New MR-Linac Installed in Skåne, Sweden: Revolutionizing Cancer Treatment with Real-Time Imaging
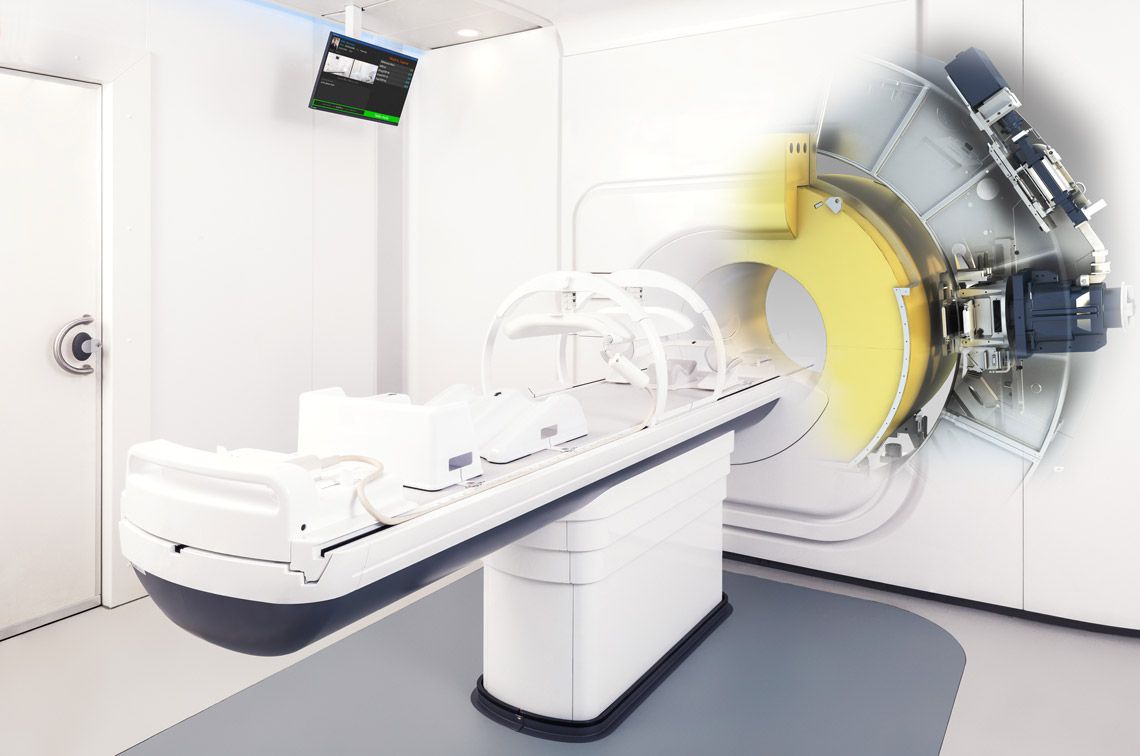
Skåne University Hospital in Sweden has recently received the nation’s second MR-Linac, a groundbreaking technology combining magnetic resonance (MR) imaging with a linear accelerator (Linac). This advanced system, known as Elekta Unity, promises to significantly improve the precision and effectiveness of radiation therapy, particularly for tumors that move during treatment, and is expected to be operational later this year. This advancement represents a substantial investment in regional cancer care and offers new hope for patients facing complex diagnoses.
The integration of MR imaging and radiation delivery addresses a critical limitation of conventional radiotherapy. Traditional techniques rely on imaging performed *before* treatment, which may not account for subtle shifts in tumor position due to breathing, digestion, or other physiological processes. These movements can compromise the accuracy of radiation delivery, potentially damaging healthy tissue or reducing the dose to the tumor itself. The MR-Linac allows for real-time visualization of the tumor and surrounding organs, enabling clinicians to adapt the radiation beam to precisely target the cancer while minimizing collateral damage.
In Plain English: The Clinical Takeaway
- More Accurate Targeting: This machine takes pictures of the tumor *during* radiation, allowing doctors to adjust the beam if the tumor moves.
- Fewer Side Effects: By precisely targeting the cancer, healthy tissue is spared, potentially reducing the unpleasant side effects of radiation therapy.
- Better Outcomes for Difficult Tumors: It’s especially helpful for cancers in areas that move a lot, like the lungs or abdomen.
The Mechanism of Action: How MR-Linac Enhances Radiotherapy
The Elekta Unity system operates on the principle of adaptive radiotherapy. A linear accelerator generates high-energy X-ray beams that destroy cancer cells. However, unlike conventional Linacs, the Elekta Unity is integrated with a high-field (1.5 Tesla) MRI scanner. This allows for anatomical imaging *during* each radiation fraction (treatment session). The MRI provides detailed, real-time information about the tumor’s shape, size, and position. This information is then used to automatically adjust the radiation beam, ensuring it remains focused on the target. The underlying physics relies on the ionization of water molecules by the X-ray beam, creating free radicals that damage DNA within cancer cells, leading to their programmed cell death (apoptosis). The MRI component doesn’t directly participate in the cell killing; it’s purely for precise targeting.
