Tiger Woods’ Arrest and Opioid Use: A Public Health Perspective
Professional golfer Tiger Woods, 50, was arrested this week following a single-vehicle accident and subsequent refusal to submit to a urine drug screen. The incident, occurring after a prior DUI arrest, has brought renewed attention to the intersection of chronic pain management, opioid dependence, and impaired driving. Reports indicate Woods possessed two hydrocodone pills at the time of the arrest, and preliminary investigations suggest he may have been under the influence of a combination of substances.
This case extends beyond a celebrity scandal; it highlights a critical public health issue: the ongoing opioid crisis and the challenges faced by individuals managing chronic pain. Woods’ history of multiple surgeries and documented pain management strategies underscore the complexities of balancing effective pain relief with the risks of opioid dependence and potential misuse. The incident similarly raises questions about the accessibility of alternative pain management therapies and the societal pressures that can contribute to substance use.
In Plain English: The Clinical Takeaway
- Opioids and Risk: Prescription painkillers, like hydrocodone, can be effective for severe pain, but carry a risk of addiction and side effects.
- Impaired Driving: Driving under the influence of any substance – alcohol or drugs – significantly increases the risk of accidents and serious injury.
- Seeking Assist: If you or someone you know is struggling with chronic pain or substance use, You’ll see resources available to help. Don’t hesitate to reach out to a healthcare professional.
The Pharmacology of Hydrocodone and the Cycle of Pain
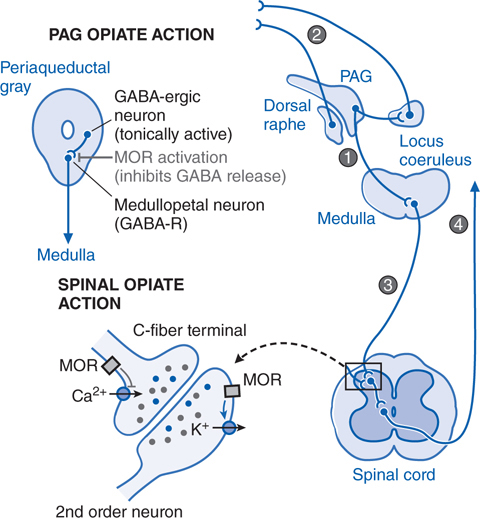
Hydrocodone is a semi-synthetic opioid analgesic, classified as a Schedule II controlled substance by the Drug Enforcement Administration (DEA) in the United States. Its mechanism of action involves binding to opioid receptors – primarily mu-opioid receptors – in the central nervous system. This binding reduces the perception of pain by altering how the brain and nervous system process pain signals. However, this same mechanism also triggers the release of dopamine, creating a euphoric effect that contributes to the potential for addiction. Chronic opioid use can lead to tolerance, requiring higher doses to achieve the same pain relief, and physical dependence, resulting in withdrawal symptoms upon cessation.
The prevalence of chronic pain in the United States is substantial. According to the Centers for Disease Control and Prevention (CDC), approximately 20.9% of U.S. Adults experienced chronic pain in 2022 [ CDC Chronic Pain Statistics]. Many individuals turn to opioids for relief, but non-opioid alternatives, such as physical therapy, cognitive behavioral therapy, and non-steroidal anti-inflammatory drugs (NSAIDs), are increasingly recommended as first-line treatments. The shift towards multimodal pain management aims to minimize opioid exposure while maximizing pain control.
Geographical Impact and Regulatory Responses
The opioid crisis is not uniformly distributed geographically. States with higher rates of opioid prescriptions and a greater prevalence of chronic pain conditions, such as West Virginia and Kentucky, have been disproportionately affected. The Food and Drug Administration (FDA) has implemented several measures to address the crisis, including stricter prescribing guidelines, increased monitoring of opioid manufacturers, and the promotion of alternative pain management strategies. These efforts are ongoing, and their effectiveness is continuously evaluated.
