South Korean entertainer Park Semi recently revealed her plans to conceive, including a chosen name for her future daughter, “Yua,” and a reported practice of performing handstands to potentially aid conception. This disclosure, made on the ‘Rolling Thunder’ channel, has sparked public interest, prompting a closer examination of the physiological factors influencing fertility and the scientific basis – or lack thereof – behind such practices.
The public discussion surrounding Park Semi’s announcement highlights a broader societal trend of openly discussing family planning, and fertility. However, it also underscores a critical need for evidence-based information regarding conception, particularly as misinformation can proliferate rapidly through social media. Whereas the desire to proactively influence fertility is understandable, it’s crucial to differentiate between scientifically supported methods and anecdotal claims.
In Plain English: The Clinical Takeaway
- Fertility is complex: Getting pregnant isn’t always uncomplicated and depends on many factors, including age, overall health, and timing.
- Handstands aren’t a proven method: There’s no strong scientific evidence that performing handstands increases the chances of conception.
- Seek professional guidance: If you’re trying to conceive, consulting a healthcare provider is the best way to address any concerns and receive personalized advice.
The Physiology of Conception: A Deep Dive
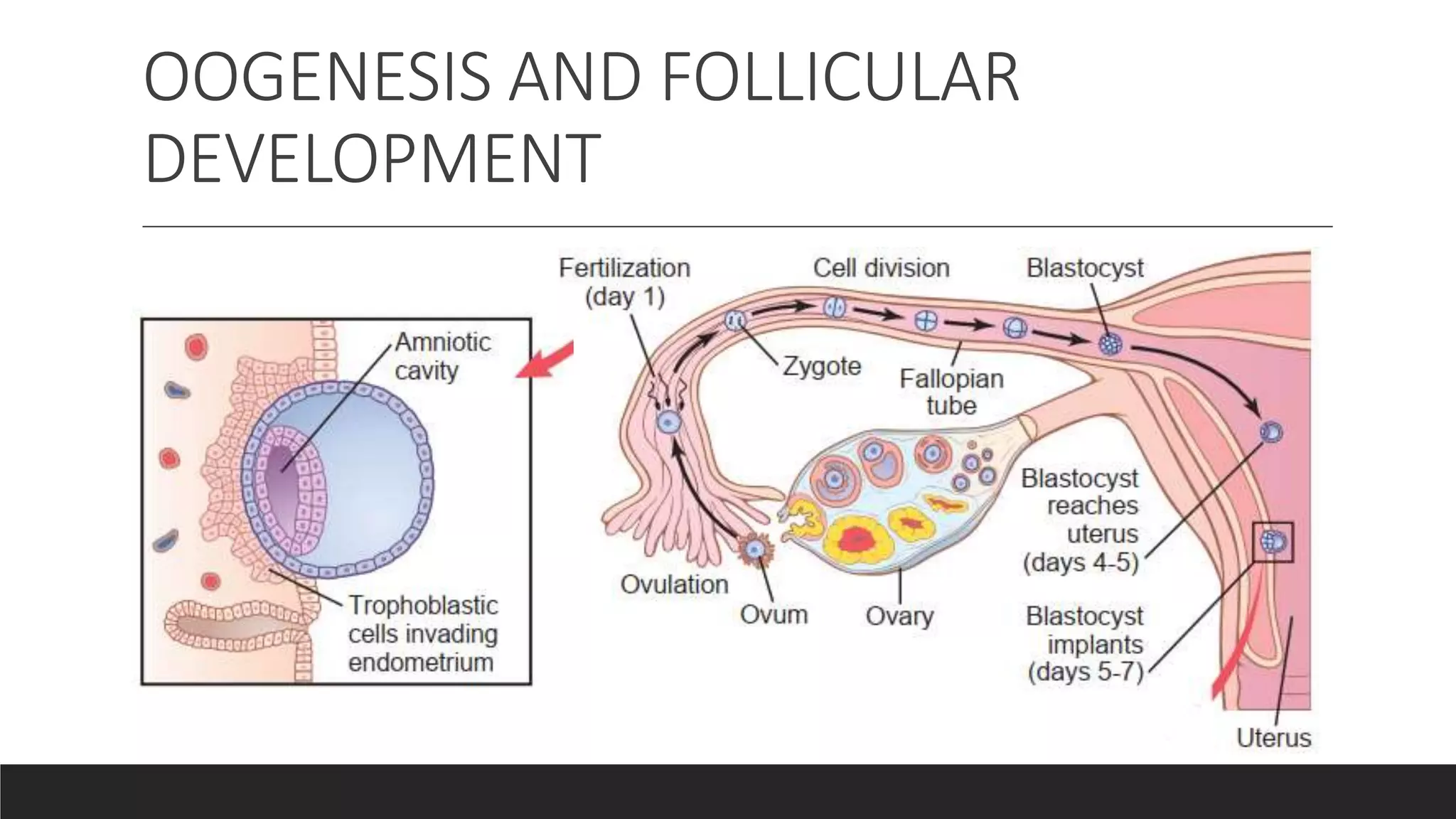
Successful conception requires a complex interplay of hormonal signaling and physiological events. Ovulation, the release of an egg from the ovary, is the critical first step. This process is governed by the hypothalamic-pituitary-ovarian (HPO) axis, a feedback loop involving hormones like gonadotropin-releasing hormone (GnRH), follicle-stimulating hormone (FSH), and luteinizing hormone (LH). Following ovulation, the egg travels through the fallopian tube, where it can be fertilized by sperm. Sperm motility – the ability of sperm to swim effectively – and morphology – the shape and structure of sperm – are crucial factors in fertilization. Once fertilized, the egg implants in the uterine lining, initiating pregnancy.
