Table of Contents
- 1. Healthcare Costs Threaten Social Security Benefits for Millions of Seniors
- 2. The Growing Financial Strain
- 3. Disparities in Healthcare Spending
- 4. Available Assistance Programs – And Barriers To Access
- 5. Looking Ahead
- 6. Understanding Medicare and Social Security
- 7. Frequently Asked Questions
- 8. How do rising prescription drug prices specifically affect Medicare beneficiaries with limited incomes?
- 9. The Impact of Rising Health Costs on Medicare Beneficiaries’ Income
- 10. Understanding the Financial Strain
- 11. Key Drivers of Increasing Medicare Costs
- 12. How Rising Costs Impact Different Income Levels
- 13. Specific Cost Categories and Their Impact
- 14. Strategies for Managing Healthcare Costs
- 15. Real-World Example: The Case of Mrs. Eleanor Vance
Washington D.C. – A New Analysis Reveals That Rising Healthcare Expenses Are Substantially Impacting The Financial Stability Of Millions Of Americans Who Rely On Social Security,With Out-Of-Pocket Costs Consuming A substantial Portion Of Their Income.
The Report, Released Today, Highlights The Increasing Burden Faced By Medicare Beneficiaries, Notably Those With Limited Incomes, As They Struggle To Afford Essential Healthcare Services Beyond What Medicare Covers.
The Growing Financial Strain
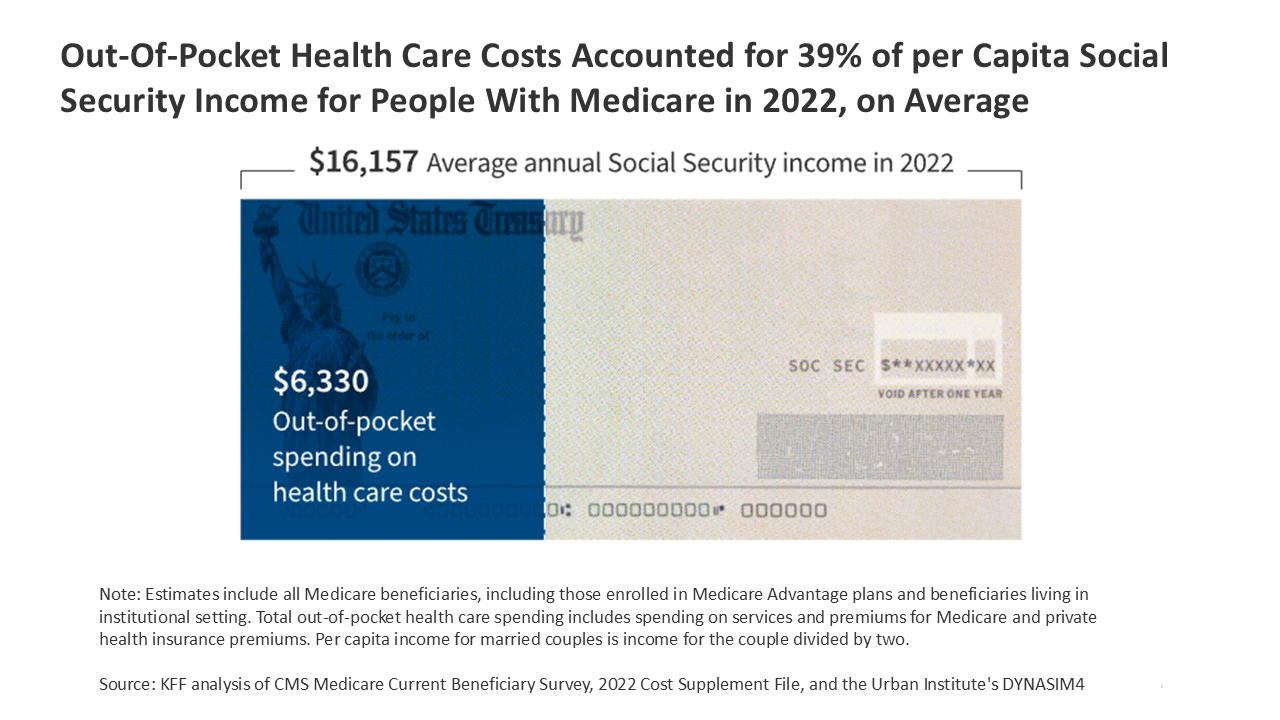
In 2022,Medicare Beneficiaries Spent An Average Of $6,330 Out Of Pocket On Healthcare,Including Premiums And Costs For Covered And Non-Covered Services Such As Dental,Vision,And Long-Term Care. This Amount Represents 39% Of The Average Per capita Social Security Income Of $16,157.
