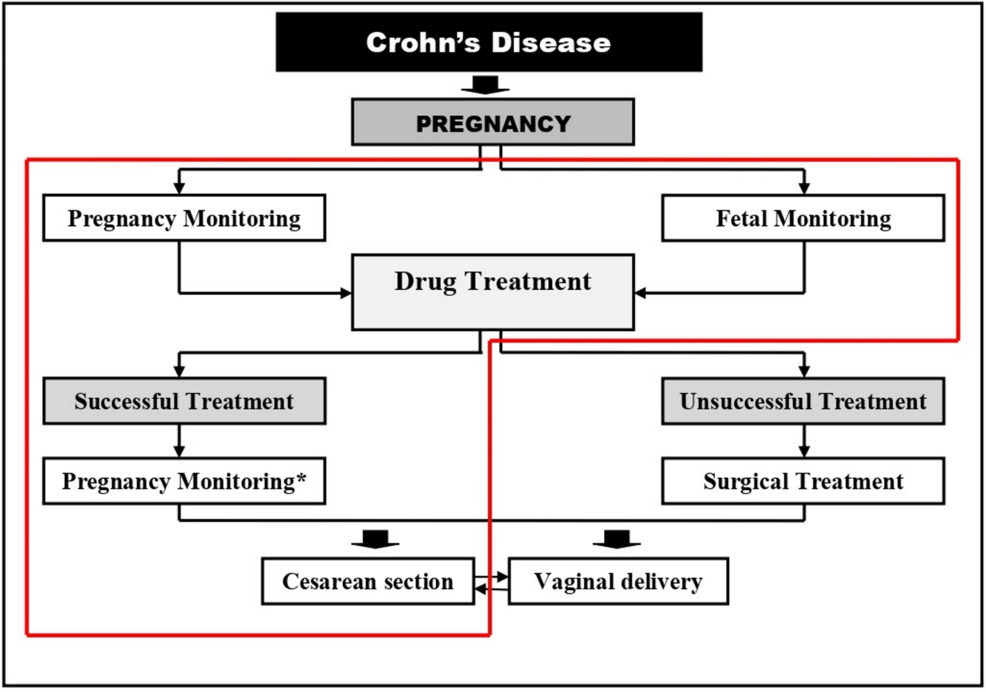
A recent clinical case report highlights the successful pregnancy and delivery of a patient with Crohn’s disease and a history of intestinal surgery. The outcome underscores the critical importance of achieving disease remission before conception and utilizing multidisciplinary care to mitigate risks associated with prior surgical interventions and chronic inflammation.
For women living with Inflammatory Bowel Disease (IBD), the prospect of pregnancy often brings a complex mixture of hope and clinical anxiety. The intersection of autoimmune instability and the physiological demands of gestation creates a high-stakes environment, particularly for those who have undergone bowel resections. This case serves as a vital proof-of-concept: while a history of intestinal surgery increases the complexity of prenatal care, It’s not a barrier to a healthy birth. Globally, this shifts the conversation from “if” a patient can conceive to “how” we optimize their biological environment to ensure safety.
In Plain English: The Clinical Takeaway
- Remission is Key: The best chance for a healthy baby and mother is to ensure the Crohn’s disease is “quiet” (in remission) before getting pregnant.
- Surgery Isn’t a Dealbreaker: Previous intestinal surgeries may require extra nutritional monitoring, but they do not prevent a successful pregnancy.
- Team-Based Care: Success requires a “bridge” between a gastroenterologist (gut specialist) and a maternal-fetal medicine specialist (high-risk pregnancy doctor).
The Synergy of Pre-conception Remission and Mucosal Healing
The cornerstone of this successful outcome was the achievement of clinical remission—a state where the patient is free of symptoms—and, more importantly, mucosal healing. Mucosal healing refers to the actual repair of the lining of the intestine, which can only be verified through endoscopy. What we have is a critical distinction because a patient may feel well (clinical remission) while still having active, microscopic inflammation that could trigger a flare during pregnancy.

