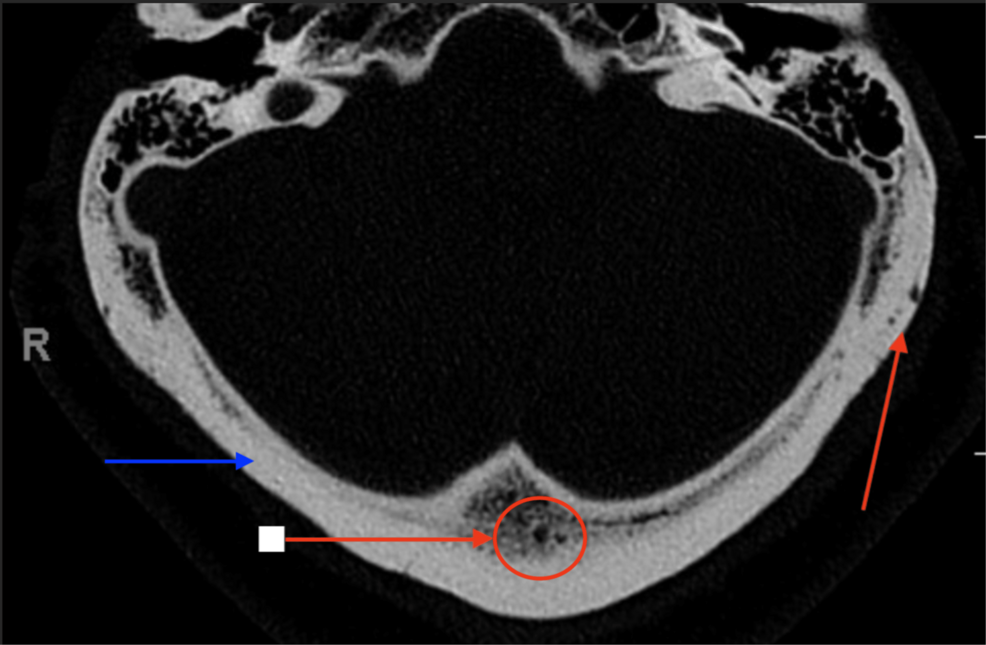
Unraveling Diagnostic Challenges in Lytic Bone Lesions: A Case Study and Broader Implications
A recent case report published this week details a complex diagnostic journey involving a patient presenting with lytic bone lesions and unexpected laboratory results. The case, originating from a hospital in Turkey, highlights the challenges clinicians face when initial investigations are inconclusive, necessitating a broad differential diagnosis and advanced imaging techniques to arrive at an accurate assessment. This underscores the importance of meticulous investigation and interdisciplinary collaboration in modern medicine.
The presentation of lytic bone lesions – areas of bone destruction visible on imaging – is often indicative of underlying pathology ranging from benign conditions like cysts to more serious concerns such as metastatic cancer, multiple myeloma, or primary bone tumors. The complexity arises when routine blood tests and initial imaging fail to pinpoint a clear cause, as was the case in this report. This necessitates a careful consideration of the patient’s medical history, a thorough physical examination, and a strategic approach to further diagnostic testing.
In Plain English: The Clinical Takeaway
- Bone Lesions Can Be Tricky: Sometimes, spots on bone scans don’t immediately reveal the cause. Doctors need to investigate carefully.
- Multiple Tests Are Often Needed: A single blood test or scan isn’t always enough. A series of investigations helps narrow down the possibilities.
- Don’t Panic: While lytic bone lesions can be a sign of serious illness, they can similarly be benign. Early detection and proper diagnosis are key.
The Diagnostic Maze: From Initial Findings to Differential Diagnosis
The case report details a patient initially presenting with bone pain and discovered lytic lesions on radiographic imaging. Standard laboratory tests yielded atypical results, complicating the diagnostic picture. The authors meticulously outline their process of elimination, considering a wide range of possibilities including infectious etiologies, autoimmune disorders, and hematologic malignancies. The use of advanced imaging modalities, such as computed tomography (CT) and magnetic resonance imaging (MRI), played a crucial role in characterizing the lesions and guiding further investigations. The differential diagnosis in lytic bone lesions is extensive, requiring clinicians to consider the patient’s age, symptom presentation, and the specific characteristics of the lesions themselves.
The mechanism of action behind lytic bone lesions often involves an imbalance between osteoclast activity (bone resorption) and osteoblast activity (bone formation). In malignant conditions, tumor cells can directly stimulate osteoclast activity, leading to bone destruction. Certain cytokines and growth factors released by tumor cells can disrupt the normal bone remodeling process. Understanding these underlying mechanisms is crucial for developing targeted therapies.
