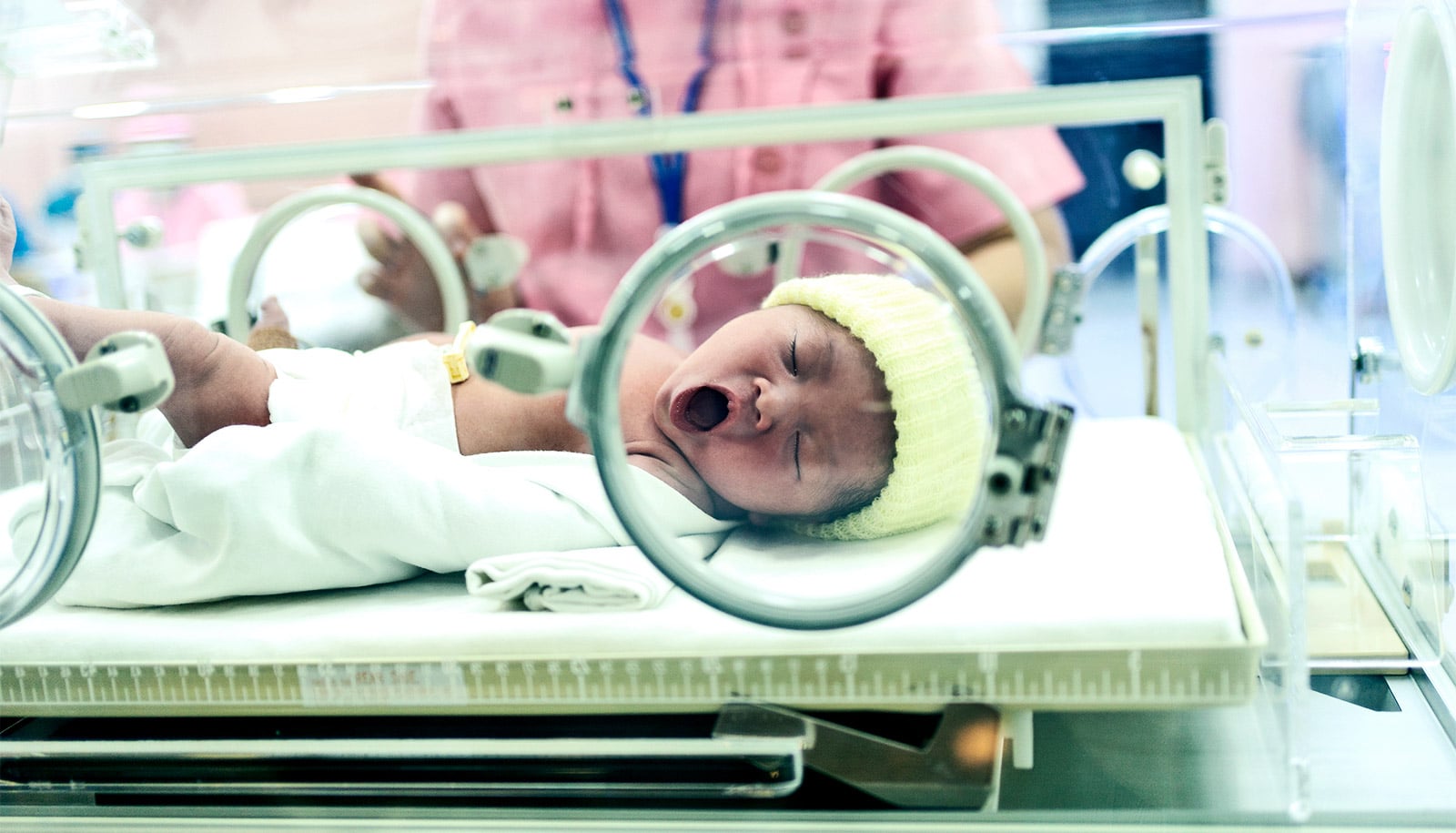
A decade-long study of 380,000 U.S. Births reveals that infants born to lower-income families face significantly higher risks of preterm birth and low birthweight. Published this week in JAMA Pediatrics, the research highlights a widening disparity in low birthweight incidence, driven by systemic financial instability and inadequate social safety nets.
This data represents more than just a statistical trend; This proves a clinical alarm. When we discuss “birth outcomes,” we are talking about the foundational biological trajectory of a human being. The correlation between socioeconomic status and neonatal health is not merely a matter of “better” doctors, but a reflection of how chronic environmental stress alters maternal physiology and fetal development.
In Plain English: The Clinical Takeaway
- The Income Gap: Families living below 200% of the federal poverty level observe significantly higher rates of babies born too early or too small.
- Worsening Trends: While most health gaps remained steady, the rate of low birthweight is increasing faster for low-income mothers than for wealthy ones.
