Lyme Disease: Understanding the Expanding Threat and Diagnostic Challenges
Lyme disease, a bacterial infection transmitted by ticks, is experiencing a concerning rise in incidence across North America and Europe. This week, attention was drawn to updates on CDC resources regarding the disease, prompting a critical review of its epidemiology, diagnostic hurdles, and evolving treatment strategies. The infection, caused by the bacterium Borrelia burgdorferi, can manifest in a wide range of symptoms, making early detection and intervention crucial.
In Plain English: The Clinical Takeaway
- Tick Checks are Vital: After spending time outdoors in wooded or grassy areas, thoroughly check yourself, your children, and your pets for ticks.
- Early Symptoms Matter: A characteristic “bullseye” rash (erythema migrans) is a key sign, but not everyone develops it. Flu-like symptoms should as well raise suspicion.
- Antibiotics are Effective: Lyme disease is typically treated with antibiotics, especially when caught early. Delaying treatment can lead to more serious complications.
The Expanding Geographic Range and Rising Incidence
Historically concentrated in the Northeastern and Mid-Atlantic regions of the United States, Lyme disease is now spreading geographically. The CDC reports a significant increase in cases in the upper Midwest and Pacific Coast states. This expansion correlates with the changing range of the black-legged tick (Ixodes scapularis) and the western black-legged tick (Ixodes pacificus), the primary vectors for the disease. Recent studies published in Emerging Infectious Diseases demonstrate a northward migration of these tick populations, driven by climate change and altered animal host distributions. CDC Lyme Disease Information
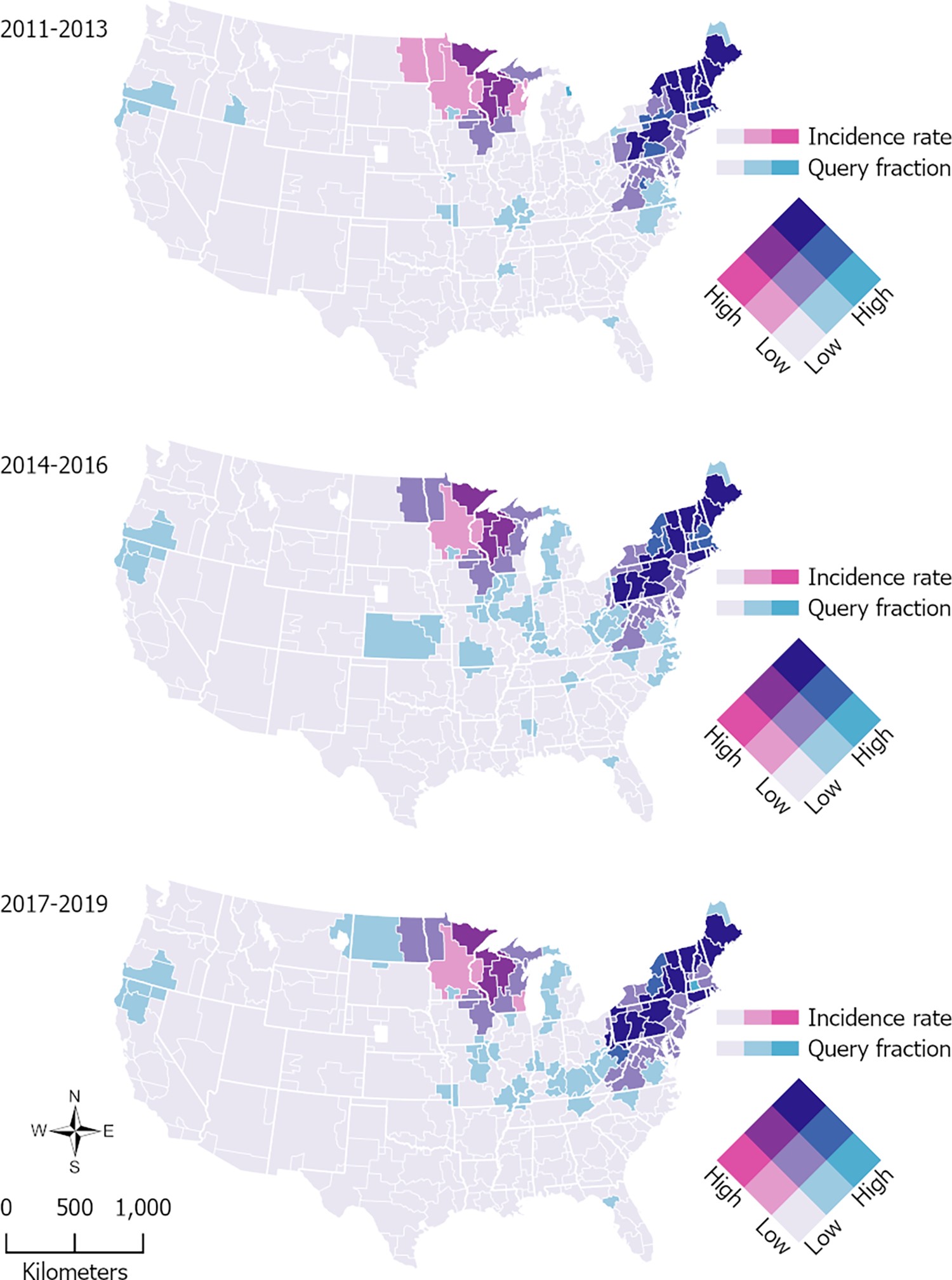
The increase in reported cases isn’t solely due to geographic expansion. Improved awareness among both the public and healthcare providers, coupled with more robust surveillance systems, contribute to higher detection rates. However, a significant underdiagnosis remains a concern, particularly in areas where Lyme disease is not traditionally considered endemic. The Centers for Disease Control and Prevention estimates that approximately 476,000 Americans are diagnosed with Lyme disease each year. CDC Lyme Disease Statistics
Diagnostic Challenges and the Role of Biomarkers
Diagnosing Lyme disease can be challenging due to the non-specific nature of early symptoms, which often mimic other illnesses like the flu or viral infections. The classic erythema migrans rash is pathognomonic – meaning it’s uniquely indicative of Lyme disease – but it only appears in 70-80% of infected individuals. Laboratory testing typically involves a two-tiered approach: an enzyme-linked immunosorbent assay (ELISA) to detect antibodies, followed by a Western blot to confirm positive ELISA results. However, these tests have limitations, particularly in the early stages of infection when antibody levels may be low.
