A case study highlights the critical challenge of diagnosing autoimmune encephalitis, a rare but potentially fatal neurological condition, when its initial symptoms closely resemble those of severe depression. The case, involving a patient whose condition rapidly deteriorated, underscores the need for heightened awareness among clinicians to avoid delayed or missed diagnoses.
The difficulty lies in the often-subtle neurological signs that can be overshadowed by prominent psychiatric symptoms. Autoimmune encephalitis occurs when the body’s immune system mistakenly attacks the brain, leading to inflammation and a range of neurological and psychiatric manifestations. Early recognition is crucial, as prompt treatment can significantly improve outcomes, even as delays can lead to irreversible brain damage and even death. The diagnostic process for autoimmune encephalitis can be complex, often requiring a multidisciplinary approach.
The Case: A Rapid Decline Mistaken for Depression
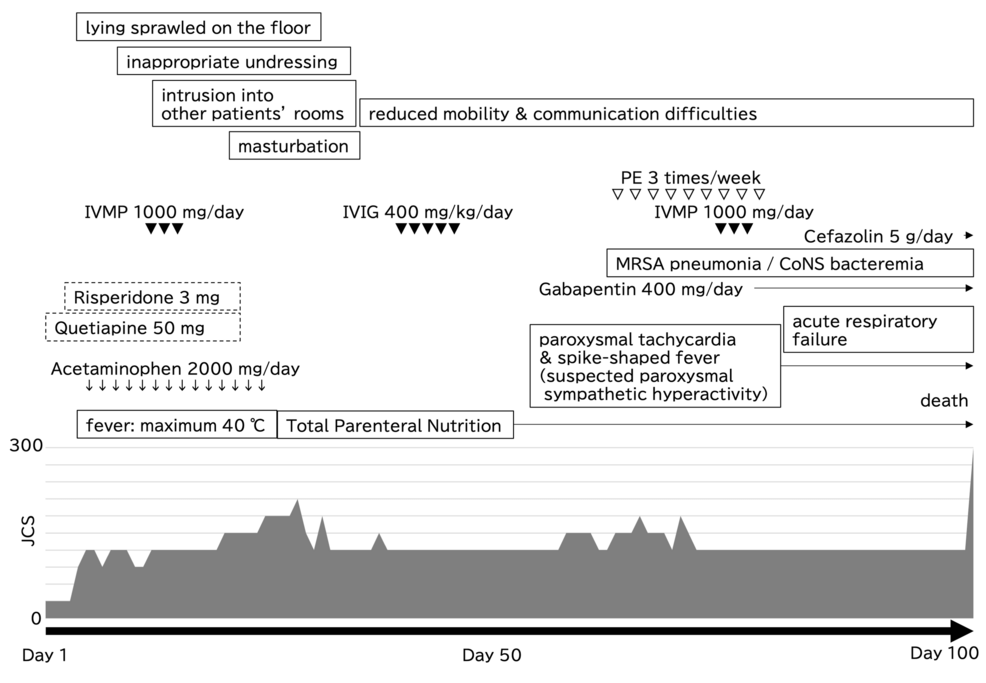
The recent case detailed a patient who initially presented with symptoms consistent with major depressive disorder. However, the patient’s condition rapidly progressed, exhibiting cognitive decline and neurological deficits that were atypical for a primary psychiatric illness. Despite the escalating symptoms, the initial clinical impression remained focused on a psychiatric etiology, delaying further investigation into potential autoimmune causes. This delay proved critical, as the patient ultimately succumbed to the illness.
Researchers emphasize that autoimmune encephalitis can present with a wide spectrum of symptoms, making diagnosis challenging. Psychiatric manifestations, including depression, anxiety, and psychosis, can occur simultaneously with, or even precede, neurological symptoms. This overlap can lead to misdiagnosis, particularly when clinicians are not fully aware of the possibility of autoimmune encephalitis. According to research, patients with autoimmune diseases affecting the brain and spinal cord, such as multiple sclerosis and Hashimoto encephalopathy, are at an increased risk for depression and other mood disorders.
Diagnostic Challenges and the Role of Seronegative Autoimmune Encephalitis
The case likewise highlights the complexities of “seronegative” autoimmune encephalitis, where standard antibody tests for known autoimmune encephalitis antigens are negative. This presents a significant diagnostic hurdle, as clinicians may be less likely to suspect an autoimmune cause in the absence of positive antibody markers. However, it’s increasingly recognized that a substantial proportion of autoimmune encephalitis cases are seronegative, meaning the specific antibodies responsible for the immune attack are not yet identified or detectable with current testing methods.
The overlap between psychiatric and neurological manifestations in autoimmune encephalitis necessitates a multidisciplinary approach for diagnosis and management. This involves collaboration between neurologists, psychiatrists, immunologists, and other specialists. A thorough neurological examination, including assessment of cognitive function, motor skills, and reflexes, is essential. Neuroimaging studies, such as MRI, and cerebrospinal fluid analysis can also provide valuable clues. Psychiatric manifestations of autoimmune encephalitis can occur simultaneously, sequentially, or even after a prolonged period of psychiatric symptoms.
Implications for Clinical Practice and Future Research
This case serves as a stark reminder of the importance of considering autoimmune encephalitis in the differential diagnosis of patients presenting with rapidly progressive psychiatric symptoms, particularly when accompanied by neurological signs. Clinicians should maintain a high index of suspicion, even in the absence of positive antibody markers. Further research is needed to identify novel autoimmune targets and develop more sensitive diagnostic tests for seronegative autoimmune encephalitis.
The long-term psychiatric consequences of autoimmune encephalitis, even after remission, are also an area of ongoing investigation. Studies have shown that a significant proportion of patients experience persistent symptoms of depression and anxiety, highlighting the need for comprehensive psychiatric care and long-term follow-up. A study found that depressive symptoms occur in up to half of all patients with multiple sclerosis, indicating a strong link between autoimmune conditions and mood disorders.
What comes next involves continued efforts to refine diagnostic criteria, improve treatment strategies, and enhance our understanding of the underlying mechanisms driving autoimmune encephalitis. Increased awareness among healthcare professionals and the development of more accessible diagnostic tools are crucial steps in improving outcomes for patients affected by this devastating condition.
Have you or someone you recognize experienced challenges in diagnosing a complex neurological or psychiatric condition? Share your thoughts in the comments below. Please also share this article to raise awareness about autoimmune encephalitis.
Disclaimer: This article provides informational content only and is not intended to be a substitute for professional medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment of any medical condition.