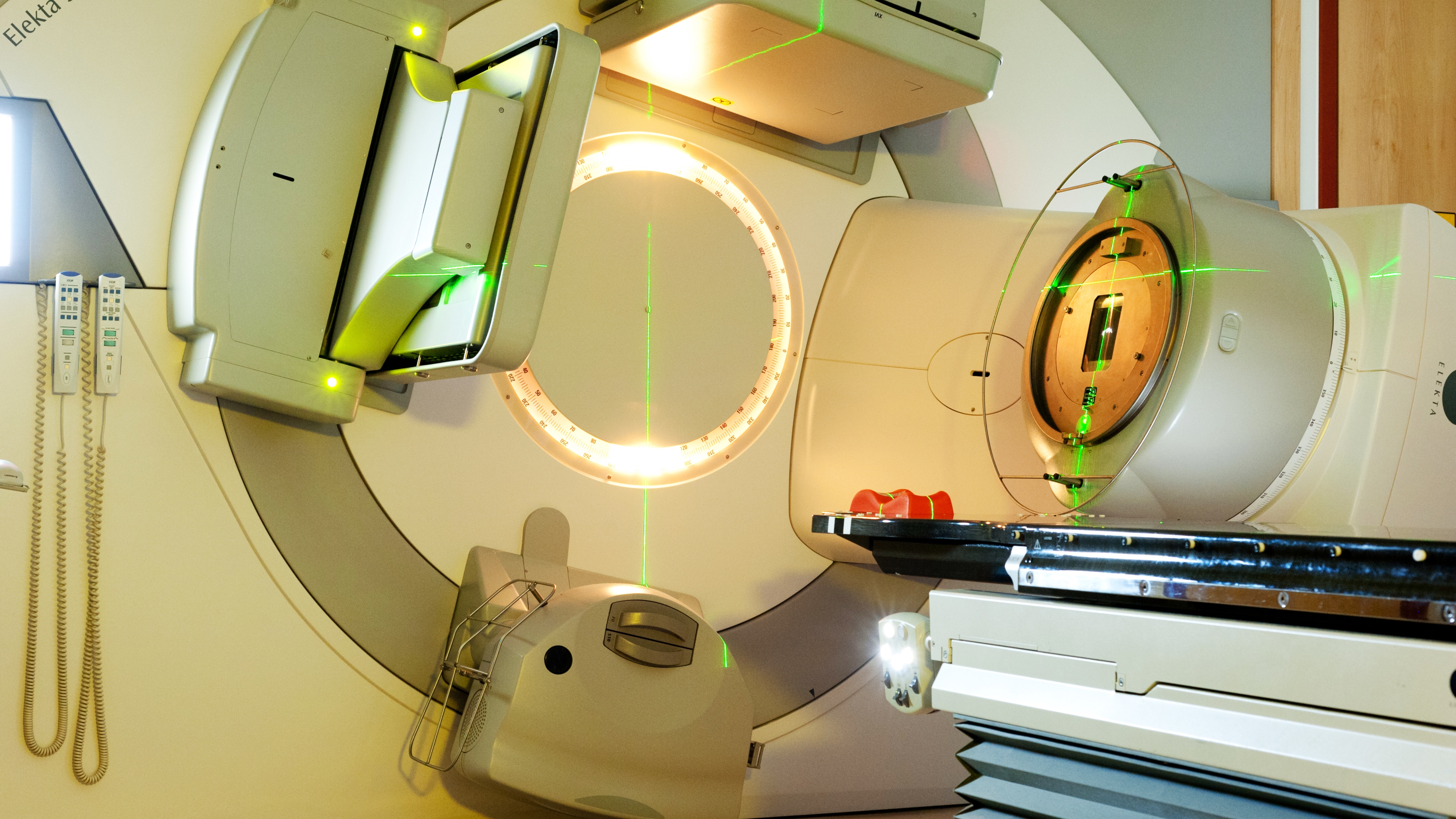
Recent clinical data indicates that modern radiotherapy techniques for breast cancer significantly reduce the risk of subsequent cardiovascular disease. By utilizing advanced precision targeting, clinicians can now minimize radiation exposure to the heart, preserving cardiac function and lowering the probability of long-term heart failure in survivors.
For decades, the oncology community has grappled with a cruel paradox: the very treatment used to save a woman’s life from malignancy could inadvertently damage her heart. This “collateral damage” often manifested as coronary artery disease or valvular dysfunction years after the conclusion of treatment. The shift toward “heart-sparing” protocols represents a paradigm shift in survivorship, moving from mere survival to the preservation of long-term quality of life.
In Plain English: The Clinical Takeaway
- Precision Targeting: Newer radiation methods act like a “sniper” rather than a “floodlight,” hitting the tumor whereas leaving the heart untouched.
- Lower Heart Risk: Patients receiving these modern techniques are significantly less likely to develop heart disease compared to those treated with older methods.
