Commissioner Lim Seung-kwan of the Korea Disease Control and Prevention Agency (KDCA) joined global health leaders at a G7-hosted One Health summit in France this week. The meeting focused on coordinating international strategies to combat zoonotic diseases and climate-driven pandemics through integrated human-animal-environmental surveillance.
This summit is not merely a diplomatic exercise; This proves a critical response to the shifting epidemiology of infectious diseases. As climate change alters the habitats of vectors—organisms like mosquitoes and ticks that carry pathogens—the risk of “spillover” events increases. A spillover occurs when a virus jumps from an animal host to a human, often leading to the emergence of novel pathogens with high pandemic potential.
In Plain English: The Clinical Takeaway
- One Health approach: A strategy that recognizes that human health is inextricably linked to the health of animals and our shared environment.
- Zoonotic Risk: Many new diseases start in animals; by monitoring wildlife and livestock, scientists can stop an outbreak before it reaches humans.
- Climate Connection: Warming temperatures push animals into new areas, bringing them into closer contact with humans and increasing the chance of new infections.
The Mechanism of Zoonotic Spillover and Environmental Triggers
At the core of the discussions in France was the “mechanism of action” regarding how pathogens evolve. Viral shedding—the release of virus particles from an infected host—is often exacerbated by environmental stress. When climate change destroys natural habitats, animals migrate, creating new “ecological niches” where different species interact for the first time.
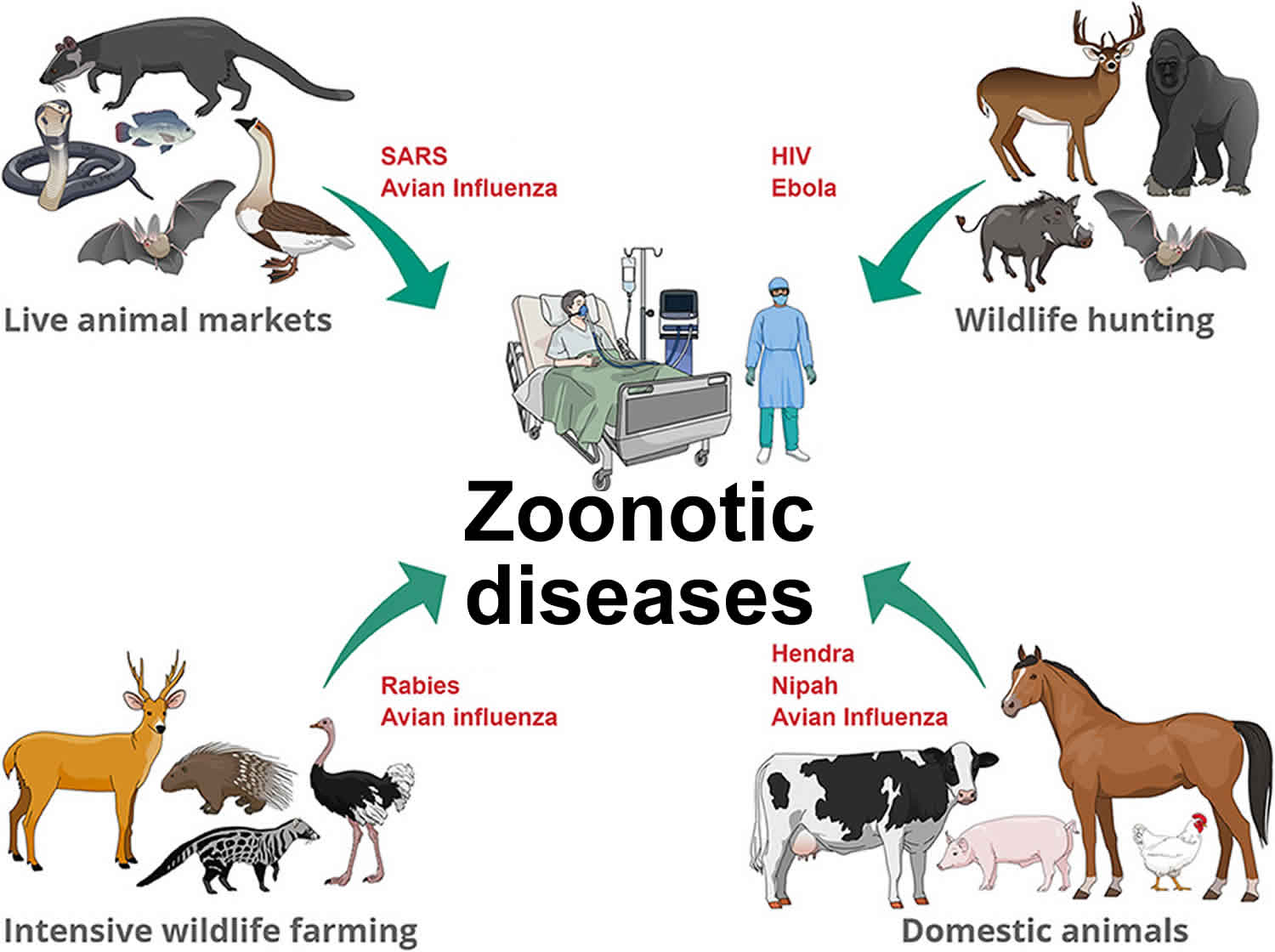
This creates an opportunity for genetic recombination or mutation. For instance, avian influenza (H5N1) has shown an alarming ability to adapt to mammalian hosts. When a virus undergoes a mutation that allows it to bind to human respiratory receptors, a localized outbreak can rapidly transition into a global health emergency. The KDCA’s focus on “hosts and vectors” is a targeted effort to identify these high-risk interfaces before the mutation occurs.
