Oregon health officials are urging unvaccinated residents to receive the MMR vaccine as measles cases rise across the state. This surge threatens the 2000 elimination status in the U.S., highlighting a critical gap in herd immunity and increasing the risk of community transmission across the Pacific Northwest.
The current situation in Oregon is a stark reminder that medical progress is not a linear trajectory. it is a maintained state. Measles is not merely a childhood rash but a systemic viral infection that exploits gaps in public health infrastructure. When vaccination rates dip below the critical threshold of 95%, the “firewall” of herd immunity—the point where enough people are immune to stop a virus from spreading—collapses. This leaves the most vulnerable, including infants too young for vaccination and the immunocompromised, at severe risk.
In Plain English: The Clinical Takeaway
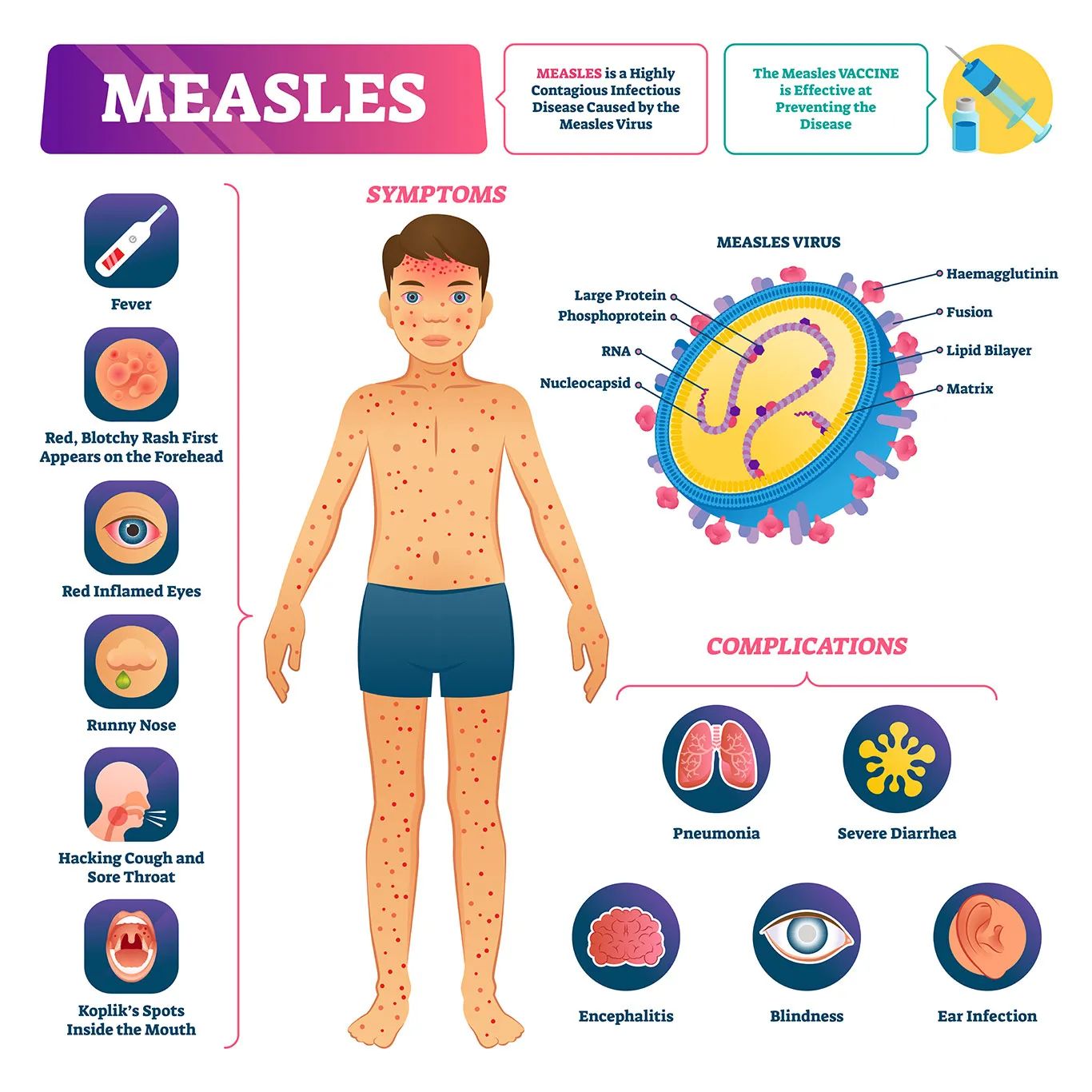
- Extreme Contagion: Measles is one of the most infectious diseases known; it can linger in the air for up to two hours after an infected person leaves a room.
- The Only Shield: There is no cure for measles. The MMR (Measles, Mumps, Rubella) vaccine is the only evidence-based method of prevention.
