Atypical Mycobacterial Infection Linked to Tap Water Exposure in Elderly Patient
An 80-year-classic male in Thailand, a former smoker who quit two decades ago, has been diagnosed with Mycobacterium kansasii, a non-tuberculous mycobacterial (NTM) infection, alongside a diagnosis of diabetes. Initial investigations suggest potential exposure through aerosolized tap water during showering, highlighting a growing, yet often overlooked, public health concern regarding waterborne pathogens.
This case, detailed by Dr. Manoon Leechawengwong, underscores the increasing incidence of NTM infections, particularly in individuals with pre-existing lung conditions. While traditionally associated with soil and natural water sources, recent evidence points to municipal water systems as a significant reservoir for these organisms. The implications extend beyond Thailand, prompting a re-evaluation of water sanitation protocols globally.
In Plain English: The Clinical Takeaway
- What is NTM? It’s a type of bacterial infection, similar to tuberculosis, but usually less contagious and often affecting people with lung problems.
- How could tap water be involved? Certain bacteria can grow in water pipes and grow airborne when you shower or use faucets. Breathing in these tiny droplets can lead to infection.
- Who is at risk? People with weakened immune systems or existing lung diseases, like COPD, are more susceptible.
Understanding Non-Tuberculous Mycobacteria (NTM)
NTM are a group of bacteria commonly found in the environment, including soil, water, and dust. Unlike Mycobacterium tuberculosis, the causative agent of tuberculosis, NTM infections are generally not spread person-to-person. However, they can cause lung infections, particularly in individuals with underlying lung disease, such as chronic obstructive pulmonary disease (COPD) or bronchiectasis. The Mycobacterium kansasii species is one of the more frequently identified NTM causing pulmonary disease. The mechanism of action involves the bacteria adhering to and invading lung tissue, triggering an inflammatory response that leads to the formation of cavities and fibrosis – scarring of the lungs.
The incidence of NTM lung disease has been steadily increasing worldwide. A study published in the American Journal of Respiratory and Critical Care Medicine showed a significant rise in NTM diagnoses in the United States between 1998 and 2018, with rates nearly tripling during that period. https://www.atsjournals.org/doi/10.1164/rccm.202003-0383OC This increase is attributed to several factors, including improved diagnostic techniques, an aging population, and potentially, changes in environmental exposures.
The Role of Water Systems and Biofilm Formation
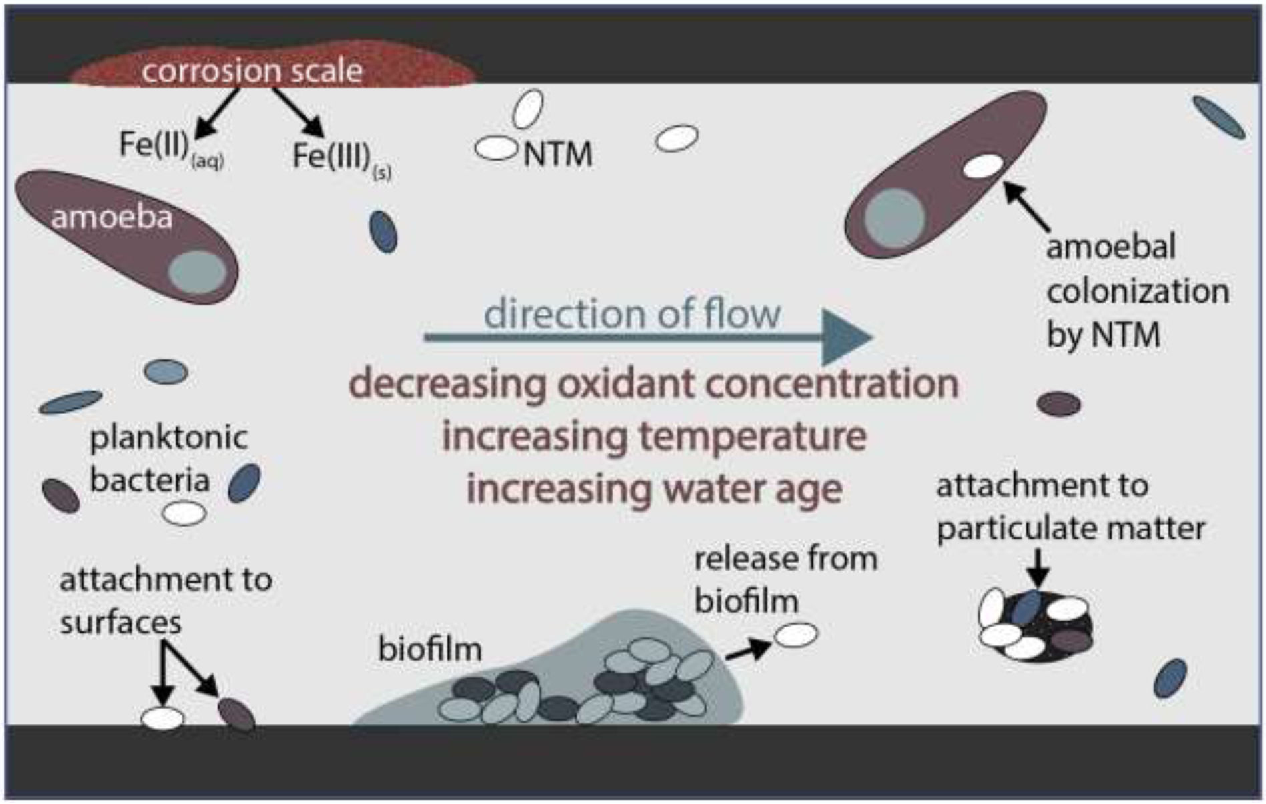
The source of NTM in water systems is often biofilm – a complex community of microorganisms that adhere to surfaces within water pipes. These biofilms can harbor NTM, protecting them from disinfection and allowing them to proliferate. Aerosolization of water during showering, flushing toilets, or even running faucets can release these bacteria into the air, creating a potential inhalation hazard.