In Europe, the European Medicines Agency (EMA) also regulates opioid medications, with similar concerns regarding overuse and addiction. National healthcare systems, like the National Health Service (NHS) in the United Kingdom, are implementing strategies to reduce opioid prescribing and improve access to non-pharmacological pain management options. The EMA’s focus is on harmonizing regulations across member states and promoting responsible opioid use.
Opioid Prescription Rates by Region (2023)
| Region | Opioid Prescriptions per 100 Population |
|---|---|
| United States | 42.5 |
| Canada | 22.1 |
| United Kingdom | 8.7 |
| Germany | 6.3 |
| Japan | 1.8 |
Data Source: IQVIA, 2024. Represents prescriptions for all opioid analgesics.
Funding and Bias Transparency
Research into pain management and opioid dependence is often funded by pharmaceutical companies, government agencies (like the National Institutes of Health – NIH), and private foundations. It’s crucial to acknowledge potential biases inherent in research funded by pharmaceutical companies, as there may be a vested interest in promoting opioid use. Independent research, funded by government agencies or non-profit organizations, is essential for providing unbiased evidence and informing public health policy. A recent study published in *JAMA Internal Medicine* highlighted the influence of pharmaceutical industry funding on opioid-related research [ JAMA Internal Medicine Study].
“The opioid crisis is a complex issue with no easy solutions. We necessitate to prioritize research into non-opioid pain management strategies and address the underlying social and economic factors that contribute to substance use.” – Dr. Nora Volkow, Director of the National Institute on Drug Abuse (NIDA).
The Role of Mental Health and Co-occurring Disorders
Substance use disorders frequently co-occur with mental health conditions, such as depression and anxiety. Individuals with pre-existing mental health conditions may be more vulnerable to opioid dependence, and opioid use can exacerbate mental health symptoms. Integrated treatment approaches that address both substance use and mental health are essential for achieving long-term recovery. The National Survey on Drug Use and Health (NSDUH) consistently demonstrates a strong correlation between mental health disorders and substance use [ SAMHSA NSDUH Data].
Contraindications & When to Consult a Doctor
Opioid medications are contraindicated in individuals with:
- A history of opioid addiction or substance use disorder.
- Severe respiratory conditions, such as asthma or chronic obstructive pulmonary disease (COPD).
- Severe liver or kidney disease.
- Known allergies to opioids.
Consult a doctor immediately if you experience any of the following symptoms while taking opioids:
- Difficulty breathing or slowed breathing.
- Severe drowsiness or confusion.
- Constipation that does not improve with over-the-counter remedies.
- Signs of an allergic reaction, such as rash, hives, or swelling.
Looking Ahead: Towards a More Sustainable Approach to Pain Management
The case of Tiger Woods serves as a stark reminder of the challenges associated with chronic pain management and the potential consequences of opioid misuse. Moving forward, a comprehensive and multifaceted approach is needed, encompassing increased access to non-opioid pain management therapies, improved mental health services, and a reduction in the stigma associated with substance use disorders. Continued research into the neurobiology of pain and the development of novel pain medications are also crucial. A shift towards a more holistic and patient-centered approach to pain management is essential for mitigating the opioid crisis and improving the health and well-being of individuals struggling with chronic pain.
References
- National Institute on Drug Abuse (NIDA). (2023). Opioid Facts. https://www.drugabuse.gov/drug-topics/opioids
- Centers for Disease Control and Prevention (CDC). (2022). Chronic Pain in America. https://www.cdc.gov/chronicpain/index.htm
- European Medicines Agency (EMA). (2024). Opioid Medicines. https://www.ema.europa.eu/medicines/human/scientific-guidelines/pharmaceutical-development/opioid-medicines
- Volkow, N. D. (2018). The opioid crisis: A call for a fresh approach to pain management. *The Lancet*, *391*(10131), 1601-1602.