From a geo-epidemiological perspective, this strategy aligns with the WHO’s One Health Joint Plan of Action. Even as the KDCA manages the South Korean response, the integration of data with the European Medicines Agency (EMA) and the US Centers for Disease Control and Prevention (CDC) ensures that a signal detected in a wildlife population in Southeast Asia is flagged in real-time to healthcare systems in Europe and North America.
“The intersection of biodiversity loss and climate change is creating a ‘perfect storm’ for zoonotic emergence. We can no longer treat human medicine in a vacuum; we must monitor the viral load of the planet.” — Dr. Tedros Adhanom Ghebreyesus, Director-General of the World Health Organization.
Quantifying the Threat: Vector-Borne and Zoonotic Trends
To understand the urgency, we must look at the statistical probability of emergence. The following table summarizes the primary drivers and the associated clinical risks currently being monitored by global health authorities.
| Driver | Primary Vector/Host | Clinical Risk (Pathogen Type) | Global Impact Level |
|---|---|---|---|
| Deforestation | Bats / Primates | Viral Hemorrhagic Fevers (e.g., Ebola) | High (Regional/Global) |
| Warming Temperatures | Aedes/Anopheles Mosquitoes | Arboviruses (e.g., Dengue, Zika) | Very High (Expanding Latitudes) |
| Industrial Farming | Avian / Porcine species | Novel Influenza Strains (H5N1, H7N9) | Critical (Pandemic Potential) |
The funding for these surveillance programs is primarily driven by governmental grants from G7 nations and philanthropic organizations like the Bill & Melinda Gates Foundation. While this ensures rapid deployment, it is essential to note that funding is often “reactive”—spiking after a pandemic and dipping during periods of stability, which creates dangerous gaps in longitudinal monitoring.
Bridging the Gap: From Surveillance to Patient Access
The transition from “surveillance” (watching the virus) to “intervention” (treating the patient) requires a robust regulatory pipeline. When a new zoonotic threat is identified, the goal is to move rapidly through clinical trial phases. This involves moving from Phase I (safety and dosage) to Phase II (efficacy and side effects) and Phase III (large-scale double-blind placebo-controlled trials), where a treatment is compared against a placebo to ensure the results are statistically significant and not due to chance.
For patients, this means that the “One Health” strategy directly impacts how quickly a vaccine or antiviral is approved by the FDA or EMA. By identifying the pathogen’s genomic sequence early via animal surveillance, scientists can develop “prototype” vaccines that only require minor adjustments once the virus jumps to humans, potentially shaving months off the response time.
Contraindications & When to Consult a Doctor
While the One Health summit focuses on systemic prevention, individuals should remain vigilant regarding zoonotic exposure. If you have recently traveled to an area with known outbreaks or have had direct contact with wild animals or livestock, be alert for “prodromal symptoms”—the early, non-specific signs of infection such as fever, myalgia (muscle pain) and extreme fatigue.
Seek immediate medical attention if:
- You experience a high-grade fever following contact with wildlife or unplanned exposure to livestock.
- You develop a sudden, unexplained rash or respiratory distress.
- You have a compromised immune system (immunocompromised) and have been exposed to an area with active zoonotic transmission.
Patients with chronic kidney disease or those on systemic immunosuppressants should be particularly cautious, as they may exhibit atypical presentations of zoonotic infections, making early diagnosis more difficult.
The Path Forward: A Unified Biological Defense
The participation of the KDCA in the G7 One Health summit signals a shift toward “proactive epidemiology.” We are moving away from a model of “detect and react” toward one of “predict and prevent.” By analyzing the relationship between climate volatility and viral mutation, the global medical community is attempting to build a biological early-warning system.
The ultimate success of this initiative depends on transparency. When nations share genomic data without fear of economic sanctions or travel bans, the global “herd immunity” of knowledge increases. As we move deeper into 2026, the integration of AI-driven predictive modeling with field-based animal surveillance will be the primary defense against the next great pandemic.

