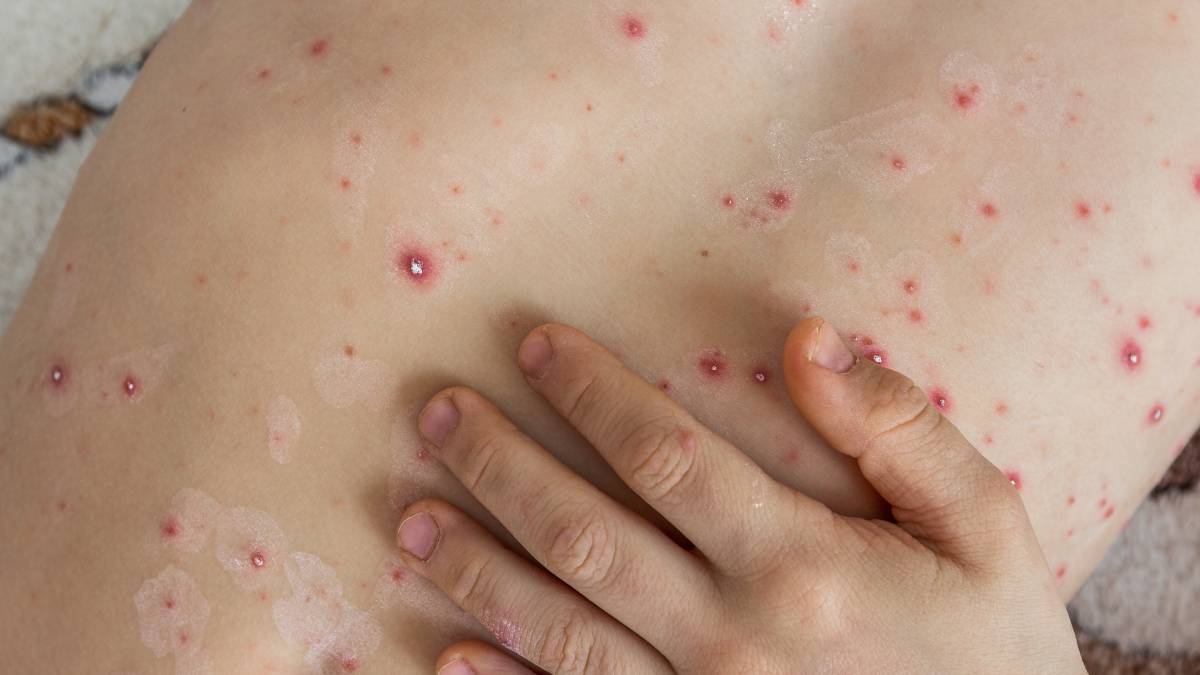
Herpes zoster typically begins with a prodromal phase characterized by burning pain, tingling, or itching in a specific area of the body, most often the torso, but potentially affecting the face or eyes. Within days, a reddish rash with fluid-filled blisters appears, following the path of the affected nerve and presenting on only one side of the body. These lesions evolve into scabs and heal over a period of two to four weeks.
When the virus affects the eye or the tip of the nose, it is considered a severe form requiring immediate medical attention, as it can lead to inflammation of the cornea (keratitis), uveitis or glaucoma, and potentially partial or irreversible vision loss.
During an outbreak, the pain can be intense and persistent, even with mild stimuli like the touch of clothing.
Postherpetic Neuralgia and Other Risks
In most cases, pain subsides as the skin heals. Though, some individuals, particularly older adults, may develop postherpetic neuralgia, a chronic pain condition lasting months or even years. In severe cases, facial paralysis can occur due to nerve damage.
The risk of developing herpes zoster increases when the immune system is compromised by factors such as cancer, HIV, immunosuppressive treatments, aging, physical or emotional stress, or poorly controlled chronic diseases like diabetes.
Prevention Through Vaccination
The most effective way to prevent herpes zoster is vaccination, especially for adults over 50 or those with risk factors. Two primary vaccines are available:
- Zostavax: Contains live, attenuated virus, but its effectiveness diminishes over time and is less commonly used now.
- Shingrix: A recombinant vaccine with approximately 90% efficacy, currently recommended. It is administered in two doses, even for individuals who have previously had the disease.
Diagnosis and Timely Treatment
Diagnosis of herpes zoster is typically clinical, based on symptoms and the appearance of lesions, particularly their unilateral distribution along dermatomes. In atypical cases, tests like PCR (polymerase chain reaction) can be used to detect the virus’s genetic material.
Antiviral treatment is most effective when initiated within 72 hours of the rash appearing, reducing the duration of the outbreak, pain, and the risk of complications.
Disclaimer: The information provided in this article is for general knowledge and informational purposes only, and does not constitute medical advice. It is essential to consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
As research continues and vaccination rates increase, monitoring the incidence of herpes zoster and the effectiveness of preventative measures will be crucial. Staying informed and proactive about your health is the best defense against this potentially debilitating condition.
What are your thoughts on the importance of vaccination for preventing shingles? Share your comments below.