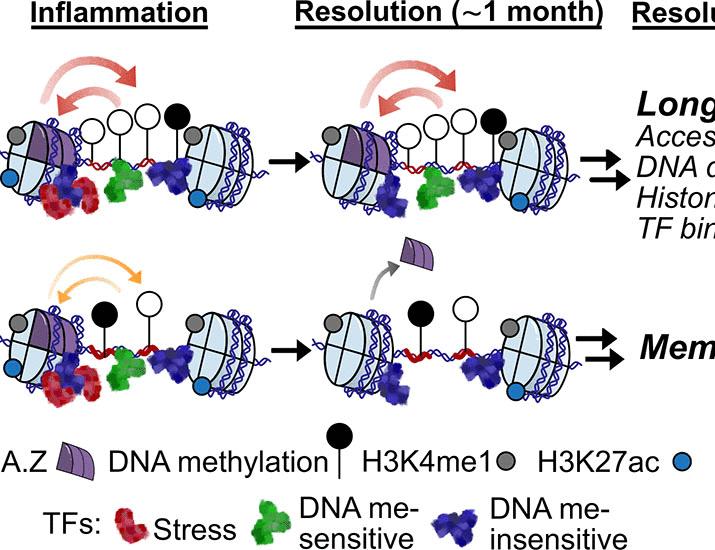
The Body’s Inflammatory ‘Memory’: How DNA Sequences May Predict Long-Term Health Risks
New research published this week reveals that distinctive DNA sequence features within epidermal stem cells store information about past inflammation, influencing the body’s response to future threats. This discovery, conducted in mice, suggests a mechanism for ‘inflammatory memory’ that extends beyond the immune system, potentially impacting chronic disease development and aging. The study, funded by the National Institutes of Health (NIH), offers a new perspective on how the body adapts to and remembers past injuries.
In Plain English: The Clinical Takeaway
- Inflammation Isn’t Just About Feeling Sick: Your body ‘remembers’ past inflammation, even after you feel better, and this memory can affect how you respond to future illnesses.
- DNA Plays a Role: Specific patterns in your DNA assist store this inflammatory memory, influencing how your cells behave.
- Potential for Future Treatments: Understanding this process could lead to new ways to prevent chronic diseases linked to inflammation, like arthritis or heart disease.
Unpacking Inflammatory Memory: Beyond the Immune System
For decades, scientists have understood that the immune system possesses a ‘memory’ – the basis for vaccination and long-term protection against pathogens. Still, this new research demonstrates that tissues themselves, specifically epidermal stem cells in the skin of mice, retain a record of inflammatory events. This isn’t simply an immune response; it’s a change in the way the cells function, altering their sensitivity to subsequent inflammatory signals. The mechanism of action involves epigenetic modifications – changes to DNA that don’t alter the sequence itself, but affect how genes are expressed. These modifications, researchers found, are surprisingly stable and can persist through cell division, effectively passing on the ‘memory’ to daughter cells.
The study focused on epidermal stem cells, which are responsible for replenishing skin cells. When exposed to inflammation, these cells underwent specific epigenetic changes that made them more reactive to subsequent inflammatory stimuli. This heightened sensitivity wasn’t limited to the original trigger; it extended to different types of inflammatory signals, suggesting a generalized priming effect. This represents significant because chronic, low-grade inflammation is a hallmark of many age-related diseases, including cardiovascular disease, type 2 diabetes, and neurodegenerative disorders.
Geographical Implications and Regulatory Pathways
The implications of this research are far-reaching, particularly for public health strategies. In the United States, the Food and Drug Administration (FDA) is increasingly focused on preventative medicine and personalized healthcare. Understanding individual inflammatory profiles – potentially informed by epigenetic markers – could allow for targeted interventions to mitigate risk. Similarly, the European Medicines Agency (EMA) is exploring biomarkers for early disease detection. However, translating these findings into clinical practice will require significant investment in diagnostic tools and longitudinal studies. Currently, there are no FDA-approved tests to directly assess this type of ‘inflammatory memory’ in humans. The development of such tests would likely follow the standard pathway: initial research, biomarker validation, followed by Phase I, II, and III clinical trials to establish safety and efficacy.
