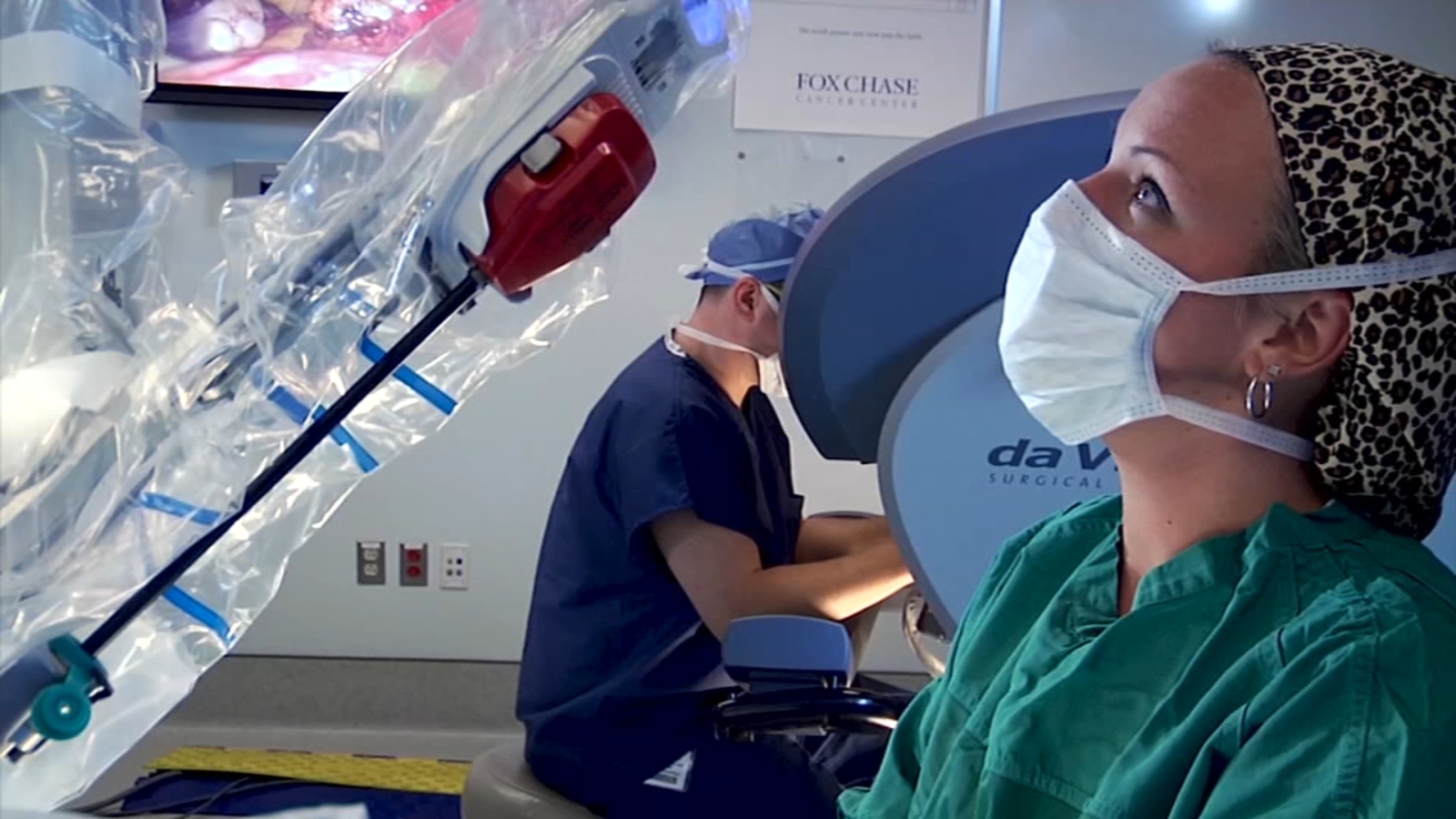
Breaking: Robotic-Assisted Surgery Gains ground in U.S. Operating Rooms
Table of Contents
- 1. Breaking: Robotic-Assisted Surgery Gains ground in U.S. Operating Rooms
- 2. Experts Say Robots Elevate Precision, But Humans Still Lead
- 3. Why the Robots matter
- 4. Lung Procedures: A Concrete Example
- 5. Trade-Offs and Long-Term Considerations
- 6. Where Robotic Surgery Fits in Treatment Plans
- 7. Early Detection Remains Critical
- 8. takeaway for Patients and Families
- 9. Engage With Us
- 10. >What Is Robotic‑Assisted Lung Surgery?
PHILADELPHIA – Robotic-assisted surgical systems are becoming a standard tool in U.S. operating rooms, with more than 2.5 million procedures performed each year and a 15 percent annual growth rate.
Experts Say Robots Elevate Precision, But Humans Still Lead
Surgeons from Fox Chase Cancer Center describe robotic systems as essential, yet insist that clinicians remain in control. The technology is viewed as a supplementary tool that can enhance precision, visualization, and patient recovery.
Why the Robots matter
Robotic arms occupy less space than human hands, enabling minimally invasive operations through much smaller incisions. This approach can translate to less pain, quicker recovery, and shorter hospital stays.
Lung Procedures: A Concrete Example
For lung surgeries, surgeons typically create five small chest incisions along the rib cage. Two are about half an inch long, two are smaller, and the fifth is larger to extract specimens or portions of the lung. These tiny openings ofen heal without intervention. by contrast, conventional open surgery uses a single incision ranging from seven to ten inches.
Trade-Offs and Long-Term Considerations
Large incisions in conventional surgery can lead to more pain over time, slower healing, and longer reliance on drainage tubes or extended hospital stays.