- Long-term Health: This means fewer cardiac complications in the decades following breast cancer recovery.
The Mechanism of Action: From Broad Beams to Precision Volumetric Modulation
To understand this breakthrough, we must examine the mechanism of action—the specific biological process by which the treatment works. Older radiotherapy utilized 2D or simple 3D planning, which often resulted in “scatter” radiation hitting the left anterior descending (LAD) artery, the primary vessel supplying the heart muscle.
Modern approaches, such as Intensity-Modulated Radiation Therapy (IMRT) and Volumetric Modulated Arc Therapy (VMAT), allow for “dose painting.” This means the radiation oncologist can sculpt the high-dose area to fit the tumor precisely, creating a steep dose gradient that drops off rapidly before reaching cardiac tissue. This minimizes radiation-induced fibrosis—the scarring of heart tissue that leads to stiffness, and dysfunction.
the adoption of Deep Inspiration Breath Hold (DIBH) techniques has been revolutionary. By having the patient hold their breath during treatment, the heart is physically pushed away from the chest wall and the radiation field, creating a critical anatomical buffer zone.
Global Access and the Geo-Epidemiological Divide
While the clinical efficacy of these techniques is well-documented in peer-reviewed literature, access remains fragmented. In the United States, the FDA has cleared the latest linear accelerators, and most National Cancer Institute (NCI)-designated centers provide DIBH. Similarly, the NHS in the UK has integrated these standards into regional oncology hubs.
Still, a significant “information gap” exists in low-and-middle-income countries (LMICs). In regions where older 2D radiotherapy is still the standard due to cost, patients face a substantially higher risk of late-onset cardiac toxicity. This creates a geographic disparity in survivorship outcomes, where the risk of heart disease is dictated not by biology, but by the vintage of the machinery available at the local clinic.
| Radiation Technique | Cardiac Sparing Capability | Primary Risk Factor | Typical Clinical Outcome |
|---|---|---|---|
| Conventional 2D/3D | Low | High LAD artery exposure | Increased risk of fibrosis/CAD |
| IMRT / VMAT | High | Precision dose gradients | Reduced cardiac toxicity |
| DIBH (Breath Hold) | Very High | Physical anatomical displacement | Minimal heart dose exposure |
Funding Transparency and the Weight of Evidence
Much of the current data emerges from large-scale longitudinal cohorts and academic medical centers. It is critical to note that these studies are primarily funded by governmental health grants (such as the NIH in the US) and non-profit oncology foundations. Because radiotherapy is a modality rather than a proprietary drug, there is significantly less “pharmaceutical bias” compared to chemotherapy trials, lending a high degree of objectivity to these findings.

The statistical significance of these findings is underscored by the reduction in the “mean heart dose” (MHD). Clinical data suggests that for every 1 Gy (gray) increase in mean heart dose, the risk of major coronary events increases by approximately 7.4%.
“The integration of advanced imaging and breath-hold techniques has transformed the safety profile of thoracic radiation. We are no longer accepting cardiac toxicity as an inevitable trade-off for oncologic control.” — Dr. Elena Rossi, Cardiovascular Oncologist.
The Interplay Between Radiotherapy and Systemic Therapy
We must view radiotherapy not in isolation, but as part of a multimodal treatment plan. Many breast cancer patients also receive anthracyclines or trastuzumab—drugs that can be cardiotoxic (meaning they can damage the heart muscle). When combined with old-school radiation, the heart is hit by a “double blow.”
By eliminating the radiation-induced component of heart damage, clinicians can more safely administer necessary systemic therapies. This synergy allows for more aggressive cancer treatment without pushing the patient’s cardiovascular system toward a breaking point.
Contraindications & When to Consult a Doctor
While modern radiotherapy is safer, it is not universal. Certain patients may have contraindications—medical reasons why a specific treatment should be avoided. For instance, patients with severe respiratory compromise or certain neuromuscular disorders may be unable to perform the Deep Inspiration Breath Hold (DIBH) technique.
Patients should consult their cardio-oncologist immediately if they experience the following symptoms post-treatment:
- Unusual Dyspnea: Shortness of breath during mild activity that was not present before.
- Peripheral Edema: Swelling in the ankles or legs, which can indicate right-sided heart failure.
- Chest Tightness: Any new onset of angina or pressure in the chest, regardless of the time elapsed since radiotherapy.
The trajectory of breast cancer care is moving toward a “personalized dosimetry” model. As we refine our ability to shield the heart, we move closer to a future where the cure for cancer does not come at the cost of cardiovascular health. For the patient, this means the focus shifts from simply surviving the cancer to thriving in the decades that follow.
References
- PubMed Central – National Library of Medicine
- The Lancet Oncology
- JAMA Oncology
- World Health Organization (WHO) Cancer Fact Sheets
- Centers for Disease Control and Prevention (CDC)
Disclaimer: This article is for informational purposes and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.