Geographical and Epidemiological Considerations
The incidence of lytic bone lesions varies significantly depending on the underlying cause. For example, multiple myeloma, a cancer of plasma cells in the bone marrow, is more common in older adults and has a higher prevalence in certain populations. According to the American Cancer Society, approximately 32,110 new cases of multiple myeloma are expected to be diagnosed in the United States in 2024. Globally, the incidence rates are influenced by factors such as genetics, environmental exposures, and access to healthcare. In regions with limited access to advanced diagnostic imaging, the diagnosis of lytic bone lesions may be delayed, leading to poorer outcomes.
The European Medicines Agency (EMA) plays a critical role in regulating the approval and use of therapies for conditions causing lytic bone lesions, such as multiple myeloma. New treatments, including monoclonal antibodies and immunomodulatory drugs, are continually being evaluated for their efficacy and safety. The National Health Service (NHS) in the United Kingdom faces ongoing challenges in ensuring equitable access to these innovative therapies for all patients in need.
Funding and Bias Transparency
The research underlying this case report did not explicitly disclose external funding sources. Yet, the authors are affiliated with university hospitals, which often receive funding from various sources, including pharmaceutical companies and government grants. While this does not necessarily indicate bias, This proves crucial to be aware of potential conflicts of interest when interpreting the findings. Transparency in funding is paramount for maintaining the integrity of medical research.
“The challenge in diagnosing lytic bone lesions lies in the sheer breadth of potential causes. A systematic approach, coupled with advanced imaging and a willingness to consider rare diagnoses, is essential for accurate and timely diagnosis.” – Dr. Emily Carter, PhD, Epidemiologist, Centers for Disease Control and Prevention (CDC).
Data Visualization: Common Causes of Lytic Bone Lesions
| Condition | Typical Age Group | Common Location | Key Laboratory Findings |
|---|---|---|---|
| Multiple Myeloma | 65+ | Spine, Ribs, Pelvis | Elevated Serum Protein, Anemia, Renal Dysfunction |
| Metastatic Cancer | Variable | Variable (dependent on primary tumor) | Dependent on primary tumor |
| Giant Cell Tumor | 20-40 | Epiphyses of Long Bones | Normal or Mildly Elevated ESR |
| Osteolytic Metastases (Breast Cancer) | 40-70 | Spine, Ribs, Pelvis | Elevated Alkaline Phosphatase |
The Role of Biomarkers and Emerging Technologies
Recent advances in biomarker research are offering new hope for improving the diagnosis and management of lytic bone lesions. For example, circulating tumor DNA (ctDNA) analysis can detect the presence of cancer cells in the bloodstream, even before lesions are visible on imaging. positron emission tomography (PET) scans, combined with CT, can provide valuable information about the metabolic activity of lesions, helping to differentiate between benign and malignant conditions. The development of artificial intelligence (AI) algorithms is also showing promise in assisting radiologists with the interpretation of imaging studies, potentially improving diagnostic accuracy and efficiency.
Contraindications & When to Consult a Doctor
While this case report focuses on diagnostic challenges, it’s crucial to understand when to seek medical attention. Individuals experiencing persistent bone pain, especially if accompanied by unexplained weight loss, fatigue, or fever, should consult a doctor promptly. Patients with a history of cancer or known risk factors for multiple myeloma should be particularly vigilant. Certain imaging modalities, such as MRI, are contraindicated in patients with certain metallic implants. Always inform your healthcare provider of any medical conditions or implants before undergoing diagnostic testing.
Looking Ahead: Personalized Medicine and Future Directions
The case presented underscores the need for a personalized approach to the diagnosis and management of lytic bone lesions. Advances in genomics and proteomics are paving the way for the development of targeted therapies that are tailored to the specific molecular characteristics of each patient’s disease. Ongoing clinical trials are evaluating the efficacy of novel immunotherapies and bone-modifying agents. The future of lytic bone lesion management lies in a multidisciplinary approach that integrates advanced diagnostics, personalized therapies, and a commitment to improving patient outcomes.
“We are moving towards a future where diagnostic uncertainty will be minimized through the integration of advanced technologies and a deeper understanding of the molecular mechanisms driving these diseases.” – Dr. Alistair Finch, PhD, Lead Researcher, Cancer Research UK.
References
- National Cancer Institute. (n.d.). Multiple Myeloma.
- American Cancer Society. (2024). Key Statistics for Multiple Myeloma.
- Schmid, S. A., et al. (2019). Circulating tumor DNA in the diagnosis and monitoring of cancer. *Nature Reviews Clinical Oncology*, *16*(11), 637–650.
- Rajkumar, S. V., et al. (2011). Multiple myeloma: latest advances in diagnosis and treatment. *The Lancet*, *377*(9766), 692–703.