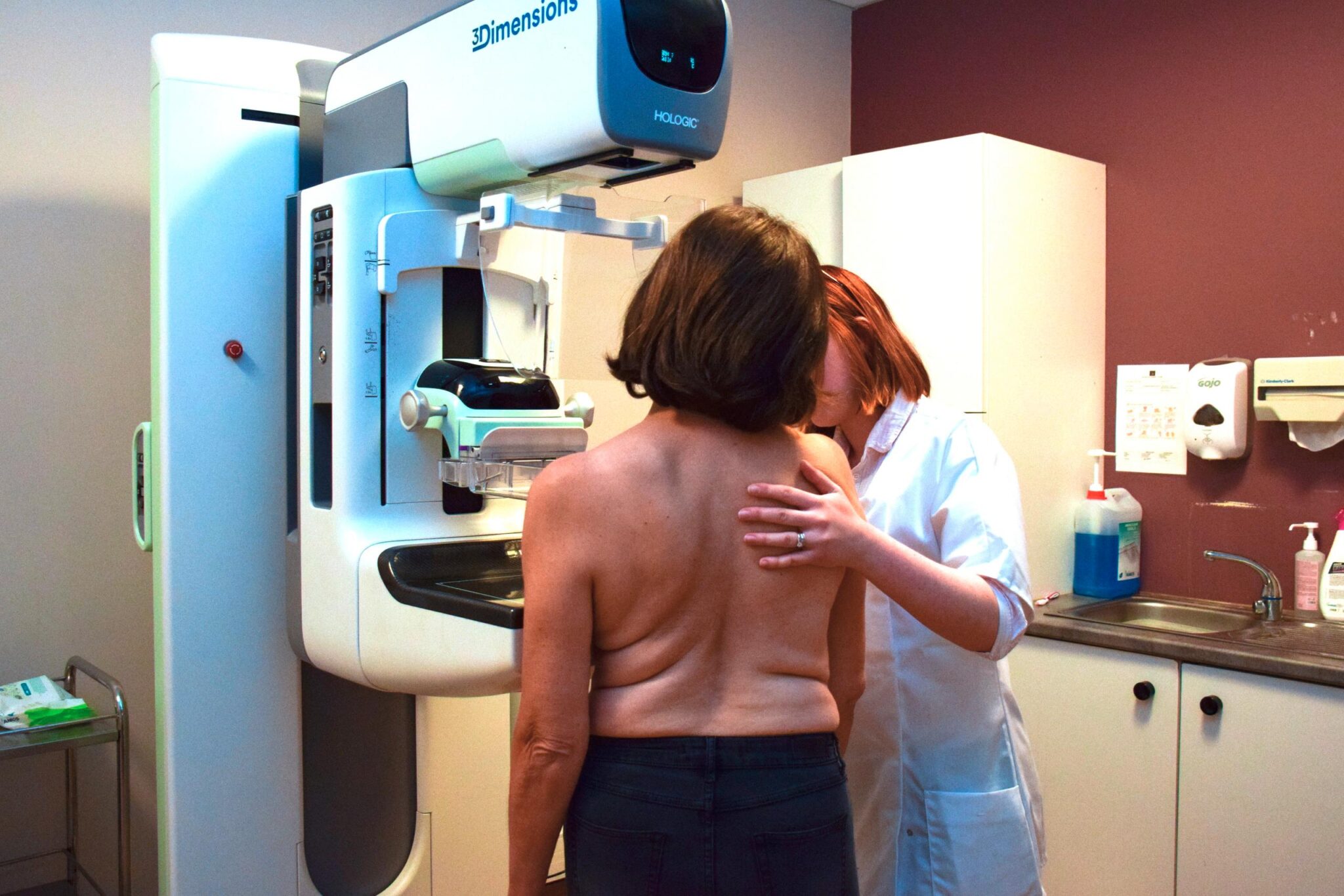
French Data Highlights Impact of Breast Cancer Screening, But Challenges Remain
Recent data from l’Institut National du Cancer (INCa) in France indicates that breast cancer screening programs saved an estimated 23,000 lives between 2004, and 2018. This underscores the critical role of early detection in improving outcomes, but as well highlights ongoing debates about screening frequency, accessibility, and the evolving landscape of diagnostic imaging. This report, published amidst advancements in prostate cancer imaging, prompts a broader discussion on the efficacy of preventative cancer screenings globally.
In Plain English: The Clinical Takeaway
- Early Detection Saves Lives: Finding breast cancer early, before symptoms appear, significantly increases the chances of successful treatment.
- Screening Isn’t Perfect: While beneficial, screening programs have limitations, including false positives (incorrectly identifying cancer) and false negatives (missing cancer).
- Talk to Your Doctor: The decision about when and how often to get screened should be made in consultation with your healthcare provider, considering your individual risk factors.