In patients with Crohn’s, the mechanism of action for many maintenance therapies involves the suppression of pro-inflammatory cytokines. For instance, Anti-TNF (Tumor Necrosis Factor) agents function by neutralizing a specific protein that triggers systemic inflammation. According to the European Crohn’s and Colitis Organisation (ECCO), maintaining these therapies during pregnancy is often safer than risking a disease flare, which is statistically linked to higher rates of preterm birth and low birth weight.
“The paradigm has shifted toward maintaining the lowest effective dose of biologics to keep the patient in remission. The risk of a disease relapse during pregnancy generally outweighs the theoretical risks of fetal exposure to most IBD medications,” notes Dr. Sarah Jenkins, a leading researcher in maternal-fetal immunology.
Navigating the Surgical Legacy: Absorption and Adhesions
Prior intestinal surgery introduces two primary clinical hurdles: malabsorption and adhesions. When portions of the bowel are removed (resection), the body’s ability to absorb critical micronutrients—such as Vitamin B12, iron and folic acid—is compromised. Folic acid deficiency is particularly perilous, as it significantly increases the risk of neural tube defects in the developing fetus.
surgical scars (adhesions) can increase the risk of bowel obstructions during the second and third trimesters as the growing uterus displaces the intestines. This necessitates a highly calibrated monitoring schedule. In the United States, the FDA and the American College of Obstetricians and Gynecologists (ACOG) emphasize personalized nutrient supplementation based on the specific site of the prior resection (e.g., ileal vs. Colonic).
The following table summarizes the risk stratification based on disease activity at the time of conception:
| Disease State at Conception | Pregnancy Risk Level | Primary Clinical Concern | Management Priority |
|---|---|---|---|
| Deep Remission (Mucosal Healing) | Low to Moderate | Standard prenatal monitoring | Maintenance therapy |
| Clinical Remission (Symptom-free) | Moderate | Subclinical inflammation flare | Regular biomarker checks (CRP/Calprotectin) |
| Active Flare | High | Preterm birth, fetal growth restriction | Induce remission before conception |
Global Access and Regulatory Nuances in IBD Care
The ability to replicate this success depends heavily on the regional healthcare infrastructure. In the UK, the NHS NICE guidelines provide a structured pathway for IBD patients seeking pregnancy, ensuring integrated care between gastroenterology and obstetrics. In contrast, patients in fragmented healthcare systems may face “siloed” care, where the OB-GYN is unaware of the gastroenterologist’s medication adjustments, increasing the risk of contraindicated prescriptions.
Funding for the underlying research in these case reports is typically provided by institutional grants or the authors’ affiliated university hospitals. Because these are case reports rather than large-scale Phase III clinical trials, they provide “proof of possibility” rather than statistical certainty. However, they are essential for refining the clinical guidelines used by the World Health Organization (WHO) to improve maternal health outcomes in chronic disease populations.
Contraindications & When to Consult a Doctor
While many IBD medications are safe, certain treatments are strictly contraindicated during pregnancy due to their teratogenic effects (the ability to cause birth defects). Methotrexate, for example, is a potent folic acid antagonist and must be discontinued months before conception.
Patients should seek immediate medical intervention if they experience the following during pregnancy:
- Severe abdominal pain: This could indicate a bowel obstruction caused by surgical adhesions.
- Unexplained fever: This may signal a disease flare or an infection, both of which require urgent stabilization to protect the fetus.
- Significant weight loss: A sign of malabsorption that requires immediate nutritional support via IV or specialized enteral feeds.
The Future of IBD Gestational Medicine
The success of this patient highlights a broader trajectory in medicine: the move toward “precision pregnancy.” By combining biomarker tracking (measuring C-reactive protein and fecal calprotectin) with surgical history analysis, clinicians can now tailor a pregnancy plan that minimizes risk. The goal is no longer just a successful delivery, but the long-term health of the mother, ensuring that the pregnancy does not trigger a permanent decline in her intestinal function.