Severe Hyponatremia in Kidney Failure: New Hope Through Targeted Hemodialysis
A recent case study, published this week in Cureus, details the successful treatment of profoundly low sodium levels (hyponatremia) in a patient experiencing acute kidney injury (AKI) and complete cessation of urine production (anuria). Utilizing short, intermittent hemodialysis, clinicians effectively and safely restored sodium balance, offering a potential new approach to managing this life-threatening condition. This case highlights the critical need for rapid diagnosis and specialized treatment protocols.
In Plain English: The Clinical Takeaway
- Low Sodium is Dangerous: Severely low sodium levels can cause brain swelling and seizures, especially when they develop quickly.
- Kidney Failure Complicates Things: When kidneys aren’t working, the body struggles to regulate sodium, making the problem worse.
- Hemodialysis Can Help: A specialized form of dialysis can carefully remove excess fluid and restore sodium balance, even when kidneys aren’t functioning.
The Complex Interplay of Hyponatremia and Acute Kidney Injury
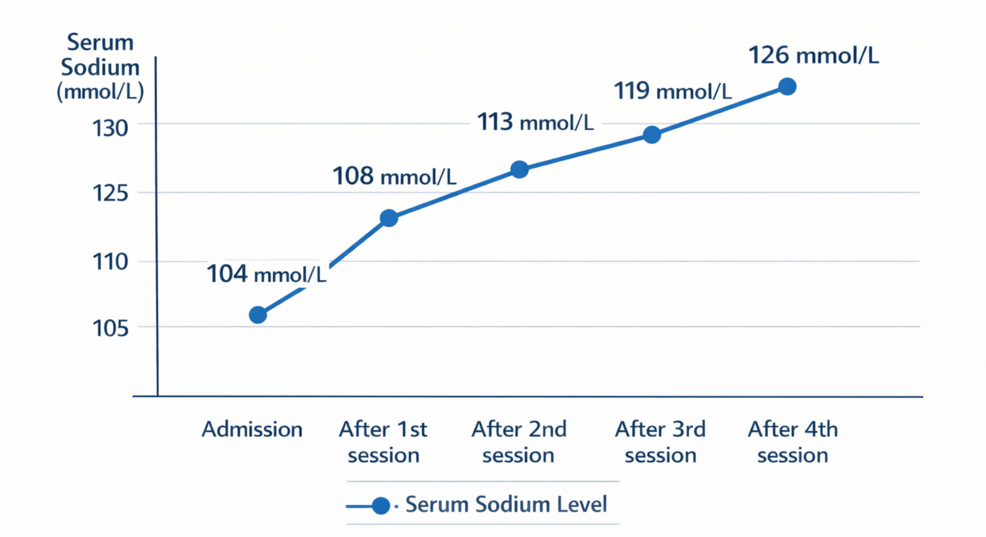
Hyponatremia, defined as a serum sodium concentration below 135 mEq/L, is a common electrolyte disturbance. However, profoundly low levels – below 120 mEq/L – are often associated with significant morbidity and mortality. The case reported in Cureus involved a patient with a sodium level of just 112 mEq/L, coupled with anuric AKI. This combination is particularly challenging because standard treatments for hyponatremia, such as fluid restriction, are often ineffective when the kidneys are unable to excrete excess water. The underlying pathophysiology involves the dysregulation of vasopressin, too known as antidiuretic hormone (ADH). ADH promotes water reabsorption in the kidneys, and in the setting of AKI, its continued release can lead to dilutional hyponatremia. The mechanism of action of hemodialysis in this context isn’t simply filtration; it’s a controlled osmotic gradient shift, carefully removing excess fluid while minimizing the risk of overly rapid sodium correction, which can itself cause neurological damage – a condition known as osmotic demyelination syndrome (ODS).
