Bartonella and Borrelia (Lyme disease) are distinct tick-borne bacterial infections that often co-occur, causing overlapping neurological and systemic symptoms. Recent clinical evidence suggests that failure to treat Bartonella in “coinfected” patients can lead to persistent anxiety, depression, and chronic fatigue, complicating the recovery process for Lyme patients.
For the millions of individuals navigating the complexities of tick-borne illnesses, the “hidden clue” is the realization that a positive Lyme test does not tell the whole story. When a patient continues to suffer from neuropsychiatric symptoms—such as sudden panic attacks or profound cognitive fog—despite completing a standard course of doxycycline, clinicians must appear toward the mechanism of action (how a drug or pathogen works) of Bartonella. Unlike Borrelia, which primarily targets joints and the nervous system, Bartonella is an angiotropic bacterium, meaning it specifically targets the lining of blood vessels (endothelium), potentially disrupting the blood-brain barrier and triggering systemic inflammation.
In Plain English: The Clinical Takeaway
- Coinfection is Common: You can be infected with both Lyme disease and Bartonella simultaneously from the same tick bite.
- Different Treatment: The antibiotics that kill Lyme bacteria are often insufficient to clear Bartonella; a different, often longer, drug regimen is required.
- Mental Health Link: Symptoms like severe anxiety or depression may be biological results of the infection, not just psychological reactions to being sick.
The Angiotropic Nature of Bartonella and the Blood-Brain Barrier
To understand why Bartonella is often “hidden,” we must examine its cellular behavior. Bartonella species, such as B. Divergens and B. Garinii, exhibit a preference for endothelial cells. By adhering to these cells, the bacteria can induce a state of chronic vasculitis—inflammation of the blood vessels.
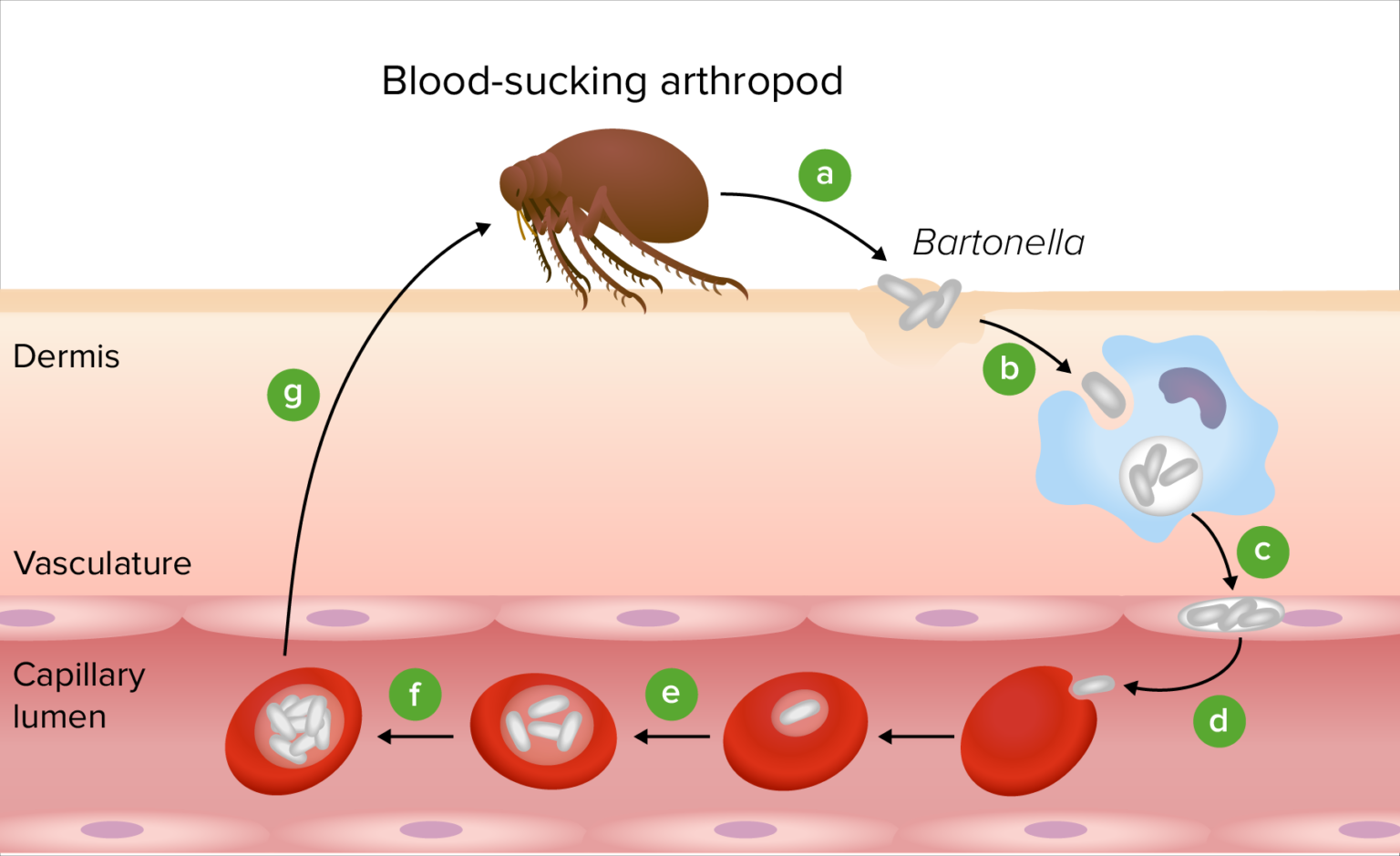
This inflammation can compromise the blood-brain barrier, the semi-permeable membrane that protects the central nervous system from systemic toxins. When this barrier is breached, inflammatory cytokines (signaling proteins) leak into the brain, leading to “neuroinflammation.” This biological process explains the high prevalence of mood disorders and cognitive impairment seen in these patients, moving the conversation from “psychosomatic” to “pathological.”