While Most Beneficiaries Have Additional Income Sources, More Than One-Third Rely On Social Security For At Least Half Of Their Income.One In Four Beneficiaries Had Income Below $21,000 In 2023, And Half Earned Less Than $36,000.
Disparities in Healthcare Spending
The Financial Burden Is Not Distributed Equally. Beneficiaries With Lower Incomes Bear A Disproportionately Higher Share Of Healthcare Costs, Accounting For 34% Of Their Total Income Compared To Just 7% For Those With Higher Incomes.
Moreover, Individuals Aged 85 And Older Experience Significantly Higher Out-Of-Pocket Expenses, Consuming 22% Of Their Income, Primarily Due To The Rising Costs Of Long-Term Care. This Is Higher Than The 9% Spent By those Aged 65-74.
Did You Know? Medicare Part B And D Premiums, Along With Cost-Sharing Requirements, Account For Nearly One-Fourth Of The Average Monthly Social Security Benefit, Not Including Other Healthcare Expenses.
Available Assistance Programs – And Barriers To Access
Programs Like Medicaid And The Medicare Savings Programs Offer Financial Assistance To Low-Income Beneficiaries, Helping To Cover Premiums And Out-Of-Pocket Costs. Though, Recent Legislative Changes May Reduce Access To These Programs, Perhaps Worsening The Financial Strain On Vulnerable populations.
Moreover, Many Eligible Beneficiaries Do Not Currently Receive The Assistance They Qualify For, Often Due To Lack Of Awareness Or Complex Submission Processes. It is estimated that Millions of eligible individuals are missing out on aid.
| Income Level | Avg. Out-of-Pocket as % of Total Income |
|---|---|
| $10,000 or Less | 34% |
| $20,000 – $29,999 | 18% |
| $30,000 – $49,999 | 12% |
| $50,000 or more | 7% |
Pro Tip: Explore State-Specific Assistance Programs. The availability and eligibility requirements for Medicare Savings Programs vary significantly by state.
Looking Ahead
Addressing The Affordability Of Healthcare For Social Security Recipients Will Require A Multi-Faceted Approach, Including Strengthening Financial Assistance Programs, Controlling Healthcare Costs, And Improving Access To Affordable Coverage Options.
Without Action, The Growing Financial Strain On Seniors Could lead To Reduced access To Care, Worsening Health Outcomes, And Increased Financial Hardship.
What Steps Can Be Taken To Ensure That Medicare Remains A Lasting and Affordable Program For Future Generations? How Can we Better Support Vulnerable seniors Who Are Struggling To Afford Healthcare?
Medicare Is A Federal Health Insurance Program Primarily For individuals 65 Or Older, As Well As Younger People With Certain Disabilities Or Conditions. It Is Composed Of Four Parts: Part A (Hospital Insurance), Part B (Medical Insurance), Part C (medicare Advantage), And Part D (Prescription Drug Insurance).
Social Security Is A Federal program That Provides Retirement, Disability, And Survivors Benefits. it is indeed Funded Through Payroll Taxes Paid By Workers And Employers.
The Interplay Between These Two Programs Is Critical For The Financial well-Being Of millions Of Americans. As Healthcare Costs Continue To Rise, it is indeed Essential To Protect The Solvency And Accessibility Of Both Medicare And Social Security.
Frequently Asked Questions
- What is Medicare? Medicare is federal health insurance for people 65+ or with certain disabilities.
- How does healthcare spending impact Social Security? High healthcare costs reduce the amount of Social Security income available for other needs.
- Are there programs to help with Medicare costs? Yes, Medicaid and Medicare savings Programs can provide financial assistance.
- Who is most affected by high healthcare costs? Low-income beneficiaries and those 85 and older are disproportionately affected.
- What can be done to address this issue? Strengthening assistance programs, controlling healthcare costs, and improving access to affordable coverage are crucial.
share this article to help raise awareness about this critical issue. Leave your comments below – we want to hear your thoughts!
How do rising prescription drug prices specifically affect Medicare beneficiaries with limited incomes?