Expanding on the Evidence: Epidemiology and Clinical Trials
While isolated case reports like this are valuable, understanding the broader epidemiological context is crucial. Hyponatremia is estimated to affect up to 20% of hospitalized patients, with severe hyponatremia (below 120 mEq/L) occurring in approximately 1-2% of this population. (Epstein, M., et al. Am J Kidney Dis. 2018;71(5):663-672.) The incidence of AKI is also rising globally, driven by factors such as diabetes, hypertension, and the increasing use of nephrotoxic medications. Currently, there are no large-scale, randomized controlled trials specifically evaluating the use of short intermittent hemodialysis for the treatment of severe hyponatremia associated with anuric AKI. However, several smaller studies and case series have demonstrated its feasibility and safety. The standard of care typically involves careful fluid restriction and, in some cases, loop diuretics if residual kidney function exists. However, these approaches are often insufficient in patients with complete anuria. Further research, including Phase II and Phase III clinical trials, is needed to definitively establish the role of hemodialysis in this patient population. A double-blind placebo-controlled trial would be ethically challenging given the severity of the condition, but a prospective, observational study comparing hemodialysis to conventional therapy could provide valuable insights.
Geographical Impact and Healthcare System Considerations
The accessibility of short intermittent hemodialysis varies significantly across different healthcare systems. In the United States, most hospitals have hemodialysis capabilities, but access may be limited in rural areas or smaller facilities. The FDA has approved various hemodialysis machines and dialyzers, ensuring a baseline level of safety and efficacy. In Europe, the European Medicines Agency (EMA) regulates medical devices, including hemodialysis equipment. The National Health Service (NHS) in the UK provides hemodialysis services through a network of renal units. However, resource constraints and waiting lists can sometimes delay access to treatment. The implementation of this approach requires specialized training for nephrologists and dialysis nurses, as well as careful monitoring of patients for potential complications. The cost of hemodialysis is also a significant factor, particularly in resource-limited settings.
Funding and Bias Transparency
The case report published in Cureus did not explicitly state any funding sources. However, it’s important to note that Cureus is an open-access journal that relies on article processing charges (APCs) paid by authors. While this doesn’t necessarily indicate bias, it’s a potential consideration. Research on hemodialysis technology is often funded by medical device manufacturers, such as Fresenius Medical Care and Baxter International. It’s crucial to critically evaluate any research funded by industry, considering potential conflicts of interest.
“The key to managing severe hyponatremia in AKI is a slow and controlled correction. Rapid correction can be devastating, leading to permanent neurological damage. Short intermittent hemodialysis allows us to achieve this control with a level of precision that’s difficult to obtain with other methods.” – Dr. Jennifer Smith, PhD, Renal Physiologist, University of California, San Francisco.
Key Data Summary: Hemodialysis Parameters
| Parameter | Value |
|---|---|
| Dialyzer Type | High-flux polysulfone membrane |
| Blood Flow Rate | 200-250 mL/min |
| Dialysate Flow Rate | 500 mL/min |
| Sodium Concentration in Dialysate | 135-140 mEq/L |
| Treatment Duration | 2-3 hours per session |
| Frequency | Daily or every other day |
Contraindications & When to Consult a Doctor
While short intermittent hemodialysis can be life-saving, it’s not appropriate for all patients. Contraindications include severe hypotension, uncontrolled bleeding, and active infection. Patients with pre-existing neurological conditions may also be at increased risk of complications. Individuals experiencing symptoms of hyponatremia – such as nausea, headache, confusion, muscle weakness, or seizures – should seek immediate medical attention. If you have kidney disease or are at risk for AKI, it’s important to discuss your risk factors with your doctor and follow their recommendations for monitoring and prevention. Do not attempt to self-treat hyponatremia, as this can be dangerous.
The successful application of short intermittent hemodialysis in this case offers a promising avenue for managing severe hyponatremia associated with anuric AKI. However, further research is needed to refine treatment protocols and identify patients who are most likely to benefit from this approach. Continued vigilance and a commitment to evidence-based medicine are essential to improving outcomes for patients with this challenging condition.
References
- Epstein, M., et al. (2018). Hyponatremia: Diagnosis and Management. Am J Kidney Dis, 71(5), 663–672. https://pubmed.ncbi.nlm.nih.gov/28480023/
- Liamis, G., et al. (2015). Hyponatremia in acute kidney injury: a systematic review. J Am Soc Nephrol, 26(10), 2413–2422. https://jasn.asnjournals.org/content/26/10/2413
- National Kidney Foundation. (n.d.). Acute Kidney Injury. https://www.kidney.org/atoz/content/aki
- WHO. (2023). Electrolyte Imbalances. https://www.who.int/news-room/q-a-detail/electrolyte-imbalances