A municipality in Val-d’Oise, France, is expanding its primary care infrastructure by integrating a nurse and a pediatric dentist into an existing multidisciplinary team that includes a pulmonologist. This strategic expansion aims to eliminate “medical deserts,” ensuring residents access essential preventative and specialized care without traveling to distant urban centers.
This development is more than a local staffing update; it is a clinical intervention against the systemic crisis of healthcare accessibility. In the medical community, we refer to the absence of sufficient healthcare providers in specific geographic areas as “medical deserts.” When a community lacks primary care, patients often bypass preventative screenings and early interventions, leading to a higher incidence of advanced-stage diseases that require expensive, acute hospitalization. By establishing a multidisciplinary hub—where a pulmonologist, a nurse, and a pediatric dentist operate in proximity—the town is implementing a “coordinated care model.” This approach reduces the fragmented nature of medicine, allowing for seamless referrals and a holistic view of patient health.
In Plain English: The Clinical Takeaway
- Earlier Detection: Local access means diseases like asthma or childhood tooth decay are caught early, preventing long-term complications.
- Reduced ER Burden: When residents have a local nurse and specialist, they are less likely to utilize emergency rooms for non-urgent issues.
- Integrated Health: Having different specialists in one area allows them to communicate, ensuring your dental health and respiratory health are managed together.
The Oral-Systemic Link: Why Pediatric Dentistry is Critical
The addition of a pediatric dentist is a vital public health move. In clinical terms, we focus on the oral-systemic link—the proven relationship between oral health and overall systemic wellness. Pediatric dental caries (tooth decay) are not merely a cosmetic or localized issue; they are often indicators of nutritional deficiencies and can lead to systemic inflammation.
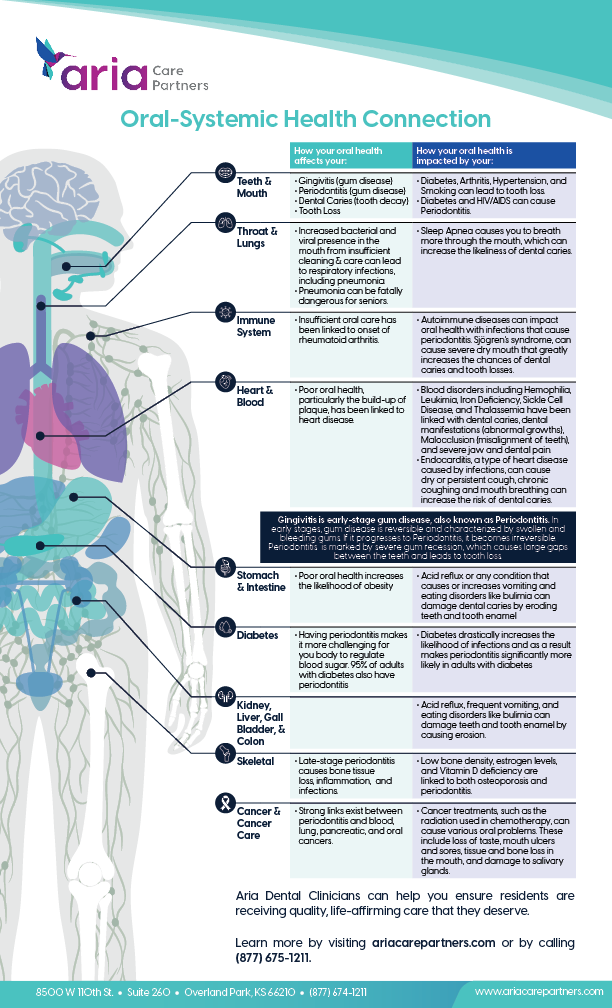
Early childhood caries can impair a child’s ability to eat and speak, which in turn affects cognitive development and nutritional uptake. Chronic oral infections can introduce bacteria into the bloodstream, potentially exacerbating other inflammatory conditions. By providing specialized pediatric care locally, the community reduces the “barrier to entry” for preventative sealant applications and fluoride treatments, which are the gold standard for preventing decay in developing dentitions.