Research is ongoing to identify more sensitive and specific biomarkers for early Lyme disease detection. One promising area of investigation focuses on detecting fragments of bacterial DNA (PCR) and identifying specific immune responses to Borrelia burgdorferi antigens. A study led by Dr. John Aucott at Johns Hopkins University is exploring the potential of using proteomics – the large-scale study of proteins – to identify unique protein signatures associated with persistent Lyme disease symptoms.
“We’re looking beyond just antibody detection to understand the complex immune dysregulation that occurs in some patients after Lyme disease treatment,” says Dr. Aucott. “Identifying these biomarkers could lead to more accurate diagnoses and personalized treatment strategies.”
Treatment Protocols and the Controversy Surrounding Persistent Symptoms
The standard treatment for Lyme disease is a course of antibiotics, typically doxycycline, amoxicillin, or cefuroxime axetil. Early treatment is highly effective in resolving the infection and preventing long-term complications. However, a subset of patients experience persistent symptoms – fatigue, joint pain, cognitive difficulties – even after completing antibiotic therapy. This condition, often referred to as “Post-Treatment Lyme Disease Syndrome” (PTLDS), remains poorly understood.
The optimal management of PTLDS is a subject of ongoing debate. Some clinicians advocate for prolonged antibiotic courses, although others emphasize symptomatic treatment and rehabilitation therapies. The Infectious Diseases Society of America (IDSA) guidelines recommend against prolonged antibiotic therapy for PTLDS, citing a lack of evidence of benefit and potential risks associated with long-term antibiotic employ. IDSA Lyme Disease Guidelines
| Treatment Phase | Antibiotic | Dosage (Adults) | Duration |
|---|---|---|---|
| Early Localized Lyme Disease | Doxycycline | 100mg twice daily | 10-21 days |
| Early Disseminated Lyme Disease | Amoxicillin | 500mg three times daily | 14-21 days |
| Late Disseminated Lyme Disease (e.g., Lyme Arthritis) | Cefuroxime Axetil | 500mg twice daily | 28 days |
Funding for Lyme disease research has historically been limited, hindering progress in understanding the disease and developing more effective treatments. The Bay Area Lyme Foundation, a non-profit organization, has played a crucial role in funding innovative research projects, including studies on biomarker discovery and novel therapeutic approaches. The foundation’s efforts are largely supported by private donations, highlighting the need for increased public funding for Lyme disease research.
Contraindications & When to Consult a Doctor
While Lyme disease is generally treatable, certain individuals should exercise extra caution. Pregnant women and individuals with compromised immune systems should seek immediate medical attention if they suspect a tick bite. Doxycycline, a commonly prescribed antibiotic, is contraindicated in pregnant women and children under the age of eight due to the risk of tooth discoloration. Consult a doctor immediately if you experience any of the following symptoms after a tick bite: fever, rash, headache, fatigue, muscle and joint aches, or neurological symptoms such as facial palsy or meningitis.
The evolving landscape of Lyme disease demands continued vigilance and a proactive approach to prevention. Understanding the risks, recognizing the symptoms, and seeking timely medical attention are essential for protecting yourself and your family from this increasingly prevalent infection. Further research is crucial to unravel the complexities of PTLDS and develop more effective strategies for managing this debilitating condition.
References
- Aucott, J. N., et al. “Post-treatment Lyme disease syndrome: a review of the literature and future research directions.” Expert Review of Anti-infective Therapy 11.6 (2013): 649-662.
- Adrion, E. M., et al. “Seroprevalence of Borrelia burgdorferi infection in the United States.” Vector-Borne and Zoonotic Diseases 18.1 (2018): 5-14.
- Centers for Disease Control and Prevention. “Lyme Disease.” https://www.cdc.gov/ticks/diseases/lyme.html
- Infectious Diseases Society of America. “Lyme Disease Guidelines.” https://www.idsociety.org/practice-guidelines/lyme-disease/

