South Korean vascular surgeons at Dajeong Cardiovascular Hospital have surpassed 4,000 successful cases utilizing a hybrid treatment approach for varicose veins. This minimally invasive technique combines endovenous laser ablation (EVLA) or radiofrequency ablation (RFA) for larger, deeper veins with phlebectomy or sclerotherapy for smaller, superficial veins, offering a comprehensive solution for this common condition. The milestone, reported this week, signals a growing trend towards personalized venous care.
Varicose veins, affecting an estimated 20-25% of the adult population globally, are not merely a cosmetic concern. They can lead to significant pain, swelling, skin changes, and, in severe cases, venous ulcers. The hybrid approach aims to address the underlying venous insufficiency – the root cause of the problem – while simultaneously improving cosmetic outcomes. This is particularly relevant as the global market for varicose vein treatments is projected to reach $4.8 billion by 2028, driven by an aging population and increasing awareness of treatment options.
In Plain English: The Clinical Takeaway
- What This proves: A two-step fix for varicose veins, using heat to close off problem veins and then removing smaller ones for better appearance.
- Why it matters: It’s less invasive than traditional surgery, meaning faster recovery and less pain.
- Who it’s for: People with visible, painful varicose veins who haven’t found relief with simpler treatments like compression stockings.
The Science Behind Hybrid Varicose Vein Treatment
The “hybrid” designation refers to the combination of techniques targeting different aspects of the venous system. Varicose veins develop when valves within veins become incompetent, allowing blood to pool and flow backward (venous reflux). EVLA and RFA utilize heat to create a controlled inflammatory response, causing the vein to collapse and eventually be reabsorbed by the body. This addresses the primary source of reflux in larger, “truncal” veins. However, smaller, reticular, and spider veins often remain visible even after truncal vein treatment. Phlebectomy involves tiny incisions to physically remove these veins, while sclerotherapy uses an injectable solution to cause them to scar and disappear. The synergy between these methods provides a more complete and aesthetically pleasing result.
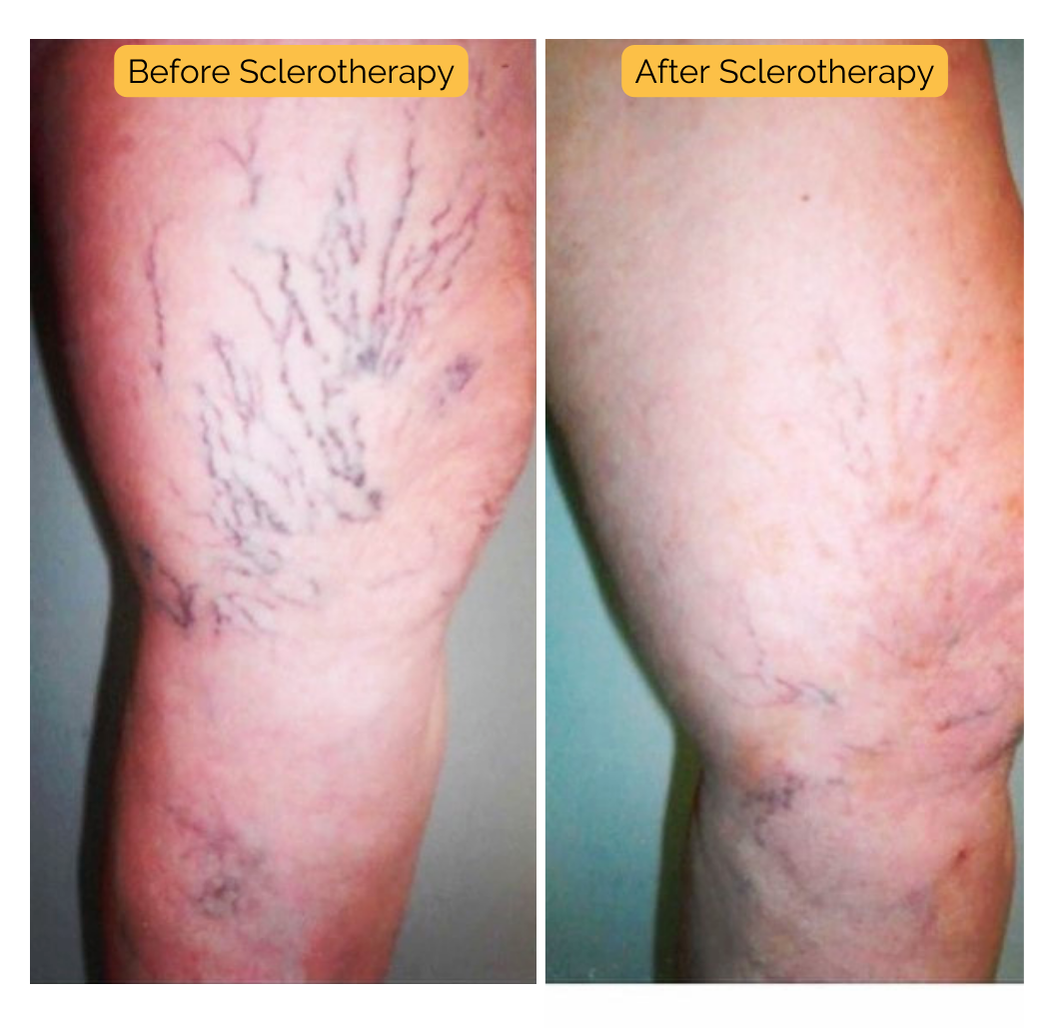
The mechanism of action for EVLA and RFA relies on targeted thermal energy. Specifically, the heat denatures the collagen within the vein wall, leading to fibrosis and eventual occlusion. This process, known as thermocoagulation, is carefully controlled to minimize damage to surrounding tissues. Sclerotherapy, conversely, induces endothelial damage and thrombosis through the chemical irritation of the vein lining. The choice between phlebectomy and sclerotherapy for superficial veins depends on vein size, location, and patient preference.
