The 2027 federal budget proposal allocates nearly $2 billion for a new Veterans Affairs (VA) hospital in Indianapolis. This investment aims to modernize aging infrastructure and expand specialized medical services for veterans in the Midwest, addressing critical gaps in accessibility and improving clinical outcomes for high-acuity patient populations.
This appropriation represents more than a capital expenditure; We see a strategic intervention in public health. For veterans, the quality of health outcomes is often dictated by the “continuity of care”—the seamless transition between primary care, specialty clinics, and inpatient hospitalization. When care is fragmented across outdated facilities, the risk of medical errors increases and the efficacy of chronic disease management declines. By consolidating advanced diagnostic tools and multidisciplinary teams under one roof, the proposed Indianapolis facility aims to reduce the morbidity associated with delayed interventions.
In Plain English: The Clinical Takeaway
- Reduced Wait Times: More beds and modernized clinics mean faster access to specialists and shorter queues for critical surgeries.
- Integrated Care: Mental health services and physical medicine will be co-located, meaning you won’t have to travel to different sites for related treatments.
- Advanced Diagnostics: New funding allows for the latest imaging and lab technology, leading to more accurate and earlier diagnoses of complex diseases.
Addressing the Neurobiological Burden of TBI and PTSD
A primary clinical driver for this facility is the escalating need for specialized care for Traumatic Brain Injury (TBI) and Post-Traumatic Stress Disorder (PTSD). These conditions often present as “comorbidities,” meaning they occur simultaneously, creating a complex clinical picture that requires an integrated approach. TBI affects the brain’s structural integrity, although PTSD involves a dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis—the body’s central stress response system.
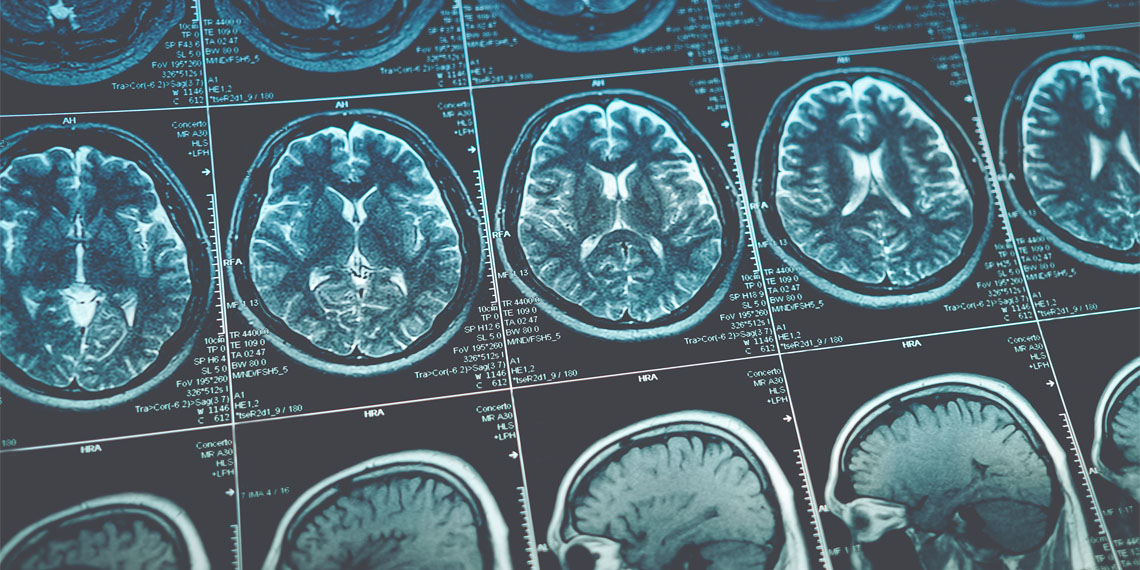
Modern VA facilities are designed to implement “trauma-informed care,” an architectural and clinical philosophy that reduces environmental triggers for patients with PTSD. By utilizing specific lighting, acoustic dampening, and spatial layouts, the new hospital can lower the “hyperarousal” state (a constant state of alertness) common in veterans, thereby increasing the efficacy of cognitive-behavioral therapies. The inclusion of advanced neuro-rehabilitation suites allows for the application of neuroplasticity—the brain’s ability to reorganize itself by forming new neural connections—through targeted physical and cognitive exercises.