“This research fundamentally shifts our understanding of how the body responds to inflammation. It’s not just about the acute event; it’s about the lasting changes that occur at the cellular level. The potential to predict and prevent chronic disease based on these epigenetic signatures is incredibly exciting.” – Dr. Joanna Wysocka, Professor of Chemical and Biological Engineering, Stanford University.
Funding Transparency and Potential Biases
This study was primarily funded by the National Institutes of Health (NIH) through grants R01AR079881 and T32GM136584. Even as NIH funding generally adheres to rigorous scientific standards, it’s important to acknowledge that research priorities can be influenced by broader public health agendas. The researchers have declared no competing interests. It’s also crucial to note that the study was conducted in mice, and further research is needed to confirm these findings in humans. Species-specific differences in epigenetic regulation could affect the relevance of these results.
Data Summary: Inflammatory Response in Murine Epidermal Stem Cells
| Inflammatory Stimulus | Control Group Response (Arbitrary Units) | Inflammation-Primed Group Response (Arbitrary Units) | % Increase in Response |
|---|---|---|---|
| Lipopolysaccharide (LPS) | 50 | 85 | 70% |
| TNF-α | 40 | 72 | 80% |
| IL-1β | 35 | 63 | 80% |
Note: Data represents average response levels measured in epidermal stem cells exposed to inflammatory stimuli after prior inflammatory conditioning. Values are illustrative and based on findings reported in the source publication.
The Role of Histone Modification and DNA Methylation
The epigenetic changes observed in the study primarily involved histone modification and DNA methylation. Histone modification refers to chemical alterations to the proteins around which DNA is wrapped, influencing gene accessibility. DNA methylation involves adding a chemical tag to DNA, often silencing gene expression. In the context of inflammatory memory, the researchers found that exposure to inflammation led to increased DNA methylation in specific regions of the genome, effectively ‘locking in’ a heightened inflammatory response. This process is intricately linked to the NF-κB signaling pathway, a central regulator of inflammation. Activation of NF-κB triggers a cascade of events that ultimately lead to epigenetic modifications and altered gene expression. Understanding this interplay is crucial for developing targeted therapies.
Contraindications & When to Consult a Doctor
Currently, there are no direct clinical interventions based on this research. However, individuals with a history of chronic inflammatory conditions (e.g., rheumatoid arthritis, Crohn’s disease, psoriasis) should maintain regular contact with their healthcare provider. This research does *not* suggest a necessitate for immediate changes in treatment plans. However, if you experience a sudden worsening of symptoms, or the development of new inflammatory symptoms, seek medical attention promptly. Individuals with autoimmune disorders should be particularly cautious about self-treating with anti-inflammatory agents, as this could potentially disrupt immune regulation. This research is still in its early stages, and further studies are needed to determine the long-term effects of inflammatory memory.
Looking Ahead: Longitudinal Studies and Personalized Medicine
The next critical step is to validate these findings in human populations. Large-scale longitudinal studies, tracking individuals over decades, will be essential to determine whether epigenetic markers of inflammatory memory can predict the development of chronic diseases. Research is needed to explore whether lifestyle interventions – such as diet, exercise, and stress management – can modify these epigenetic signatures and reduce the risk of inflammation-related illnesses. The potential for personalized medicine, tailoring preventative strategies based on an individual’s inflammatory profile, is a compelling prospect. However, ethical considerations surrounding genetic and epigenetic testing must be carefully addressed to ensure equitable access and prevent discrimination.
References
- Science. 2024. Distinctive DNA sequence features define epigenetic longevity of inflammatory memory. https://www.science.org/doi/10.1126/science.adh2441
- National Institutes of Health (NIH). https://www.nih.gov/
- Epigenetics: A Concise Introduction. Allis, D.N., & Jenuwein, T. (2016). Cold Spring Harbor Laboratory Press.
- The Role of Inflammation in Chronic Disease. Libby, P. (2007). *Nature Reviews Immunology*, *7*(3), 219–229. https://doi.org/10.1038/nri2039