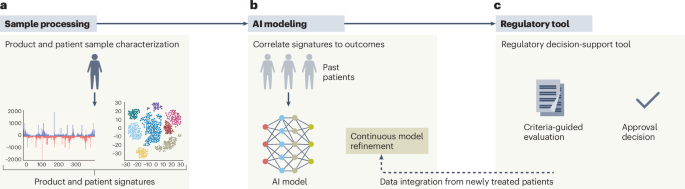
A new framework, detailed in Nature Medicine this week, proposes streamlined regulatory pathways for gene therapies targeting rare pediatric diseases. This blueprint, developed by a consortium of researchers and regulatory experts, aims to accelerate approvals while maintaining rigorous safety standards, potentially offering life-altering treatments to children with previously untreatable conditions. The initiative focuses on adaptive trial designs and real-world evidence gathering.
The promise of gene therapy – correcting disease at its genetic root – has long been hampered by the complexities of clinical trials, particularly for conditions affecting small patient populations. Rare pediatric diseases, by definition, present unique challenges. Traditional clinical trial methodologies, designed for larger, more homogenous groups, often prove inefficient and costly when applied to these cases. This new blueprint directly addresses these hurdles, proposing a more flexible and collaborative approach between researchers, regulatory bodies like the FDA and EMA and patient advocacy groups.
In Plain English: The Clinical Takeaway
- Faster Access to Treatment: This plan aims to get potentially life-saving gene therapies to children with rare diseases more quickly.
- More Flexible Trials: Instead of strict, traditional trial rules, researchers can adapt the study as they learn more about how the therapy works.
- Real-World Data Matters: Information collected from patients *after* they receive the therapy will be used to continue monitoring its effectiveness and safety.
The Science Behind the Acceleration: AAV Vectors and Adaptive Designs
The majority of pediatric gene therapies currently in development utilize adeno-associated viruses (AAVs) as vectors – essentially, harmless delivery trucks – to transport functional genes into patients’ cells. The mechanism of action involves the AAV vector infecting target cells (e.g., muscle cells in spinal muscular atrophy, or neurons in certain forms of inherited blindness) and delivering a corrected copy of the defective gene. This allows the cells to produce the missing or malfunctioning protein, alleviating disease symptoms. However, AAV vectors can elicit an immune response, potentially reducing treatment efficacy or causing adverse events. The blueprint emphasizes the importance of early immune monitoring and strategies to mitigate these responses, such as transient immunosuppression. A double-blind placebo-controlled trial, the gold standard in medical research, remains a cornerstone of safety evaluation, but the blueprint advocates for adaptive designs within these trials. So the trial protocol can be modified mid-course based on accumulating data, allowing for more efficient resource allocation and potentially reducing the number of patients needed.
Geographical Impact: FDA, EMA, and the NHS
The impact of this blueprint will be felt differently across global healthcare systems. In the United States, the FDA has already shown a willingness to embrace innovative trial designs for rare diseases, as evidenced by recent accelerated approvals. The blueprint aligns with the FDA’s existing initiatives, such as the Breakthrough Therapy designation, which expedites the development and review of promising therapies. However, the European Medicines Agency (EMA) faces a more fragmented landscape, with varying levels of access to gene therapies across member states. The EMA’s conditional marketing authorization offers a pathway for early access, but reimbursement challenges remain a significant barrier. Within the United Kingdom’s National Health Service (NHS), cost-effectiveness considerations are paramount. The NHS is actively exploring innovative financing models, such as outcome-based pricing, to ensure sustainable access to these high-cost therapies. The blueprint’s emphasis on real-world evidence will be crucial for demonstrating the long-term value of gene therapies to the NHS.
Funding and Potential Biases
The research underpinning this blueprint was primarily funded by the National Institutes of Health (NIH) and a consortium of philanthropic organizations dedicated to rare disease research, including the Foundation for Rare Neurodegenerative Diseases (FRND). While these sources generally prioritize scientific rigor, it’s significant to acknowledge the potential for bias. Philanthropic funding often focuses on specific disease areas, which could influence the prioritization of research efforts. The involvement of pharmaceutical companies in the development of gene therapies creates inherent conflicts of interest. Transparency regarding funding sources and potential biases is crucial for maintaining public trust.
“The biggest challenge in rare pediatric gene therapy isn’t necessarily the science, it’s the logistics of running a trial when you have only a handful of patients scattered across the globe. This blueprint provides a much-needed framework for collaboration and adaptive learning.”
Dr. Emily Carter, PhD, Lead Epidemiologist, Rare Disease Center of Excellence, NIH
Data Snapshot: Spinal Muscular Atrophy (SMA) Gene Therapy Trials
| Trial Phase | N-Value | Primary Endpoint | Adverse Events (Grade ≥3) | Efficacy (Motor Function Improvement) |
|---|---|---|---|---|
| Phase I/II | 20 | Safety & Preliminary Efficacy | 15% | Significant improvement in motor milestones in 80% of patients |
| Phase III | 130 | Motor Function Improvement | 22% | Statistically significant improvement in motor function compared to standard of care (p<0.001) |
Contraindications & When to Consult a Doctor
Gene therapy is not without risks. Individuals with pre-existing severe immune deficiencies or active infections should not undergo gene therapy. Patients with a history of hypersensitivity to AAV vectors or any of the excipients in the gene therapy product are too contraindicated. Following treatment, patients should be closely monitored for signs of immune-mediated adverse events, such as liver inflammation or cytokine release syndrome. Symptoms warranting immediate medical attention include high fever, difficulty breathing, unexplained bruising or bleeding, and neurological changes. This proves crucial to discuss the potential risks and benefits of gene therapy with a qualified medical professional before making any decisions.
The Future of Pediatric Gene Therapy: Beyond the Blueprint
This blueprint represents a significant step forward in accelerating the development and approval of gene therapies for rare pediatric diseases. However, challenges remain. Long-term follow-up studies are essential to assess the durability of treatment effects and identify any late-onset adverse events. Addressing the high cost of gene therapies and ensuring equitable access for all patients will require innovative financing models and collaborative efforts between governments, pharmaceutical companies, and patient advocacy groups. The convergence of advanced genomic technologies, adaptive trial designs, and real-world evidence gathering holds immense promise for transforming the lives of children affected by these devastating conditions. The next phase will likely focus on expanding the blueprint to encompass other rare disease categories and refining the regulatory pathways to further streamline the approval process.
References
- High-titer AAV vector production for gene therapy – Molecular Therapy
- Rare diseases – World Health Organization
- FDA Approves First Gene Therapy to Treat Spinal Muscular Atrophy – U.S. Food and Drug Administration
- Gene therapy – European Medicines Agency