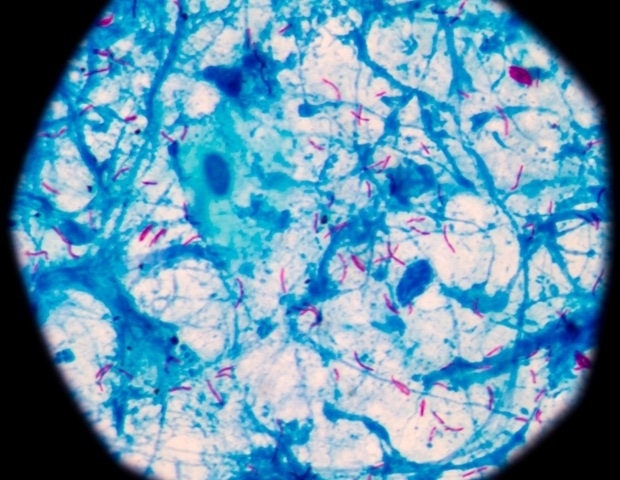
Tuberculosis (TB) remains one of the world’s most significant public health challenges, claiming an estimated 1.3 million lives in 2022 alone. The emergence of drug-resistant strains, particularly in regions like the Asia-Pacific, underscores the urgent need for innovative treatment strategies. Now, researchers are shedding light on how a new class of experimental antibiotics interferes with the bacterium that causes TB, Mycobacterium tuberculosis, offering a potential pathway to urgently needed new therapies.
A study published recently in Nature Communications details how three naturally occurring antibiotic compounds – ecumicin, ilamycin, and cyclomarin – disrupt a critical process within the TB bacterium. This research offers a deeper understanding of how to combat this resilient pathogen and potentially overcome growing antibiotic resistance.
The team, comprised of scientists from the University of Sydney and the Centenary Institute, focused on the ClpC1–ClpP1P2 complex, a molecular machine essential for the bacterium’s survival. This complex functions as a recycling system, breaking down damaged or unnecessary proteins, allowing M. Tuberculosis to adapt and thrive even under stressful conditions. Blocking this process effectively cripples the bacterium, making it an attractive target for drug development.
“TB bacteria depend on this recycling system to stay alive, particularly under stressful conditions inside the human body,” explained Professor Warwick Britton, Laboratory Head in the Centenary Institute’s Centre for Infection &. Immunity. “Our findings show these compounds don’t simply shut the system down. Instead, each one interferes with it in a different way, triggering widespread imbalances across the whole bacterium. This disruption weakens its ability to function and survive.”
Unraveling the Complexity of Antibiotic Action
The researchers meticulously tracked changes in over 3,000 proteins within M. Tuberculosis to understand the full impact of these experimental antibiotics. Isabel Barter, a PhD candidate at the University of Sydney who too conducted research at the Centenary Institute, described the scope of the investigation. “By tracking changes across most of the bacterium’s protein network, we were able to notice how disrupting a single essential complex can reshape the bacterium’s entire internal protein landscape,” she said. “This deeper understanding gives us valuable insight into how we might refine these compounds and design more precise and effective anti-TB treatments.”
The study revealed that each of the three compounds interacts with the ClpC1–ClpP1P2 complex in a unique way, creating a cascade of disruptions throughout the bacterial cell. This nuanced understanding is crucial for optimizing the design of future anti-TB drugs.
A Promising, Yet Underexplored, Drug Target
Professor Richard Payne from the University of Sydney emphasized the potential of directly targeting the ClpC1–ClpP1P2 complex. “Our study highlights the potential of directly targeting this protein degradation system,” he stated. “By understanding how different compounds interact with it and disrupt its normal function, we can more strategically design the next-generation of anti-TB drugs.”
The team’s work builds on previous research into mRNA vaccines for tuberculosis. A groundbreaking study published in February 2025 demonstrated the effectiveness of a new mRNA vaccine in pre-clinical trials, boosting immunity against TB. This vaccine, developed in collaboration with the Centenary Institute and Monash University, showed promise in both initial vaccination and as a booster to the existing BCG vaccine.
The Centenary Institute is also actively involved in developing new TB vaccines and drugs, improving understanding of TB immunology, and discovering new biomarkers to aid in diagnosis and treatment. Their research is part of the Centre of Research Excellence in Tuberculosis Control, facilitating the translation of discoveries into practical tools for TB control, as detailed on the Centenary Institute website.
What’s Next in the Fight Against Tuberculosis?
This latest research represents a significant step forward in the ongoing effort to combat tuberculosis, including drug-resistant forms of the disease. While these experimental antibiotics are still in the early stages of development, the detailed understanding of their mechanism of action provides a strong foundation for future drug design. The team believes this work will contribute to an expanded pipeline of potential treatment options, offering hope for a future where TB is no longer a global health crisis.
Further research will focus on refining these compounds and conducting more extensive pre-clinical and clinical trials to assess their safety and efficacy in humans. The ongoing collaboration between the University of Sydney and the Centenary Institute will be crucial in translating these promising findings into tangible benefits for patients worldwide.
What are your thoughts on the potential of new antibiotic research to combat drug-resistant infections? Share your comments below.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.