- Beyond the Rash: The virus can cause “immune amnesia,” effectively erasing the body’s memory of how to fight other previously conquered infections.
The Mechanism of Action: How the MMR Vaccine Works
The MMR vaccine utilizes a live-attenuated virus. In clinical terms, “attenuated” means the virus has been weakened in a laboratory setting so that it can no longer cause the disease in a healthy person, but it remains potent enough to trigger a primary immune response. This process mimics a natural infection without the associated pathology.
Once administered, the vaccine stimulates the production of neutralizing antibodies and activates T-lymphocytes. These cells create a “molecular memory” of the virus. If the individual is later exposed to the wild-type measles virus, the immune system recognizes the surface proteins—specifically the hemagglutinin protein—and neutralizes the pathogen before it can achieve systemic dissemination. This double-blind placebo-controlled efficacy is well-documented, with two doses providing approximately 97% lifelong protection for the vast majority of the population.
The Danger of Immune Amnesia and Systemic Impact
Although the immediate symptoms of measles—high fever, cough, and the characteristic maculopapular rash—are concerning, the most insidious effect is “immune amnesia.” Peer-reviewed research published in Science indicates that the measles virus targets memory B and T cells, the cells responsible for remembering previous infections.
Essentially, the virus “wipes the hard drive” of the immune system. This leaves a patient susceptible to bacteria and viruses they had already fought off years prior. This phenomenon explains why measles outbreaks are often followed by a spike in other respiratory and gastrointestinal infections. The funding for these longitudinal studies is primarily provided by government health agencies and non-profit academic institutions, ensuring that the data remains decoupled from pharmaceutical profit motives.
“Measles is a sentinel event. When we spot it return to a community, it is a signal that our collective immunity is fracturing, and the risk of secondary opportunistic infections increases for everyone, not just the unvaccinated.” — Dr. Ashish Jha, infectious disease expert and public health advisor.
Epidemiological Comparison: Measles vs. Other Respiratory Viruses
To understand why Oregon health officials are reacting with such urgency, one must look at the R0 (Basic Reproduction Number). The R0 represents the average number of people one infected person will infect in a completely susceptible population.
| Pathogen | Approximate R0 Value | Primary Transmission Route | Prevention Strategy |
|---|---|---|---|
| Seasonal Influenza | 1.3 – 1.8 | Droplet/Aerosol | Annual Vaccination |
| SARS-CoV-2 (Omicron) | 8.0 – 10.0 | Aerosol/Droplet | Vaccination/Masking |
| Measles (Rubeola) | 12.0 – 18.0 | Airborne (Aerosol) | MMR Vaccination |
Geo-Epidemiological Bridging: From Oregon to Global Systems
The rise in Oregon is not an isolated event but is linked to global migration and travel patterns. The World Health Organization (WHO) has noted a global decline in measles vaccination coverage, which creates “reservoirs” of the virus internationally. When an unvaccinated traveler imports the virus into a region with low local vaccination rates, the high R0 value leads to exponential growth.
In the United States, the CDC manages the surveillance, but the actual delivery of the vaccine falls to state health authorities like the Oregon Health Authority. This decentralized system can create disparities in patient access. While the vaccine is widely available, “vaccine deserts” in rural areas or systemic distrust in urban centers can lead to pockets of vulnerability, making these regions prime targets for outbreaks.
Contraindications & When to Consult a Doctor
While the MMR vaccine is exceptionally safe, it is not suitable for everyone. Contraindications—medical reasons why a particular treatment should not be used—include:
- Severe Allergic Reactions: Individuals with a known life-threatening allergy to neomycin or gelatin.
- Severe Immunosuppression: Patients undergoing chemotherapy or those with advanced HIV/AIDS should avoid live vaccines, as their immune systems cannot safely handle the attenuated virus.
- Pregnancy: The MMR vaccine is generally avoided during pregnancy as a precautionary measure.
Try to seek immediate medical attention if you or your child exhibit the following “red flag” symptoms:
- Koplik Spots: Tiny white spots inside the cheeks (a pathognomonic sign, meaning it is specifically characteristic of measles).
- High Fever: A temperature exceeding 103°F (39.4°C) accompanied by a cough.
- Neurological Changes: Extreme lethargy, confusion, or a stiff neck, which may indicate encephalitis (inflammation of the brain).
The Path Forward: Restoring Public Trust
The climb in measles cases in Oregon is a clinical failure of prevention, not a failure of the vaccine itself. The science remains robust: the MMR vaccine is highly effective and has saved millions of lives globally. The challenge now is translational—moving the evidence from the peer-reviewed journal to the clinic and the community.
As we move further into 2026, the priority must be the restoration of herd immunity. This requires transparent communication regarding the risks of the virus versus the negligible risks of the vaccine. For the vast majority of the population, the statistical probability of a severe adverse reaction to the vaccine is infinitesimally lower than the risk of complications from a wild-type measles infection.