The Impact of Rising Health Costs on Medicare Beneficiaries’ Income
Understanding the Financial Strain
Rising healthcare costs are a notable concern for all Americans, but the impact is especially acute for those on Medicare. Many beneficiaries live on fixed incomes – Social security,pensions,and personal savings – making them especially vulnerable too increases in health expenses. This article explores how these rising costs affect Medicare beneficiaries’ income, available resources, and overall financial well-being. we’ll cover specific cost drivers, the impact on different income levels, and strategies for managing these challenges.
Key Drivers of Increasing Medicare Costs
Several factors contribute to the escalating costs within the Medicare system. Understanding these drivers is crucial for appreciating the financial burden on beneficiaries.
Prescription drug Prices: The cost of medications,particularly specialty drugs,has risen dramatically. While Medicare Part D helps cover these costs, beneficiaries frequently enough face ample out-of-pocket expenses, including deductibles, copayments, and the dreaded “donut hole” (coverage gap).
Technological Advancements: While medical innovation is vital, new technologies and treatments often come with a high price tag. These advancements, while improving care, contribute to overall healthcare spending.
Aging Population: As the population ages, the demand for healthcare services increases, putting upward pressure on costs.More people qualifying for Medicare benefits means greater utilization of the system.
Chronic Disease Prevalence: The increasing prevalence of chronic conditions like diabetes,heart disease,and arthritis requires ongoing medical care,driving up long-term healthcare expenditures. Medicare and chronic disease management are intrinsically linked.
Healthcare provider Costs: Fees for services from doctors, hospitals, and other healthcare providers continue to rise, impacting Medicare costs and beneficiary expenses.
How Rising Costs Impact Different Income Levels
The effect of rising health costs isn’t uniform across all Medicare recipients. The impact varies significantly based on income level.
Low-Income Beneficiaries: Individuals with limited income frequently enough struggle to afford Medicare premiums, deductibles, and copayments. They may delay or forgo necessary care,leading to poorer health outcomes. Programs like Medicare Savings Programs (msps) can help with these costs, but eligibility requirements can be strict.
Middle-Income Beneficiaries: This group may find their fixed incomes stretched thin by increasing healthcare expenses. They may need to make challenging choices between healthcare and other essential needs like food,housing,and transportation. Medicare advantage plans can sometimes offer lower out-of-pocket costs, but may come with network restrictions.
High-Income Beneficiaries: While better able to absorb higher costs,even those with substantial income can be significantly impacted by major medical events or long-term care needs. Income-related Monthly Adjustment Amount (IRMAA) adjustments to Medicare Part B and Part D premiums further increase their expenses.
Specific Cost Categories and Their Impact
Let’s break down specific cost categories and how they affect Medicare beneficiaries’ finances.
Medicare Part B Premiums: These premiums, covering doctor visits and outpatient care, can be substantial, especially for higher-income earners subject to IRMAA.
Medicare Part C (Medicare Advantage) Costs: While offering potential benefits, Medicare Advantage plans often have copayments, deductibles, and network limitations that can impact out-of-pocket spending.
Medicare part D Premiums & Costs: Prescription drug coverage through Part D involves premiums, deductibles, copayments, and navigating the coverage gap.
Medigap Policies: These supplemental insurance policies help cover out-of-pocket costs, but come with monthly premiums that add to the overall financial burden.
* Out-of-Pocket Maximums: Even with Medicare coverage, beneficiaries can face significant out-of-pocket expenses until they reach their plan’s maximum.
Strategies for Managing Healthcare Costs
Fortunately, several strategies can definitely help Medicare beneficiaries manage rising healthcare costs and protect their income.
- Review Yoru Medicare Plan Annually: During Medicare Open Enrollment (October 15 – December 7), carefully compare different Medicare plans to find the best coverage for your needs and budget.
- Explore Cost-Saving Programs: Investigate eligibility for programs like MSPs, Low-Income Subsidy (LIS) for Part D, and state-specific assistance programs.
- Generic Medications: Discuss with your doctor the possibility of switching to generic medications, which are typically much cheaper than brand-name drugs.
- Preventive Care: Take advantage of Medicare’s preventive services, which are often covered at no cost, to help prevent costly health problems down the road.
- Negotiate Medical Bills: Don’t hesitate to negotiate medical bills with your healthcare providers. You may be able to secure a discount or payment plan.
- Health Savings Accounts (HSAs): If eligible, consider contributing to an HSA to save for future healthcare expenses. (Note: HSAs are generally not available to those enrolled in traditional Medicare.)
- Understand your benefits: Knowing what your Medicare benefits cover can help you avoid unexpected costs.
Real-World Example: The Case of Mrs. Eleanor Vance
Mrs. Vance