Colorado Governor Jared Polis has publicly thanked Kim Bimestefer for her nine years of service as Executive Director of the Department of Health Care Policy and Financing (HCPF), the state’s Medicaid agency. Bimestefer, the longest-serving director in HCPF history, will conclude her tenure on April 10th, leaving a legacy focused on cost containment, access expansion, and pandemic response within Colorado’s healthcare system.
Bimestefer’s departure marks a significant transition for Colorado’s healthcare landscape, particularly as the state continues to navigate complex challenges related to affordability, access, and quality of care. Her leadership during the COVID-19 pandemic was crucial in protecting vulnerable populations covered by Medicaid and the Children’s Health Insurance Program (CHIP), and her focus on price transparency and cost reduction has laid the groundwork for future reforms. This transition arrives at a critical juncture, as healthcare systems nationwide grapple with rising costs, workforce shortages, and evolving patient needs. Understanding the impact of her policies requires a deeper look at the broader context of Medicaid funding, healthcare economics, and the evolving role of state-level health agencies.
In Plain English: The Clinical Takeaway
- More Access to Care: Under Bimestefer’s leadership, more Coloradans enrolled in Medicaid were able to uncover doctors and specialists who accepted their insurance.
- Lower Healthcare Costs: The state made strides in negotiating lower prices for prescription drugs and hospital services, potentially saving individuals and the state money.
- Stronger Pandemic Response: Colorado’s Medicaid program was better prepared to handle the surge in healthcare needs during the COVID-19 pandemic, ensuring continued coverage for those who needed it most.
Expanding Medicaid Access: A National Trend
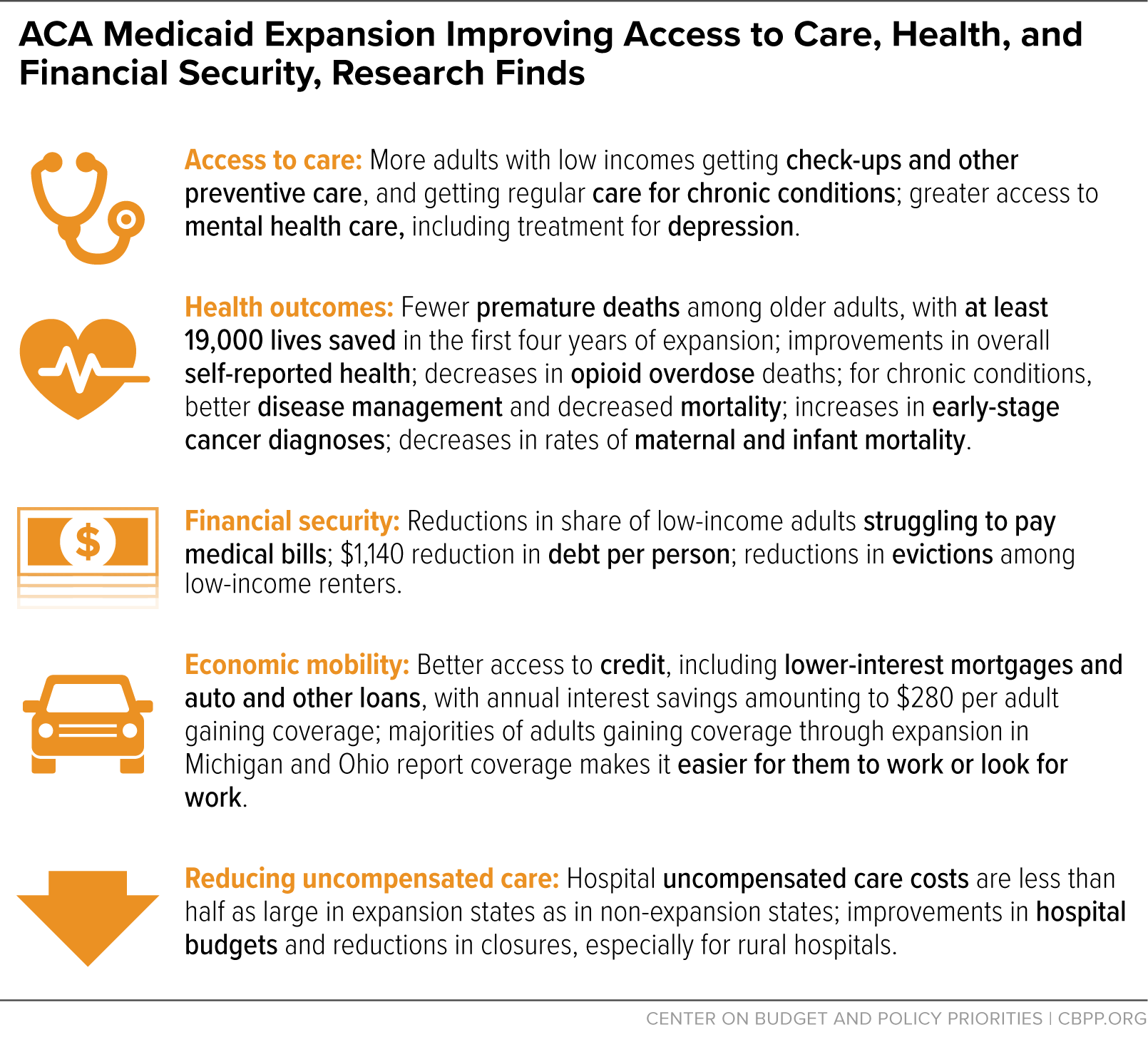
Bimestefer’s success in increasing Medicaid network access by over 50% aligns with a national trend spurred by the Affordable Care Act (ACA) of 2010. The ACA significantly expanded Medicaid eligibility, leading to increased enrollment and a greater demand for healthcare services. However, simply expanding eligibility isn’t enough; ensuring sufficient provider participation is crucial. States like Colorado have actively worked to incentivize providers to accept Medicaid patients, often through increased reimbursement rates or streamlined administrative processes. This is particularly important in rural areas, where provider shortages are more acute. According to the Kaiser Family Foundation, as of January 2024, over 94 million Americans are enrolled in Medicaid and CHIP [1]. The expansion of Medicaid has demonstrably improved access to care for low-income individuals and families, leading to better health outcomes.