Global Adoption and Regulatory Landscape
While the Dajeong hospital’s 4,000-case milestone is significant, hybrid approaches to varicose vein treatment are gaining traction globally. In the United States, the Food and Drug Administration (FDA) has approved various devices for EVLA and RFA, as well as sclerosing agents. However, the specific combination and sequencing of these techniques are often at the discretion of the treating physician. The European Medicines Agency (EMA) similarly regulates these technologies within the European Union. The National Health Service (NHS) in the United Kingdom offers varicose vein treatments, with guidelines emphasizing minimally invasive options where appropriate. Access to these treatments can vary based on regional healthcare policies and individual patient needs.

The increasing adoption of hybrid techniques is partly driven by evidence from clinical trials. A meta-analysis published in the Journal of Vascular Surgery ( https://pubmed.ncbi.nlm.nih.gov/32889389/) demonstrated that combined techniques resulted in higher rates of vein closure and improved patient satisfaction compared to single-modality treatments. However, long-term follow-up studies are still needed to assess the durability of these results and identify potential late complications.
“The hybrid approach represents a paradigm shift in varicose vein management. By addressing both the underlying physiological problem and the cosmetic concerns, You can offer patients a more comprehensive and satisfying outcome,” says Dr. Peter Lawrence, a leading vascular surgeon and researcher at the University of Michigan.
Data on Efficacy and Patient Demographics
| Treatment Component | Typical Success Rate | Common Side Effects | Duration of Procedure |
|---|---|---|---|
| Endovenous Laser Ablation (EVLA) | 90-95% | Bruising, mild pain, temporary skin discoloration | 30-60 minutes per leg |
| Radiofrequency Ablation (RFA) | 88-93% | Similar to EVLA | 30-60 minutes per leg |
| Phlebectomy | 80-90% | Small scars, minor bleeding | 15-30 minutes per leg |
| Sclerotherapy | 60-80% (multiple sessions often required) | Temporary bruising, skin staining, mild discomfort | 15-30 minutes per session |
Funding and Potential Biases
It’s important to note that much of the research supporting varicose vein treatments is funded by medical device manufacturers. While this doesn’t necessarily invalidate the findings, it’s crucial to consider potential biases. For example, studies sponsored by companies that produce EVLA or RFA devices may be more likely to report favorable outcomes for those technologies. Transparency regarding funding sources is essential for maintaining the integrity of medical research. The Dajeong hospital’s data, while impressive, would benefit from independent verification and publication in a peer-reviewed journal.
Contraindications & When to Consult a Doctor
While generally safe, hybrid varicose vein treatment is not suitable for everyone. Contraindications include active deep vein thrombosis (DVT), severe peripheral artery disease, uncontrolled diabetes, and certain autoimmune conditions. Pregnant or breastfeeding women should also postpone treatment. Individuals with a history of blood clotting disorders should discuss the risks and benefits with their physician. Consult a doctor if you experience any of the following symptoms: persistent leg pain, swelling, skin ulcers, or changes in skin color. Early diagnosis and treatment can prevent complications and improve quality of life.
The future of varicose vein treatment likely lies in even more personalized approaches, incorporating genetic factors and advanced imaging techniques to optimize treatment selection and predict outcomes. Continued research and innovation are essential for improving the care of patients with this common and often debilitating condition.