Research conducted by the Centers for Disease Control and Prevention (CDC) has identified Mycobacterium avium complex (MAC) as the most common NTM species found in U.S. Water systems. https://www.cdc.gov/nontuberculousmycobacteria/environmental/index.html While M. Kansasii is less prevalent, its presence in potable water has been documented, particularly in older plumbing systems. The patient’s pre-existing lung condition, specifically the presence of bronchiectasis (widening of the airways), likely created an environment conducive to the establishment of infection following exposure.
Contraindications & When to Consult a Doctor
While NTM infections are not typically contagious, individuals with the following conditions should be particularly vigilant and consult a doctor if they experience respiratory symptoms:
- Individuals with COPD, bronchiectasis, or cystic fibrosis.
- Immunocompromised individuals (e.g., those with HIV/AIDS, organ transplant recipients, or those undergoing chemotherapy).
- Individuals with a history of chronic lung disease.
Symptoms warranting medical attention include persistent cough (lasting more than 3 weeks), coughing up blood, fatigue, weight loss, and shortness of breath. Early diagnosis and treatment are crucial to prevent disease progression.
Treatment and Prognosis
The patient in Thailand was initiated on a multi-drug regimen including Rifampicin, Ethambutol, Azithromycin, and Moxifloxacin. This combination therapy is commonly used to treat M. Kansasii infections. Treatment duration typically ranges from 12 to 18 months, requiring careful monitoring for potential side effects.
The efficacy of NTM treatment varies depending on the species involved, the severity of the infection, and the patient’s overall health. Drug susceptibility testing is essential to ensure the chosen antibiotics are effective against the specific strain of NTM.
| Antibiotic | Common Side Effects | Monitoring Requirements |
|---|---|---|
| Rifampicin | Liver enzyme elevation, nausea, orange discoloration of bodily fluids | Regular liver function tests |
| Ethambutol | Optic neuritis (inflammation of the optic nerve) | Regular visual acuity testing |
| Azithromycin | Gastrointestinal upset, QT prolongation | ECG monitoring, assessment of gastrointestinal symptoms |
| Moxifloxacin | Tendinitis, QT prolongation | Assessment of musculoskeletal symptoms, ECG monitoring |
Geographical and Regulatory Implications
The increasing recognition of waterborne NTM raises concerns about the adequacy of current water sanitation practices. While the U.S. Environmental Protection Agency (EPA) regulates disinfectants used in public water systems, there are currently no federal standards specifically addressing NTM levels. Several states and municipalities are beginning to implement voluntary monitoring programs and explore advanced disinfection technologies, such as ultraviolet (UV) irradiation and ozone treatment, to reduce NTM contamination.
“The presence of NTM in water systems is a complex issue that requires a multi-faceted approach, including improved water treatment technologies, regular monitoring, and public awareness campaigns,” states Dr. Amy Stout, an epidemiologist at the CDC specializing in waterborne diseases. “We need to better understand the factors that contribute to NTM growth in water pipes and develop effective strategies to mitigate the risk of exposure.”
The European Union’s Drinking Water Directive likewise lacks specific NTM limits, even though member states are encouraged to assess and manage the risk. The World Health Organization (WHO) is currently reviewing guidelines for water quality in relation to NTM, with updated recommendations expected in the coming years.
Funding for research into NTM and waterborne pathogens is primarily provided by government agencies, such as the National Institutes of Health (NIH) in the United States, and philanthropic organizations. Transparency regarding funding sources is crucial to ensure the objectivity and credibility of research findings.
Looking Ahead
The case of this 80-year-old patient serves as a stark reminder of the potential health risks associated with waterborne pathogens. Further research is needed to fully elucidate the relationship between water systems and NTM infections, and to develop effective strategies for prevention and control. Public health officials, water utilities, and healthcare providers must collaborate to address this emerging threat and protect vulnerable populations.
References
- American Thoracic Society. (2020). Increasing Epidemiology of Nontuberculous Mycobacterial Lung Disease. American Journal of Respiratory and Critical Care Medicine, 202(10), 1433–1444.
- Centers for Disease Control and Prevention. (n.d.). Nontuberculous Mycobacteria (NTM). Retrieved from https://www.cdc.gov/nontuberculousmycobacteria/index.html
- World Health Organization. (n.d.). Drinking Water Quality. Retrieved from https://www.who.int/water_sanitation_health/dwq/en/
- Thomson, R. M., et al. (2019). Nontuberculous mycobacterial pulmonary disease: current knowledge and future directions. Seminars in Respiratory and Critical Care Medicine, 40(6), 761–775.