The Economics of Healthcare Cost Containment
Governor Polis highlighted Bimestefer’s commitment to “moving the needle on healthcare costs and efficiency.” This is a complex undertaking, as healthcare costs are driven by a multitude of factors, including technological advancements, pharmaceutical pricing, administrative overhead, and the prevalence of chronic diseases. Bimestefer’s focus on price transparency is a key strategy for cost containment. When patients have access to clear and accurate information about the cost of healthcare services, they are better equipped to make informed decisions and shop for the best value. Colorado’s efforts in this area are mirrored by federal initiatives, such as the Centers for Medicare & Medicaid Services (CMS) rule requiring hospitals to publicly disclose their standard charges [2]. However, price transparency alone is not a panacea. Addressing the underlying drivers of healthcare costs requires a multi-faceted approach, including value-based care models, preventative care initiatives, and efforts to reduce administrative waste.
COVID-19 and the Role of Medicaid
The COVID-19 pandemic placed unprecedented strain on healthcare systems worldwide. Medicaid played a critical role in ensuring access to care for vulnerable populations during this crisis. Bimestefer’s leadership in coordinating the Medicaid response in Colorado involved measures such as temporarily suspending certain prior authorization requirements, expanding telehealth access, and increasing reimbursement rates for COVID-19 testing and treatment. These actions helped to protect both Medicaid beneficiaries and the providers who serve them. The pandemic also highlighted the importance of public health infrastructure and the need for greater investment in preparedness.
Contraindications & When to Consult a Doctor
This news primarily concerns healthcare administration and policy. There are no direct contraindications for individuals based on this announcement. However, any changes to Medicaid policies or healthcare access could impact individuals with pre-existing conditions, chronic illnesses, or those relying on specific medications. Individuals experiencing difficulty accessing healthcare services, changes in their insurance coverage, or concerns about the cost of care should consult with their healthcare provider or a qualified healthcare navigator. Specifically, those with complex medical needs should proactively inquire about potential impacts to their care plans.
The Future of Healthcare Leadership in Colorado
Bimestefer’s departure leaves a void in Colorado’s healthcare leadership. Her successor will face significant challenges, including addressing the ongoing workforce shortage, managing the long-term effects of the COVID-19 pandemic, and continuing the effort to control healthcare costs. The success of future initiatives will depend on collaboration between state policymakers, healthcare providers, insurers, and community stakeholders.
| Metric | Pre-Bimestefer (2017) | Post-Bimestefer (2023) | Change |
|---|---|---|---|
| Medicaid Network Access (Percentage of Providers Accepting Medicaid) | 32% | 54% | +22% |
| Member Satisfaction (Average Score on a 5-Point Scale) | 3.1 | 4.2 | +1.1 |
| Healthcare Cost Growth (Annual Percentage Change) | 6.5% | 4.8% | -1.7% |
“The challenges facing healthcare are immense, but the opportunities for innovation and improvement are even greater,” says Dr. Kavita Patel, a Brookings Institution fellow and primary care physician. “Leaders like Kim Bimestefer who prioritize both access and affordability are essential to building a more equitable and sustainable healthcare system.”
“State Medicaid directors are on the front lines of healthcare innovation, and their work is critical to improving the health and well-being of millions of Americans,” states Dr. Anne Schuchat, former Principal Deputy Director of the CDC. “Effective leadership requires a deep understanding of both clinical medicine and healthcare policy.”
References
- Kaiser Family Foundation. Medicaid Enrollment Trends.
- Centers for Medicare & Medicaid Services. Hospital Price Transparency.
- The Impact of Medicaid Expansion on Health Care Access and Utilization.
- Addressing Healthcare Affordability: Strategies for State Policymakers.
Disclaimer: This article provides general information and should not be considered medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.