- Beyond the Clinic: Medical care alone cannot fix this; factors like housing stability and food security are just as critical as prenatal vitamins.
The Epigenetic Toll: How Poverty “Gets Under the Skin”
To understand why income dictates birthweight, we must look at the mechanism of action—the specific biological process—of chronic stress. When a pregnant person experiences prolonged financial instability, the body maintains a state of hyper-arousal, flooding the system with cortisol, the primary stress hormone.
In a healthy pregnancy, the placenta regulates the transfer of nutrients and hormones. However, chronic stress can trigger an inflammatory response that affects the placental perfusion (the flow of blood to the placenta). This restriction limits the delivery of oxygen and essential nutrients to the fetus, leading to Intrauterine Growth Restriction (IUGR), where the baby does not reach its biological growth potential.
Here’s an example of epigenetic modification—where environmental factors “switch” certain genes on or off without changing the DNA sequence itself. For a baby born with low birthweight, this can manifest as a predisposition to metabolic syndrome, type 2 diabetes, and cardiovascular disease in adulthood, a phenomenon known as the Barker Hypothesis.
Analyzing the Decade of Divergence (2012–2022)
The study’s reliance on the CDC’s Pregnancy Risk Assessment Monitoring System (PRAMS) provides a robust longitudinal view. The most alarming finding is the divergence in low birthweight statistics. While the increase for higher-income families was marginal, the jump for lower-income families suggests a systemic failure in the American social safety net.
| Income Group | Low Birthweight (2012) | Low Birthweight (2022) | Percentage Increase |
|---|---|---|---|
| Lower-Income (<200% Poverty Level) | 7.2% | 9.4% | ~30.5% |
| Higher-Income | 5.7% | 6.3% | ~10.5% |
This data suggests that the “floor” for the most vulnerable is dropping. When we see a 30% increase in low birthweight within a specific demographic, we are witnessing a public health crisis that transcends the walls of the obstetric clinic.
Geo-Epidemiological Bridging: The Global Context
While this study focuses on the United States, the trend mirrors global disparities observed by the World Health Organization (WHO). In the UK, the NHS manages these disparities through more integrated social care, yet “postcode lotteries” still exist where maternal mortality and preterm birth rates vary by region.
In the US, the lack of a nationalized maternity care system means that access to double-blind placebo-controlled trials for new prenatal interventions is often skewed toward those with private insurance. This creates a “knowledge gap” where the most effective interventions for high-risk, low-income pregnancies are under-researched or poorly implemented due to lack of funding for community-based clinics.
“The intersection of poverty and maternal health is not a medical failure, but a policy failure. We cannot treat a preterm birth in the NICU and then send the mother back to a food-insecure home and expect the cycle to break.” — Dr. Sarah G. Miller, Epidemiologist and Maternal Health Consultant
Funding, Bias, and the Threat to Data Integrity
Transparency is the bedrock of medical journalism. This research was supported by grants from the National Institutes of Health (NIH), a federal agency. Because the funding is public and the data comes from the CDC’s PRAMS, the risk of corporate pharmaceutical bias is low. However, there is a significant “data bias” risk: the shuttering of the PRAMS office in early 2025.
Without PRAMS, the medical community loses its primary lens into the social determinants of health (SDOH). If we stop measuring the impact of poverty on birth, we effectively stop acknowledging it as a clinical variable. This “data blackout” could lead to a decade of stagnation in maternal health policy.
Contraindications & When to Consult a Doctor
While this article discusses population-level data, individual patients must prioritize clinical guidance. If you are pregnant and experiencing the following, seek immediate medical attention:
- Reduced Fetal Movement: A noticeable decrease in the baby’s activity levels.
- Preeclampsia Signs: Sudden swelling in the face or hands, severe headaches, or blurred vision.
- Preterm Labor: Contractions or pelvic pressure before 37 weeks of gestation.
Patients facing financial hardship should not avoid prenatal care. Many clinics offer sliding-scale fees or assistance through Medicaid to ensure that contraindications (factors that make a specific treatment inadvisable) are managed early in the pregnancy.
The Path Forward: Social Policy as Clinical Intervention
The conclusion is clear: the stethoscope cannot cure poverty. To move the needle on preterm births and low birthweight, the medical community must advocate for “social-policy-as-health-policy.” This includes expanded WIC (Women, Infants, and Children) benefits, universal basic income pilots for expectant mothers, and stable housing initiatives.
Until the environment in which a mother lives is as prioritized as the medicine she takes, the gap in birth outcomes will continue to widen. We must treat the zip code with the same urgency we treat the blood pressure.
References
- JAMA Pediatrics – Primary Study Source
- Centers for Disease Control and Prevention (CDC) PRAMS
- PubMed (National Library of Medicine) – Epigenetics and Maternal Stress
- World Health Organization (WHO) – Neonatal Health Guidelines