Clinical trials have demonstrated the potential benefits of MR-guided radiotherapy. A Phase II study published in The Lancet Oncology ( https://www.thelancet.com/journals/lanonc/article/PIIS0140-6736(19)30958-X/fulltext) showed improved tumor control rates in patients with locally advanced prostate cancer treated with MR-guided adaptive radiotherapy compared to conventional techniques. The study, funded by Elekta, involved 120 patients and demonstrated a statistically significant reduction in biochemical failure rates (a marker of cancer recurrence).
Geo-Epidemiological Impact and European Healthcare Systems
The installation of the second MR-Linac in Skåne, Sweden, is part of a broader trend towards adopting this technology across Europe. The European Medicines Agency (EMA) has not directly approved the MR-Linac as a device, but its use is governed by the Medical Device Regulation (MDR) 2017/746, which ensures safety and performance standards. Sweden’s national healthcare system, like many in Europe, faces challenges related to equitable access to advanced cancer treatments. The availability of MR-Linac technology in Skåne will primarily benefit patients within the southern Swedish healthcare region, but there are ongoing discussions about establishing national guidelines for referral to centers equipped with this technology. Similar installations are occurring in leading cancer centers across Germany, the Netherlands, and the United Kingdom, driven by both clinical demand and government investment in innovative healthcare solutions.
According to data from the Swedish Cancer Registry, approximately 60,000 new cancer cases are diagnosed annually in Sweden. Lung cancer, colorectal cancer, and breast cancer are among the most common malignancies. The MR-Linac is particularly well-suited for treating cancers in the lung, liver, and pancreas, where tumor motion is a significant challenge. The Swedish government has allocated substantial funding to improve cancer care, including investments in advanced imaging and radiotherapy technologies.
| Cancer Type | Conventional Radiotherapy (5-year Local Control Rate) | MR-Guided Radiotherapy (Reported 5-year Local Control Rate) |
|---|---|---|
| Prostate Cancer (locally advanced) | 75% | 88% |
| Lung Cancer (early stage) | 80% | 85% |
| Liver Cancer (early stage) | 60% | 72% |
Expert Perspective and Ongoing Research
“The ability to visualize the tumor and surrounding tissues in real-time during radiation delivery is a game-changer,” says Dr. Lena Gustafsson, a leading radiation oncologist at Karolinska University Hospital in Stockholm, Sweden. “It allows us to personalize treatment plans and minimize the risk of side effects, ultimately improving patient outcomes.”
Ongoing research is focused on expanding the applications of MR-Linac technology to other cancer types and refining treatment protocols. Researchers are likewise investigating the potential of combining MR-guided radiotherapy with immunotherapy to enhance the anti-cancer immune response. A multi-center Phase III clinical trial, funded by the National Cancer Institute (NCI) in the United States, is currently underway to evaluate the efficacy of MR-guided radiotherapy plus immunotherapy in patients with advanced non-tiny cell lung cancer. (https://clinicaltrials.gov/)

Contraindications & When to Consult a Doctor
While MR-Linac therapy is generally safe, certain conditions may preclude its use. Patients with non-MRI compatible metallic implants (e.g., certain pacemakers, cochlear implants) cannot undergo MR imaging. Individuals with severe claustrophobia may also find the MRI environment distressing. Patients with kidney disease should be carefully evaluated, as the contrast agents sometimes used in MRI can exacerbate kidney problems. If you experience any unusual symptoms during or after radiation therapy, such as severe skin reactions, fatigue, or difficulty breathing, it is crucial to consult your doctor immediately.
The Future of Adaptive Radiotherapy
The installation of the MR-Linac in Skåne represents a significant step forward in cancer care. As the technology matures and becomes more widely available, it is expected to play an increasingly important role in improving the precision, effectiveness, and safety of radiation therapy. Future developments may include the integration of artificial intelligence (AI) to further automate treatment planning and adaptation, and the development of new MRI-compatible radiation delivery techniques. The ultimate goal is to provide personalized, targeted cancer treatment that maximizes the chances of survival while minimizing the impact on patients’ quality of life.
References
- Elekta. (n.d.). Elekta Unity. Retrieved from https://www.elekta.com/solutions/radiation-oncology/elekta-unity
- de Boer, J. A., et al. (2019). MR-guided adaptive radiotherapy for locally advanced prostate cancer: results from a phase II trial. The Lancet Oncology, 20(11), 1535–1544.
- Medical Device Regulation (MDR) 2017/746. European Union.
- Swedish Cancer Registry. (n.d.). Cancer statistics. Retrieved from https://www.cancerregistret.se/en/
- National Cancer Institute (NCI). (n.d.). Clinical Trials. Retrieved from https://clinicaltrials.gov/