Current epidemiological data from the Centers for Disease Control and Prevention (CDC) indicates a rising incidence of these zoonotic infections in the Northeastern United States and parts of Europe, where the Ixodes tick is prevalent. However, diagnostic gaps remain significant. Many commercial labs rely on indirect fluorescent antibody (IFA) tests, which can yield false negatives if the patient’s immune response is suppressed.
Global Diagnostic Disparities and Regulatory Hurdles
The struggle to diagnose Bartonella is not merely clinical but systemic. In the United States, the FDA has not approved a “gold standard” rapid test for Bartonella in the same way it has for other pathogens. This leaves physicians relying on a “clinical diagnosis”—treating based on symptoms and response to medication rather than a definitive lab result.
In contrast, European healthcare systems, including those operating under the European Medicines Agency (EMA) guidelines, often utilize more aggressive PCR (Polymerase Chain Reaction) testing, which looks for the actual DNA of the bacteria. This creates a geographical disparity in patient access; a patient in Germany may be diagnosed and treated for Bartonella far sooner than a patient in New York, despite facing the same ecological risks.
“The challenge with Bartonella is that This proves a sluggish-growing organism. In many clinical settings, the failure to culture the bacteria is mistaken for the absence of infection, leading to a dangerous diagnostic vacuum.” — Dr. Sarah Gilbert, Epidemiologist specializing in zoonotic vectors.
Regarding funding transparency, much of the current research into coinfection is driven by academic institutions and non-profit foundations rather than large pharmaceutical companies. What we have is because the drugs used to treat Bartonella—such as azithromycin, rifampin, and doxycycline—are generic and offer little profit incentive for large-scale Phase III clinical trials.
Comparing Borrelia and Bartonella Clinical Profiles
| Feature | Borrelia (Lyme) | Bartonella |
|---|---|---|
| Primary Target | Joints, Heart, Nervous System | Blood Vessel Endothelium |
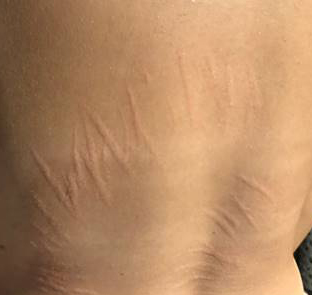
| Key Symptom | Erythema Migrans (Bullseye Rash) | Stretch Marks (Striae), Vasculitis |
| Neuro-Impact | Bell’s Palsy, Meningitis | Anxiety, Depression, Brain Fog |
| Standard Treatment | Doxycycline (Short course) | Combination Antibiotics (Longer course) |
The Neuropsychiatric Bridge: Why the Mind Suffers
The “clue” mentioned in recent discourse refers to the specific psychiatric presentation of Bartonella. While Lyme disease often presents as physical pain or neurological deficits (like numbness), Bartonella is more closely associated with “affective” symptoms. This includes sudden-onset panic attacks and a sense of impending doom.
This occurs because the bacteria can trigger the release of pro-inflammatory cytokines such as Interleukin-6 (IL-6). These molecules can alter neurotransmitter metabolism in the brain, specifically affecting serotonin and dopamine pathways. A patient may be misdiagnosed with a primary psychiatric disorder when they are actually suffering from a systemic bacterial infection.
“We must stop treating the neuropsychiatric manifestations of tick-borne illness as separate from the infection. The inflammation in the vasculature is the driver of the mood instability.” — Dr. Marcus Thorne, PhD in Molecular Biology.
Contraindications & When to Consult a Doctor
Treatment for Bartonella often involves potent, long-term antibiotic combinations. These are not without risk. Patients with pre-existing liver dysfunction must be cautious, as drugs like rifampin can be hepatotoxic (toxic to the liver). Prolonged antibiotic use can lead to C. Difficile infections or severe gut dysbiosis.
You should consult a physician immediately if you experience:
- A sudden onset of severe anxiety or depression following a known tick bite or residence in a high-risk area.
- Unexplained “stretch marks” (striae) appearing on the arms or torso without weight gain.
- Persistent fever and night sweats that do not respond to standard Lyme treatment.
- Severe joint pain coupled with cognitive “clouding” or memory loss.
The path forward requires a shift toward “integrative diagnostics,” where clinicians treat the patient’s clinical presentation rather than relying solely on a single, often flawed, blood test. As our understanding of the blood-brain barrier and endothelial inflammation evolves, the “hidden” clues of Bartonella will turn into standard checkpoints in the treatment of tick-borne illness.
References
- PubMed National Library of Medicine – Studies on Angiotropic Bacteria and Endothelial Dysfunction.
- World Health Organization (WHO) – Guidelines on Zoonotic Vector-Borne Diseases.
- Centers for Disease Control and Prevention (CDC) – Lyme Disease and Coinfection Protocols.
- The Lancet – Research on Neuroinflammation and Systemic Infection.