“The integration of primary oral health care into general health services is essential for reducing health inequalities. When children have access to early dental intervention, we see a direct correlation in improved overall health outcomes and reduced school absenteeism.” — Dr. Maria Neira, Director of the Department of Environment, Climate Change and Health at the WHO.
Respiratory Health and the Urban-Periurban Interface
The presence of a pulmonologist—a physician specializing in the respiratory system—is particularly salient for the Val-d’Oise region. This area, situated on the periphery of the Paris metropolitan basin, is subject to specific environmental stressors, including particulate matter (PM2.5) and nitrogen dioxide (NO2).
The mechanism of action for these pollutants involves the inhalation of microscopic particles that penetrate deep into the alveoli (the tiny air sacs in the lungs), triggering an immune response and causing chronic inflammation of the bronchial tubes. This can lead to the exacerbation of Chronic Obstructive Pulmonary Disease (COPD) and asthma. Having a local pulmonologist allows for the implementation of longitudinal monitoring—tracking a patient’s lung function over years—rather than relying on episodic, emergency care. This shift from reactive to proactive respiratory management is the only way to significantly lower mortality rates associated with chronic lung disease.
Comparing Healthcare Delivery Models
To understand the impact of this expansion, we must compare the multidisciplinary model (like the one being built in Val-d’Oise) against traditional solo practices or hospital-centric care.
| Feature | Solo Practitioner | Hospital-Centric | Multidisciplinary Hub (MSP) |
|---|---|---|---|
| Patient Access | Limited by one provider’s hours | High barrier (ER/Appointment) | High (Diversified providers) |
| Care Coordination | Low (External referrals) | Moderate (Internal) | High (Immediate collaboration) |
| Preventative Focus | Variable | Low (Acute focus) | High (Screening focus) |
| Patient Travel | Moderate | High (Centralized) | Low (Local) |
Funding, Bias, and Regional Policy
The expansion of these medical offers in France is typically funded through a combination of state subsidies from the Agence Régionale de Santé (ARS) and private practitioner investments. These initiatives are designed to incentivize physicians to move away from saturated urban centers. While the goal is purely public health, the success of these hubs depends on the “retention rate” of the providers. If the infrastructure does not support the practitioners’ quality of life, the “medical desert” simply shifts elsewhere.
From a regulatory standpoint, this mirrors the “Primary Care Network” models used by the NHS in the UK or “Federally Qualified Health Centers” (FQHCs) in the United States. All three systems are attempting to solve the same epidemiological problem: the dangerous gap between the patient’s home and the first point of clinical contact. When this gap is bridged, we see a statistically significant decrease in “avoidable hospitalizations.”
Contraindications & When to Consult a Doctor
While the arrival of new providers is positive, patients must know when to seek immediate care versus scheduled appointments. The following guidelines apply to the services being added:
- Pediatric Dentistry: Schedule a visit immediately if a child exhibits “white spots” on teeth (early decalcification) or reports pain during eating. Contraindication: In cases of severe facial swelling or high fever associated with a tooth abscess, proceed directly to an emergency department to prevent sepsis.
- Pulmonology: Consult the pulmonologist for chronic cough, shortness of breath during mild exertion, or a history of smoking. Urgent Warning: Sudden onset of severe dyspnea (difficulty breathing) or bluish tint to the lips (cyanosis) is a medical emergency; do not wait for a clinic appointment.
- Nursing Care: Utilize the nurse for wound management, vaccination, and chronic disease monitoring (e.g., diabetes glucose checks).
The expansion of healthcare in Val-d’Oise represents a calculated move toward “health equity.” By decentralizing specialized care, the state reduces the socio-economic barriers that often prevent the most vulnerable populations from receiving timely treatment. The long-term success of this initiative will be measured not by the number of providers hired, but by the decrease in regional emergency admissions and the improvement in pediatric health indices over the next decade.