The claim that handstands might improve fertility stems from the idea that they could increase blood flow to the pelvic region, potentially enhancing uterine lining thickness and egg quality. However, there is limited scientific evidence to support this hypothesis. While increased blood flow is generally beneficial for reproductive health, the transient increase achieved through handstands is unlikely to have a significant impact on these complex physiological processes. A 2018 meta-analysis published in Human Reproduction Update [ https://pubmed.ncbi.nlm.nih.gov/29447283/] highlighted that lifestyle factors like maintaining a healthy weight, avoiding smoking, and managing stress have a far more substantial impact on fertility than isolated physical maneuvers.
Global Fertility Trends and Regional Healthcare Access
Globally, infertility rates are rising. According to the World Health Organization (WHO), approximately 1 in 6 people worldwide experience infertility. [ https://www.who.int/news-room/fact-sheets/detail/infertility] This increase is attributed to factors such as delayed childbearing, lifestyle changes, and environmental exposures. Access to fertility treatments, however, varies significantly across regions. In countries with robust healthcare systems like the United Kingdom (NHS) and many European nations (covered by the European Medicines Agency – EMA), subsidized IVF (In Vitro Fertilization) and other assisted reproductive technologies (ART) are available, though often with waiting lists. In the United States, access is largely dependent on insurance coverage and individual financial resources, leading to significant disparities. The Food and Drug Administration (FDA) regulates ART procedures and technologies in the US, ensuring safety and efficacy standards are met.
“The increasing prevalence of infertility is a significant public health concern. Addressing this requires a multi-faceted approach, including promoting awareness of risk factors, improving access to affordable fertility care, and investing in research to develop more effective treatments.” – Dr. Zita Legerski, Epidemiologist, CDC (as stated in a 2024 CDC report on infertility trends).
Funding and Bias Transparency
Research into fertility treatments is often funded by pharmaceutical companies and medical device manufacturers. It’s crucial to be aware of potential biases when evaluating study results. For example, studies evaluating the efficacy of new ART drugs are frequently funded by the companies that produce those drugs. Transparency regarding funding sources is essential for maintaining scientific integrity. A recent study published in The Lancet [ https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(23)02484-X/fulltext] emphasized the importance of independent research and rigorous peer review to mitigate the influence of commercial interests.
| Fertility Treatment | Success Rate (per cycle) | Common Side Effects | Average Cost (USD) |
|---|---|---|---|
| Intrauterine Insemination (IUI) | 10-20% | Mild cramping, spotting | $1,000 – $2,000 |
| In Vitro Fertilization (IVF) | 30-50% | Bloating, mood swings, ovarian hyperstimulation syndrome (OHSS) | $10,000 – $15,000 |
| Intracytoplasmic Sperm Injection (ICSI) | 40-60% | Similar to IVF | $12,000 – $18,000 |
Contraindications & When to Consult a Doctor
While generally safe, certain medical conditions may contraindicate attempting conception or undergoing fertility treatments. These include uncontrolled chronic illnesses (e.g., diabetes, hypertension), active infections, and certain autoimmune disorders. Individuals with a history of ectopic pregnancy or pelvic inflammatory disease should also consult with a healthcare provider before attempting to conceive. Symptoms that warrant immediate medical attention include severe pelvic pain, heavy vaginal bleeding, and signs of infection (fever, chills). We see also crucial to seek medical advice if you have been trying to conceive for 12 months (or 6 months if over 35) without success.
“It’s vital for individuals to have realistic expectations about fertility and to understand that there is no ‘quick fix.’ A comprehensive evaluation by a reproductive endocrinologist is the best way to identify any underlying issues and develop a personalized treatment plan.” – Dr. Anya Sharma, PhD, Reproductive Biologist, Harvard Medical School.
Park Semi’s announcement serves as a reminder of the complexities surrounding fertility and the importance of relying on evidence-based information. While personal anecdotes may be intriguing, they should not replace the guidance of qualified healthcare professionals. Continued research and improved access to affordable fertility care are essential for addressing the growing global challenge of infertility.
References
- Human Reproduction Update. 2018;24(6):639-651.
- World Health Organization. Infertility. https://www.who.int/news-room/fact-sheets/detail/infertility
- The Lancet. 2023;402(10412):1533-1544.
- CDC. Infertility. https://www.cdc.gov/reproductivehealth/infertility/index.htm