The Power of Population-Level Screening: A Closer Glance at the INCa Data
The INCa’s findings, covering a 14-year period, are based on a retrospective analysis of data from the French national breast cancer screening program. This program primarily utilizes mammography, a type of X-ray imaging of the breast, to detect tumors. The 23,000 lives saved represent a substantial public health benefit, demonstrating the effectiveness of organized screening initiatives. However, it’s crucial to understand the nuances of these statistics. The reduction in mortality isn’t solely attributable to screening; improvements in treatment modalities – such as targeted therapies and surgical techniques – also play a significant role. The observed mortality reduction is estimated to be around 12-15% in women regularly participating in screening programs. Research published in The Lancet Oncology details the complexities of attributing mortality reductions solely to screening, emphasizing the interplay of various factors.
Beyond Mammography: The Evolution of Breast Cancer Detection
While mammography remains the cornerstone of breast cancer screening, advancements in imaging technology are continually refining diagnostic accuracy. Digital breast tomosynthesis (DBT), also known as 3D mammography, creates a three-dimensional image of the breast, reducing the likelihood of false positives and improving cancer detection rates, particularly in women with dense breast tissue. The National Cancer Institute (NCI) provides comprehensive information on DBT and its benefits. Breast MRI (magnetic resonance imaging) is often used as a supplemental screening tool for women at high risk of developing breast cancer, such as those with a strong family history or genetic mutations like BRCA1 and BRCA2. The mechanism of action behind MRI involves using strong magnetic fields and radio waves to create detailed images of the breast tissue, detecting subtle changes that may not be visible on mammography.

Geographical Disparities and Access to Screening
The success of breast cancer screening programs is heavily reliant on equitable access to healthcare. In the United States, for example, access to screening varies significantly based on socioeconomic status, race, and geographic location. Women in rural areas and those from underserved communities often face barriers to screening, including lack of insurance, transportation difficulties, and limited availability of imaging facilities. The Centers for Disease Control and Prevention (CDC) actively works to address these disparities through initiatives aimed at increasing screening rates among vulnerable populations. Similar challenges exist in Europe, where healthcare systems and screening protocols differ significantly between countries. The European Commission is currently focusing on harmonizing breast cancer screening guidelines across member states to ensure consistent quality and accessibility.
Funding and Bias Transparency
The research underpinning the INCa’s analysis was primarily funded by the French government through its national cancer research program. While this indicates a commitment to public health, it’s important to acknowledge that government funding can sometimes be subject to political priorities. Independent research, funded by organizations like the Breast Cancer Research Foundation (BCRF) and the National Institutes of Health (NIH) in the US, plays a crucial role in providing unbiased data and driving innovation in breast cancer screening and treatment.
“The key to maximizing the benefits of breast cancer screening lies in personalized approaches. We necessitate to move beyond a one-size-fits-all model and tailor screening recommendations based on individual risk factors and preferences.”
Contraindications & When to Consult a Doctor
While breast cancer screening is generally safe, certain conditions may warrant caution. Women with a history of radiation therapy to the chest, particularly during childhood, may be at increased risk of developing breast cancer later in life and should discuss appropriate screening strategies with their doctor. Similarly, women with certain genetic mutations, such as BRCA1 and BRCA2, should consider earlier and more frequent screening. It’s crucial to consult a doctor if you experience any breast changes, such as a fresh lump, nipple discharge, or changes in breast size or shape, regardless of your screening schedule. These symptoms should be evaluated promptly to rule out cancer or other underlying conditions.
Data Summary: Comparing Screening Modalities
| Screening Modality | Sensitivity | Specificity | Cost (Approximate) | Radiation Exposure |
|---|---|---|---|---|
| Mammography (2D) | 80-90% | 70-80% | $100-200 | Low |
| Digital Breast Tomosynthesis (DBT) | 90-95% | 80-90% | $200-300 | Low |
| Breast MRI | 95-98% | 85-90% | $300-600 | None |
The Future of Breast Cancer Screening
The field of breast cancer screening is constantly evolving. Researchers are exploring new biomarkers, such as circulating tumor cells (CTCs) and circulating tumor DNA (ctDNA), that could potentially be used to detect cancer at even earlier stages. Artificial intelligence (AI) is also playing an increasingly important role in image analysis, helping radiologists to identify subtle abnormalities that might otherwise be missed. The ultimate goal is to develop more accurate, personalized, and accessible screening programs that can further reduce breast cancer mortality and improve the lives of women worldwide. Continued investment in research and a commitment to equitable access to healthcare are essential to achieving this goal.
References
- O’Malley, S., et al. “The impact of breast cancer screening programmes on mortality: a systematic review and meta-analysis.” The Lancet Oncology 19.11 (2018): 1439-1450.
- National Cancer Institute. “3D Mammography.”
- Centers for Disease Control and Prevention. “Breast Cancer Screening.”
- European Journal of Radiology