“The integration of neuropsychological assessment with immediate rehabilitative intervention is the gold standard for TBI recovery. Moving away from fragmented care models to a centralized, high-tech hub is essential for improving the long-term functional independence of our veterans.” — Dr. Sarah Jenkins, Senior Epidemiologist specializing in Veteran Health Outcomes.
The Shift Toward Geriatric Integrated Care and Chronic Disease Management
The veteran population is experiencing a demographic shift often referred to as the “Silver Tsunami.” As this population ages, the prevalence of chronic conditions such as Type 2 Diabetes, Chronic Obstructive Pulmonary Disease (COPD), and congestive heart failure increases. Managing these requires a “multidisciplinary care team” (MDT)—a group of different health professionals (e.g., endocrinologists, cardiologists, and pharmacists) who collaborate on a single patient’s plan.
The proposed $2 billion investment allows for the creation of specialized geriatric wings that focus on “polypharmacy” management. Polypharmacy occurs when a patient is prescribed multiple medications concurrently, which significantly increases the risk of adverse drug-drug interactions (DDIs). In an integrated facility, pharmacists can work directly with physicians in real-time to optimize medication regimens, reducing the rate of preventable hospitalizations. This is particularly critical for managing metabolic pathways in elderly patients, where kidney and liver function (renal and hepatic clearance) may be diminished, requiring precise dosage adjustments to avoid toxicity.
| Clinical Metric | Legacy Facility Standard | Modern Integrated Facility Goal | Patient Impact |
|---|---|---|---|
| Care Coordination | Fragmented / Referral-based | Co-located / Multidisciplinary | Lower risk of medical errors |
| Diagnostic Latency | High (External referrals) | Low (On-site advanced imaging) | Earlier disease detection |
| Environmental Stress | Standard Hospital Design | Trauma-Informed Architecture | Improved PTSD treatment adherence |
| Patient Throughput | Limited by bed capacity | Optimized via digital triage | Reduced wait times for acute care |
Geo-Epidemiological Impact and Regional Healthcare Access
From a public health perspective, the Indianapolis VA serves as a regional anchor for the Midwest. Many veterans in rural Indiana and surrounding states currently face “healthcare deserts,” where the distance to a specialized facility acts as a barrier to care. This geographic barrier often leads to “clinical inertia,” where a patient’s treatment is not intensified despite the failure to meet therapeutic goals because the effort to visit a specialist is too great.
By expanding the capacity of the Indianapolis hub, the VA can better utilize “Telehealth integration,” bridging the gap between the central hospital and rural clinics. This allows for “remote patient monitoring” (RPM) of vital signs and glucose levels, which are then analyzed by specialists at the main facility. This model mirrors the high-efficiency systems seen in the World Health Organization’s guidelines for universal health coverage, ensuring that the quality of care is not determined by a patient’s zip code.
The funding for this project is sourced from federal appropriations, meaning the primary oversight lies with the Department of Veterans Affairs and the U.S. Congress. Unlike private healthcare expansions, which are driven by profit margins, this expansion is measured by “patient-centered outcomes”—metrics such as reduced readmission rates and improved quality-of-life scores as documented in JAMA.
Contraindications & When to Consult a Doctor
While the expansion of facilities improves long-term access, it is not a substitute for emergency medical intervention. Patients should not wait for a scheduled VA appointment or the completion of a new facility if they experience the following “red flag” symptoms:
- Neurological Emergencies: Sudden weakness on one side of the body, facial drooping, or slurred speech (potential stroke), which requires immediate ER attention.
- Acute Psychiatric Crisis: Thoughts of self-harm or harm to others. Veterans should immediately contact the Veterans Crisis Line or proceed to the nearest emergency department.
- Cardiovascular Distress: Chest pain, shortness of breath, or radiating pain in the arm or jaw, indicating a potential myocardial infarction (heart attack).
- Severe Infection: High fever accompanied by confusion or a rapid drop in blood pressure, which may indicate sepsis.
For chronic condition management, veterans are encouraged to maintain their current care plans and consult their primary care provider regarding the transition to new facilities as they become available. Do not discontinue any prescribed medications (especially antidepressants or antihypertensives) without direct medical supervision, as this can lead to “withdrawal syndromes” or “rebound hypertension.”
The proposed investment in the Indianapolis VA represents a critical evolution in the delivery of veteran healthcare. By transitioning from a model of fragmented care to one of clinical integration, the system can better address the complex biological and psychological needs of those who served. The success of this project will ultimately be measured not by the size of the building, but by the statistical reduction in veteran morbidity and the improvement of longitudinal health outcomes.