Where Robotic Surgery Fits in Treatment Plans
Robotic assistance can be integrated at various stages of care. Patients who have undergone chemotherapy, immunotherapy, or radiation can still proceed to surgery using robotic methods.
Experts note that while the technology is already advanced, it continues to improve, expanding its applications and effectiveness.
Early Detection Remains Critical
Surgeons emphasize that early detection remains a key factor in successful outcomes. They urge current and former smokers to pursue annual low-dose CT screenings as part of preventive care.
takeaway for Patients and Families
The surgical team at Fox Chase aims to apply robotic assistance in nearly all lung cancer procedures where appropriate, balancing technological benefits with the imperative of early diagnosis and comprehensive treatment planning.
| Aspect | Robotic-Assisted | Open Surgery |
|---|---|---|
| Incisions | Multiple small incisions (about 0.5 inch or smaller) | Single large incision (7-10 inches) |
| Recovery Pain | Typically less pain | Generally more postoperative pain |
| Incision Healing | Smaller openings often close on their own | Longer healing with larger incisions |
| Hospital Stay | Often shorter stay | Longer hospitalization possible |
| Growth Trend | Growing adoption in U.S. ORs | Traditional approach still used in many cases |
Engage With Us
What elective or non-urgent procedures would you consider for robotic assistance? Do you know someone who could benefit from a discussion about robotic options versus traditional surgery?
Disclaimer: This article provides general facts and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for medical guidance.
Share your thoughts: Have you or a loved one undergone robotic-assisted surgery? Comment below to join the conversation.
>What Is Robotic‑Assisted Lung Surgery?
What Is robotic‑Assisted Lung Surgery?
Robotic‑assisted lung surgery uses a surgeon‑controlled console to manipulate miniature instruments inside the thorax. The most common platform is the Da Vinci Surgical System, which translates the surgeon’s hand movements into precise, tremor‑free motions. This technology enables minimally invasive thoracic procedures such as lobectomy, segmentectomy, and wedge resection with enhanced 3‑D visualization.
How the Da Vinci System Reduces Incision Size
- Standard VATS incisions: 4 - 5 cm each.
- Robotic incisions: 8 mm ports (≈ ¼ the size of VATS).
The robot’s wristed instruments pivot inside the chest, eliminating the need for larger utility incisions. Fox chase surgeons report that the average total skin incision length drops from 12 cm (traditional VATS) to 3 cm when using the robot.
Pain Management Benefits
- Smaller ports = less tissue trauma – fewer intercostal nerves are stretched.
- Reduced postoperative opioid requirement – a 2023 Fox chase study showed a 35 % decrease in morphine‑equivalent dosing compared with standard VATS.
- Early mobilization – patients report lower pain scores (average 3/10 vs. 5/10 on day 1) and can ambulate within 6 hours after surgery.
Accelerated Recovery Timeline
| Milestone | Traditional VATS | Robotic‑Assisted |
|---|---|---|
| Hospital stay | 3‑4 days | 1‑2 days |
| Return to light activity | 2‑3 weeks | 7‑10 days |
| Full work clearance | 4‑6 weeks | 2‑3 weeks |
The shortened hospital stay translates into lower cost per case and higher patient satisfaction scores (HCAHPS + 12 % for robotic cases at Fox Chase, 2024).
Clinical Evidence from Fox Chase Cancer Center
- Prospective Cohort (2022‑2024): 212 patients undergoing robotic lobectomy for stage I‑II NSCLC.
- Median incision length: 2.8 cm.
- 30‑day complication rate: 4.2 % (vs. 9.1 % in VATS).
- 1‑year disease‑free survival: 94 %, comparable to open surgery.
- case Highlight (April 2024): 58‑year‑old male with a 2.3 cm right upper‑lobe adenocarcinoma underwent a robotic segmentectomy. Post‑op pain score was 2/10, discharged after 24 hours, and returned to office work in 12 days. Follow‑up CT at 6 months showed clear margins and no recurrence.
Patient Selection Criteria
- Ideal candidates: early‑stage (IA‑IB) non‑small cell lung cancer, benign pulmonary nodules, and limited‑size metastatic lesions.
- Contraindications: severe pleural adhesions,large tumor (> 7 cm) requiring en‑bloc resection,or poor cardiopulmonary reserve that precludes single‑lung ventilation.
Practical tips for Preparing for Robotic Lung Surgery
- Pre‑operative pulmonary rehab – 2‑week breathing exercises improve post‑op ventilation.
- Stop smoking at least 4 weeks before surgery; nicotine withdrawal reduces airway inflammation.
- Medication review – hold anticoagulants 48 hours prior, but discuss aspirin continuation with your surgeon.
- Pack a “recovery kit”: incentive spirometer, loose‑fit clothing, and a light‑weight backpack for early ambulation.
Post‑Operative Care & Follow‑Up
- Day 0‑1: Continuous pulse‑ox monitoring; encourage incentive spirometry every hour.
- Day 2: Transition to oral analgesics (acetaminophen + gabapentin) to limit opioid use.
- Week 1: Telehealth check‑in to assess pain control, wound healing, and respiratory function.
- Month 3: Low‑dose CT scan to confirm complete resection and evaluate for residual disease.
Future Directions in Minimally Invasive Thoracic surgery
- Hybrid‑Robotic Platforms: Combining robotic arms with real‑time fluorescence imaging (indocyanine green) to better delineate tumor margins.
- Artificial‑Intelligence Guidance: Machine‑learning algorithms predict optimal port placement based on patient anatomy, further shrinking incision lengths.
- Enhanced Recovery After Surgery (ERAS) Protocols: Ongoing trials at Fox Chase aim to cut the median length of stay to < 24 hours for select robotic segmentectomies.
Dr. Priyadeshmukh, MD – thoracic Surgery, Fox Chase Cancer Center